-
PDF
- Split View
-
Views
-
Cite
Cite
Konstantinos Tsigritis, Neofytos Basios, Anastasia Pikouli, Dionysios Dellaportas, Dimitrios Papaconstantinou, Efstratios Kofopoulos-Lymperis, Charalampos M Charalampous, Nikolaos Pararas, Sclerosing angiomatoid nodular transformation of the spleen presenting with declining hematocrit: a case report and review of the literature, Journal of Surgical Case Reports, Volume 2025, Issue 8, August 2025, rjaf434, https://doi.org/10.1093/jscr/rjaf434
Close - Share Icon Share
Abstract
Sclerosing angiomatoid nodular transformation (SANT) of the spleen is an extremely rare benign lesion originating from the splenic red pulp. The pathophysiologic mechanism has not yet been explained thoroughly. These tumors are mostly asymptomatic but cause nonspecific abdominal symptoms. Most SANTs are discovered incidentally on radiographic examination during workup for another disease or during surgery for an unrelated condition. We present a case of a 53-year-old female, whose anemia workup revealed a splenic mass. Progressive enlargement led to the decision of surgical removal. Pathology report of the spleen revealed the rare diagnosis of SANT. After removal, the patient’s anemia gradually improved and on follow-up has completely recovered. Due to the risk of malignancy, surgical removal of the spleen is the preferred management. Careful preoperative planning is important to avoid unexpected hemorrhage during the operation. Depending on the size, open surgery should be preferred over laparoscopic.
Introduction
Sclerosing angiomatoid nodular transformation (SANT) of the spleen is a very rare benign vascular lesion originating from the red pulp with unclear etiopathogenesis and variable clinical presentations. Many benign but also malignant splenic masses could mimic sclerosing angiomatoid nodular transformation, both clinically and radiologically. Most patients have no major symptoms, and most of the lesions are incidentally found on imaging for other medical conditions. Imaging modalities can substantially help in narrowing the differential diagnosis, despite the lack of a specific pathognomonic imaging sign. Due to the diagnostic dilemma, most patients are offered splenectomy due to the risk of splenic rupture and fear of a malignant lesion. Herein, we report a case of SANT in female patient presenting with symptoms of fatigue and a declining level of hematocrit. Splenectomy is the treatment of choice for these patients to resolve the intractable anemia.
Case presentation
A 53-year-old Caucasian White female reached for surgical consultation after suspicious imaging findings of the spleen. Her past medical history is clear except for symptomatic cholecystectomy 4 years prior. During preoperative ultrasound guided evaluation, a 2 cm abnormal mass is identified in the splenic parenchyma. After recovery from the cholecystectomy, persistent symptoms of dizziness and fatigue prompted evaluation with a complete blood count, which revealed: hematocrit level of 32%, and MCV of 60.7 fl. Because of the previous ultrasound finding, a computer tomography scan is ordered, and the splenic mass is measured at 5 cm of maximal diameter. The patient’s symptoms resolved but presented again 2 years after, and repeat CBC and computed tomography (CT) were conducted, resulting in a hematocrit level of 29% and the mass measured at 10 cm of maximal diameter (Fig. 1). Positron emission tomography revealed increased fluorodeoxyglucose (FDG) uptake of the spleen which raised concerns for surgical intervention. Therefore, the patient was ruled as a candidate for splenectomy. Laparoscopic removal was chosen but due to excessive hemorrhage the operation was converted to open surgery. The spleen was removed and the patient recovered after 5 days of hospitalization. Monthly postoperative blood checks showed a gradual increase and stabilization of the hematocrit at 38%, 6 months after surgery. At the 1-year follow-up with a positron emission tomography - computed tomography (PET-CT) scan, no signs of malignancy were observed. Eighteen months after surgery the patient has completely recovered and has no symptoms of recurrence.
