-
PDF
- Split View
-
Views
-
Cite
Cite
Badria Aljohani, Fatima Ali, Entisar Mohieldeen, Bayan Alharbi, Nipple neuroma presenting as focal asymmetry: diagnostic challenges and clinical implications at King Salman bin Abdulaziz Medical City, Journal of Surgical Case Reports, Volume 2026, Issue 2, February 2026, rjag051, https://doi.org/10.1093/jscr/rjag051
Close - Share Icon Share
Abstract
Traumatic neuromas are benign nerve proliferations that arise as reparative responses after injury, rather than true tumors. They are common in extremities and head–neck sites but rarely occur in the breast, particularly within the nipple–areolar complex. We report the case of a 49-year-old woman with persistent nipple discomfort. She denied nipple discharge, bleeding, or trauma. Blood tests revealed mild anemia and reduced potassium. Her history included right breast surgery for abscess drainage 4 years earlier. No personal or family history of breast or ovarian cancer was reported. Imaging suggested a benign lesion, but surgical excision confirmed a nipple neuroma. Grossly, the excised nipple lesion measured 1.4 × 1.2 × 0.6 cm with a firm whitish cut surface. Histopathology showed disorganized fascicles of peripheral nerve fibers within the dermis. This case illustrates diagnostic difficulties and reinforces the importance of distinguishing neuroma from recurrent malignancy.
Introduction
Traumatic neuroma (TN) represents a reactive hyperplastic process following partial or complete nerve transection. It consists of tangled axons, Schwann cells, and fibrous tissue [1]. Although well documented in amputation stumps, neck dissections, and limb surgeries, breast-related neuromas are exceptionally uncommon. Fewer than 15 cases have been described, usually near mastectomy scars [2, 3]. Involvement of the nipple is particularly rare.
Clinically, TN presents as a small painful or tender nodule, often less than 2 cm, sometimes eliciting tingling on palpation (Tinel’s sign) [4]. Pain may be described as burning, stabbing, or gnawing [5]. Because of their overlap with recurrent breast carcinoma in clinical and radiological appearance, neuromas pose significant diagnostic dilemmas. We present an unusual case of nipple neuroma arising 4 years after breast surgery.
Case presentation
A 49-year-old postmenopausal woman presented with tingling pain localized to the right nipple. She denied nipple discharge, bleeding, or trauma. Her history included right breast surgery for abscess drainage 4 years earlier. No personal or family history of breast or ovarian cancer was reported.
On examination, there was no palpable lump, nipple retraction, discharge, or skin abnormality. The contralateral breast and regional lymph nodes were unremarkable.
Blood tests revealed mild anemia (Hb 10.5 g/dl, hematocrit test [HCT] 33.3%) and slightly reduced potassium (3.49 mmol/l) as mentioned in Table 1. Other laboratory values were within reference limits.
| Test name . | Result . | Normal range . |
|---|---|---|
| HGB (hemoglobin) | 10.50 | 11.6 to 15 g/dl |
| HCT (hematocrit test) | 33.30% | 35–45% |
| Potassium | 3.49 (mmol/l) | 3.5–5.2 (mmol/l) |
| Test name | Result | Normal range |
|---|---|---|
| HGB (hemoglobin) | 10.50 | 11.6 to 15 g/dl |
| HCT (hematocrit test) | 33.30% | 35–45% |
| Potassium | 3.49 (mmol/l) | 3.5–5.2 (mmol/l) |
Bilateral mammography and ultrasound (January 2025) demonstrated focal asymmetry with ductal changes in the right breast, categorized as Breast Imaging Reporting and Data System (BI-RADS) 3. The left breast contained a simple cyst. No suspicious calcifications, architectural distortion, or abnormal lymph nodes were observed. Given persistent symptoms, excisional surgery was undertaken.
Grossly, the excised nipple lesion measured 1.4 × 1.2 × 0.6 cm with a firm whitish cut surface. Histopathology showed disorganized fascicles of peripheral nerve fibers within dermal and subepidermal fibrous tissue, without atypia or malignancy. Final diagnosis was reported as traumatic neuroma of the nipple. Postoperatively, the patient recovered uneventfully with symptom resolution and no recurrence during follow-up.
