-
PDF
- Split View
-
Views
-
Cite
Cite
Akiko Hida, Akira Shimomura, Adult Bochdalek hernia incarcerated after laparoscopic nephrectomy: a case report, Journal of Surgical Case Reports, Volume 2026, Issue 4, April 2026, rjag252, https://doi.org/10.1093/jscr/rjag252
Close - Share Icon Share
Abstract
Adult Bochdalek hernia (BH) is rare and often asymptomatic, but it can occasionally lead to life-threatening complications such as bowel obstruction or strangulation. Latent BHs may become clinically apparent following abdominal surgery, possibly due to increased intra-abdominal pressure or postoperative anatomical changes. We report the case of an 81-year-old man who developed an incarcerated left-sided BH after laparoscopic nephrectomy for upper tract urothelial carcinoma. The patient presented with acute bowel obstruction caused by herniation of the transverse colon into the thoracic cavity and required emergency surgery. This case highlights the potential for asymptomatic BHs to progress after minimally invasive surgery and raises the question of whether elective repair should be considered in selected high-risk adult patients. This emphasizes the importance of early recognition.
Introduction
Bochdalek hernia (BH) is a congenital diaphragmatic defect that is typically diagnosed in neonates and infants. Adult BH is rare and often detected incidentally during imaging performed for unrelated reasons. However, adult cases can occasionally present with acute complications, including bowel obstruction, strangulation, and necrosis, which may be life-threatening [1, 2]. Therefore, once the diagnosis is established, surgical repair is often considered, even in asymptomatic patients.
Recent case reports have suggested that latent BHs in adults may become clinically apparent or incarcerated following abdominal surgery [3]. Increased intra-abdominal pressure, postoperative anatomical changes, or iatrogenic factors may precipitate herniation of abdominal organs through a previously silent diaphragmatic defect. We report a case of incarcerated adult BH that developed after laparoscopic nephrectomy, highlighting the potential risk of progression in asymptomatic cases and the importance of considering prophylactic surgical repair.
Case presentation
An 81-year-old man presented to our clinic with epigastric pain and nausea lasting 2 days. His medical history was significant for bladder stone surgery, left inguinal hernia repair, right hip surgery, prostate cancer, ascending colon cancer, chronic kidney disease, hypertension, and a laparoscopic left nephrectomy for upper tract urothelial carcinoma performed 5 years prior to the current presentation. Initial abdominal computed tomography (CT) showed no evidence of bowel obstruction, and the patient was discharged home. However, the following morning, he developed worsening nausea and vomiting and revisited our clinic. Abdominal radiography revealed air–fluid levels in the small intestine and intrathoracic bowel gas in the left lower lung field. Repeat abdominal CT demonstrated herniation of the transverse colon into the left thoracic cavity (Fig. 1). He was urgently referred to a critical care medical center with suspected obstructive ileus.
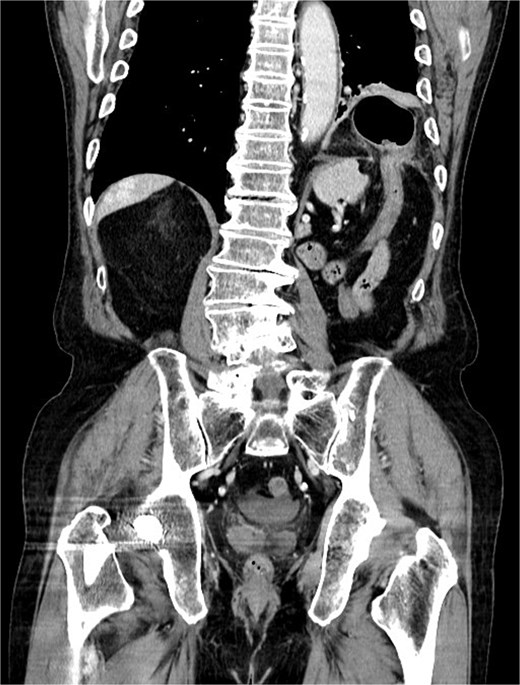
Coronal contrast-enhanced computed tomography image demonstrating a left-sided diaphragmatic defect with herniation of the transverse colon into the left thoracic cavity. No radiological signs of bowel strangulation were observed.
