-
PDF
- Split View
-
Views
-
Cite
Cite
Tricia Chiu, Nithya Niranjan, Kate FitzGerald, Endometrioma causing recurrent small bowel obstruction in a virgin abdomen—a case report and literature review, Journal of Surgical Case Reports, Volume 2023, Issue 7, July 2023, rjad392, https://doi.org/10.1093/jscr/rjad392
Close - Share Icon Share
Abstract
There has been a modest number of cases of bowel obstruction secondary to endometriosis reported. Delays in diagnoses can cause significant morbidity to patients. We describe the case of a 45-year-old female with a 2-year history of recurrent small bowel obstructions (SBOs) without a history of abdominal surgery. She underwent multiple computed tomography scans, and a magnetic resonance enterography, which queried possible terminal ileitis secondary to Crohn’s fibro-stenosing disease or a Meckel’s diverticulum. Colonoscopy up to TI was normal. Elective laparoscopy showed a cicatrizing small bowel mass in her distal ileum ~15 cm from the TI, which was resected. There were no other findings. Histopathological testing revealed endometriosis. At 2-month post-resection, she remains symptom-free and was referred to gynaecology. Endometriosis causing bowel obstruction should be considered early in female patients, especially those with virgin abdomens. Timely elective laparoscopy is a safe and effective way of diagnosing and treating small bowel obstruction, avoiding an emergency procedure.
INTRODUCTION
Endometriosis is a condition where endometrial glands and tissue implant grow outside the uterus with an estimated prevalence of 6–25% [1]. It has been increasingly seen as an underdiagnosed condition [2]. Despite the relatively high prevalence of endometriosis, the occurrence of endometriosis or endometriomas in the gastrointestinal tract (GIT) resulting in bowel obstructions is rare [3]. A large population-based study in Canada [1] reported that the prevalence of women aged 18–55 with endometriosis who have experienced at least one episode of bowel obstruction is 52 in 10 000 [1].
A comprehensive literature review of the past 20 years revealed a modest number of cases of endometriosis causing bowel obstructions in various locations of the GIT, from the rectum to the small bowel. Along the GIT, the rectosigmoid is the most involved by endometriosis [4]. In other reported cases, other stigmata of endometriosis were found on laparoscopy [3, 5, 6], and the majority of cases were managed in an emergency setting with a small bowel obstruction (SBO) not amenable to conservative therapy [3, 5]. Some case studies also report a monthly, cyclical pattern of SBO symptoms [7, 8]. In cases with ileal endometriosis, colonoscopy was usually positive for a mass or stricture [8, 9].
We report the first case of a SBO due to cicatrizing ileal endometrioma resulting in recurrent SBOs, with a normal colonoscopy and a laparoscopy negative for any further stigmata of endometriosis, that was managed in an elective setting.
CASE REPORT
A 45-year-old female presented to the emergency department in 2022 with nausea, constipation and abdominal cramping on the background of at least four recurrent similar episodes in 2021. Her medical history includes Graves’ disease, Iron Deficiency Anaemia (IDA) with a negative faecal occult blood test (FOBT) and anxiety. She had no surgical history. Her menstrual history includes period pain on Day 1, with no pain after. She did not have a family history of inflammatory bowel disease. She did not smoke or drink alcohol. Routine bloods were normal. Due to her Graves’ disease, radiology performed a CT of her abdomen and pelvis without IV contrast. This showed a SBO with multiple distended loops of bowel up to the level of the ileum, with a transition point somewhere in the right iliac fossa (RIF). Her symptoms settled with conservative treatment, and she was discharged home with the presumptive diagnosis of a congenital adhesion.
She represented 4 months later with similar symptoms and vomiting. Again, a non-con CT was done showing similar findings to the first CT. On retrospective review of the CT, there might have been a mass present close to the IC valve (Fig. 1). A repeat CT with IV contrast was done within the same admission, which showed a possible stricture at the terminal ileum (TI). Her faecal calprotectin was high at 95.8 μg/g (<50). Blood tests were unremarkable. Again, she resolved with conservative management and was discharged with a plan for an outpatient magnetic resonance enterography (MRE) and colonoscopy.
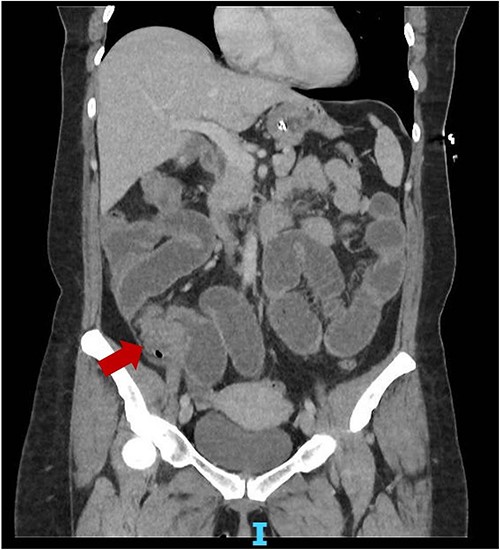
Coronal slice CT abdomen pelvis showing SBO with transition point at the distal ileum secondary to a possible mass.
