-
PDF
- Split View
-
Views
-
Cite
Cite
Moatasem H Al-janabi, Tariq Khaddour, Rabab Salloum, Papillary thyroid carcinoma arising from a mature ovarian teratoma coexisting with stromal luteoma: the first case report in the literature, Journal of Surgical Case Reports, Volume 2023, Issue 5, May 2023, rjad285, https://doi.org/10.1093/jscr/rjad285
Close - Share Icon Share
Abstract
Mature cystic teratomas are the most common ovarian tumors in women of reproductive age. The malignant transformation of mature cystic teratomas is a rare entity. The most common malignant tumor in mature cystic teratomas is squamous cell carcinoma, whereas papillary thyroid carcinoma is an exceptional event. On the other hand, stromal luteoma is an uncommon benign steroid cell tumor of the ovary that occurs mostly in postmenopausal females. The coexistence of different ovarian tumor subtypes is an extremely rare pathological event. In this report, we describe a case of papillary thyroid carcinoma arising in mature cystic teratomas coexisting with stromal luteoma. To the best of our knowledge, this is the first report in English literature. Both mature cystic teratoma (with papillary thyroid carcinoma) and stromal luteoma are very rare entities. Pathologists should be aware of malignant transformation and exclude it when investigating mature cystic teratomas, especially in older patients.
INTRODUCTION
Mature cystic teratoma (MCT) is the most common type of ovarian germ cell tumor, accounting for approximately 20% of all ovarian tumors [1, 2]. Malignant transformation in MCT is very rare, varying from 1 to 3%, according to the literature [1]. MCT with malignant transformation is mainly found in postmenopausal women [1, 2]. The most common malignant tumor in MCT is squamous cell carcinoma [1–3]. Other types of malignancy, like adenocarcinomas, malignant melanomas, basal cell carcinomas, carcinoid tumors, and thyroid carcinomas, are less common [2, 3]. Moreover, papillary thyroid carcinoma arising within mature cystic teratomas is exceedingly rare [1–3]. However, stromal luteoma is a very rare ovarian tumor that occurs mainly in postmenopausal females [4]. The coexistence of different ovarian tumor subtypes is a very rare pathological entity [5]. In this paper, we report the first case in the literature of a 48-year-old female with a papillary thyroid carcinoma arising within a mature cystic ovarian teratoma in the right ovary coexisting with a stromal luteoma in the left ovary.
CASE PRESENTATION
A 48-year-old peri-menopausal female, gravida 4, para 4, all deliveries were by lower segment cesarean sections, presented to the gynecology clinic with the complaint of abdominal pain from the last six months. There was no known history of tumors, particularly gynecological malignancies, in her family. The patient smoked eight cigarettes per day. Routine laboratory tests were within normal limits. Tumor marker CA 125 was 24.4 U/mL (normal range of 0–35 U/mL). Physical examination revealed a palpable abdominal mass with pain in the right iliac fossa. Abdominal ultrasound showed a large, solid cystic mass measuring 8.6 cm × 9.1 cm in size in the right adnexal region (Fig. 1). No abnormal findings were observed in the left ovary. The patient underwent a subtotal abdominal hysterectomy with bilateral salpingo-oophorectomy. The specimen was sent for histopathological evaluation. A gross examination of the right adnexal mass revealed a large cystic teratoma measuring 9.5 cm × 9 cm × 7.5 cm and weighing 307.5 g, filled with hair shafts, greasy brown material, and teeth. The capsule was smooth and intact. Furthermore, a well-defined nodule, measuring 4 cm × 3 cm × 2 cm, was adherent to the teratoma (Fig. 2A). On cross-section, the nodule cut surface was tan with a glairy meaty appearance, and multiple small cysts containing yellow gelatinous material were seen (Fig. 2B). The macroscopic examination of the left ovary specimen showed a small, solid yellow nodular lesion, about 1 cm in maximum dimension, with clear borders (Fig. 2C). The microscopic examination of the teratoma showed a wall lined by stratified squamous epithelium with mature skin appendages (hair follicles and sebaceous glands) (Fig. 3A). Hematoxylin- and eosin-stained sections of the nodule revealed remnants of the ovarian cortex with residual thyroid tissue (Fig. 3B). Well-developed papillae with epithelium composed of cuboidal cells were observed (Fig. 3C). The nuclei have an ovoid, crowded with ground glass (‘Orphan Annie’ eye) appearance. Pseudo-inclusions and nuclear grooves were also present (Fig. 3D). Histological evaluation of the small nodule in the left ovary showed nests and islands of polygonal cells with abundant eosinophilic granular cytoplasm and small, rounded, centrally placed nuclei, surrounded by ovarian stroma (Fig. 4A–C). The mitotic figures were rare. Immunohistochemical stains showed markedly positive staining for inhibin (Fig. 4D). The final diagnosis was papillary thyroid carcinoma arising within a mature cystic ovarian teratoma in the right ovary, coexisting with a stromal luteoma in the left ovary. The malignant tumor was confined to the ovary and has an excellent prognosis. An abdominal and pelvic computed tomography scan was performed, and no regional lymph nodes had metastases. The patient had a stable recovery, and she was discharged a few days after the surgery.
