-
PDF
- Split View
-
Views
-
Cite
Cite
D G E Thiem, B Al-Nawas, P W Kämmerer, Ankylosis of the temporomandibular joint—impression free CAD/CAM based joint replacement using patient-specific implants, Journal of Surgical Case Reports, Volume 2020, Issue 10, October 2020, rjaa416, https://doi.org/10.1093/jscr/rjaa416
Close - Share Icon Share
Abstract
In recent years, alloplastic temporomandibular joint (TMJ) replacement has become a permissible procedure for the reconstruction of severely destroyed TMJs. The use of computer-aided design/computer-aided manufacturing (CAD/CAM) has extended the range of applications to complex anatomical situations. The aim of the treatment is to improve the usually restricted mouth opening and thus oral hygiene and nutrition, which leads to a regular improvement in the general quality of life. The following case report describes the bilateral replacement of ankylotically destroyed TMJs using patient-specific endoprostheses with simultaneous displacement of the maxilla. Innovative in the case described is the impression-free CAD/CAM planning, whereby the upper and lower prostheses were produced on the basis of 3D printed patient models.
INTRODUCTION
Ankylosis of the temporomandibular joint (TMJ) involves bony fusion of the mandibular condyle to the skull base. Depending on its aetiology, a distinction is made between an intra- and extra-articular form. While the former mainly results from trauma and infection, extraarticular ankylosis is a consequence of periarticular tumour growth, prolonged coronoid process [1], ossifying myositis, scarring, radiation or trismus. Epidemiologically, trauma-induced ankylosis is considered the most frequent type that develops from fibrous organization of haematoma with subsequent ossification. In Europe, the incidence of TMJ ankylosis is declining, with affected patients frequently reporting falls in childhood. In this context, fractures of the condyle often remain undiagnosed due to overshadowing soft tissue injuries of the chin [2]. Early diagnosis and the initiation of appropriate therapy (surgical or conservative/orthodontic) are of particular importance, since children under 10 years of age are predisposed to develop post-traumatic ankylosis and treatment is difficult due to growth and high rates of re-ankylosis [3–5]. Reasons for late diagnosis are slowly decreasing mouth opening without pain, thus ankylosis often manifests itself only in advanced stages [6]. The leading symptoms are progressive mandibular hypomobility, reduced food intake and malnutrition, communication restrictions, dysphagia, malocclusion, pain, facial asymmetries (retrognathia/micrognathia), snoring, obstructive sleep apnoea and poor oral hygiene. In accordance with the current guidelines, therapy goals are permanent ankylosis elimination, improvement of mandibular mobility and function, pain relief, improvement of oral/dental hygiene, upper airways’ obstruction removal, improvement of occlusion and communication skills and aesthetics [5]. The therapeutic concepts are divided into conservative and surgical procedures, with the latter following the former, as ankylosis can only be treated surgically.
CASE REPORT
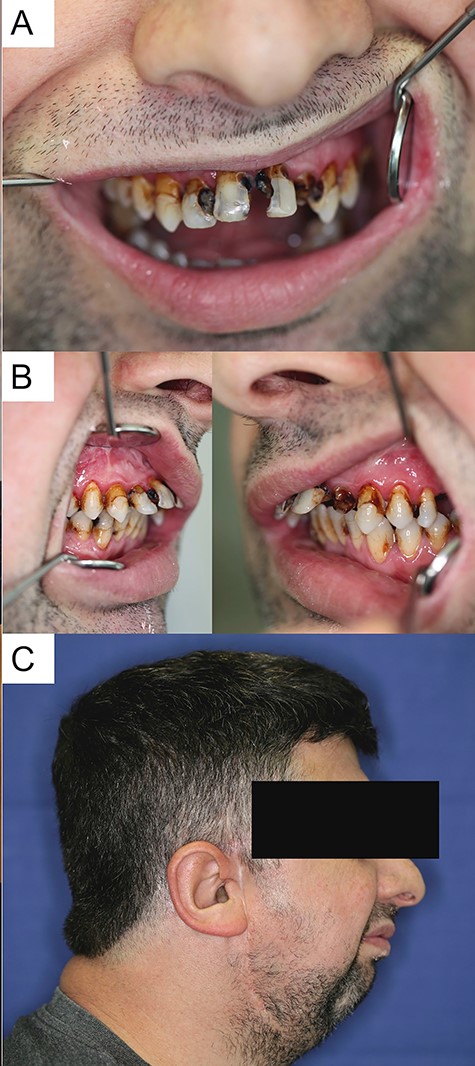
