-
PDF
- Split View
-
Views
-
Cite
Cite
Clifford L Crutcher, John M Wilson, Kevin D Morrow, Jessica A Shields, Lindsay M Lasseigne, Frank Culicchia, Gabriel Tender, Management of cerebrospinal fluid leak from cervical gunshot wounds with external ventricular drainage: a small case series, Journal of Surgical Case Reports, Volume 2020, Issue 12, December 2020, rjaa484, https://doi.org/10.1093/jscr/rjaa484
Close - Share Icon Share
Abstract
Historically, the surgical management of gunshot wounds to the spine has been controversial. Repair of a persistent cerebrospinal fluid (CSF) leak is a generally agreed upon indication. The management of such CSF leaks typically involves lumbar drainage or direct surgical repair. Here, the authors report two cases of CSF diversion with an external ventricular drain (EVD) in patients with cervical gunshot wounds. Both patients had spinal canal obliteration or physiologic myelographic block at or below the level of injury. To the best of the author’s knowledge, these are the first two reports of successful EVD treatment of persistent CSF leaks related cervical gunshot wounds. The authors also propose a CSF treatment algorithm for cervical gunshot wounds that includes EVD.
INTRODUCTION
Gun violence continues to be an epidemiological problem for the USA. In 2018, there were 39 740 firearm related deaths [1]. Long-term gunshots to the brain and spine are particularly devastating and often leave patients with permanent neurological deficits. Cervical injures are particularly challenging as patients may be permanently quadriplegic and may require long-term ventilatory support. The estimated lifetime cost of cervical spinal cord injuries can be as high as $4 729 788 [2].
Although there is debate in literature surrounding the operative intervention related to gunshot wounds, the literature clearly supports surgical intervention in the case of persistent cerebrospinal fluid (CSF) leak. Standard treatments for CSF leaks include lumbar drainage and direct repair. There is a paucity of data in the literature regarding the use of external ventricular drains (EVDs) for difficult to treat CSF leaks related to cervical gunshot wounds. Here the authors report on two cases of patients suffering from CSF leak after gunshot wounds to the cervical spine treated with external ventricular drainage.
CASE SERIES
Case 1
History and presentation
A 24-year-old African–American male presented with a gunshot wound through the left face and neck. On exam the patient was noted to be pulseless and apneic. After resuscitation, initiation of a mass transfusion protocol and return of spontaneous circulation, the patient was GCS 11 (E4V1TM6) and was noted to have no movement in any extremities. A computed tomographic (CT) cervical spine scan and CT angiography of the neck revealed a bullet trajectory through the left C2–3 facet with fractured c3 posterior elements and a bullet fragment at the C3 level, a left vertebral artery dissection, and left internal and external carotid artery transections (Fig. 1). The patient underwent an emergent tracheostomy, neck exploration, left ICA/ECA ligation and partial wound closure. This was followed by endovascular embolization of the left vertebral artery. The patient was noted to have serosanginous drainage from the neck wound consistent with a CSF leak. After an unsuccessful trail of conservative management, a lumbar drain was placed and confirmed with fluoroscopic guidance without CSF egress. A magnetic resonance imaging (MRI) scan of the cervical spine was obtained which demonstrated a pronounced CSF fistula and a complete obstruction of the CSF space at the C3–6 levels (Fig. 2).
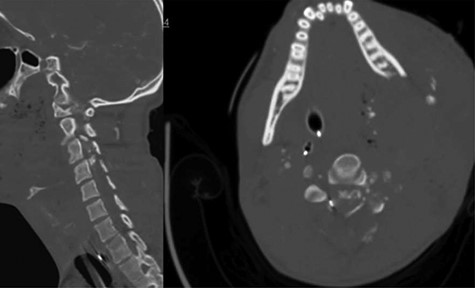
CT angiogram of the neck demonstrates a bullet trajectory through the left C2–3 facet with fractured c3 posterior elements and bullet and bony fragments within the canal at the C3–4 level; left: sagittal view; right: axial view.
