-
PDF
- Split View
-
Views
-
Cite
Cite
Yasuyuki Omichi, Daisuke Hamada, Ryo Okada, Keizo Wada, Yasuaki Tamaki, Shinichiro Yamada, Tomohiro Goto, Koichi Sairyo, Hematogenous prosthetic knee joint infection with Klebsiella pneumoniae caused by asymptomatic gallbladder abscess: a case report and literature review, Journal of Surgical Case Reports, Volume 2023, Issue 6, June 2023, rjad355, https://doi.org/10.1093/jscr/rjad355
Close - Share Icon Share
Abstract
Klebsiella pneumoniae has the ability to form biofilm; therefore, the treatment of prosthetic joint infection involving K. pneumoniae is often challenging. This report describes the first case of acute hematogenous prosthetic knee joint infection with K. pneumoniae that occurred as a result of an asymptomatic gallbladder abscess. The patient was a 78-year-old man who underwent bilateral total knee arthroplasty 6 years ago. He had pain and swelling in his right knee. The synovial fluid culture of the right knee revealed K. pneumoniae and prosthetic joint infection was diagnosed. Computed tomography revealed a gallbladder abscess in the absence of right upper abdominal pain. The patient underwent simultaneous debridement of the knee and open cholecystectomy. The treatment was successful and the prosthesis was retained. In cases of hematogenous prosthetic joint infection with K. pneumoniae, other sources of infection should be suspected and investigated regardless of whether they are symptomatic.
INTRODUCTION
Periprosthetic joint infection (PJI) is one of the significant complications of total knee arthroplasty (TKA) and is often difficult to treat. PJI occurs in 0.5–1.9% of primary TKAs and in 8–10% of revision TKAs [1]. According to the Tsukayama classification, PJI is classified into four types based on type of infection and interval between first surgery and onset as follows: type I, early infection; type II, late chronic infection; type III, acute hematogenous infection; and type IV, positive intraoperative culture at the time of the revision surgery performed based on aseptic loosening preoperatively [2].
Klebsiella pneumoniae is a gram-negative pathogenic bacterium and part of the Enterobacteriaceae family [3]. Klebsiella pneumoniae is the second leading cause of bloodstream infections caused by gram-negative bacteria [4]. Klebsiella spp. are occasionally found in early PJI, but PJI resulting from acute hematogenous spread of Klebsiella spp. is rare [5].
In this report, we describe the first case of acute PJI due to asymptomatic gallbladder abscess caused by K. pneumoniae and of simultaneous treatment of PJI and cholecystitis.
REPORT OF THE CASE
Written informed consent was obtained from the patient for publication of this case report.
The patient was a 78-year-old man with a history of type 2 diabetes mellitus, old myocardial infarction and lacunar infarction who had undergone bilateral TKA for knee osteoarthritis 6 years earlier and had a good postoperative course.
One week earlier, he had visited a local doctor with pain and swelling in his right knee. Cloudy synovial fluid was aspirated from the right knee and PJI was suspected. He was referred to our hospital on the same day and presented with pain, swelling, warmth and redness in the right knee and a slight fever. A plain radiograph showed no aseptic loosening (Fig. 1). An alpha defensin test (Synovasure, Zimmer-Biomet, Warsaw, IN) on synovial fluid was positive [6], and PJI was diagnosed. He was admitted on the same day and scheduled for surgical knee debridement on the following day.
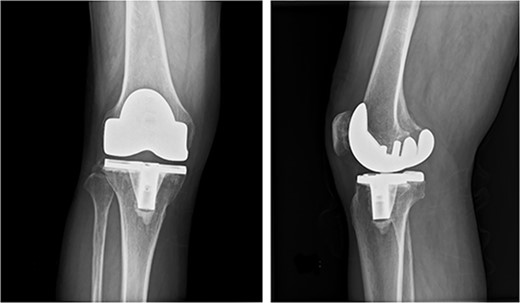
Preoperative anteroposterior and lateral radiographs of the knee show no evidence of aseptic loosening.
The results of the synovial fluid culture obtained by the previous doctor revealed K. pneumoniae on the next day, which is uncommon in PJI. Computed tomography (CT) imaging of the trunk was performed to screen for other sources of infection. CT revealed multilocular swelling of the gallbladder with diffuse wall thickening, gallstones lodged in the bile duct, and an abscess that had spread to the liver (Fig. 2). There was no bloating or pain in the right upper quadrant but Murphy’s sign was positive. We diagnosed cholecystitis with abscess that had been asymptomatic. We considered that emergency cholecystectomy would be high risk in view of his multiple comorbidities and the fact that he was on antiplatelet therapy. Instead, we elected to treat the cholecystitis first using antibiotics.
