-
PDF
- Split View
-
Views
-
Cite
Cite
Andrej Nikolovski, Kristina Mickovska, Ivan Argirov, Lidija Maznevska, Perforated giant peptic ulcer of the stomach in a female patient with multiple sclerosis, Journal of Surgical Case Reports, Volume 2024, Issue 7, July 2024, rjae466, https://doi.org/10.1093/jscr/rjae466
Close - Share Icon Share
Abstract
Giant peptic ulcer of the stomach is defined with a diameter of more than 3 cm. About 2/3 of them are benign peptic ulcers and perforate in 1%–2% of all peptic ulcer stomach perforations. High rates of postoperative morbidity and mortality are reported. The treatment options include omental patch repair, jejunal serosal patch repair, duodenal exclusion, and gastric resection. Postoperative omental patch repair failure is reported and is strongly associated with the ulcer diameter. This case reports a giant peptic stomach ulcer perforation in a female patient treated successfully with omental patch repair, according to Cellan–Jones.
Introduction
Giant peptic stomach ulcer (GPSU) is defined when the diameter of the ulcer is equal to or greater than 3 cm [1]. More than 1/3 of the stomach giant ulcers are described to be malignant (37.8%), and the rest have a benign peptic nature [2]. Stomach ulcers may penetrate some of the adjacent organs, or a free perforation can occur, thus resulting in diffuse peritonitis, clinically presented with an acute abdomen [3]. Out of the total number of stomach ulcer perforations, ~1%–2% are perforated large/giant ulcers. The post-perforation morbidity and mortality rates are reported to be significant (20%–70% and 15%–40%, respectively). The high rates of mortality are reported to be directly associated with the perforated ulcer diameter [4]. Different surgical options are described in the treatment of the perforated GPSU, starting with omental patch repair (omentopexy), jejunal serosal patch repair, duodenal exclusion with gastro-jejunostomy, and partial gastric resection [4, 5]. We present a case of a perforated giant pre-pyloric stomach ulcer in a female patient with previously diagnosed multiple sclerosis treated with open omental patch repair, according to Cellan–Jones. Written informed consent was obtained from the patient.
Case report
A 42-year-old woman presented in the emergency department due to abundant vomiting, nausea, and intense stomach pain. Vomiting was present for several days at the start following food or liquid consumption. The vomit was described as dark colored, and the stomach pain was mild until the admission day, when it became increasingly heavy.
In her recent medical history, the patient has complained of urinary and stool incontinence for five months. The patient was diagnosed with multiple sclerosis in 2015. Regular immunomodulatory therapy was prescribed. Additionally, oral metamizole sodium and diazepam were prescribed as needed, but frequently. The patient was an active cigarette smoker (20 cigarettes per day).
Physical examination revealed clinical signs of an acute abdomen with a rigid abdomen with diffuse abdominal wall tenderness. Laboratory blood analysis, an abdominal computed tomography (CT) scan, and a chest X-ray were performed after admission. The following laboratory findings were abnormal: hemoglobin level of 91.00 g/L (120.00–165.00 g/L); leukocytes count of 23.40 109/L (3.50–10.00 X109/L); neutrophil count of 21.40109/L (1.20–8.00 x109/L); platelets count of 1089.00109/L (150.00–390.00109/L); serum urea value of 9.40 mmol/L (2.10–8.20 mmol/L); total serum protein value of 57.30 g/L (64.00–83.00 g/L); serum albumin level of 30.00 g/L (35.00–50.00 g/L); C reactive protein level of 287.20 mg/L (0.00–5.00 mg/L). A CT scan revealed large air pockets in the abdomen and pneumoperitoneum presence. Free fluid with a density of up to 15 Hounsfield units was observed in all spaces of the abdomen. A defect on the anterior gastric wall was seen (Fig. 1). According to the findings suggestive of a hollow intraabdominal viscus perforation, an emergency laparotomy was undertaken. The calculated risk and predicted survival according to Boey’s score [6] of the patient were 2, with a calculated morbidity risk of 75% and a mortality risk of 33%.