Her MRE showed a small bowel lesion ~10 cm proximal to the ileocaecal valve, favoured to represent a Meckel’s (Fig. 2). A colonoscopy was done to exclude a diagnosis of Crohn’s disease. A colonoscope was passed into the TI and advanced a further 5 cm, with normal mucosa throughout.
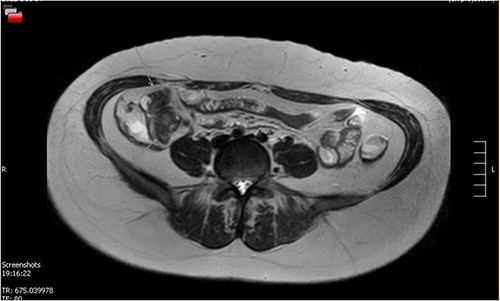
MRE showing small bowel lesion ~10 cm proximal to the ileocaecal valve.
She then underwent an elective diagnostic laparoscopy which showed a cicatrizing small bowel mass in distal ileum ~15 cm from TI (Figs 3 and 4), with a normal appendix and no other abnormalities. There were no stigmata of endometriosis, and no free fluid or blood in the pelvis/abdomen. A wedge resection of the mass with a side-to-side small bowel anastomosis and planned removal of the appendix (due to pre-operative concerns of further adhesions in the area) was performed.
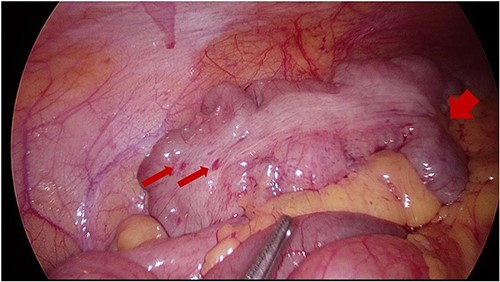
Intraoperative image at laparoscopy showing TI tethered down into cicatrizing mass. Foci of endometriosis on proximal large bowel.
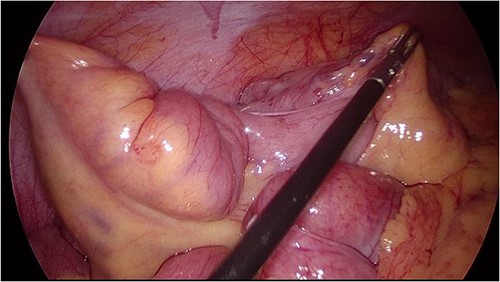
Intraoperative image at laparoscopy showing dilated distal small bowel loop and tethered TI (unable to straighten out bowel).
Histopathological testing revealed endometriosis, with the epithelium being ER +, and CK7+ and the endometriotic stroma ER + and CD10+. There was mural cystic endometriosis with associated chronic inflammation in the small bowel and endometriotic foci in the appendix. There was no granulomatous inflammation, dysplasia or neoplasia in the small bowel.
She made an uneventful recovery from her surgery and was discharged home. On follow-up 2 months later, she was pain-free and symptom-free and was scheduled to visit an obstetrics and gynaecology specialist for review and follow-up, given her diagnosis of endometriosis.
DISCUSSION
The symptoms and signs of endometriosis are often nonspecific [4], leading to diagnostic dilemmas and underdiagnoses [2]. Imaging techniques such as MRI with specific MRI protocols for endometriosis such as bowel preparation, and imaging outside of the active menstrual period, are considered the best imaging techniques for endometriosis in the preoperative staging period [4]. At present, direct visualization via laparoscopy is still considered the gold standard for diagnosing endometriosis [10].
Our patient faced multiple challenges to reach her diagnosis. She did not have the more common symptoms [4] experienced by women with endometriosis such as pelvic pain, infertility or dysmenorrhea. She did have IDA with a negative FOBT, likely due to heavy periods. However, this is common in menstruating women who might not have endometriosis. She also had a delayed diagnosis possibly due to the nonspecific findings on imaging and a normal colonoscopy. Thankfully, an emergency operation was avoided, and she was treated with an elective resection of her small bowel and appendix.
Many patients with recurrent SBO thought to be secondary to adhesions who settle with conservative therapy are often discharged from acute surgical units with little specialist follow-up. This is less common in the case of recurrent SBO in a virgin abdomen, where there is often an underlying cause [11]. We believe that reaching an early definitive diagnosis, especially in women of childbearing age, with a virgin abdomen and recurrent SBO provides the opportunity to intervene and manage the patient electively rather than in the setting of an acute obstruction where emergency surgery is sometimes inevitable. These patients should be followed up and investigated until a definitive diagnosis is reached.
CONFLICT OF INTEREST STATEMENT
There are no conflicts of interest to be declared.
FUNDING
This paper has not been funded.
CONSENT FOR PUBLICATION
Patient has provided informed consent for this case report to be published.
DATA AVAILABILITY
All data underlying the results are available as part of the article and no additional source data are required.
References
- small bowel obstruction
- computed tomography
- colonoscopy
- crohn's disease
- endometriosis
- gynecology
- intestinal obstruction
- intestine, small
- laparoscopy
- abdomen
- meckel's diverticulum
- morbidity
- distal ileum
- endometrioma
- abdominal surgery
- crohn's disease of terminal ileum
- histopathology tests
- magnetic resonance enterography



