-
PDF
- Split View
-
Views
-
Cite
Cite
Surendar Jatoth, Tarun K Suvvari, Shashank J, Aiman P Afsar, Shivani Ravipati, Lakshmi S Mukkamala, Vimal Thomas, Unveiling the mystery of sigmoid volvulus with multiple adhesions—an unusual case report, Journal of Surgical Case Reports, Volume 2023, Issue 7, July 2023, rjad391, https://doi.org/10.1093/jscr/rjad391
Close - Share Icon Share
Abstract
Intestinal obstruction is a common surgical emergency that requires prompt intervention. We present a case report of a 30-year-old male with recurrent intestinal obstruction due to sigmoid volvulus. Our case highlights the challenges associated with managing recurrent intestinal obstructions caused by adhesions following surgical interventions for sigmoid volvulus. It emphasizes the need for careful evaluation and meticulous surgical techniques to minimize the risk of adhesion formation and subsequent complications.
INTRODUCTION
Intestinal obstruction is a common surgical emergency that necessitates immediate intervention. Among the numerous etiological factors that can lead to intestinal obstruction, sigmoid volvulus (characterized by the twisting of the sigmoid colon) is a widely recognized cause [1]. However, the development of multiple adhesions shortly after the initial surgery, leading to recurrent symptoms, is an uncommon and intriguing occurrence. Sigmoid volvulus occurs when the sigmoid colon rotates around its mesentery, resulting in a closed-loop obstruction [2]. It is typically associated with risk factors such as chronic constipation, megacolon and anatomical abnormalities. Prompt diagnosis and surgical intervention are vital to relieve the obstruction and prevent potential complications, including ischemia, perforation or peritonitis [3].
In this case report, we present the remarkable case of a 30-year-old male patient who experienced recurrent episodes of intestinal obstruction due to sigmoid volvulus. By presenting this unique case, we aim to provide insights into the potential consequences of suboptimal management and underscore the importance of meticulous approaches to minimize adhesion formation and prevent symptom recurrence.
CASE PRESENTATION
A 30 year-old-male presented to emergency department with severe abdominal pain. The patient reported tenderness in the abdominal region, accompanied by bloating, gas, and two episodes of vomiting. The patient underwent sigmoidopexy surgery for sigmoid volvulus at a regional healthcare centre 3 months ago. However, following the surgery, the patient experienced changes in bowel habits, including both diarrhea and constipation. On examination, the patient had a slightly tense abdomen but did not display any other signs of acute obstruction such as abdominal distension, muscle rigidity or guarding. Initially, conservative treatment was provided for 48 hours, but the symptoms did not improve.
A computed tomography (CT) scan of the abdomen revealed moderate dilation of the proximal and mid- to small bowel loops, with a transition point in the pelvic ileal loop, indicating small bowel obstruction and gall bladder distension. Immediately Elective Sigmoidectomy was performed, and the patient had an uncomplicated postoperative recovery lasting for 25 days. However, the patient subsequently presented to the emergency department with symptoms of acute obstruction. The erect abdominal X-ray reveals air-fluid levels, indicating the presence of fluid and air accumulation in the proximal large bowel and terminal ileum (Fig. 1). Following a thorough evaluation, the patient underwent an exploratory laparotomy. Intraoperatively, multiple adhesions between the loops of the bowel and identified a thick band at the terminal ileum (Fig. 2). Adhesiolysis (surgical removal of adhesions) was performed, and the patient experienced a smooth recovery without any complications till date. The patient’s prior surgical history of sigmoidopexy and sigmoidectomy is relevant to understanding multiple adhesions and subsequent occurrences of sigmoid volvulus.
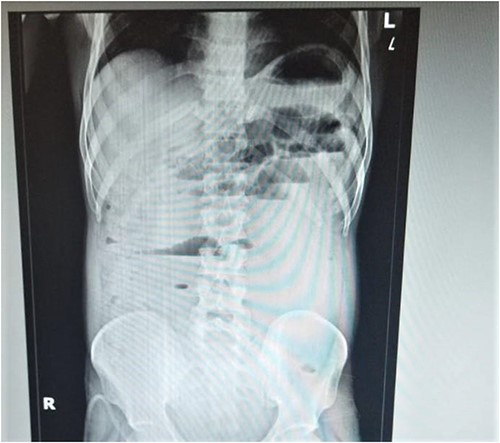
The erect abdominal X-ray reveals air-fluid levels, indicating the presence of fluid and air accumulation in the proximal large bowel and terminal ileum.