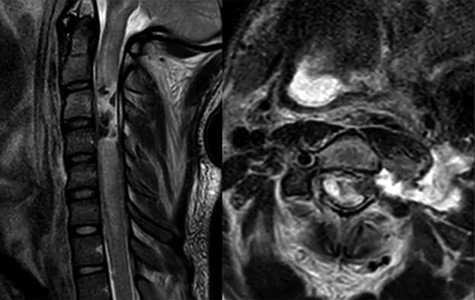
MRI T2 weighted sequence sagittal (left) and axial (right) at the c3 level demonstrates severe spinal cord damage, canal obliteration from c3 to c6 and a large left sided csf fistula at the C3 level.
An EVD was placed in the intensive care unit after informed consent was obtained. The EVD was placed under sterile conditions using local anesthesia consisting of lidocaine with 1% epinepherine and mild conscious sedation consisting of 5 mg of diazepam, and 2 mg of morphine. Ten milliliter of CSF was drained every hour. The EVD was exchanged on Day 14 as customary at our institution due minimal but persistent CSF leak. CSF diversion was continued for a total of 25 days due to the large size of the wound and the initial partial closure. The external drain was removed after a successful 48-hour clamp trial. There were no complications associated with the csf diversion. The patient remained free of CSF leak at 1 year follow-up. Dynamic cervical films revealed no gross instability and the patient remained ASIA A on ventilatory support.
Case 2
A 39-year-old African–American male presented with a gunshot wound through the right neck. The patient suffered a comminuted C6, C7 and T1 fractures with suspected right vertebral artery injury (Fig. 3). The patient was taken emergently to the operating room by the trauma surgery team for emergent neck exploration, right external jugular vein ligation and partial wound closure. The patient was noted to have a C4 ASIA A spinal cord injury. On hospital Day 2 the patient underwent a digital subtraction angiogram and embolization of a right vertebral arteriovenous fistula. On hospital Day 3, the patient was noted to have a CSF leak. Despite additional attempts to achieve a wound closure and several days of conservative management, the csf leak persisted. We decided to place an EVD because the spinal canal at c6/7 appeared completely obliterated.
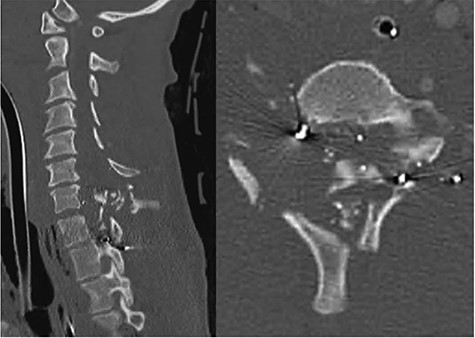
CT cervical spine; sagittal (left): demonstrates comminuted c6, c7 and T1 fractures, and the axial (right) demonstrated complete spinal obliteration with bullet and bone fragments at the C6/7 level.
An EVD was placed in the intensive care unit after informed consent was obtained. The EVD was placed under sterile conditions using local anesthesia consisting of lidocaine with 1% epinepherine and mild conscious sedation consisting of 5 mg of diazepam, and 2 mg of morphine. Ten milliliter of csf was drained every hour for a total of 7 days. The EVD as removed after a successful 48 h clamp trial. There were no complications as a result of the CSF diversion. The patient underwent a delayed C3-T3 posterior cervicothoracic fusion once the CSF fistula resolved. There patient remained free of CSF leak at 6-month follow-up and regained limited use of his left upper extremity.