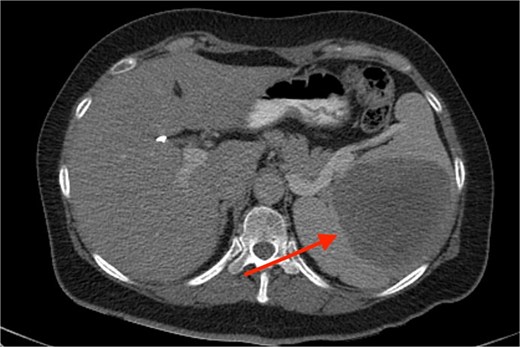
Discussion
The first literature report of SANT was by Martel et al. in 2004, which is also one of the largest case series studies available [1]. It is described as a non-neoplastic vascular lesion of the spleen and is thought to develop from a vascular insult or insufficiency, with a subsequent healing reaction involving vascular proliferation [2]. The differential diagnosis of SANT includes benign hematomas, hemangiomas, inflammatory pseudotumors as well as malignant entities like angiosarcoma, lymphoma, and metastatic tumor of the spleen. It is important to note that the diagnosis of SANT cannot be based on imaging modalities alone. Imamura et al. reviewed the features of SANT, including the efficacy of FDG uptake, and suggested that PET-CT may be able to provide an accurate diagnosis [3].
Existing literature mainly consists of scattered case reports and some case series. The largest case series by Wang et al. [4] consists of 30 pediatric patients with SANT. To the best of our knowledge, the most comprehensive systemic review is by Aziret et al. and combined data available from 230 cases of SANT described in published manuscripts across medical databases [5]. Certain epidemiologic characteristics can be inferred from this manuscript. SANT is more prevalent among women with a median age of 46 years old. Most comorbidities were anemia, gallbladder disease, and malignancies unrelated to the spleen. The most common presenting symptoms were abdominal pain, fullness, and distention.
As far as diagnostic modalities used, CT or MR scan are the most widely preferred. Many SANT lesions are described as exhibiting the “spoked wheel” pattern. This “spoked wheel” has been shown on detailed radiological and pathological findings, which is equivalent to the classic central stellate fiber interstitial fibrillar nodules isolated nodules [6].
Katsuda et al. have proposed the use of ultrasound guided fine needle aspiration biopsy. However, this remains controversial due to the complications associated with such an invasive technique. Especially in patients with bigger lesions, it can cause devastating hemorrhage outweighing the benefits of a biopsy result [7].
A case of SANT has been also associated with autoimmune disorders such as granulomatosis with polyangiitis [8].
It is difficult to exclude malignancy preoperatively via imaging. In fact, the only way to confirm SANT is immunohistochemistry. SANT has a distinctive immunohistochemical configuration characterized by CD34 (−), CD31 (+), CD8 (+) sinusoids, CD34 (+), CD31 (+), CD8 (−) capillaries, and CD34 (−), CD31 (+), CD8 (−) small veins. The surrounding macrophages are positive for CD68.
Surgery is the treatment of choice. Surgeons can choose between open versus laparoscopic approach. Most patients with SANT reported in published literature underwent open surgery, but laparoscopy has also been described as effective. Prognosis is good after both techniques and Jin et al. with their retrospective study reported no statistically significant differences regarding outcomes or complications between the two [9]. Compared with open splenectomy, laparoscopic splenectomy limits wound incision, reduces post-operative pain and complications, and provides a better quality of life after the operation.
Asplenia, however, is associated with various long-term risks, and 1 year penicillin prophylaxis is required. Moreover, vaccination against Streptococcus pneumoniae, Neisseria meningitidis, Haemophilus influenzae Type b and influenza virus are strongly recommended and should be administered at least 2 weeks before surgery in elective cases or at least 2 weeks after the surgical intervention in emergency cases [10].
Conclusion
As with every splenic lesion, it is important to investigate the mass’ origin. The rarity of splenic primary tumors and the infrequency of SANT combined with the spleen’s fragility and the malignant potency of the splenic neoplasms mandate a fast and accurate diagnosis. This case highlights a different, not yet described in the literature, clinical presentation of such a rare entity. More research and larger case series are required in order to clarify its pathogenesis and true epidemiology.
Conflict of interest statement
All authors declare no conflict of interest regarding publication of this article.
Funding
None declared.
Data availability
Previously reported case reports were used to support this study and are available and cited at relevant places within the text as references.
Consent for publication
Written informed consent for publication of this manuscript and any accompanying images were obtained from the patient.