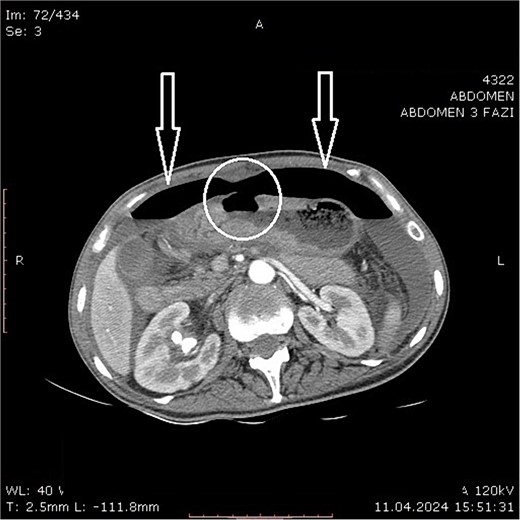
Abdominal computer tomography (axial scan) with pneumoperitoneum (arrows) and visible discontinuity of the anterior stomach wall suggestive of ulcer perforation (encircled).
Intraoperatively, a giant ulcer in the antropyloric region of the stomach adhered to the round ligament was noted (Fig. 2), accompanied by diffuse fibrinous peritonitis. The ulcer was detached from the anterior abdominal wall, and the diameter was measured to be 4 × 3.5 cm (Fig. 3). A biopsy of the ulcer was taken. A thorough intraabdominal lavage with warm saline was conducted. The ulcer was treated with omental patch ulcer closure according to Cellan–Jones [7] by the use of six slowly absorbable sutures. Two intraabdominal drains were placed in the Morisons’s space and Douglas’s pouch, respectively.
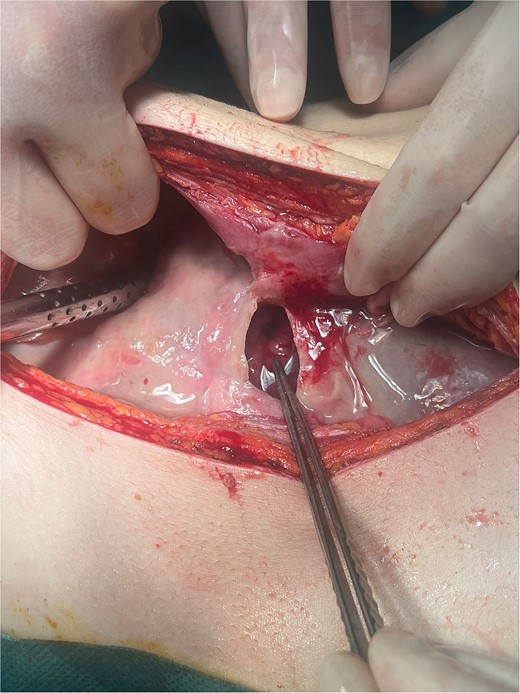
Giant ulcer of the anterior wall of the stomach adhered to the round ligament (intraoperative finding during laparotomy).
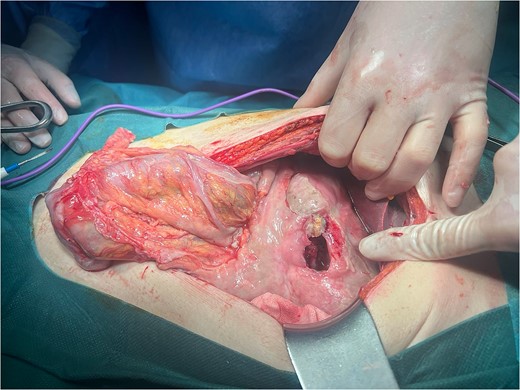
The postoperative period was uneventful. Liquid oral intake began on postoperative Day 4. The length of hospital stay was 10 days. The biopsy results excluded ulcer malignancy.
Discussion
GPSUs are defined according to their diameter size, which exceeds 3 cm [8]. The prevalence of GPSU is ~0.5% [9]. The reported risk factors for giant peptic ulcer occurrence are certain drugs used, such as non-steroidal anti-inflammatory drugs, methylprednisolone, cyclosporine, and mycophenolate mofetil, medications given to solid organ-transplant patients [3, 9, 10]. In this report, the patient did not report the use of known ulcerogenic drugs.
Peptic ulcer perforations occur in 10%–20% of all peptic ulcer complications, whereas large and giant peptic ulcers perforate in ~1%–2% of the cases [4].