A 37-year-old patient presented himself in the outpatient consultation hours of the Department of Oral and Maxillofacial Surgery of our institution after referral by his general dentist for dental rehabilitation. The clinical examination revealed an extensive need for dental restoration, a skeletal class II with 7-mm distal bite, maxillary hypoplasia and a strongly restricted mouth opening (maximum incisal edge distance of 1.0 cm) (Fig. 1A–C). In addition, the patient who relied on forearm crutches, suffered from obesity (BMI > 40), load-dependent dyspnoea and an obstructive sleep apnoea syndrome, which forced him to sleep in an upright position. The medical history revealed a TMJ replacement via a costochondral graft on the right due to TMJ arthrosis resulting from fall in childhood with bilateral untreated condyle fracture. TMJ imaging was carried out using cone-beam computed tomography (CBCT) on the day of the first presentation. According to Sawhney and Wilkes, CBCT confirmed the suspected diagnosis of a bilateral TMJ-ankylosis Wilkes-Type-IV on the right and type-III on the left side (Fig. 2A and B). The interdisciplinary surgical-prosthetic treatment concepts’ central components were bilateral alloplastic TMJ replacement using patient-specific implants (PSI), maxillary forward displacement (1 cm) with anterior (2 mm) and dorsal impaction (4 mm) and the fabrication of an upper and lower partial prosthesis for occlusion encryption, carried out as 3D-Virtual-Backward-Planning. The prostheses were fabricated solely based on the 3D printed patient models, since a sufficient intraoral impression was not possible due to the restricted mouth opening (Fig. 3A–C). After tooth restoration and prostheses insertion, LeFort-I-osteotomy, realignment and osteosynthesis were performed using a computer-aided design/computer-aided manufacturing (CAD/CAM) fabricated occlusal splint. A corticocancellous bone graft from the iliac crest was simultaneously raised and inserted as an interposition osteoplasty to increase the bony attachment following the maxillary displacement (Fig. 4A and B). The right TMJ was exposed by extending the preauricular approach along the existing scar to the retro/submandibular region, whereby the left TMJ was visualized via a preauricular and additionally retromandibular approach extended to the parietal region. The ankylotic mass/former TMJ was then resected on both sides including zygomatic arches’ base modulation for support-surface preparation for the fossa components (Zimmer-Biomet-Holdings, Warsaw, IN, USA) (Fig. 5A–D). After insertion of the mandibular prosthesis and the final occlusal splint, the patient-specific TMJ prostheses (Zimmer-Biomet-Holdings, Warsaw, IN, USA) (Fig. 6) were inserted and fixed to the local mandible via osteosynthesis screws. The postoperative course was inconspicuous, so that the patient could be discharged after 10 days for home care and outpatient follow-up. Following 3 weeks of moderate mouth-opening training using a wooden spatula, movements were intensified using the TheraBite-System® (Atos Medical GmbH, Germany). The system was used according to the manufacturer’s recommendation, consisting of seven daily applications with seven stretches for 7 s each. After 6 months, mouth opening was increased to 4.2 cm. Furthermore, the patient lost 20 kg of body weight and his general condition improved significantly, which enabled him to sleep in a lying position (Fig. 7A and B).
