-
PDF
- Split View
-
Views
-
Cite
Cite
Shareefa Abdulghaffar, Noor Badrawi, Swaroop Keshe Gowda, Usama AlBastaki, Dana AlNuaimi, Acute pancreatitis as a late complication of intra-gastric balloon insertion, Journal of Surgical Case Reports, Volume 2021, Issue 4, April 2021, rjab139, https://doi.org/10.1093/jscr/rjab139
Close - Share Icon Share
Abstract
Intra-gastric balloon (IGB) insertion is a safe, well-tolerated and an effective weight loss procedure. It is commonly used as a step prior to bariatric surgery in obese patients with co-morbidities and failed conservative weight-loss methods. The main side effects post-IGB placement include nausea, vomiting and abdominal pain. The reported complications of IGB include balloon over-inflation, balloon migration, esophagitis, ulceration, gastric perforation and bowel obstruction. We report a case of acute pancreatitis attributed to IGB placement, which is a rare complication of this procedure. The diagnosis of acute pancreatitis due to IGB was made after excluding other causes of acute pancreatitis by radiological imaging. The patient underwent endoscopic IGB removal with rapid post-surgical improvement of her clinical course.
INTRODUCTION
Obesity is considered a global health pandemic, and it is a well-documented predisposing factor to serious medical conditions such as hypertension, cardiovascular diseases and diabetes mellitus type II. Many surgical and non-surgical methods of treatment have been explored and showed varying degrees of efficacy and satisfactory results ranging from lifestyle modification to bariatric surgery [1]. One of the relatively safe methods is placement of an intragastric balloon (IGB). It is a short-term non-surgical weight reduction method with an estimated overall weight loss of approximately 15–20% of total body weight [2]. Many side effects have been reported ranging from mild symptoms such as nausea, abdominal pain and gastroesophageal reflux to serious life-threatening complications including ulceration, perforation and bowel obstruction [1]. According to literature, a handful of cases have reported acute pancreatitis as a complication of IGB placement [3–7]. Most of these cases reported this complication shortly after IGB insertion; however, in our case, it occurred 1 year after IGB placement.
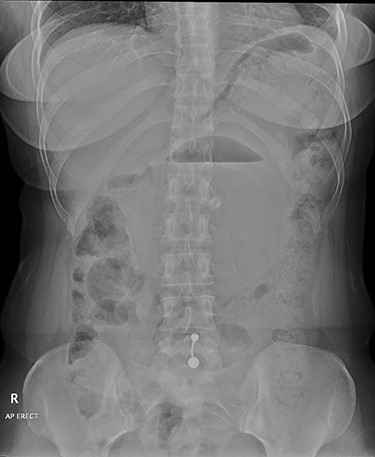
Anterior–posterior erect abdominal radiograph showing a large balloon seen in the middle of the abdomen with air/fluid level. No features of intestinal obstruction or perforation. No abnormal abdominal calcifications are noted.
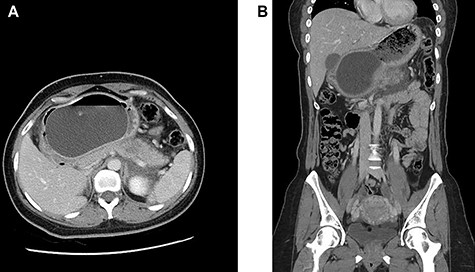
(A and B) Axial and coronal intravenous contrast-enhanced computed tomography images of the abdomen and pelvis showing an IGB compressing the pancreatic body with resultant pancreatic interstitial oedema and peri-pancreatic fluid collection.