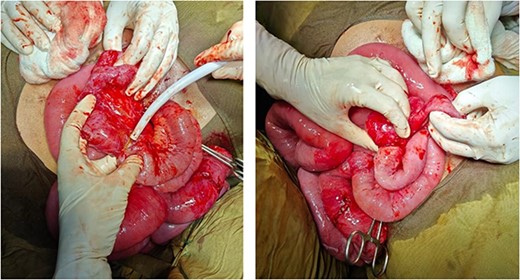
Adhesions from constriction ring at the level of terminal ileum causing intestinal obstruction.
DISCUSSION
Sigmoid volvulus accounts for approximately 8% of all cases of intestinal obstructions, predominantly occurs in individuals aged between their third and seventh decades of life. Elderly males, African Americans, individuals with chronic constipation, and those with associated neuropsychiatric disorders, are at an increased risk of developing sigmoid volvulus [3]. Another significant cause of intestinal obstruction is postoperative fibrosis or adhesion formation. If left untreated, intestinal obstruction can lead to severe and potentially life-threatening complications, including tissue necrosis, perforation and infection [1, 3]. Studies have reported postoperative complications, such as recurrence, in 23% of patients who underwent sigmoidopexy alone, and anastomotic leaks in 15.4% of patients who underwent sigmoidopexy [4]. Additionally, wound infections were observed in 23% of patients who underwent sigmoidopexy and 15.4% of patients who underwent sigmoidectomy [4].
Post-operative adhesions account for approximately 60% of all cases of small bowel obstructions [5]. Open abdominal surgeries are associated with a higher risk of adhesion formation compared to laparoscopic procedures, with adhesions occurring in about 9 out of 10 patients [6–8]. Likewise, it is worth mentioning that the patient in our case developed adhesions following an open sigmoidectomy. In our case, the patient was initially diagnosed with sigmoid volvulus, and sigmoidopexy was considered a beneficial treatment option due to its relative minimally invasive nature, safety and simplicity. However, the recurrence of sigmoid volvulus necessitated additional surgery, limiting the patient’s options and increasing the risk of complications such as anastomotic leaks, peritonitis, wound infections, small bowel obstruction, postoperative bleeding and urinary tract injuries [4, 9]. Various methods can be employed to prevent these complications, including hydroflotation, chemical compounds (such as icodextrin 4% or ferrous hyaluronate 0.5%), mechanical barriers like hyaluronic acid or carboxymethyl cellulose, and experimental approaches like chlorine dioxide [10]. While there are several studies focusing on the development of small bowel obstruction resulting from adhesions, limited attention has been given to the timing of this progression. Typically, adhesions take weeks, months or even years to progress to the point of causing obstruction [11]. However, in our case, small intestinal obstruction occurred within just 3 weeks, which is a rare phenomenon deserving further investigation as a significant finding.
The development of multiple adhesions following sigmoidopexy and subsequent sigmoidectomy emphasizes the risk of adhesion formation after surgical interventions for sigmoid volvulus. Timely diagnosis, appropriate surgical intervention and consideration of preventive measures against adhesions are essential for improving patient outcomes.
CONCLUSION
In conclusion, this case highlights the challenges associated with managing recurrent intestinal obstructions caused by adhesions following surgical interventions for sigmoid volvulus. It emphasizes the need for careful evaluation and meticulous surgical techniques to minimize the risk of adhesion formation and subsequent complications. Further research is warranted to explore the timing and progression of adhesions leading to obstruction in these cases.
ACKNOWLEDGEMENTS
Sincere thanks to Squad Medicine and Research (SMR) for their support and guidance for the case report and publication.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
INFORMED CONSENT
Written informed consent was taken from patient.
AUTHORS' CONTRIBUTIONS
Surendar Jatoth (Conceptualization, Resources, Investigation, Writing—Original Draft), Tarun K. Suvvari (Writing—Original Draft, Writing—Review and Editing, Supervision), Shashank J (Conceptualization, Resources, Investigation, Writing—Review and Editing, Supervision), Aiman P. Afsar (Writing—Original Draft, Writing—Review and Editing), Shivani Ravipati (Writing—Original Draft, Writing—Review and Editing), Lakshmi S. Mukkamala (Writing—Original Draft, Writing—Review and Editing), Vimal Thomas (Writing—Original Draft, Writing—Review and Editing, Supervision, Project administration).
DATA AVAILABILITY
The data underlying this article will be shared on reasonable request to the corresponding author.



