-
PDF
- Split View
-
Views
-
Cite
Cite
Dana Tasabehji, Mohammad Jarrah, Mohamad Mokadem, Atypical presentation of an epiphrenic esophageal diverticulum 20 years post fundoplication: a case report and review, Journal of Surgical Case Reports, Volume 2024, Issue 5, May 2024, rjae316, https://doi.org/10.1093/jscr/rjae316
Close - Share Icon Share
Abstract
Esophageal diverticulum is a rare condition characterized by the herniation of the esophageal mucosa outside the esophageal wall. Here, we explore the prevalence of ED and its associated esophageal dysmotility. We also shed light on the potential impact of previous surgical interventions, such as Nissen’s fundoplication, on the development of ED. This manuscript presents the case of a 72-year-old woman with a history of Nissen’s fundoplication surgery who experienced worsening symptoms of dysphagia, heartburn and postprandial cough. Despite exhibiting a normal motility pattern, upper endoscopy revealed a large epiphrenic esophageal diverticulum. The patient underwent successful surgical resection with myotomy, resulting in the resolution of symptoms with no complications. This case highlights the rarity of symptomatic ED and the need to recognize it while choosing the optimal treatment modality.
Introduction
Esophageal diverticulum is an uncommon entity that involves herniation of the esophageal mucosa outside the esophageal wall, with a prevalence ranging from 0.06% to 4% according to radiologic and endoscopic series [1–4]. These diverticula may occur in various locations, with different nomenclature based on the location. Diverticula in the pharyngoesophageal area are known as Zenker’s diverticulum, and those distally are referred to as epiphrenic diverticula (ED) [1]. ED are protrusions of the esophageal lumen originating in the distal third of the esophagus near the diaphragm [5–7]. Radiological studies, mainly contrast esophagography, show a prevalence of ED at ~0.0015% in the USA, 0.77% in Japan, and 2% in Europe [8–10]. The estimated prevalence of ED is 1 in 5 compared to Zenker’s diverticulum [5]. Patients can be asymptomatic or might present with features of dysphagia, regurgitation, or compressive symptoms due to mechanical pressure from increasing size [4, 11]. Here, we present a case of a patient with a symptomatic esophageal ED who had a surgical history of Nissen’s fundoplication and no underlying esophageal motility disorder on manometry. With surgical resection of the diverticulum, the patient’s symptoms resolved with no complaints afterwards.
Case presentation
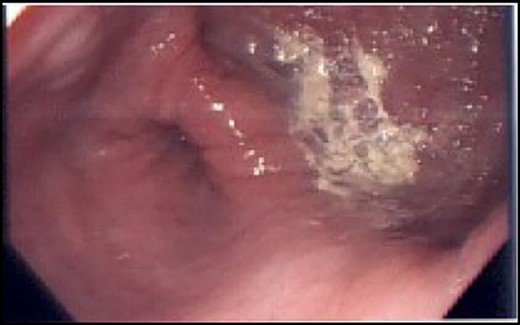
A 72-year-old woman with a past medical history of coronary artery disease and chronic gastroesophageal reflux disease (GERD) with hiatal hernia status postsurgical correction by Nissen’s fundoplication 20 years ago, presented with worsening episodes of intermittent dysphagia, heartburn, and postprandial cough of ~2 years duration but worsening symptoms over the past 2 months. She denies any symptoms of food regurgitation, nausea, vomiting, appetite, or weight changes. Upon her initial clinic evaluation, she had normal vital signs and unremarkable findings on the physical exam. The decision was made to start her empirically on a proton pump inhibitor, assuming her symptoms are related to GERD, to which she did not respond appropriately. A subsequent upper endoscopy revealed a large epiphrenic wide-mouthed ED (Fig. 1). Additionally, an esophagram showed a 6.0 × 5.0 cm epiphrenic ED with a 3.3 cm neck (Fig. 2). High-resolution esophageal manometry (HREM) was performed; thereafter, revealing a normal motility pattern (Fig. 3). She was then referred to cardiothoracic surgery for consideration of surgical repair. She was initially advised to follow a dysphagia-specific diet and wait conservatively on her symptoms, but no changes were observed in her clinical course over 6 months. The patient subsequently underwent a successful uncomplicated esophageal diverticulectomy with myotomy, conducted through a lateral thoracotomy. During surgery, an esophagogastroduodenoscopy (EGD) revealed an ED at 35 cm in the gastroesophageal (GE) junction at 40 cm in the epiphrenic region. A standard posterior lateral thoracotomy was performed in the serratus-sparing fashion, and the pleural space was entered at the seventh intercostal space. The esophagus was encircled with a Penrose drain lifting it up, and it was freed from the periaortic tissue, and the ED cleared off all muscle fibers. The diverticulum was excised from the esophagus using a purple load stapler with an EGD scope in place to prevent esophageal narrowing. A myotomy was performed from the GE junction proximally, with negative leak testing. The muscle layer was then imbricated over the area of diverticulectomy, and a chest tube was inserted for drainage. A postoperative esophagram confirmed no presence of an ED (Fig. 4). Immediately after the surgery, the patient had a complete resolution of her symptoms, and during her 1-year follow-up visit, she remained asymptomatic.
