-
PDF
- Split View
-
Views
-
Cite
Cite
Jackson J Pat, Muhammad Rafaih Iqbal, Christopher Wright, An unexpected surprise: rare association of neuroendocrine tumours in inflammatory bowel disease, Journal of Surgical Case Reports, Volume 2020, Issue 9, September 2020, rjaa306, https://doi.org/10.1093/jscr/rjaa306
Close - Share Icon Share
Abstract
Neuroendocrine neoplasms are rare malignancies, more so when cancerous metastasis occurs without a known primary source. Here we discuss a case of an ulcerative colitis sufferer, 43-year-old lady presented with what was thought to be a flare up. Situation deteriorated and was taken to theatre to find a significantly ischaemic colon, secondary to extensive venous thrombosis. The ischaemic bowel was resected alongside with what was thought to be a large, reactive lymph node. To our surprise, the resected lymph node returned with evidence of neuroendocrine neoplastic metastasis. Multiple laboratory and imaging investigations were performed in hope to identify the primary source. A second metastatic lymph node was identified and subsequently resected but the primary remains elusive. Currently, there are no visible evidences of active disease.
INTRODUCTION
The correlation between inflammatory bowel disease (IBD) and colorectal adenocarcinoma is well documented and has been shown to be an independent risk factor for its development [1]. Infrequently, association between IBD and non-epithelial malignancies such as lymphomas are also identified especially within the cohort of immunosuppressed patients [2]. Neuroendocrine neoplasm is, in itself, uncommon but found to be rarer in the context of IBD. It was suggested that long-standing inflammation of the mucosa may be the result of this particular neoplasia [3–5]. The following case initially describes a common presentation of IBD, which brought about an interesting surprise following an emergency diagnostic laparotomy. It also highlights the importance of multidisciplinary working in the management of critically ill patients.
CASE REPORT
A 43-year-old lady presented to the lower GI clinic secondary to rectal bleeding. She reported her bowels open approximately four times a day and stools were described to be small and loose with occasional clots and ribbon-like characteristics. She also denied having any unintentional weight loss. No previous surgical or medical history.
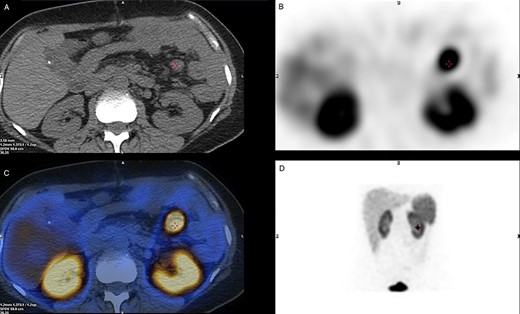
SPECT/CT Octreotide imaging. (A) A CT cross-section view indicating the location of the malignant lymph node. (B) A SPECT cross-section of the same plane indicating high uptake over the Region of Interest. (C) A combined view of SPECT/CT with superimposed images demonstrating hotspot over the malignant lymph node. (D) Octreotide SPECT coronal view showing the position of the malignant lymph node.
Initial examination showed soft, non-tender abdomen. Rectal examination revealed a suspicious anterior rectal mass. An urgent colonoscopy was therefore arranged and biopsies returned to show evidence of ulcerative colitis (UC) but no masses/neoplasia. Despite establishing the diagnosis and initiating appropriate Asacol and mesalazine treatment, she subsequently became significantly unwell and presented through the emergency department with severe abdominal pain, distention and vomiting. Physical examination revealed a blood pressure of 101/67 mmHg, HR of 123 beats/min, respiration rate of 24 breaths/min and saturations of 90% in room air. Computed tomography (CT) abdomen and pelvis not only showed descending colon inflammation and severe terminal ileitis but also moderate volumes of free fluid with extensive intra-abdominal inflammation. Initial laboratory blood tests were Hb 132, WBC 8.23, Plts 44, lactate 1.2, CRP 72, K+ 3.3, AST 46, Albumin 37. PR bleeding continued and haemoglobin levels began to drop out of proportion, reaching a low of 70 g/l as well as derangement of her coagulation studies. She was then escalated to critical care given her persistent hypotension and DIC, but ultimately she underwent emergency laparotomy. In theatre, we identified a massive retroperitoneal haematoma and approximately 30 cm of gangrenous terminal ileum. Patchy gangrene tissue of the ascending and descending colon was noted with preservation of the sigmoid colon. A subtotal colectomy was performed with end ileostomy and the cross-stapled sigmoid stump was left in situ. Additionally, two large (3 cm) abnormal mesenteric lymph nodes were also identified adjacent to the DJ flexure. These were resected for histological analysis. Histology of the lymph node surprisingly showed evidence of metastatic neuro-endocrine carcinoma with characteristics of solid trabecular growth and moderate nuclear pleomorphism (Figs 3 and 4). Post-operatively, she underwent a number of investigations in hope to identify the primary, as well as tests to identify the cause of the thrombosis.