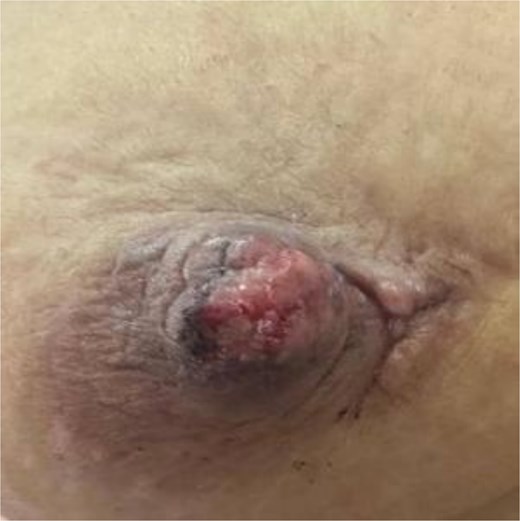
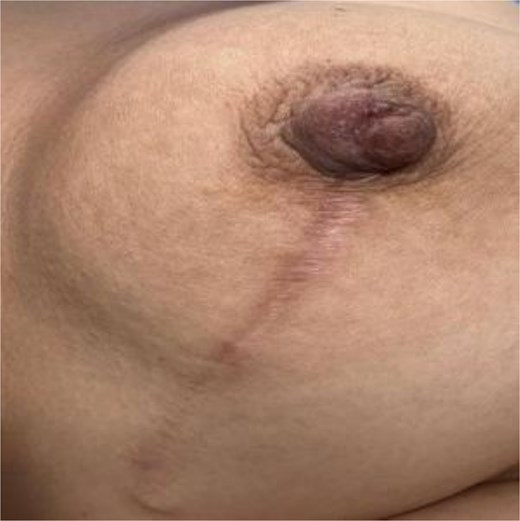
However, given the patient’s persistent symptoms and imaging features of focal asymmetry with ductal changes. Histopathological analysis revealed features consistent with a nipple neuroma, characterized by proliferation of non-malignant peripheral nerve fibers within the dermis and subepidermal region of the nipple (Fig. 1). A surgery have been done for scar excision and nipple correction post operative (Fig. 2).
Discussion
TN is a reactive hyperplasia rather than a true tumor, usually develops after nerve injury. It consists of interlacing nerve fascicles embedded in fibrotic tissue [1]. According to Foltan et al., TN arises when simultaneous nerve regeneration and fibrous proliferation entrap regenerating fibers, producing chronic proliferative changes [1]. Two forms are described: spindle neuromas, from chronic irritation of intact nerves, and terminal neuromas, following nerve transection [6]. Breast-related TNs, especially at mastectomy scars, are terminal type, typically found in pectoralis muscle or subcutaneous fat, often asymptomatic, and associated with thoracic or intercostal nerve injury [7].
Imaging generally reveals benign features. On mammography, TN appears as a small, circumscribed nodule or focal distortion [8, 9]. Ultrasound typically shows an oval, well-defined, parallel-oriented hypoechoic mass with absent vascularity and occasionally the “tail sign” indicating continuity with a nerve [10]. Magnetic resonance imaging findings include T1 isointensity, T2 hyperintensity, and benign enhancement [10]. On computed tomography (CT), rare descriptions show isoattenuation to adjacent muscle [10].
Histologically, TNs consist of disorganized axons, Schwann cells, and fibroblasts within fibrous stroma. Rosso et al. described associated granular cell changes, mucinous stroma, mast cell infiltration, and reticulin fibers—features also observed in some TNs, resembling Wallerian degeneration but distinct from granular cell tumors [11]. Such alterations highlight the need to differentiate TN from other granular lesions, including apocrine carcinoma and alveolar soft part sarcoma.
Clinically, traumatic breast neuroma may present as a palpable or incidental lesion [6]. Although sometimes painless [9], chronic pain has been reported [12]. Our case was atypical in arising 4 years post-surgery rather than within the expected 1–12 months [6].
Published case reports document diverse clinical presentations. In one case report of a 74-year-old woman with breast cancer history had a BI-RADS 4 lesion later confirmed as TN on biopsy [10]. Another report described a 62-year-old woman with a position emission tomography-CT–positive lesion that histology identified as TN [10]. A third case involved a 43-year-old with prior mastectomy; a nodular lesion near the scar was confirmed as TN without recurrence [2].
Differential diagnoses include benign nipple lesions (adenoma, neurofibroma, schwannoma, leiomyoma, papilloma) and malignancies such as Paget’s disease or invasive carcinoma [13]. The most critical distinction is from local recurrence, which typically appears as irregular, non-circumscribed, vascular masses on ultrasound, whereas TNs are oval, parallel, avascular, and sometimes display the tail sign [6]. Despite imaging clues, histopathology remains essential for confirmation. Biopsy can be technically challenging in post-mastectomy patients but may be aided by hydrodissection [10].
Conclusion
Nipple TN is a rare benign entity that may mimic recurrent carcinoma after breast surgery. Awareness of this diagnosis is essential for clinicians and radiologists faced with persistent nipple pain or nodularity. Although imaging may provide suggestive features such as an oval avascular nodule with a “tail sign,” histology remains the gold standard. Surgical excision is curative and prevents unnecessary interventions. This case adds to the limited literature on nipple neuroma and emphasizes careful evaluation of atypical post-surgical breast symptoms.
Conflicts of interest
None declared.
Funding
None declared.
Ethical approval
Ethical Approval was not required for this case report in accordance with our institutional policies.
Consent
Written consent was obtained from the patient and will be provided to the Editor-in-Chief upon request.



