-
PDF
- Split View
-
Views
-
Cite
Cite
Gustavo de Castro Gouveia, Letícia Yukari Okada, Beatriz Pires Paes, Thalita Millene Moura, Amarildo Henrique da Conceição Júnior, Rodrigo Nascimento Pinheiro, Tailgut cyst: from differential diagnosis to surgical resection—case report and literature review, Journal of Surgical Case Reports, Volume 2020, Issue 7, July 2020, rjaa205, https://doi.org/10.1093/jscr/rjaa205
Close - Share Icon Share
Abstract
Tailgut cyst is a rare tumor originating from the embryonic remnant located in the retrorectal space. The diagnosis is usually incidental duse to the absence of symptoms. When present, they are nonspecific, such as abdominal pain, dysuria and tenesmus. Imaging tests are a great help in the diagnosis and surgical planning. The standard treatment is resection, which the surgeon must perform to avoid future complications, such as malignancy. We present a case of tailgut cyst in a young patient with prior pilonidal cyst excision, subsequently submitted to surgical resection, to share our experience with a rare case, with few reports in the literature.
INTRODUCTION
Tailgut cyst is a rare, multicystic congenital lesion that originates from the remaining part of the post-anal embryonic intestine [1–4]. The literature generally describes such tumors in middle-aged women in a 3:1 ratio compared to men [2, 5]. It is difficult to evaluate the real incidence since the literature presents reports of simple cases or small case series, not to mention there are undiagnosed asymptomatic cases [3].
The diagnosis of the tailgut cyst is difficult since about 26–50% of patients are asymptomatic, usually seen as an accidental clinical or imaging finding [1, 2, 6]. However, it may become symptomatic due to a mass effect on adjacent organs, presenting pollakiuria, dysuria, defecation pain, a sensation of rectal filling, constipation or by infection, which can manifest as a pelvic abscess, hypogastric pain or, mainly, fistulas [1, 2, 3, 7].
Also, it has a long-term risk of malignancy [4, 7]. Delayed recognition or incomplete treatment can lead to increased risk [5].
Imaging exams assist in preoperative diagnosis and planning [6–9]. The procedure adopted in the case of a tailgut cyst is complete surgical excision, indicated to establish a diagnosis and avoid future complications [1].
Considering the limited number of reports on this pathology, we conclude that this study adds some contribution to the literature on the tailgut cyst, its treatment, possible sequels and prognosis. This study aims to report a case of tailgut cyst in a young patient and perform a narrative literature review to clarify a case of a rare tumor and its surgical approach.
CASE REPORT
A 28-year-old female patient with a surgical history of excision of a pilonidal cyst 2 years ago presented with local discomfort when sitting for 6 months. The examinations performed suggested a tailgut cyst, and the principal differential diagnosis was a recurrence of the pilonidal cyst. Abdominal and pelvic MRI identified an extensive collection occupying soft tissues in the sacrococcygeal region, extending anteriorly under the sacrum and coccyx to the retrorectal space on a closed end, apparently without continuity with the subcutaneous mesh in the buttocks region. It had thin and regular walls and partial parietal enhancing of the rectosacrococcygeal portion, measuring 9.9 × 7.9 × 3.9 cm, with an estimated volume of 158 ml. The collection exerted a modest compressive effect on an adjacent posterior rectal wall but maintained a well-defined cleavage plane (Fig. 1). Colonoscopy showed extrinsic compression in the posterior and right lateral wall of the inferior rectum, above the puborectalis muscle (Fig. 2). Rectal ultrasonography showed multicystic content in the retrorectal space (Fig. 3). The patient underwent a complete resection of the tailgut cyst via posterior intergluteal access. She was discharged on the first postoperative day, with no complications or sequelae and no evidence of recurrence until 18 months of postoperative follow-up.
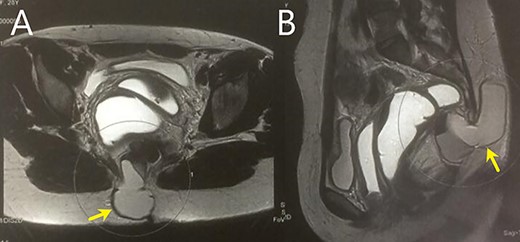
(A and B) MRI shows a large collection in the rectosacrococcygeal region, extending anteriorly to the retrorectal space.
