-
PDF
- Split View
-
Views
-
Cite
Cite
Karlijn Hummelink, Michiel A. IJsseldijk, Anne Marie Bosch, Richard P.G. ten Broek, K.C. Anthon van Engelenburg, Resection of a bony tumour of the chest wall with direct reconstruction using a sandwich technique: a standard technique for closure of large chest wall defects, Journal of Surgical Case Reports, Volume 2015, Issue 4, April 2015, rjv040, https://doi.org/10.1093/jscr/rjv040
Close - Share Icon Share
Abstract
Bony tumours of the chest wall are rare and radical surgical resection forms the cornerstone of treatment. Closure of the defect following radical resection can be challenging. We report the case of a 59-year-old woman with a large tumour of the thoracic wall, which was surgically resected with direct reconstruction using a sandwich technique with a Palacos® patch placed in a double-layer Marlex mesh. Pathological examination showed a fibrous dysplasia of the rib. The patient had a good functional and cosmetic result.
INTRODUCTION
Bony tumours of the chest wall are rare; the differential diagnostic considerations comprise benign tumours such as osteochondroma, chondroma, fibrous dysplasia (FD) and malignant tumours such as soft tissue sarcomas, osteosarcoma and Askin tumours. Surgical resection is the primary treatment for most benign and malignant chest wall tumours, which can be performed with acceptable morbidity [1].
However, closure of the chest wall defect following resection can be challenging. First and foremost development of a flail chest has to be avoided. Further closure should be airtight with acceptable pain and cosmetic results. Various methods for closure of chest wall defects have been described, including prosthetic mesh, musculocutaneous flaps, titanium plates and bone cement [2–4]. Rigid fixation techniques provide good chest wall stability, but too rigid fixation might induce pain and increase the risk for infection.
In this study, we present a case of a 59-year-old woman with a large tumour caused by FD, which was surgically resected with direct reconstruction using a sandwich technique of a mesh reinforced with methyl methacrylate in a double-layer Marlex mesh.
CASE REPORT
A 59-year-old woman presented at the outpatient clinic of the Department of Pulmonology with complaints of chronic cough. Apart from gastroesophageal reflux disease, she had no history of disease. She presented with chronic cough without other pulmonary complaints; specifically, she had no haemoptoe, shortness of breath or weight loss. Pulmonary function tests revealed normal lung function with vital capacity of 4.5 l (130% of predicted), forced expiratory volume in 1s of 3.8 l (130% of predicted) and a diffusing capacity of 105%. On plain X-ray, a mass in the left thoracic wall was found. Previous radiographs obtained from another hospital already revealed the mass in 2005. The mass did not appear to grow on the consecutive X-rays.
Additional imaging was obtained by a chest CT scan, which showed a calcified tumour on the left thoracic wall growing from the second rib with slight impression of the lung with a maximal diameter of 4.7 cm (Fig. 1A). Differential diagnostic consideration included chondroma, FD or low-grade sarcoma. No other lesions in the lung or chest wall were identified.
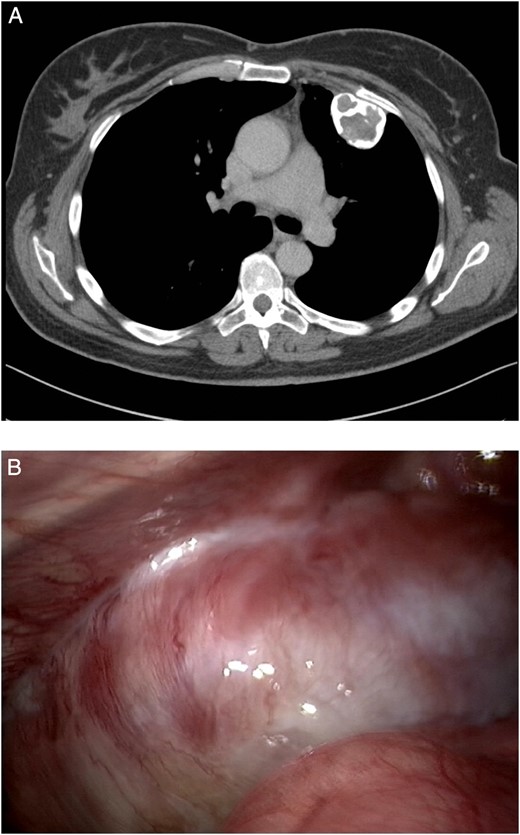
(A) A calcified tumour on the left chest wall growing from the second rib with slight impression of the lung with a maximal diameter of 4.7 cm. (B) Bony tumour originating from the left second and third rib, with some pleural adhesions.
With no other lesions explaining the chronic cough, resection through video-assisted thoracoscopy (VATS) was planned in multidisciplinary consultation. During VATS, a bony tumour was found originating from the left second and third rib, with some pleural adhesions (Fig. 1B). The procedure was converted to thoracotomy to perform wide resection of the thoracic wall (Fig. 2).