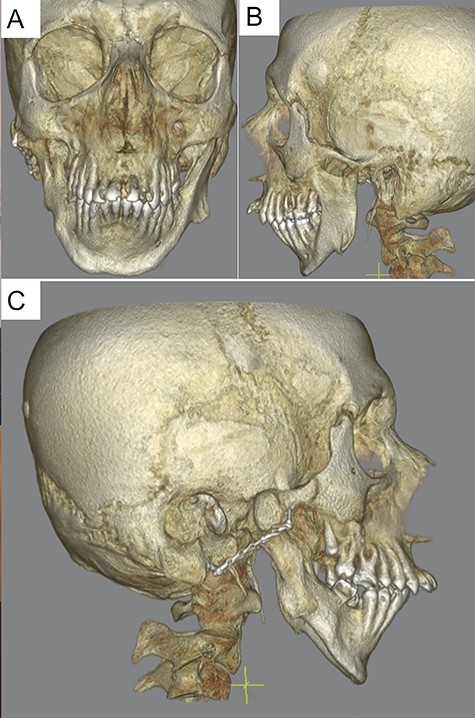
Preoperative computed tomography after initial presentation with a presentation of the bilateral deforming arthrosis of the temporomandibular joint.
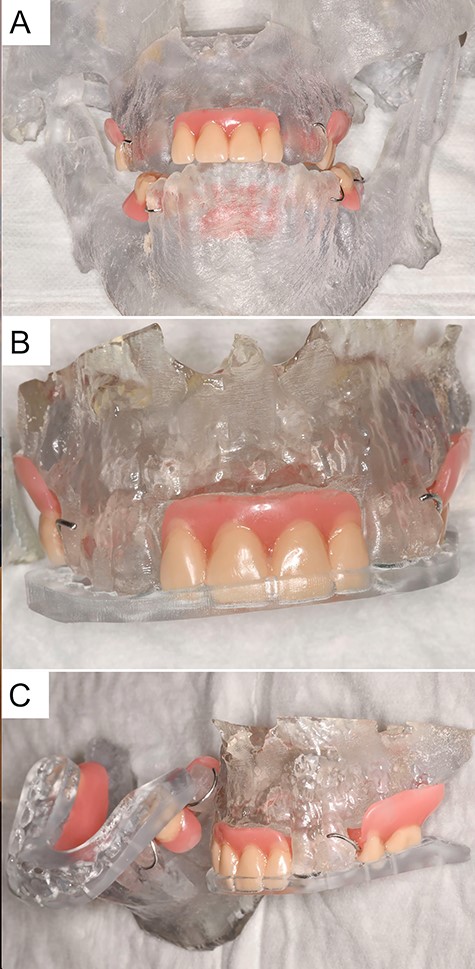
Patient 3D model with an integrated prosthesis in the upper and lower jaw as well as an intermediate and final occlusal splint.
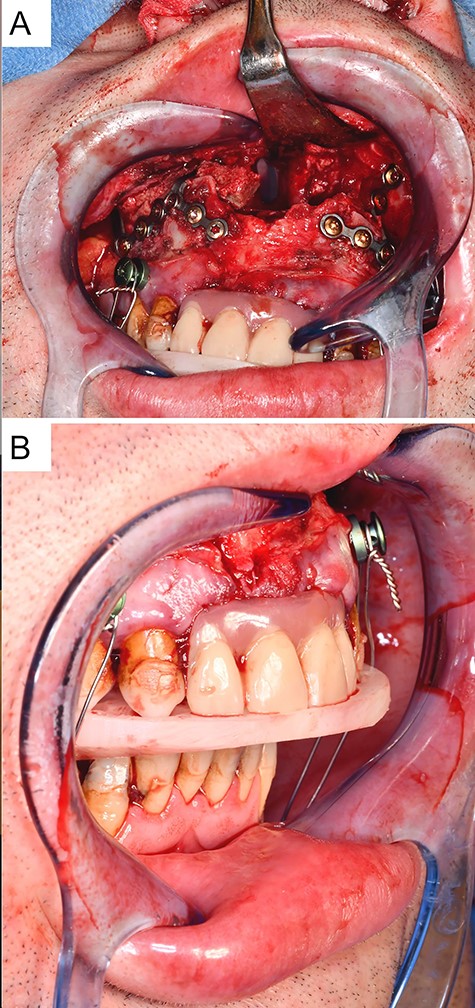
Intraoperative situation with (A) presentation of the osteosynthetically fixed interposition osteoplasty in the maxilla after LeFort-I-osteotomy and advancement of the maxilla, and (B) intermediate position after advancement of the maxilla with an intermediate splint and rigid intermaxillary fixation.