Initial basic laboratory investigations on presentation are mentioned above; however given the complexity of this case, further investigation was required. An octreotide single-photon emission computed tomography (SPECT/CT) imaging was performed in hope to identify any additional active tumour cells (Fig. 1). An avid ~15 mm node was noted in the proximal mesenteric jejunum (Fig. 2), as seen intra-operatively, with no additional pancreatic, small bowel or colonic uptake. Other specialized laboratory investigations included chromogranin A&B, which were within normal values of 20 and 88 pmol/L, respectively. 24-h urine 5-HIAA test was also normal of 14 μmol/24 h. The overall image and appearance closely points to a well-differentiated grade 2 neuro-endocrine carcinoma.
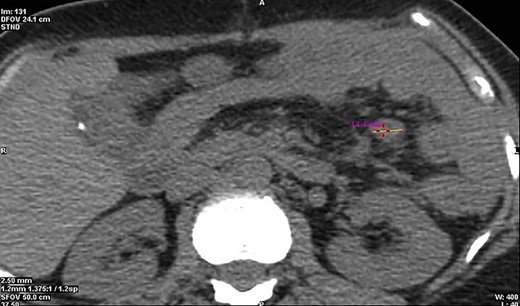
CT cross-section illustrating a diameter of 14.4 mm of the malignant neuroendocrine tumour.
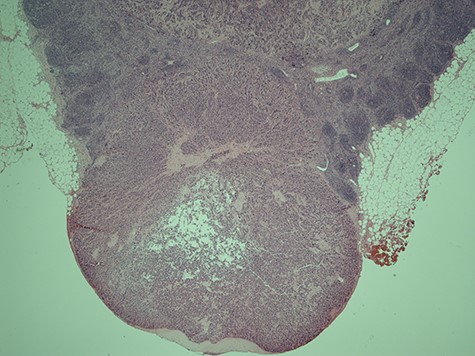
Histological slice of the specimen acquired on the second lymph node removal.
The patient continues to experience passing blood per rectum secondary to the ulcerative proctitis however she is making a good recovery post-surgery.
DISCUSSION
Neuroendocrine tumours (NETs) are rare neoplasms arising from the endocrine and nervous systems. These are frequently, but not always, derived from the gastrointestinal system. The World Health Organization emphasizes NET classification via its tumour grade over anatomical/cytological derivative. Typically for gastroenteropancreatic tumours, it incorporates the mitotic count and Ki-67 proliferation for the classification and divides into three grades:
G1—well differentiated, low grade.
G2—well differentiated, intermediate grade.
G3—poorly differentiated, high grade [6,7].
When compared to typical colorectal adenocarcinoma, NETs tend to adopt a poorer prognosis. Associations between UC and NETs are usually documented in the form of carcinoids.
Some authors such as Sigel et al. [9] suggest that a link may be present with non-carcinoid neuroendocrine differentiation. They studied 14 IBD patients with associated NET and observed that all tumours arose from areas with affected inflammation. Greenstein et al. [8] concluded however that there were no direct associations between the two.
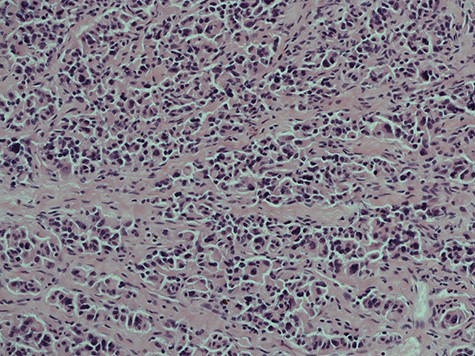
A histological slice of the resected second lymph node tumour; viewed under x20 power.
Comparatively in our case, we have only located evidence of metastatic neuroendocrine neoplasms within the mesenteric lymph nodes and the source of metastasis remains unidentified. As this may be uncommon, literature paradoxically suggests that patients with these tumours tend to have relatively favourable prognoses.
Dorffel et al. [10] discuss the association between common biostructures of colonic microbiota in neuroendocrine tumours and Crohn’s disease. They suggest that the pathway of neuroendocrine differentiation may stem from a similar biological origin as the pathological development of IBD. We believe this case has presented with essential take home messages:
(i) The importance of doing a thorough exploratory laparotomy even in context of identifiable pathology.
(ii) The invaluable input from the multidisciplinary team, ensuring safe stabilization and smooth HDU transfer of critically unwell patients.
(iii) And lastly, we are to remember ischaemic bowel be very difficult condition to diagnose. Early surgical intervention is paramount especially in patients that are severely deteriorating with unclear presentation.
In summary, we have a 43-year-old IBD patient presented with an unexpected NET of unknown primary. Her case was exacerbated by an acute mesenteric venous thrombosis and resulted in a colectomy. Laboratory and imaging investigations were not able to identify the cause of the NET primary. This opens doors for debate as to whether active surveillance should be continued despite known radiation risk or a ‘watch and wait’ regime should be adopted.
CONFLICT OF INTEREST
None declared.



