-
PDF
- Split View
-
Views
-
Cite
Cite
Sabrina Weber, Method Kabelitz, Nina Kabelitz, Veit Schoenborn, Haemophilus haemolyticus: an atypical pathogen of septic arthritis of the knee joint, Journal of Surgical Case Reports, Volume 2020, Issue 9, September 2020, rjaa318, https://doi.org/10.1093/jscr/rjaa318
Close - Share Icon Share
Abstract
Septic knee arthritis is a common disease, mostly due to bacterial infections. We describe a rare case of Haemophilus haemolyticus causing unilateral septic arthritis of a native knee. The affected patient presented with persistent severe knee pain after repeated intra-articular injections. Patient history included knee arthroscopy and a known rheumatoid arthritis treated by steroids. Since conservative treatment was ineffective and infection could not be excluded, diagnostic arthroscopy was performed. Synovial fluid and biopsies verified the uncommon microorganism and antibiotic therapy was initiated. Clinical findings and blood results showed rapid improvement. The patient was discharged in a good condition after 6 weeks. A review of the current literature describes only one joint infection with H. haemolyticus as underlying cause. In immunocompromised patients with septic knee arthritis also atypical pathogens must be considered. Nevertheless, the established treatment algorithm with arthroscopy and anti-infective therapy seems to be effective leading to satisfactory results.
INTRODUCTION
Septic arthritis of the knee joint is a common diagnosis, mostly established due to infections with commensal bacteria, such as staphylococcus or streptococcus.
An acute septic arthritis of the knee caused by bacterial pathogens could be an emergency. If left untreated it can lead to substantial joint destruction. In literature several risk factors for development of septic arthritis are already described.
The diagnosis is based on clinical findings such as swelling, reddening, hyperthermia and dysfunction as well as increased typical laboratory values and inflammatory markers from serum and joint fluids.
Haemophilus haemolyticus belongs to gram-negative bacteria and is a hemoglobin splittingpathogen unknown for causing any morbidity. It colonizes the respiratory and genital tract and is generally considered to be a commensal organism that is rarely involved in causing human diseases. However some serious cases like endocarditis have been described. To our knowledge, only one case of septic arthritis due to H. haemolyticus is reported in current literature.
The initial and general antibiotic regimen should cover methicillin-resistant Staphylococcus aureus as well as gram-negative and gram-positive organisms. The therapy should be specified following the culture results of the infected joint. Operative management involves either arthrotomy or arthroscopy of the knee with thorough irrigation and debridement of all infected tissue. The Gächter classification is useful in establishing a prognosis or in determining the need for an extensive debridement [1–4].
CASE REPORT
An 82-year-old female presented in a corresponding hospital with isolated acute atraumatic exacerbation of pain of the left knee joint. Patient’s history showed a bilateral knee-arthroscopy over 20 years ago and a history of chronic joint pain due to a rheumatoid arthritis, which was treated with prednisolone 5 mg/d and Ethanercept (Enbrel) for many years. Due to increasing pain, her family doctor performed an intra-articular injection with oxygen and ozone 6 days prior to first presentation in hospital. Two days after this first infiltration, clinical signs of acute inflammation occurred, so a cortisone injection was applied. Pain decreased immediately but only another 2 days later, a new exacerbation of symptoms occurred, followed by presentation in hospital. Since the patient was in good general condition, initial treatment was only done by increasing her prednisolone dose (newly 30 mg/d) and analgesia. Because of persistent pain a puncture of the knee joint followed another 3 days later. Results showed a pleocytosis and an increased number of leucocytes with 80% neutrophils. Neither crystals nor bacteria could be found after incubation of 7 days. Since pain lasted despite the prednisolone-therapy, analgesia and physiotherapy, once more a knee-infiltration with 40 mg of Triamcinolon/Lidocain was performed. One month after first presentation and still no improvement of pain, the patient was then referred to internal medicine department of our hospital for further treatment.
In our emergency department, despite of lasting severe knee pain, patient’s general condition was good.
Vital signs were normal with a blood pressure of 112/57 mmHg and a heart rate of 60/min, an oxygen saturation of 92% and a normal body temperature. The blood results showed a leucocytosis of 13.1 × 10E3/μl with slightly elevated CRP of 45.2 mg/l. The affected joint itself showed hyperthermic conditions and effusion. There was no redness. Due to excessive pain active knee movement was not possible. Passive flexion reached 110° with an extension deficit of 30°. There was a tenderness of palpitation on the medial and lateral joint line. An aspiration was performed which showed dingy joint fluid. After an incubation of 14 days in the laboratory, the microbiological results showed new growth of H. haemolyticus as only pathogenic germ.