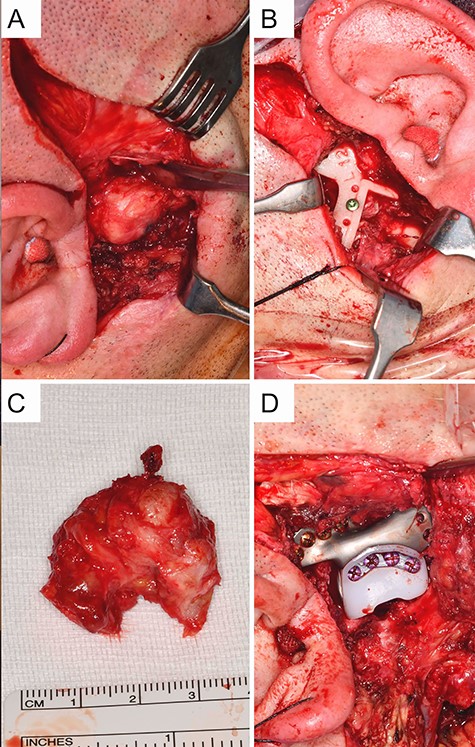
Intraoperative situation with (A) exposed view of the ankylosed deformed temporomandibular joint on the right via a preauricular approach, (B) shows the inserted resection template on the left, (C) resected ankylotic mass, (D) osteosynthetically fixed fossa component on the right (Zimmer Biomet Holdings, Warsaw, IN, USA).
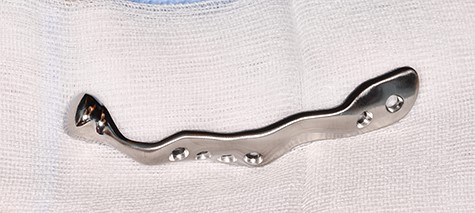
Patient-specific TMJ implant of the right side (Zimmer Biomet Holdings, Warsaw, Indiana, USA).
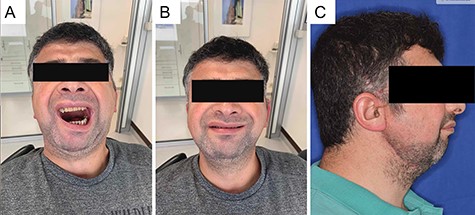
Clinical situation 6 months after surgery with increased mouth opening with integrated prostheses in the upper and lower jaw and overall improved general health condition.
DISCUSSION
The current guidelines on ankylosis and mandibular hypomobility recommend early surgery for progressive ankylosis due to higher complications in advanced stages. Surgical concepts of TMJ ankylosis include TMJ expansion under sedation or general anesthesia, arthroplasty, partial autologous or alloplastic and total alloplastic replacement. In order to avoid re-ankylosis, resective procedures place particular emphasis on complete removal of the ankylotic mass and early postoperative mobilization [5, 7]. Advanced stages with extensive resections and height reduction require reconstructive measures. Computer-aided (CAD/CAM) planning and fabrication of PSI for complex anatomical conditions (deformation, preliminary operations) has become the gold standard and dates back to 1974. While alloplastic materials are used almost exclusively in adults, autologous costochondral grafts are still recommended in children due to their growth potential, despite considerable undesirable side effects [5]. However, facing modern materials, alloplastic TMJ replacements in adolescents with severe (re-)ankylosis and failed autologous grafts are again discussed under consideration of strict indication criteria [8]. Proponents emphasise the advantages such as shorter operation times and length of stay, no need for graft vascularisation, avoidance of donor side morbidity, postoperative loading and the correction of severly deformed TMJs while accepting the risk of possible prosthesis exchanges during the further course [4, 8]. Although the indication for TMJ replacement has become more common [9] and the durability of the modern prosthesis is estimated at over 20 years [10], joint replacement remains the ultima ratio in patients with severely damaged TMJs without response to conservative or minimally invasive therapies [4].
FUNDING
The authors have nothing to disclose. No financial funding was received.



