-
PDF
- Split View
-
Views
-
Cite
Cite
Eivor Alette Laugsand, Athanasios Xanthoulis, Management of a life-threatening intercostal artery bleeding, difficult to visualize in open surgery: a case report, Journal of Surgical Case Reports, Volume 2020, Issue 10, October 2020, rjaa444, https://doi.org/10.1093/jscr/rjaa444
Close - Share Icon Share
Abstract
Life-threatening bleeding from an intercostal artery is a rare and challenging event. A 74-year-old patient with a right-sided pleural effusion was treated by a pigtail pleural drain. He developed a large haemothorax, initially addressed by a large bore chest tube. As he became haemodynamically unstable, he required an emergency anterolateral right thoracotomy. It was difficult to visualize and reach the bleeding vessel during open surgery. A 30° laparoscopy camera was introduced and the bleeding site was identified. An incision was made directly over the bleeding site and the two ends of the lacerated intercostal artery were ligated by two externally placed figure-of-eight sutures. The patient survived and recovered fully. As most general surgeons, even at smaller hospitals, are familiar with laparoscopy, the technique described here may be useful for other surgeons to employ if a life-threatening intercostal artery injury occurs.
INTRODUCTION
Intercostal artery (ICA) injury is a rare but feared complication to common elective and emergency thoracic procedures such as thoracentesis, pleural biopsy, thoracoscopy or chest drain insertion [1]. It can also occur in penetrating or blunt thoracic trauma, or it may occur spontaneously [2, 3]. As the tortuosity of intercostal arteries and traversing collaterals increase with age, older people are at higher risk [4].
A cause of fatality in ICA injury is not recognizing it and/or not initiating prompt management [1]. Chest X-ray (CXR) and ultrasound are reliable primary tools to establish the diagnosis of a pleural effusion in stable patients, whereas ultrasound alone may be preferred in trauma [5]. A contrast-enhanced computed tomography (CT) scan of the chest is indicated, if opacity persists on CXR after placement of a chest tube in a haemodynamically stable patient [5]. In unstable patients, there may not be time for refined imaging.
Regardless of the cause, most patients with a haemothorax can be adequately treated with chest tube insertion, fluid resuscitation and/or transfusion of blood products [5]. If the bleeding is not self-limiting, the most common treatment options are thoracotomy or endovascular embolization [5]. In hospitals without thoracic surgeons or interventional radiologists, an emergency thoracotomy may be the only option if the patient is haemodynamically unstable with a massive haemothorax [5]. Even with an open chest, identification and control of the bleeding vessel can be challenging [6].
CASE REPORT
A 74-year-old male patient with a history of type 2 diabetes mellitus, ankylosing spondylitis and cystoprostatectomy with Bricker bladder was admitted with acute renal failure not responding to conservative measures. He needed haemodialysis. Due to clinical deterioration with dyspnoea, hypotension and inadequate peripheral perfusion during intermittent haemodialysis, he was transferred to the intensive care unit (ICU). A right-sided pleural effusion was found, and the intensivist inserted a pigtail pleural drain under ultrasound guidance. The fluid was somewhat bloody, but control with ultrasound and CXR (Fig. 1) after the procedure was normal.
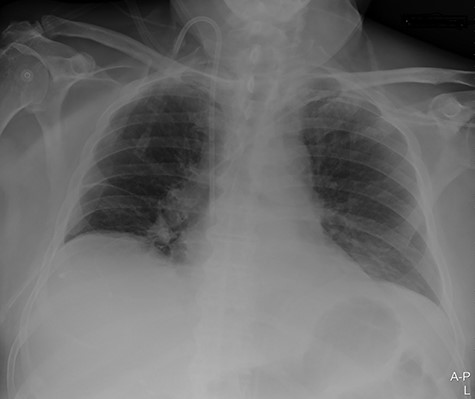
Portable chest X-ray with no pleural effusion after placement of pigtail pleural drain.
Our surgical team was contacted after 4 h, as the pleural fluid had become grossly haemorrhagic. A CXR showed haemothorax (Fig. 2). Upon clinical deterioration, the patient was intubated, and a 24Ch chest tube was introduced. Approximately, 500 ml of blood was immediately drained, followed by 300 ml during the first 30 min. ICA laceration was suspected. Despite transfusion of red blood cells and plasma and infusion of noradrenaline, the patient remained circulatory unstable. A new CXR showed massive haemothorax despite drainage (Fig. 3). The patient was now utterly haemodynamically unstable and not suited for transportation. As there are no thoracic surgeons or interventional radiologists in our hospital, the general surgeons decided to take him to the operating theatre. A wide anterolateral right thoracotomy was performed with patient lying in left lateral decubitus position. The right pleural cavity was full of fresh and coagulated blood. The pulsating bleeding was seen coming from the posterolateral, caudal chest wall, but the exact site deep down in the sharp costophrenic angle could not be localized and was inaccessible for any surgical haemostatic manoeuvre.