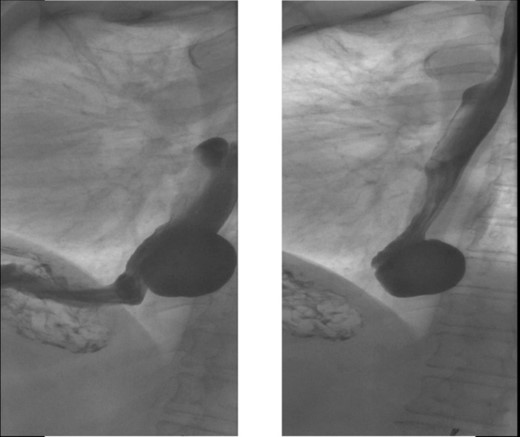
X-ray esophagram fluoroscopy showing a 6.0 × 5.0 cm epiphrenic ED with a 3.3 cm neck.
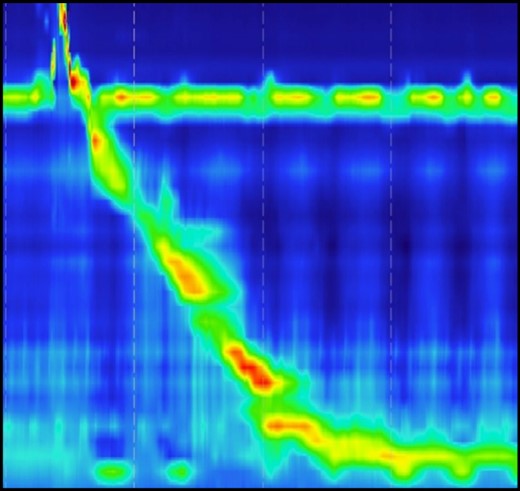
Normal motility pattern on high-resolution manometry test in a patient with epiphrenic ED.
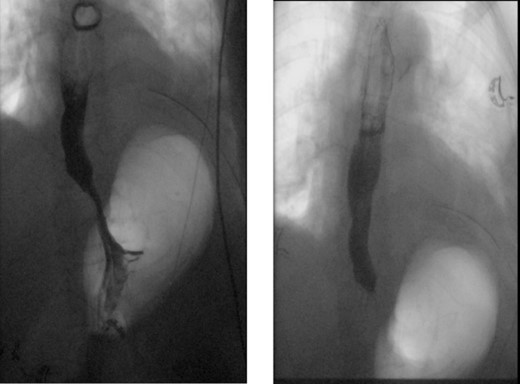
Normal X-ray esophagram fluoroscopy postdiverticulectomy with myotomy surgery.
Discussion
ED, or epiphrenic diverticula, are uncommon protrusions of the esophageal mucosa located in the lower esophagus near the gastroesophageal junction [12]. The exact cause of ED is not fully known, but it is believed to be associated with increased intraluminal esophageal pressure and underlying esophageal motility disorders [2, 13]. Symptoms can vary depending on the size of the diverticulum and coexisting morbidities [14]. Diagnostic workup typically includes a barium swallow study, upper endoscopy, and high-resolution esophageal manometry (HREM) [15–17]. It is important to perform HREM before intervention to incorporate any discovered dysmotility into the treatment plan [4, 18, 19]. However, it is worth noting that in rare cases, motility disorders may not be identified, as seen in our patient [20]. Surgical treatment is recommended for symptomatic patients and those with large diverticula [21]. The standard approach is diverticulectomy with myotomy [22–31], although less invasive techniques like laparoscopy and per-oral endoscopic myotomy (POEM) are gaining popularity [32–35]. The choice of surgical technique varies, with some studies advocating for myotomy alone [26, 28] and others suggesting a combination of myotomy and fundoplication [31]. In our patient's case, she presented with symptomatic ED following a history of Nissen's fundoplication. There is limited research exploring the impact of previous surgical interventions, such as fundoplication, on the development of ED [18]. Surgical intervention was warranted due to the patient's symptomatic presentation and large diverticulum, resulting in complete resolution of her symptoms [25]. While traditional surgical approaches are effective, less invasive methods such as laparoscopy and POEM offer reduced postoperative morbidity and mortality [21, 27–30, 32–35]. POEM, in particular, is gaining traction for its minimally invasive nature and ability to avoid the need for diverticulectomy [32–35]. Further research is needed to determine the optimal treatment modality for ED and to explore the correlation between ED and previous fundoplication surgeries.
In conclusion, ED is a rare condition that can cause various symptoms in the lower esophagus near the GE junction. It is associated with increased esophageal pressure and underlying motility disorders. Diagnosis typically involves imaging and HREM, which often reveal abnormal motility patterns. Surgical treatment is recommended for symptomatic patients and those with large diverticula, with diverticulectomy and myotomy being the standard approaches. However, less invasive techniques, like laparoscopy and POEM, are emerging as alternative options. The impact of previous surgical interventions, specifically fundoplication, on the development of ED requires further investigation. Future research will provide a better understanding of the optimal treatment modality and outcomes for ED.
Conflict of interest statement
None declared.
Funding
This work was supported by the VA Merit Review Program (I01 BX004774), The University of Iowa Department of Internal Medicine and Fraternal Order of Eagles Diabetes Research Center.
Data availability
All data related to this manuscript are patient-protected and are available upon request by contacting the corresponding author.
References
- deglutition disorders
- cough
- esophageal diverticula
- esophageal motility disorder
- upper gastrointestinal endoscopy
- cell motility
- fundoplication
- heartburn
- hernias
- postprandial period
- surgical procedures, operative
- myotomy
- acquired supradiaphragmatic diverticulum of esophagus
- diverticulectomy
- esophageal mucous membrane
- excision
- atypical