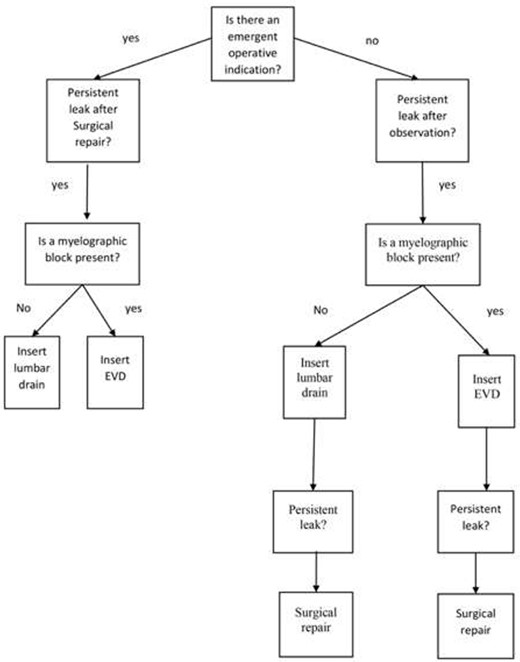
Cervical gunshot wound cerebrospinal fluid fistula treatment algorithm.
DISCUSSION
Here the authors present a small case series of CSF fistula resolution secondary to cervical gunshot wounds using external ventricular drainage without complication. Significant controversy remains in the literature regarding surgical indications for gunshot and missile injuries to the spine. However, general accepted indications for surgery include decompression or bullet removal for incomplete spinal cord injury with ongoing compression, persistent neuropathic pain, mechanical instability, concern for infection and persistent CSF leak [3–7].
The data regarding the management of cervical CSF leaks after firearm related injuries are sparse. Although Lee et al. [8] do not specifically address CSF leaks in the setting of penetrating bullet injuries, the authors provide a small series describing the use of a combination of fibrin glue, a submuscular drain, and head of bed elevation to treat traumatic cervical CSF leaks discovered after surgical decompression. Previously described treatments for thoracolumbar cerebrospinal fistula includes laminectomy with primary or patch closure of the dura with or without fibrin glue [6, 7]. The application of a lumbar drain or a lumbar drain as an adjunct to surgery has also been described in the literature with success in the thoracolumbar spine [6, 9].
Currently there are no guidelines for repairing traumatic CSF leaks [10]. It is generally accepted that persistent CSF leaks that do not resolve spontaneously should be addressed surgically. In the authors’ experience, trauma surgeons generally advocate against primary closure in gunshot blast injuries due to the significant amount of devitalized tissue and risk of infection. This is in direct opposition to the goal of preventing csf fistula formation.
In the first case presented, surgical exploration for stabilization and CSF leak repair was offered, but the patient declined, the patient then underwent CSF diversion with a lumbar drain which was ultimately unsuccessful due to a physiologic myelographic block from c3 to c6 (Fig. 2). Ultimately the csf fistula was treated successfully after placement of an EVD. In the second case, there was a high index of suspicion of a csf block at the level of injury and a lumbar drain was not placed. The patient was successfully treated with CSF diversion through EVD for 7 days.
In the setting of a cervical gunshot wound with csf fistula, the authors propose a new treatment algorithm (Fig. 4) flowchart developed based on our clinic experience and a thoughtful review of the literature. Patients initially deemed nonoperative patients should be observed for spontaneous resolution. Patients should be evaluated for a myelographic block with either a CT myelogram or MRI if the leak persist. A lumbar drain can be placed if there is no myelographic block. In patients where a lumbar drain is ineffective secondary to a myelographic block or severe canal narrowing, an EVD should be considered followed by surgical exploration and repair. In operative patients, a primary closure or patch repair should be attempted with fibrin glue. An adjuvant lumbar drain should be considered. In the setting of severe arachnoiditis, adhesion formation or myelographic block an EVD should be used if csf leak persist despite surgical repair. Although, the authors do not have direct experience with csf fistula related to thoracic gunshot wounds, a similar algorithm seems reasonable. The current treatment algorithm was developed through our clinical experience and thoughtful review of the literature. The authors recognize that our findings are limited by the small size of our case series, and that a larger series or prospective trail may provide more information.
CONCLUSION
CSF diversion via an EVD is a viable and safe option for treating CSF leaks from cervical gunshot wounds if other treatment modalities have been unsuccessful.
DISCLOSURES
The authors have no financial disclosures.
CONFLICT OF INTEREST STATEMENT
None declared.