Contrast-enhanced CT revealed herniation of the transverse colon through a left posterolateral diaphragmatic defect, consistent with an incarcerated BH. Emergency laparotomy was performed via a transabdominal approach. Intraoperatively, a left-sided diaphragmatic defect was identified on the anterior surface of the spleen, through which the transverse colon at the splenic flexure and the greater omentum were herniated and incarcerated. The initial defect measured approximately 25 × 25 mm. However, to allow safe reduction and adequate assessment of the incarcerated contents, the defect was intentionally enlarged to approximately 70 × 60 mm. Partial discoloration of the herniated omentum was observed, and the affected portion was resected. The transverse colon was adherent but showed no evidence of perforation. Although a small amount of ascites was present, there were no signs of intra-abdominal contamination. The diaphragmatic tissue surrounding the defect appeared healthy and without fragility, therefore, primary closure was achieved using interrupted sutures. Mesh reinforcement was not applied, as tension-free closure was possible and no tissue weakness was observed. The postoperative course was uneventful, and the patient was discharged on postoperative day 9.
Discussion
BH is caused by failure of closure of the posterolateral foramen of the diaphragm during embryonic development. While it is commonly diagnosed in neonates with respiratory distress, adult presentations are rare. CT-based studies report that the incidence of incidental adult BH ranges from 0.17% to 6% among adults undergoing chest or abdominal CT [4, 5]. Most adult BHs are asymptomatic and detected incidentally; however, incarceration and strangulation requiring emergency surgery are also reported [6]. A review of reported adult BH cases showed that a substantial proportion of patients presented with incarceration or acute symptoms, suggesting that incarceration is not uncommon in adults [7]. These reports suggest that even asymptomatic BHs can progress to life-threatening conditions. Several factors have been proposed as triggers for the progression or incarceration of latent BHs in adults. Iatrogenic factors, including abdominal surgery and increased intra-abdominal pressure, may play an important role. In particular, laparoscopic surgery involves pneumoperitoneum, which can elevate intra-abdominal pressure and potentially unmask congenital diaphragmatic defects.
A unique aspect of this case is the possible association between laparoscopic nephrectomy for upper tract urothelial carcinoma and the subsequent development of incarcerated BH. The patient had no prior diagnosis of diaphragmatic hernia, and CT images obtained before the nephrectomy showed no evidence of herniation. Retrospective review of the preoperative CT images with attention to the diaphragm revealed no diaphragmatic defect. It is plausible that pneumoperitoneum during laparoscopic surgery or postoperative anatomical changes weakened tissue support around a latent diaphragmatic defect, leading to herniation. Previous reports have suggested that CO₂ pneumoperitoneum may allow gas passage through congenital diaphragmatic weak points. The resulting increase in intra-abdominal pressure may unmask latent diaphragmatic defects [8, 9]. A similar case of post-nephrectomy BH has been reported, supporting the concept of iatrogenic progression of latent diaphragmatic defects [3].
Currently, there is no consensus regarding prophylactic surgery for asymptomatic adult BH. However, given the risk of sudden incarceration, strangulation, and bowel necrosis, early surgical intervention may be considered in selected high-risk patients, particularly those undergoing abdominal surgery or with conditions associated with increased intra-abdominal pressure. Previous studies suggest that emergent repair for incarcerated BH is associated with higher morbidity and mortality than elective repair, supporting early intervention in selected cases [6]. This case highlights the importance of considering latent BH as a differential diagnosis in postoperative patients presenting with symptoms of bowel obstruction. Although these defects are often asymptomatic, their potential for progression should not be underestimated.
Acknowledgements
The authors would like to thank the medical and nursing staff involved in the care of this patient.
Conflict of interest
The authors declare no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethical approval
Ethical approval was not required for this case report in accordance with institutional policy.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images.