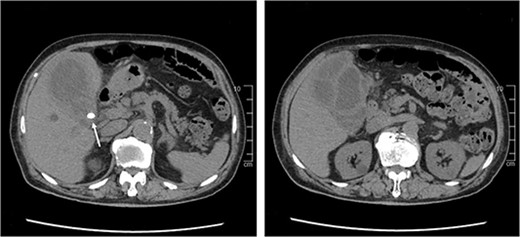
CT scan of the abdomen shows diffuse thickening of the gallbladder wall and gallstones lodged in the bile duct (white arrow).
Knee debridement surgery was performed as scheduled and revealed cloudy synovial fluid with scarring and necrotic tissue in the joint. No loosening was observed. Considering the short duration of knee symptoms, the polyethylene insert was exchanged and the original prosthesis was retained. Antibiotic therapy consisting of sulbactam/cefoperazone and levofloxacin was started postoperatively. Intraoperative cultures grew hypervirulent K. pneumoniae.
Percutaneous transhepatic biliary drainage and endoscopic retrograde cholangiopancreatography were performed for the gallbladder abscess and cholelithiasis on day 5. Culture of the fluid drained from the gallbladder revealed K. pneumoniae. Even after the procedure, the gallbladder drainage fluid continued to contain pus, indicating ongoing cholecystitis and a need for gallbladder surgery (Fig. 3).
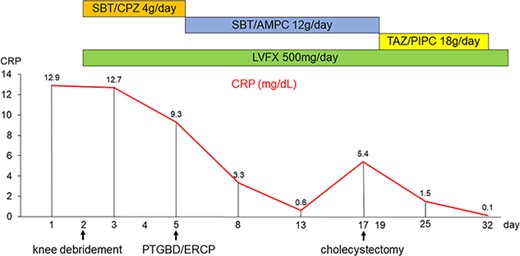
Timeline of antibiotic and surgical treatment, and changes in the C-reactive protein level. CRP, C-reactive protein; ERCP, endoscopic retrograde cholangiopancreatography; LVFX, levofloxacin; PTBD, percutaneous transhepatic biliary drainage; SBT/AMPC, sulbactam/ampicillin; SBT/CPZ, sulbactam/cefoperazone; TAZ/PIPC, tazobactam/piperacillin.
Open cholecystectomy was performed on day 17. His subsequent course was uneventful, and antibiotic therapy was stopped 100 d after knee debridement. There has been no recurrence of PJI during the more than 2 years since his surgery. The prosthesis was retained, and the patient’s knee joint function recovered before onset of PJI.
DISCUSSION
Klebsiella pneumoniae is a pathogen that is both common hospital-acquired and community acquired [4, 7]. Hospital-acquired K. pneumoniae bloodstream infections are most commonly associated with malignancy, whereas those that are community-acquired are most often associated with diabetes mellitus and chronic liver disease [8]. Recent studies of community-acquired pathogens have reported colonisation rates of 15% in the nasopharynx [9] and 19–23% in the gastrointestinal tract [10]. Our patient had a history of diabetes mellitus but it did not interfere in his activities of daily life. It is presumed that he was a carrier of community-acquired K. pneumoniae in the gastrointestinal tract and that K. pneumoniae caused the cholecystitis and subsequent PJI via hematogenous spread.
PJI with K. pneumonia is rare. Bentio et al. reported that hematogenous spread of Klebsiella spp. accounted for 0.4% of 268 cases of PJI [5]. To date, there have been only three reports of hematogenous PJI in which K. pneumoniae was the causative organism (Table 1) [11–13].