CASE REPORT
A 36-year-old Middle—Eastern female presented to the accident and emergency department with a one-day history of severe epigastric pain associated with abdominal distention and nausea. However, there was no vomiting, constipation or urinary symptoms. The patient has no history of chronic illnesses or recent trauma. Her surgical history included laparoscopic appendectomy done 10 years back and intra-gastric balloon insertion done a year ago. The patient denied any history of alcohol consumption, and she is not on any medication. On physical examination, the patient was afebrile and vitally stable. Her abdomen was distended with no skin erythema. On palpation, severe tenderness was noted at the epigastric, right hypochondria and lumbar region with no palpable organomegaly. On auscultation, the bowel sounds were normal. Initial laboratory workup showed leucocytosis, raised lipase and amylase enzymes and elevated C—reactive protein levels. Liver and renal function tests as well as her urinalysis were within normal limits.
A plain erect abdominal radiograph (Fig. 1) was done, and it showed a large rounded balloon with air fluid level seen in the middle of the abdomen. No features of intestinal obstruction or perforation.
Intravenous contrast-enhanced computed tomography of the abdomen, pelvis was done (Fig. 2), and it showed an intra-gastric balloon compressing the pancreatic body with resultant ill-defined hypodensities noted at the pancreatic body and surrounding peri-pancreatic fluid collection suggestive of acute interstitial pancreatitis. No cholelithiasis, intrahepatic or extrahepatic biliary dilatation was seen.
Other causes of acute pancreatitis were ruled out clinically and by diagnostic imaging so the diagnosis of acute pancreatitis due to IGB compression was made, and the patient was admitted under general surgery care for urgent endoscopic removal of IGB. Upper GI endoscopy was done one day after admission, and it revealed an intact and healthy gastric mucosa with no ulcerations. The balloon was deflated and removed. The patient clinical course improved significantly postendoscopic removal of IGB with no postoperative complaints. After normalisation of her laboratory inflammatory markers, the patient was discharged home with a follow-up appointment in 2 weeks in the surgical clinic.
DISCUSSION
IGB is rapidly increasing in popularity as a safe and minimally invasive method of weight reduction. It aims to increase satiety by mechanical gastric distention leading to decrease food intake [1]. IGB involves placement of a balloon in the stomach filled with 400–700 mL of fluid under endoscopy. Duration of therapy with IGB is approximately six months after which it is to be removed [2]. Commonly seen side effects may include nausea, vomiting, abdominal pain and gastroesophageal reflux. Nevertheless, the procedure may cause serious complications including ulceration, perforation and balloon migration [1]. Rarely, acute pancreatitis may also occur as a serious complication as presented in this case.
IGB-related pancreatitis, or balloon pancreatitis, typically presents as with other causes of acute pancreatitis with epigastric pain, nausea, vomiting and fever. Biochemical markers are usually significantly elevated with evident leucocytosis, high C-reactive protein and most importantly increased levels of serum amylase and lipase [3].
Cross-sectional imaging with contrast enhancement is the modality of choice in assessment of balloon pancreatitis. It usually reveals the presence of a fluid-filled balloon distending the stomach and features of acute interstitial pancreatitis. Most common features of pancreatitis include diffuse enlargement of the gland with peripancreatic inflammation and fat stranding. The mechanism of balloon pancreatitis can be appreciated on computed tomography with the distended balloon causing mechanical pressure on the pancreatic parenchyma and obstructing of the pancreatic duct [3].
CT is also useful in detecting complications of pancreatitis or other complications related to IGB insertion such as gastric outlet obstruction, gastric ulceration, perforation and balloon migration as well as vascular compression. Imaging will also aid in exclusion of other differential diagnosis [3].
Removal of the balloon via endoscopy is the ultimate method of treatment leading to significant resolution of the symptoms and normalization of inflammatory markers decreasing the chance of significant long-term sequelae [3, 4].
CONCLUSION
Acute pancreatitis is a rare late complication of intra-gastric balloon insertion, and it is increasing in incidence with the increasing popularity of the procedure as a weight loss method. It presents with a triad of a history of a recent gastric balloon insertion, symptoms consistent with acute pancreatitis, and radiological and biochemical evidence of pancreatitis. Therefore, correlation of clinical presentation and radiological findings is crucial in achieving accurate diagnosis.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.



