-
PDF
- Split View
-
Views
-
Cite
Cite
Richard Lu, Kimberly Brown, Ikenna Okereke, Cologastric strictures: What is the best treatment?, Journal of Surgical Case Reports, Volume 2017, Issue 1, January 2017, rjw229, https://doi.org/10.1093/jscr/rjw229
Close - Share Icon Share
Abstract
A 31-year-old gentleman who had undergone an emergent esophagectomy and reconstruction with a colon interposition graft, presented with a long-standing cologastric stricture. He had undergone multiple attempts at endoscopic dilation over multiple decades with little symptomatic relief. He underwent a resection and reconstruction of the anastomosis entirely through an abdominal approach. He did well from surgery and experienced complete symptomatic relief immediately. Complications of colon interposition grafts can occasionally be treated using an abdominal incision only.
INTRODUCTION
Caustic esophageal injury in infants is a devastating insult to the gastrointestinal tract and will often require major reconstructive surgery to replace the damaged esophagus. Esophageal replacement with colonic interposition has been utilized since Dale and Sherman performed the first retrosternal colonic interposition in 1955 [1]. Up to 80% of patients with colonic interposition develop late complications [2], with as many as 30% requiring reoperation [3]. Late complications include anastomotic strictures and graft redundancy. Risk factors for developing anastomotic strictures are perioperative ischemia and anastomotic leak [4]. Endoscopic dilation is relatively safe and effective for the initial treatment of anastomotic strictures, but surgical management is indicated in refractory cases. When surgery is required, graft revision utilizing both a thoracotomy and laparotomy is common. We report a case of cologastric stricture treated with resection and reconstruction of the anastomosis solely through an abdominal approach, which can offer less morbidity and mortality.
CASE REPORT
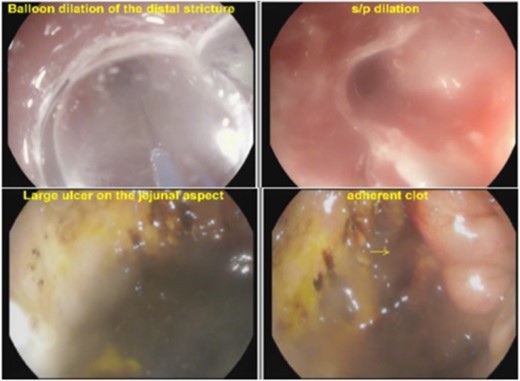
Endoscopic images of cologastric stricture before and after balloon dilation. Ulcerative disease is seen at the jejunal aspect of the patient's gastrojejunostomy.
Endoscopic evaluation revealed the severe cologastric stricture, severe inflammation just proximal to the cologastric anastomosis, and significant ulcerative disease at his gastrojejunal anastomosis. There was retained food in his stomach suggestive of gastroparesis. Multiple attempts to dilate the cologastric stricture were unsuccessful.
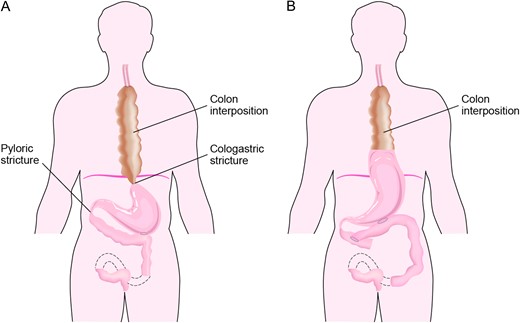
Preoperative cologastric and pyloric strictures (A) and post-operative changes including new cologastric, gastrojejunal, duodenojejunal anastomoses (B).
The patient tolerated the procedure well and was transferred to the intensive care unit. On post-operative Day 2, he was transferred to the floor. His post-operative course was remarkable for development of an intra-abdominal fluid collection, which required percutaneous drainage, but was otherwise uncomplicated. He was discharged to home on a regular diet.
DISCUSSION
Caustic injury of the esophagus is a devastating injury that can have lifelong sequelae. Eighty percent of ingestion injuries worldwide occur in children [5]. Severe esophageal damage may require resection with creation of a neo-esophagus. Because these operations occur in children, complications in regards to the colonic interposition graft may arise over the period of decades.
Endoscopic dilation is a common treatment modality in the management of strictures. Our patient had recurrent symptoms despite multiple endoscopic interventions. Classically, a transthoracic approach has been used to resect the entire colonic graft. In this situation, a repeat colon graft may be needed, which carries high morbidity and mortality. Our transabdominal approach is novel but offers some advantages. In particular, the majority of the proximal colon graft, which was functional, was able to be spared. Morbidity was reduced in our patient without thoracotomy. Given our patient's preoperative nutritional status, he would be at a predisposed risk for wound healing complications. Via transabdominal approach, the cologastric anastomotic stricture was able to be resected and reconstructed. To the best of our knowledge, this is the first written report of using a completely transabdominal approach for revision of the colonic graft. Our patient had previously been refused surgery by multiple surgeons. If this relatively less complex surgical management was used, perhaps he would have had definitive treatment much earlier.
Our patient did well with our transabdominal approach given the chronicity of his symptoms. In light of his clinical dilemma of continued non-operative versus operative intervention, his symptoms were relieved immediately. This surgical approach should be considered in patients with history of colonic interposition requiring reoperation for complications of the colonic graft.



