-
PDF
- Split View
-
Views
-
Cite
Cite
Kazuaki Nemoto, Masanori Okamoto, Munehisa Kito, Kaoru Aoki, Shuichiro Suzuki, Akira Takazawa, Yasuo Yoshimura, Hiroyuki Kato, Combined treatment using Mohs’ paste and neoadjuvant chemotherapy for giant gluteal soft tissue sarcoma with malignant fungating wound: a case report, Journal of Surgical Case Reports, Volume 2019, Issue 5, May 2019, rjz137, https://doi.org/10.1093/jscr/rjz137
Close - Share Icon Share
Abstract
A malignant fungating wound is a cutaneous infiltration of malignant tumor or metastatic lesion that develop into ulceration. Local control is often difficult to obtain, because the Quality of Life of patients can decrease considerably due to bleeding, exudation, odor and pain from the wound. There are few studies in the literature that report the use of Mohs’ paste for soft tissue sarcoma with malignant fungating wound. We report a case resulting in good local control for a patient with dedifferentiated liposarcoma with gluteal ulceration by the combined use of Mohs’ paste and chemotherapy as a pre-operative adjuvant therapy. Mohs’ paste controlled the infection, odor and exudation in approximately 2 weeks, and good visualization of the surgical field was obtained due to tumor volume reduction. We found that Mohs’ paste is effective as a neoadjuvant therapy for disintegrated soft tissue sarcoma.
INTRODUCTION
A malignant fungating wound (MFW) is a cutaneous infiltration of malignant tumor or metastatic lesion that develop into ulceration [1]. Due to bleeding, exudation, odor, contact pain and frequent wound care, the Quality of Life of patients can decrease considerably and local control is often difficult to obtain. We report a case of effective treatment using Mohs’ paste for MFW in giant gluteal soft tissue sarcoma.
CASE REPORT
A 74-year-old male presented to our institution with soft tissue sarcoma in the left gluteal region and bleeding from the tumor (Fig. 1A). The perianal tumor was 15 cm in size. Redness, exudation and fetid odor were observed, and the patient exhibited poor mobility compared to baseline. Although the Eastern Cooperative Oncology Group Performance Status was 0 [2], the patient was unable to tolerate the supine position due to the giant tumor mass and also required assistance for defecation. On contrast-enhanced MRI, a tumor with fatty component was revealed primarily inside the left gluteus maximus muscle (Fig. 2A and B). On culture examination, Streptococcus gallolyticus, Bacteroides fragilis and Enterococcus avium were identified from the wound exudate, which was suggestive of an infection concurrent with the tumor. The needle biopsy indicated a spindle cell tumor with positive immunostaining for MDM2 and Cdk4. Based on these findings, the left gluteal region was diagnosed as dedifferentiated liposarcoma with wound infection and American Joint Committee on Cancer Stage III (T2bN0M0, high grade).
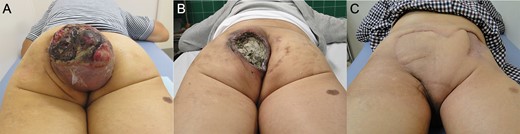
Photograph. (A) At first examination, the tumor was disintegrated and exposed with fetid odor and exudation. (B) The protruding areas of the tumor were resected after tissue fixation using Mohs’ paste. (C) At 6 months postoperatively, the patient is making satisfactory progress.
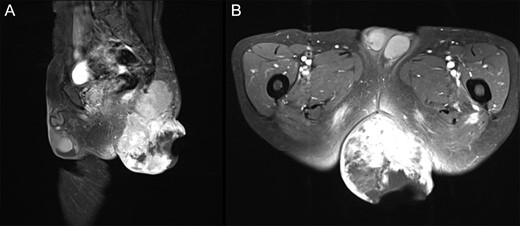
T1WI contrast-enhanced MRI with fat suppression at first visit. (A) Sagittal image. (B) Axial image. Left gluteal region: a 15 cm tumor extending from the gluteus maximus muscle to the subcutaneous tissue with enhancement of irregular margins was observed. A portion of the tumor had disintegrated, and the internal mass was heterogeneous.
Two months after initial examination, the patient was hospitalized at our department. To prevent a secondary infection from defecation, we first performed an artificial anastomosis. Mohs’ paste was subsequently applied a total of 16 times over 3 months. The wound infection improved 2 weeks after administering Mohs’ paste and antibiotics (ampicillin/sulbactam). After the infection subsided, three courses of neoadjuvant chemotherapy (Doxorubicin) were performed. The disintegrated portion of the tumor recessed by using Mohs’ paste, and the bleeding, exudation and odor subsided. Moreover, the patient was able to tolerate both sitting and supine positions (Fig. 1B). The contrast-enhanced MRI revealed that the protruding area of the tumor was resected with no increase in the internal tumor size (Fig. 3A and B). One day prior to curative surgery, embolization of the left inferior gluteal artery.
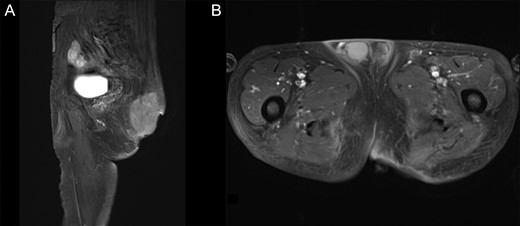
Pre-operative T1WI contrast-enhanced MRI with fat suppression. (A) Sagittal image. (B) Axial image. The protruding tumor was resected, and the internal tumors showed no considerable changes in size.