The diagnosis of a perforated peptic ulcer begins with a physical exam. If the patient presents with clinical signs of acute abdomen due to diffuse peritonitis accompanied by shock, an indication for exploratory laparotomy/laparoscopy may be established. In cases with a contained intraabdominal leak, signs of peritonitis may be absent or minimal, and additional diagnostic tools are needed. An upright chest X-ray with free air under the diaphragm reveals hollow viscus perforation, but it is not always present. In such cases, intravenous contrast-enhanced abdominal computerized tomography is indicated. In negative findings, a water-soluble oral contrast is suggested [11].
Although non-operative management in strictly selected patients is reported, if signs of peritonitis accompanied by pneumoperitoneum are present, surgery is recommended. The use of a minimally invasive approach (laparoscopic) is recommended in stable patients with a perforation diameter of <5 mm and the proper surgical skills. Otherwise, open surgery should be preferred [11].
The reported procedures for GPUS comprehend omental patch repair, omental plugging, jejunal serosal patching, pyloric exclusion with gastro-jejunostomy, and gastric resection (with or without additional vagotomy) [4, 5]. The omental patch repair is considered to be the ‘gold standard’.
Overall postoperative morbidity in patients treated for GPUS is high and reported to be between 9.6% and 73.3% [4, 5, 12]. The reported mortality rate in the series of Kosenkov et al. [12] for the patients operated on for giant stomach ulcer perforation was 10%, and it was a consequence of suture failure. In the series of Chan et al. [5] with 110 patients with peptic ulcer perforation (ulcer diameter ≥ 20 mm), the all-cause mortality rates for the omental patch repair group and the gastrectomy group were 17.3% and 20.7%, respectively. In the series of Khalifa et al., the groups treated with jejunal serosal patching and gastric resection had a mortality rate of 6.6% (each), and in the omental plugging group, no mortality was reported [4].
Giant ulcer perforation presents as a surgical urgency with the need for an emergent laparotomy. Ulcer size measurement is done intraoperatively, and so is its definition of being giant [4].
Omental patch repair failure (leakage) is a well-described early postoperative complication of sutured peptic ulcer perforation. In the retrospective analysis of Maghsoudi and Ghaffari conducted on 422 patients with duodenal and stomach ulcer perforation, the reported rate of omental patch leak accompanied by generalized peritonitis was 4%. The options for leak treatment in this study comprehended subhepatic drainage and abdominal cavity irrigation, reinsertion of the omental patch accompanied by subhepatic drainage, jejunal serosal patch and drainage, and abdominal cavity irrigation. The mortality rate in these patients was 29.4%. Factors associated with mortality were age over 65, delayed surgery (delay more than 24 h), and the size of perforations [13].
The outcome of leaked repair and its associated factors following omentopexy for perforated peptic ulcer disease was analyzed in the retrospective multicenter cross-sectional study of Ogbuanya et al. The authors report a leak rate of 11.7%. Relaparotomy was performed in 92.9% of them. The surgical techniques/procedures employed to manage leaked repairs were jejunal serosal patch, proximal gastrojejunostomy, modified Graham’s patch, falciform ligament patch, and cholecystoduodenoplasty. Sealing of the leak occurred in 71.4% of cases. In the rest (28.6%), a 50% mortality rate was reported. The procedure with the highest success for leaked repair was the jejunal serosal patch. Factors significantly associated with a leaked repair after omental patch repair were immunosuppression/steroid therapy, the large diameter of the perforated ulcer, delayed presentation, sepsis, and perioperative shock [14].
Conclusion
The treatment of perforated giant peptic ulcers of the stomach is a challenging emergency surgical procedure due to the expected technical difficulties and the high rates of postoperative morbidity and mortality. The choice of surgical procedure should be individualized for each patient depending on their current condition and the local intraabdominal findings. In patients with poor conditions and delayed diagnosis, a simple omental patch repair should be attempted since the severity of the developed peritonitis may preclude a safe extensive procedure, such as partial gastric resection. In the presented case, the omental patch repair, according to Cellan–Jones, resulted in a successful treatment of the perforated GPSU.
Conflict of interest statement
None declared.
Funding
None declared.