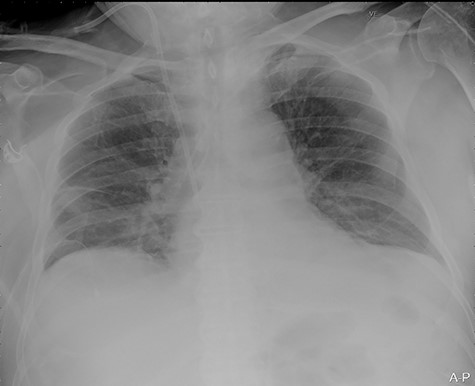
Portable chest X-ray in half-upright position showing haemothorax 4 h after placement of pigtail pleural drain.
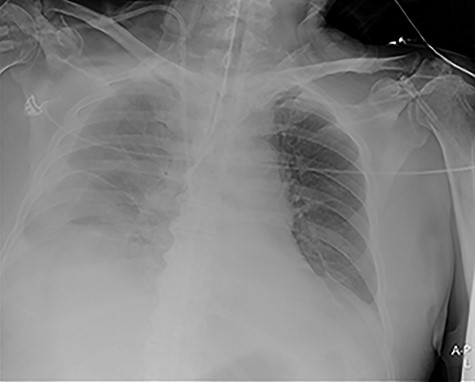
Portable chest X-ray in half-upright position showing massive haemothorax despite chest tube.
A 30° laparoscopy camera was introduced through the thoracotomy and the bleeding site was identified. The skin and subcutaneous tissue were incised directly over the injured artery. Under direct visualization by the laparoscope, the two ends of the injured artery were suture ligated by means of two externally placed figure-of-eight sutures of absorbable polyglactin 2-0. This manoeuvre controlled the bleeding effectively. Two chest drains were introduced, and the thoracotomy was closed in layers. The patient was transported to the ICU. The two chest drains were removed at 6th and 8th postoperative day, respectively. The patient survived and recovered fully, but died of lymphoma >6 months after surgery.
DISCUSSION
ICA injury can be life-threatening or even fatal. In our case, a life-threatening bleeding occurred as a complication to thoracentesis. Thoracentesis is a common bedside procedure, with few complications. The incidence of haemothorax after thoracentesis is 0.01–0.1% [7]. Older patients with advanced renal insufficiency and severe coagulopathy, as ours, are considered at increased risk [7]. As recommended, the pleural drain in this case was introduced by advancing the needle above the superior aspect of the rib under ultrasound guidance [4]. However, the degree to which the ICA is exposed within the intercostal space varies significantly [8], and the sensitivity for detection of ICA by ultrasound is 0.86 when compared with CT [9].
Haemothorax caused by ICA injury should be suspected with signs of circulatory instability, respiratory distress and accumulation of pleural fluid after chest trauma or thoracic procedures. Signs of complex echogenic or septated effusions are early ultrasonographic features of haemothorax [7]. In hospitals with thoracic surgeons and equipment for video-assisted thoracic surgery available, minimally invasive methods for definitive ICA ligation may be possible [10]. Although embolization therapy may be an alternative, an urgent thoracotomy is still the procedure of choice for massive haemothorax or persistent bleeding [5]. A thoracotomy may even be warranted at a lower bleeding rate in haemodynamically unstable patients not transportable to a hospital with interventional radiology suite or thoracic surgical expertise.
Controlling bleeding from intercostal arteries can be technically difficult and several options exist. Haemostatic clips or suture ligation can be used for readily accessible bleeding sites, whereas blind figure-of-eight sutures proximally and distally can be used for challenging ones. In such cases, keeping the path of the needle parallel to the ribs is essential, as the intercostal space only allows limited movement of the needle [6]. If anything else fails, placement of proximal and distal sutures around the nearest rib including the entire intercostal vascular bundle and tying the artery up against the rib works, but comes at a cost of postoperative neuralgia [6].
In our case, we used the two figure-of-eight sutures [6], but we placed them externally and under the visualization of a 30° laparoscope. As most general surgeons are familiar with laparoscopy and the equipment is readily available, this approach may be time- and life-saving in smaller hospitals without thoracic surgeons or interventional radiologists.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
ETHICAL STATEMENT
All applicable international, national and institutional guidelines were followed. Written, informed consent was given to publish all information obtained from the study participant.
AUTHORS’ CONTRIBUTIONS
Both authors performed the surgery, wrote the manuscript and approved the final version of it.
ACKNOWLEDGEMENT
The authors would like to thank Arne Sollie (MD) for his valuable contribution during surgery.
REFERENCES
Author notes
Eivor Alette Laugsand and Athanasios Xanthoulis contributed equally to this work