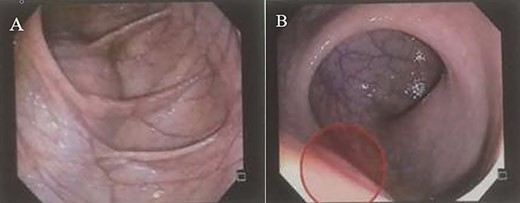
(A and B) Colonoscopy shows extrinsic compression on the rectum.
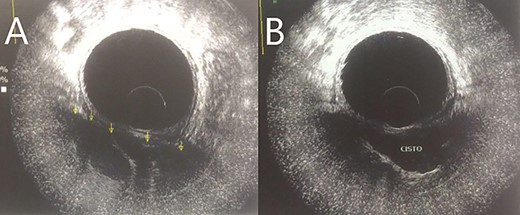
DISCUSSION
Tailgut cysts are located almost exclusively in the retrorectal space [1, 2]. The primary differential diagnoses are the retrorectal tumors of different etiologies, such as congenital, neurogenic, osteogenic and miscellaneous [1, 3, 6].
Transabdominal USG shows multicystic lesions in the retrorectal space. Transrectal USG provides information on the nature of the retrorectal mass, such as solid versus cystic, extension and degree of invasion of the rectal wall, if any [2, 9].
CT shows a granulomatous or mucous area with well-defined edges and homogeneous soft tissue density. It preserves the adjacent fat planes, and the sacrum is usually intact. When the marginal sharpness is lost, or invasion of adjacent structures is present, infection or malignancy should be suspected [3, 9]. Computed tomography also reported edge calcification [9].
MRI allows us to rule out retrorectal space-related differential diagnoses. It contributes to the choice of the surgical approach, allowing the evaluation of tumor extension, consistency and invasion of adjacent structures [3, 6, 7]. Tailgut cyst is often multilocular, while meningocele, epidermoid cyst, dermoid cyst, rectal duplication cysts and presacral cystic masses are generally unilocular [2, 6, 7]. Polypoid masses, irregular cyst walls or solid components on MRI indirectly suggest malignant transformation [10].
About 2–13% of tailgut cyst cases undergo malignant transformation [2–4, 7, 10]. The most frequent histological type is adenocarcinoma. However, there are reports of neuroendocrine tumors, carcinomas and sarcomas [3, 4, 6].
Surgical resection is indicated both in symptomatic and asymptomatic patients due to the possibility of malignancy and complications [1, 4, 7].
The transabdominal approach, reserved for lesions above S3 or the sacral promontory, is the route of choice if malignancy is suspected [1, 3, 4, 7]. Minimally invasive transanal surgery is recommended for small, inferior and uninfected tumors, due to increased risk of pelvic infection by this route [1, 4, 7]. Surgical treatment selection must consider the surgeon’s skill and expertise to avoid neural injury, leading to a worsening of neurogenic bladder and sexual dysfunction [1, 3]. Surgical management must be individualized [2, 3, 7].
Longer survival is associated with complete excision and the histological characteristics of the tumor, with a better prognosis for neuroendocrine tumors than for adenocarcinomas [1, 6, 10].
The present case is compatible with the literature concerning the affected sex, but regarding the symptoms, the patient presented only local discomfort when sitting. We adopted the complete resection approach via posterior intergluteal access. Hospital discharge happened on the first postoperative day, with no complications or sequelae and no evidence of recurrence.
In conclusion, retrorectal space tumors are rare and heterogeneous due to the tissue diversity that can arise from embryonic remnants in this topography. Considering the lack of guidelines and the scarcity of information in the literature, this report, therefore, aimed to inform and emphasize the importance of considering the tailgut cyst as a differential diagnosis for the symptoms presented to make an earlier diagnosis.
CONFLICT OF INTEREST STATEMENT
None declared.