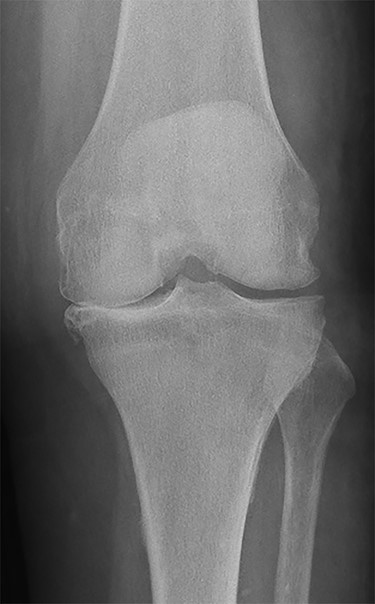
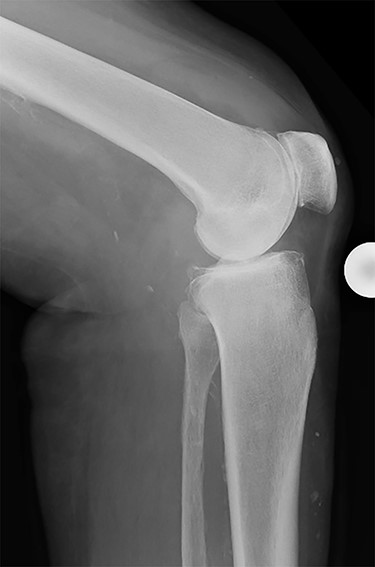
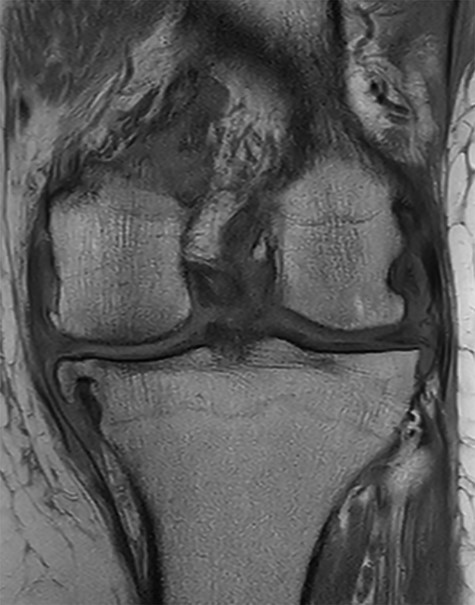
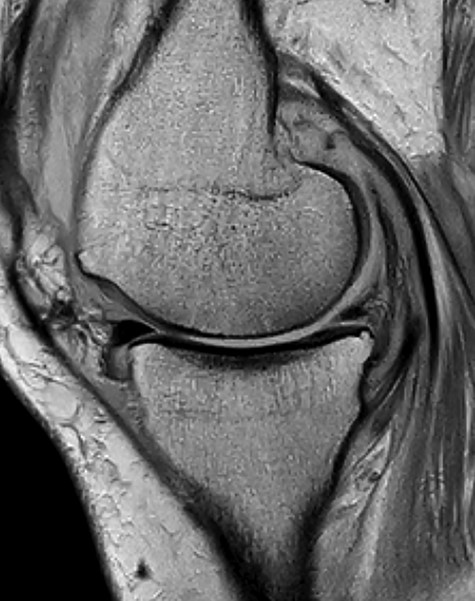
Conventional radiographs in an anteroposterior and lateral view showed advanced osteoarthritis (Kellgren stage III) accentuated medially and patellofemoral (Figs 1 and 2). An additional magnetic resonance imaging (MRI) was performed, which confirmed the medial accentuated osteoarthritis, it revealed some minor meniscal tears, some signs of general synovitis and joint effusion (Figs 3 and 4).
After interdisciplinary discussion of the clinical and microbiological findings an arthroscopy of the knee with lavage and sampling was performed. Intraoperatively a septic arthritis (Gächter stage III) could be diagnosed. An empiric intravenous antibiotic therapy with amoxicillin/clavulanic acid 2,2 g three times a day was introduced [1, 3]. Growth of an ampicillin-sensitive H. haemolyticus could eventually be verified in all of the intraoperative taken samples (4/4), so the initiated antibiotic therapy could be continued. After 3 weeks of parenteral therapy oral application has been started and was applied for another 3 weeks. Physiotherapy war performed daily and a reduction of the prednisolone-dose and analgesia was done.
With the antibiotic therapy, analgesia and physiotherapy the further hospitalization was uneventful. The swelling decreased and blood values normalized. Due to some persistent pain the prednisolone medication was only gradually reduced until 15 mg/d. Eventually the patient felt better und could be discharged with a satisfying range of motion and in a good general condition. Until now, there were no further consultations because of the previous symptomatic.
DISCUSSION
Review of current literature shows only one case of septic knee arthritis with H. haemolyticus [4]. Common pathogens such as staphylococcal or streptococcal could not be found in our samplings. But we were able to detect an uncommon pathogen which is mostly known to cause influenza [4, 5].
Although this pathogen was detected shortly after cultivation, it is very important to cultivate the samples at least 14 days, so difficult to detect pathogens, such as Cutibacterium acnes will not be missed [6].
Besides the common bacteria, in immunocompromised patients with septic knee arthritis also atypical pathogens must be considered. Nevertheless, the established treatment algorithm with arthroscopy and anti-infective therapy seems to be an effective treatment option leading to satisfactory results [3].
Our patient presented at our hospital without any signs of infection but severe pain of the left knee. She was always in a relatively good general condition, but despite analgesia, steroids and physiotherapy no long-lasting and sufficient reduction of pain could be established. Finally, decision for surgery was made. The postoperative immediate and persistent relief of pain supported this approach.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
References
Anderson R, Wang X, Briere EC, Katz LS, Cohn AC, Clark TA, et al. Haemophilus haemolyticus isolates causing clinical disease.
Bossard DA, Ledergerber B, Zingg PO, Gerber C, Zinkernagel AS, Zbinden R, et al. . Optimal length of cultivation time for isolation of Propionibacterium acnes in suspected bone and joint infections is more than 7 days.
Author notes
Sabrina Weber and Method Kabelitz contributed equally to this work and are shared first authors.
- rheumatoid arthritis
- arthritis
- bacterial arthritis
- bacterial infections
- biopsy
- arthroscopy
- anti-infective agents
- immunocompromised host
- intra-articular injections
- knee joint
- steroids
- synovial fluid
- infections
- diagnosis
- medical history
- persistence
- pathogenic organism
- antibiotic therapy
- knee pain
- knee arthroscopy
- microorganisms
- septic knee
- joint infections
- conservative treatment
- haemophilus haemolyticus
- verification