Summary of a case of hematogenous prosthetic knee joint infection with Klebsiella pneumoniae
| Case . | Sex . | Age . | Comorbidities . | Symptoms . | Source of K. pneumoniae . | First surgical strategy . | Final surgical treatment . |
|---|---|---|---|---|---|---|---|
| Lin et al. (2006) | M | 70 | DM | Right upper Abdominal pain, High fever, Knee symptoms | Acute cholecystitis | Arthroscopic debridement | Prosthesis replacement |
| Chodos et al. (2009) | M | 56 | DM | Right lower abdominal pain, High fever, Knee symptoms | Occult adenocarcinoma of the cecum | Insert exchange and DAIR | AST |
| Pepke et al. (2013) | M | 79 | Prostatic carcinoma | Knee symptoms | Urinary tract infection | Prosthesis removal | Prosthesis replacement |
| Our case | M | 78 | DM, OMI | Knee symptoms, Slight fever | Asymptomatic gallbladder abscess | Insert exchange and DAIR | AST |
| Case . | Sex . | Age . | Comorbidities . | Symptoms . | Source of K. pneumoniae . | First surgical strategy . | Final surgical treatment . |
|---|---|---|---|---|---|---|---|
| Lin et al. (2006) | M | 70 | DM | Right upper Abdominal pain, High fever, Knee symptoms | Acute cholecystitis | Arthroscopic debridement | Prosthesis replacement |
| Chodos et al. (2009) | M | 56 | DM | Right lower abdominal pain, High fever, Knee symptoms | Occult adenocarcinoma of the cecum | Insert exchange and DAIR | AST |
| Pepke et al. (2013) | M | 79 | Prostatic carcinoma | Knee symptoms | Urinary tract infection | Prosthesis removal | Prosthesis replacement |
| Our case | M | 78 | DM, OMI | Knee symptoms, Slight fever | Asymptomatic gallbladder abscess | Insert exchange and DAIR | AST |
AST, antibiotic suppressive therapy; DAIR, debridement, antibiotics, and implant retention; DM, diabetes mellitus; OMI, old myocardial infarction; PJI, prosthetic joint infection
Summary of a case of hematogenous prosthetic knee joint infection with Klebsiella pneumoniae
| Case . | Sex . | Age . | Comorbidities . | Symptoms . | Source of K. pneumoniae . | First surgical strategy . | Final surgical treatment . |
|---|---|---|---|---|---|---|---|
| Lin et al. (2006) | M | 70 | DM | Right upper Abdominal pain, High fever, Knee symptoms | Acute cholecystitis | Arthroscopic debridement | Prosthesis replacement |
| Chodos et al. (2009) | M | 56 | DM | Right lower abdominal pain, High fever, Knee symptoms | Occult adenocarcinoma of the cecum | Insert exchange and DAIR | AST |
| Pepke et al. (2013) | M | 79 | Prostatic carcinoma | Knee symptoms | Urinary tract infection | Prosthesis removal | Prosthesis replacement |
| Our case | M | 78 | DM, OMI | Knee symptoms, Slight fever | Asymptomatic gallbladder abscess | Insert exchange and DAIR | AST |
| Case . | Sex . | Age . | Comorbidities . | Symptoms . | Source of K. pneumoniae . | First surgical strategy . | Final surgical treatment . |
|---|---|---|---|---|---|---|---|
| Lin et al. (2006) | M | 70 | DM | Right upper Abdominal pain, High fever, Knee symptoms | Acute cholecystitis | Arthroscopic debridement | Prosthesis replacement |
| Chodos et al. (2009) | M | 56 | DM | Right lower abdominal pain, High fever, Knee symptoms | Occult adenocarcinoma of the cecum | Insert exchange and DAIR | AST |
| Pepke et al. (2013) | M | 79 | Prostatic carcinoma | Knee symptoms | Urinary tract infection | Prosthesis removal | Prosthesis replacement |
| Our case | M | 78 | DM, OMI | Knee symptoms, Slight fever | Asymptomatic gallbladder abscess | Insert exchange and DAIR | AST |
AST, antibiotic suppressive therapy; DAIR, debridement, antibiotics, and implant retention; DM, diabetes mellitus; OMI, old myocardial infarction; PJI, prosthetic joint infection
Our patient had no abdominal pain, and had we not performed CT, diagnosis and treatment of the gallbladder abscess would have been delayed. In the case reported by Lin et al., the patient had acute cholecystitis that was treated by antibiotic therapy alone, resulting in prolonged cholecystitis and removal of the prosthesis [11]. Patients with PJI in which the causative organism is K. pneumoniae should be investigated for potential hematogenous spread of infection from another site, such as the gastrointestinal tract or urinary tract, regardless of whether the patient is symptomatic.
Treatment of PJI involving K. pneumoniae is challenging. Klebsiella pneumoniae has the ability to form biofilm, which allows the pathogen to evade the host immune response and action of antibiotics and to survive on prosthetic surfaces[14,]. In recent years, there have been reports of PJI with multidrug-resistant K. pneumoniae, treatment of which is even more challenging [15]. Formation of biofilm and multidrug resistance should be considered when treating PJI with K. pneumoniae.
We encountered a case of PJI in the knee that resulted from hematogenous spread of K. pneumoniae from an asymptomatic gallbladder abscess in which the prosthesis was successfully retained. When treating hematogenous PJI in which the causative organism is K. pneumoniae, other sources of infection should be suspected and investigated, regardless of whether they are symptomatic.
AUTHORS’ CONTRIBUTIONS
Y.O. contributed to data curation, formal analysis, writing—original graft. D.H. contributed to conceptualisation, supervision, writing—review and editing. R.O., K.W., YT., S.Y., T.G. interpreted the clinical data, and revised the manuscript critically for important content. K.S. contributed to supervision. All authors have reviewed and approved the final manuscript.
CONFLICT OF INTERESTS STATEMENT
None declared.
FUNDING
None.
DATA AVAILABILITY
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Written informed consent was obtained from the patient for publication of their case. A statement of the ethics committee was not required for this anonymised case report in accordance with the legislation of the Institutional Review Committee of Tokushima University Hospital.
CONSENT FOR PUBLICATION
Written informed consent was obtained from the patient for her clinical information to be published in this report.