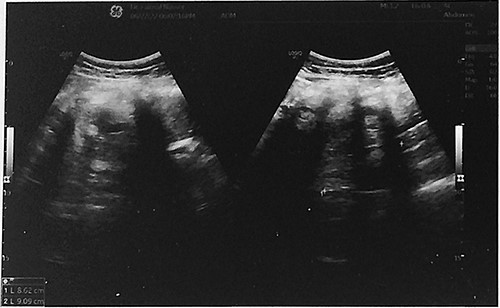
Abdominal ultrasound showed a large solid cystic mass measuring 8.6 cm × 9.1 cm in size in the right adnexal region.
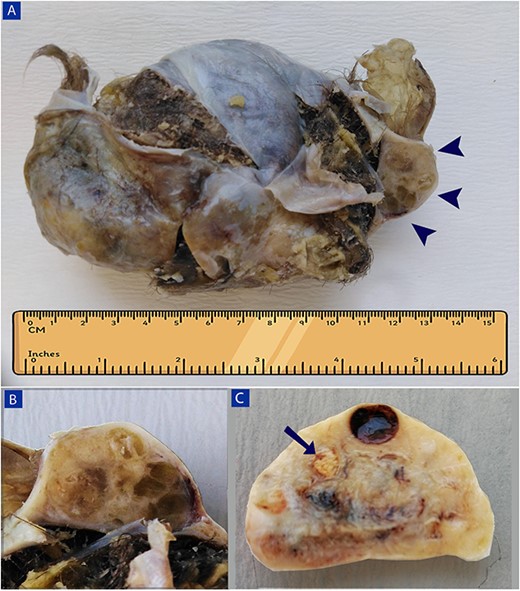
A gross image of the right adnexal mass (A and B) and left ovary (C). (A) A large cystic teratoma, filled with hair shafts and greasy brown material, with a well-defined nodule measuring 4 cm × 3 cm × 2 cm, is adherent to the teratoma (arrowheads). (B) The nodule’s cut surface is tan with a glairy meaty appearance, and multiple small cysts containing yellow gelatinous material are seen. (C) A small solid yellow nodular lesion, about 1 cm in maximum dimension with clear borders, is noted in the left ovary (arrow).
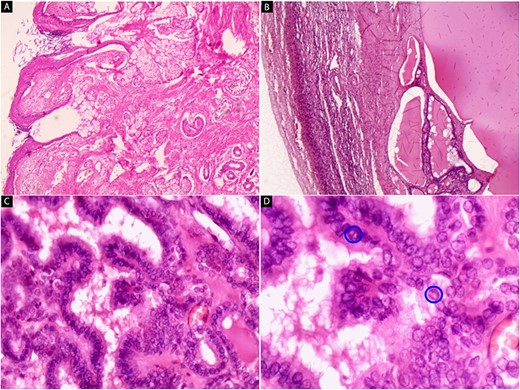
Hematoxylin and eosin stain (A–D). Microscopic images of the right adnexal mass. (A) Cyst wall lined by stratified squamous epithelium with mature skin appendages (hair follicles and sebaceous glands) and loose keratin flakes in the lumen (x40). (B) The ovarian cortex is on the left side of the image with residual thyroid tissue on the right side (x40). (C) Well-developed papillae with epithelium composed of cuboidal cells are present (x200). (D) The nuclei are ovoid, crowded with ground glass appearance (‘Orphan Annie’ eye), and have grooves (blue circles) (x400).
