-
PDF
- Split View
-
Views
-
Cite
Cite
Alex Paul Guachilema Ribadeneira, Cristhian Ramiro García, Andrea Daniela Basantes, Radical neck dissection with advancement flap in advanced papillary thyroid cancer: a therapeutic option, Journal of Surgical Case Reports, Volume 2020, Issue 12, December 2020, rjaa558, https://doi.org/10.1093/jscr/rjaa558
Close - Share Icon Share
Abstract
Papillary thyroid cancer (TC) is the most common TC subtype with a global incidence of 80–90% and an annual rate of increase of 5% in the last ten years.
Papillary TC has the peculiar tendency to spread to the central and lateral lymph nodes (LNs) of the neck, and recurrence occurs in 60–75% of cases. The most affected site is the central compartment.
Total thyroidectomy with radical dissection achieved the best results for differentiated TC with LN involvement, with a complication rate of 6%.
Classic radical dissection is an effective surgical approach when performed by experienced surgeons in cases in which there is a good knowledge of local anatomy, decreasing recurrence and improving survival.
INTRODUCTION
The incidence of thyroid cancer (TC) is increasing worldwide. TC is classified into subtypes according to the degree of cellular differentiation: well differentiated, including papillary and follicular TCs, and poorly differentiated including medullary and anaplastic TCs. The anaplastic TC has a worse short-term prognosis [1].
The prognosis of papillary TC is better than that of other TC types, and 10-year survival after diagnosis reaches 90%. However, lymph node (LN) involvement occurs in 80% of cases. LNs lateral with metastases are more numerous compared to those in central compartment [1, 2].
Due to the clinical implications of radical neck extensive dissection, surgical experience and familiarity with local anatomy are essential to avoid nerve and vascular injuries.
We present a rare case of classic radical dissection to treat advanced TC and invasion of neighboring structures. The results demonstrate that this type of surgical procedure is safe.
CASE REPORT
A 70-year-old female patient had a history of hypertension and underwent neck surgery 14 years before admission. The patient was transferred to the Head and Neck Surgery Department because of the detection of a large, slow-growing mass that had developed over a 2-year period on the left lobe of the thyroid. Physical examination showed a large firm deep mass measuring approximately 15 cm in diameter with irregular margins (Fig. 1A). Laboratory results were normal. Computed tomography (CT) showed a large heterogeneous mass with necrotic behavior and increased focal uptake and a mass effect on neighboring tissues, including neck muscles, without invasion of the internal carotid artery. Laryngoscopy indicated the presence of mobile vocal cords. Surgery was scheduled.
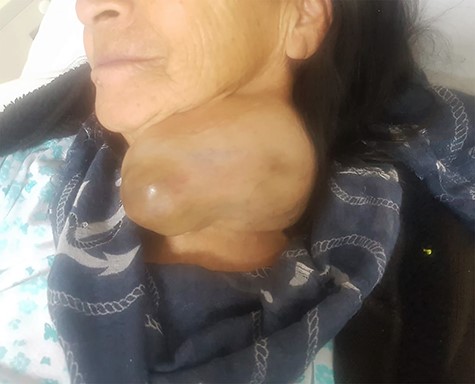
Firm mass approximately 15 cm in diameter with irregular margins located in deep tissue on the left lobe of the thyroid.
Intraoperatively, the skin was atrophic, and a firm mass on the left lobe measuring 15 × 8 × 8 cm had invaded the left jugular vein, sternocleidomastoid, omohyoid muscles and spinal nerve on the same side.
Moreover, a nodule was found on the lower aspect of the right lobe. Total thyroidectomy with classic radical dissection and advancement flap was performed, with no surgical complications (Fig. 2A–D).