Five months after initial examination, surgical wide resection (combined with anorectal resection) was performed and reconstruction by right inferior gluteal artery perforator flap with split thickness skin grafting. The histopathological imaging revealed a palisading arrangement of atypical spindle cells in the tumor tissue. The area treated with Mohs’ paste appeared denatured, turned ashen, exhibited cell destruction, and was believed to be necrotic (Figs 4 and 5A and B). Radiotherapy (60 Gy/30 fr) and one course of chemotherapy (Ifosfamide) were performed postoperatively. There was no local recurrence at 6 months postoperatively (Fig. 1A), and good progress was observed with a Musculoskeletal Tumor Society Score of 93% and Toronto Extremity Salvage Score of 43%.
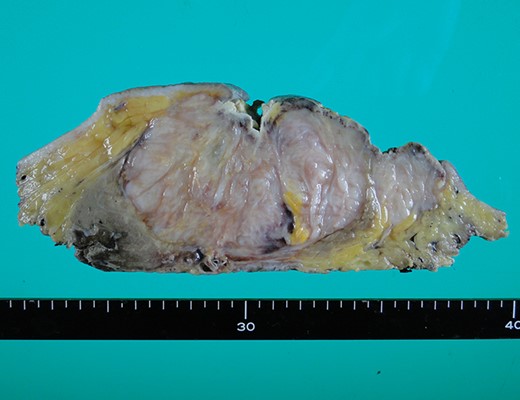
Histopathological finding. Macroscopic image. Area treated with Mohs’ paste was denatured and appeared grayish white.
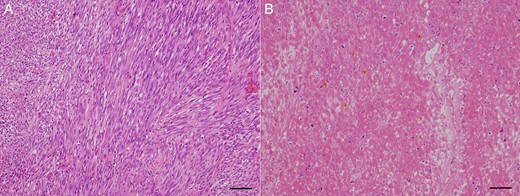
Histopathological finding. (A) Micro-image. Viable residual tumor was observed. Scale bar: 500 μm. (B) Micro-image. Tissue imaging showed necrosis in area treated with Mohs’ paste. Scale bar: 500um.
DISCUSSION
The following problems were encountered in this case: inability to tolerate the supine position due to the giant tumor mass, inability to defecate independently, exposure of the tumor due to disintegration, concurrent infection and poor visualization of the surgical field on the anal side. Therefore, an artificial anus was first constructed to prevent a secondary infection, and Mohs’ paste was used to treat the MFW of the disintegrated tumor.
The control of its infection, odor, exudation, bleeding, pain, and mental distress are important in the treatment of MFW [3]. In this case, infection was accompanied by disintegration of the perianal tumor, fetid odor and exudation; however, these symptoms rapidly improved by using Mohs’ paste. Within 2 weeks, the infection was under control, enabling systemic chemotherapy with doxorubicin. No remarkable reduction in the internal tumor diameter was observed, and only the protruding section from the body surface was resected after applying Mohs’ paste.
Mohs’ paste was devised as a method to chemically fix and remove superficial tumors with zinc chloride in the 1930s [4]. The fixative is currently used in the field of dermatology for malignant tumors and breast cancers that infiltrate the skin [5]. For squamous cell carcinoma of the skin, it is used for curative treatment [6] and palliative treatment [7]. Little has been reported on its use for soft tissue sarcoma, except for one report on the palliative treatment of angiosarcoma [8]. There are no reports that describe the combined use of Mohs’ paste with neoadjuvant chemotherapy.
The original composition of the paste includes stibnite and sanguinaria canadensis; however, due to availability in Japan, our paste consisted of zinc chloride (70 g), zinc oxide (15 g), starch (15 g), purified water (25 ml) and glycerin for adjusting its viscosity. Written informed consent was obtained under the permission of the institutional ethics review committee prior to its use.
A 1-mm thick layer of Mohs’ paste has a fixative penetration depth of up to 5 mm in 48 h and 10 mm in 72 h, and the application time between 15 min and 3 h is common, depending on cases and the purpose of treatment [5]. In this case, petroleum jelly was used to protect the surrounding healthy skin, and Mohs’ paste was applied for 10–30 min according to pain. The paste was subsequently washed, necrotic sections were removed after 2–3 days, and the paste was reapplied to repeat the process. Necrosis was confirmed with a thickness of approximately 5 mm in the histopathological image of the resected specimen.
Mohs’ chemosurgery is a tissue fixation technique wherein tissues fixed by Mohs’ paste are repeatedly excised with a scalpel until the complete histopathological removal of the tumor is achieved for curative and palliative treatment of local invasion in malignant skin tumor and breast cancer [9, 10]. In this case, Mohs’ paste enabled the resection of the tumor from the body surface to facilitate a supine position. Furthermore, a good visualization of the surgical field was obtained. Mohs’ paste proved to be a suitable treatment as a neoadjuvant therapy for giant soft tissue sarcoma with MFW.
ACKNOWLEDGEMENTS
We would like thank the contributing departments at our institution for their support in this treatment.
CONFLICT OF INTEREST STATEMENT
None declared.