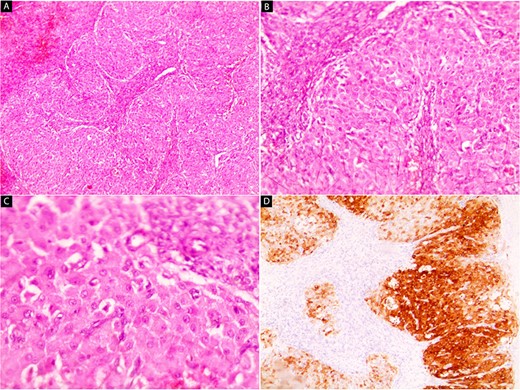
Hematoxylin and eosin stain (A–C) and IHC (D). Microscopic images of the left ovary. (A and B) Nests and islands of polygonal cells with abundant eosinophilic granular cytoplasm surrounded by ovarian stroma (x40 and x100) (C) Small, rounded, centrally placed nuclei are seen (x200). (D) Tumor cells are markedly positive for inhibin (x100).
DISCUSSION
Mature cystic teratoma is the most common type of ovarian germ cell tumor. It is mainly found in women between 20 and 50 years of age; only about 20% are detected in postmenopausal women [1, 6]. The incidence of malignant transformation in MCT is rarely reported and represents only 1–3% of benign cystic teratomas [1, 2, 6]. The presence of thyroid tissue in the ovaries was first described by Von Kahlden in 1895 [3]. The most common thyroid-type carcinoma that occurs in MCT is papillary carcinoma, followed by follicular carcinoma [2, 3, 6]. Many patients are asymptomatic, and the tumors are discovered on routine examination. Symptoms such as pelvic discomfort or abdominal pain occur when the tumor reaches a large size, as in our case [1, 3, 6]. Most thyroid carcinoma cases in mature teratoma are diagnosed postoperatively through histological sections [1, 7]. However, papillary thyroid cancer has characteristic nuclear features like ground-glass nuclei, nuclear pseudo inclusions, and grooves [3]. The optimal treatment of thyroid carcinoma arising within MCT is uncertain due to the rarity of the disease [2, 3]. The treatment varies and depends on the age of the patient and the presence of metastases [1, 3, 8]. For women of a reproductive age, if there is no capsular invasion or metastasis, cystectomy or unilateral salpingo-oophorectomy is recommended, whereas for postmenopausal women, hysterectomy and bilateral salpingo-oophorectomy are indicated [1, 3, 8, 9]. The prognosis of early-stage thyroid carcinoma in mature ovarian teratomas is excellent following treatment [8], as in this case. On the other hand, stromal luteoma is a very rare tumor of the ovary that constitutes about 25% of all steroid cell tumors. It is always benign and often seen in postmenopausal females [4, 10]. Usually, it is without symptoms, but it may present with vaginal bleeding [4, 10]. Histopathologically, a luteoma may simulate the Leydig cell tumor, which is seen in the ovarian hilus and contains steroid cells that include Reinke crystalloids, in contrast to luteoma, which is centered in the ovarian stroma [4]. Pregnancy luteoma can be identical to stromal luteoma, but the history of pregnancy can help in the diagnosis of the former. Luteoma is often discovered incidentally at the time of a cesarean section or other surgery for unrelated reasons [4, 10], like in our case.
CONCLUSION
Both the malignant transformation of mature cystic ovarian teratoma, particularly thyroid carcinoma, and stromal luteoma are very rare entities. The diagnosis in most cases is incidental. Pathologists should be aware of malignant transformation and exclude it when investigating mature cystic teratomas, especially in older patients.
CONFLICT OF INTEREST STATEMENT
The authors have no conflicts of interest to declare.
FUNDING
None.
ETHICAL APPROVAL
No ethical approval is required for this case report.
CONSENT
Written consent was obtained.
GUARANTOR
Moatasem Hussein Al-janabi.