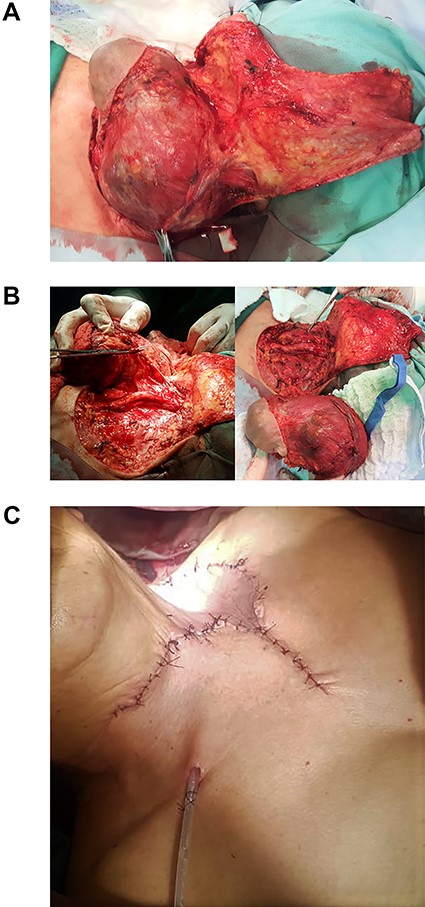
(A) Atrophic skin, lymph node tumor invading the jugular vein, sternocleidomastoid and omohyoid muscles, and ipsilateral spinal nerve. (B) Classic radical dissection. Surgical specimen. (C) Advancement flap.
Postoperatively, the flap was well perfused (Fig. 3), and there were no clinical symptoms of hypocalcaemia. However, calcium was not within normal limits and was administered orally. The patient presented XI cranial nerve palsy evidence by shoulder drop and was discharged on the third day.
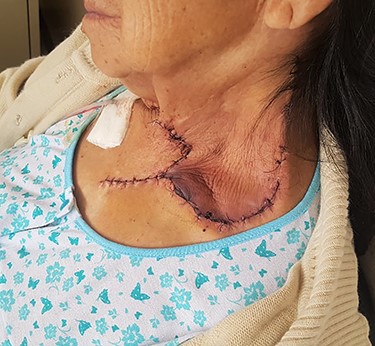
The flap was well perfused at 24 hours postoperatively. The patient presented left shoulder drop.
Pathology showed a mass size of 16 × 10 × 8 cm with lymphatic invasion and chronic inflammation, without involving cutaneous and subcutaneous tissue or compromising surgical margins. The final diagnosis was mixed papillary-follicular carcinoma (classic, oncocytic, tall cell variant).
DISCUSSION
TC is among the ten most common cancers worldwide, and epidemiological data show that the average annual incidence has increased 5% in the past ten years, and average mortality has increased 0.8% per year in the last ten years [3].
Age is one of the most important prognostic factors for mortality in patients with papillary TC. Adam et al. showed that patients who underwent surgery with a diagnosis of papillary TC, the specific-causes survival rates at 10 years were excellent for 50-year-old patients (better than 99%), but worsened with advancing age: 50–59 years, 98.1%; 60–69 years, 94.8%; 70–79 years, 91.5%; 80–89 years, 79.2%; and C 90 years, 73.9% [4].
Cervical LN metastases occur in 30–90% of diagnosed cases. The presence of cervical LN metastases decreases survival in papillary TC patients older than 45 years [3].
The most common route of spread of papillary TC is neck LNs, including central compartment (levels VI and VII), ipsilateral compartment (levels II–V) and contralateral compartment. Jumping metastases (affecting lateral LNs only) also occur [2, 3].
Metastasis to the larynx, trachea, pharynx, esophagus, recurrent laryngeal nerve, muscles or carotid artery occurs in 7–16% of patients with TC [5].
The diagnostic tools used for detecting LN metastasis include ultrasound and CT. The latter plays an important but not definitive diagnostic role because of the false-negative results due to low sensitivity and specificity. [1] The sensitivity of ultrasound and CT is low because most LNs are small and located deep in the neck tissue or behind the breastbone, preventing adequate visualization. The reported sensitivity of these two techniques is 51–67% and 62–66%, respectively [6].
The current surgical approaches to neck dissection in papillary TC with LN metastases are:
Modified radical neck dissection, with the complete removal of lateral LNs and preservation of non-lymphatic tissues, including the spinal accessory nerve, internal jugular vein and sternocleidomastoid muscle.
Selective dissection involving the removal of some LNs and preservation of non-lymphatic tissues [6].
There are controversies about extensive resection and radical surgery versus iodine treatment and radiation therapy. Studies suggest that these tumors lose their ability to take up iodine and that radiation therapy improves local control only in cases in which the largest tumor is resected. Therefore, radical surgery with subsequent reconstruction is recommended [7].
Nodal metastases of TC are important for recurrence, but do not affect survival. So, total thyroidectomy with extensive resection is recommended to reduce recurrence.
Furthermore, LN dissection performed by high-volume surgeons is technically simple and does not increase the risk of morbidity, due to nerve and vascular injuries.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.