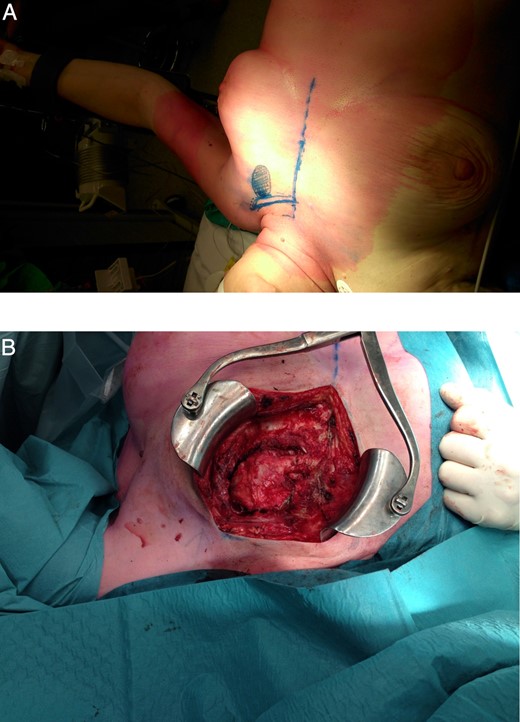
(A) Conversion to thoracotomy. (B) Chest wall defect after resection of the tumour.
The size of the thoracic wall defect following resection measured 8 by 5.5 cm A patch was prepared using two polypropylene meshes and interpolate of methyl methacrylate (Fig. 3). The patch was placed and tightened to the periosteum using prolene sutures (Fig. 4). Figure 5 shows the resected tumour. Finally, subcutaneous tissue and skin were closed in layers using a Vicryl and intracutaneous Monocryl suture.
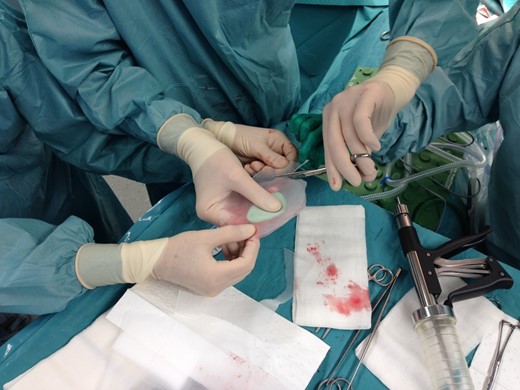
Preparation of the patch with two polypropylene meshes and interpolate of methyl methacrylate.
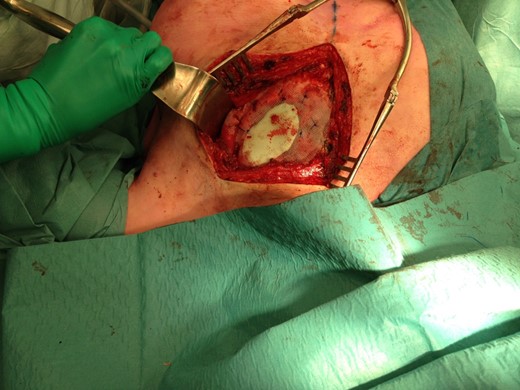
Positioning of the mesh and fixation to the periosteum of adjacent ribs.
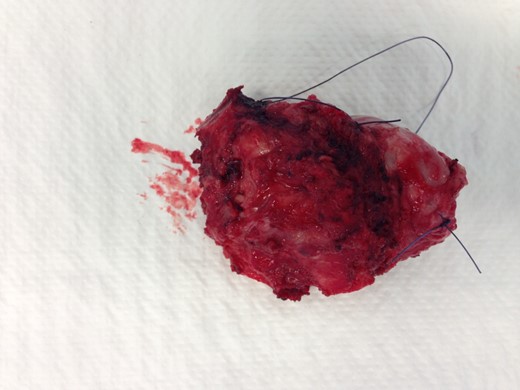
The resected tumour. Marking: short, cranial side; long, lateral side.
Pathology examination of the specimen was performed by an expert bony tumour panel. Definitive pathology of the specimen revealed FD that was radically removed. At follow-up 6 weeks later on the outpatient clinic, the patient was in good health. The wound had healed properly and complaints of chronic cough had stopped.
DISCUSSION
Differential diagnostic considerations for chest wall tumours comprise benign tumours such as osteochondroma, chondroma, FD and malignant tumours such as soft tissue sarcomas, osteosarcoma, Askin tumours or metastasis of the ribs [1]. Surgery of chest wall tumours indicated for confirmatory biopsy, correction of deformities, failure of non-surgical therapy, prevention of pathological changes and eradication of symptomatic lesions [5].
Optimal closure of chest wall defects remains somewhat controversial. In general, chest wall reconstruction is indicated for any chest wall defect greater than 5 cm, although on the posterior side, function might not be impaired with defects up to 10 cm. The methods for chest wall reconstruction can grossly be divided in two groups: rigid fixation (using a sandwhich technique as described here or titanium) and non-rigid fixation (non-rigid mesh or myocutaneous flaps).
The technique of using a polypropylene mesh with methyl methacrylate as described in our case was developed ∼25 years ago [6]. However, this technique has still an important number of benefits. Pulmonary complications are the most important cause of morbidity after chest wall resection and reconstruction. Such complications are better prevented by rigid fixation techniques, as they better prevent paradoxical chest movements [2, 7].
Furthermore, the technique is easy to apply by surgeons who only sporadically encounter large chest wall defects. In contrast to myocutaneous flaps and titanium plates, this technique does not require specific skill or equipment [4, 8, 9]. A further problem with titanium plating is that such osteosynthesis material might eventually break, as no bone healing is expected after large resections of the chest wall. Little is known about the long-term results of plating.
In our case, we achieved excellent functional and cosmetic results with this polypropylene meshes and a methyl methacrylate sandwich technique. In conclusion, FD of the chest wall is a rare condition that can present with chronic cough, pain or respiratory failure. Radical resection of the involved ribs is indicated suspect for malignancy. The use of a sandwich technique—a mesh reinforced with methyl methacrylate cement—can ensure chest wall integrity while preventing a frail chest.
CONFLICT OF INTEREST STATEMENT
None declared.



