-
PDF
- Split View
-
Views
-
Cite
Cite
Yazan AlHabil, Qasem N Dola, Abdelatif Khader, Interrelation of cancers of unknown primary, chylous ascites, and cavernous mesenteric lymphangioma in a 57-year-old female patient: a case report, Journal of Surgical Case Reports, Volume 2024, Issue 2, February 2024, rjae129, https://doi.org/10.1093/jscr/rjae129
Close - Share Icon Share
Abstract
Cancers of unknown primary (CUPs) pose diagnostic and therapeutic challenges because of their aggressive nature and elusive identification through conventional diagnostic means. This case report presents a unique finding in a 57-year-old female patient who, alongside her CUP, developed a cavernous mesenteric lymphangioma—a rare lymphatic malformation that is more commonly observed in pediatric populations. The interrelation between CUPs, chylous ascites, and lymphangiomas is explored, shedding light on this uncommon occurrence. Our patient’s journey began with a CUP diagnosis, marked by metastatic adenocarcinoma. Subsequent symptoms led to the discovery of a mesenteric lymphangioma. The case unfolds the patient’s diagnostic challenges, surgical interventions, and postoperative course. By highlighting the distinctive features of our case, we aim to contribute to the limited understanding of the interplay between lymphatic malformations and metastatic malignancies.
Introduction
Cancers of unknown primary (CUPs) denote aggressive, histologically ascertained, metastatic malignancies with poorly differentiated features. Importantly, they lack identifiable primary locations upon traditional evaluation methods. Annually, around 2%–5% of cancer patients receive a CUP diagnosis. Data indicate a median survival interval of 2–12 months, reflecting the challenging nature of comprehending and effectively managing these cancers [1, 2].
Alterations in the lymphatic system can result in various defects, exemplified by lymphangiomas—uncommon, benign lesions typically diagnosed in pediatric patients, mainly before the age of five [3]. Lymphangiomas are categorized into capillary, cystic, and cavernous types. Capillary lymphangiomas consist of small, thin-walled lymphatic spaces on cutaneous surfaces. In contrast, cystic and cavernous lymphangiomas involve dilated lymphatic spaces in stromal tissues, with cystic lesions found in collagenous and smooth muscle tissues and cavernous lesions in lymphoid tissues. Typically located in the neck and axilla, lymphangiomas rarely manifest in the small intestine’s mesentery. An exceptionally rare consequence of mesenteric lymphangiomas is the extravasation of abdominal or thoracic lymph fluid into the abdominal cavity, termed chylous ascites [4].
The interconnection between chylous ascites and lymphangiomas within the context of CUPs remains unexplored in the existing literature. Herein, we present this uncommon occurrence, as observed in a 57-year-old female patient.
Case report
A 57-year-old female presented to our emergency department with diffuse abdominal pain, distention, constipation, nausea, and back pain of one-month duration, accompanied by a 19.8 lbs (9 kg) weight loss. Three months earlier, the patient sought care at another hospital for recurrent abdominal pain. Computed tomography (CT) scans revealed suspiciously enlarged lymph nodes in the peripancreatic and para-aortic regions, notably a 4.1 × 2.4 cm necrotic and heterogeneous node in the para-aortic area (Fig. 1). Subsequent ultrasound-guided fine needle aspiration and fine needle biopsy confirmed a metastatic poorly differentiated adenocarcinoma and an acellular smear, respectively. Upper and lower endoscopic studies showed unremarkable findings. The diagnosis of CUP origin was made.
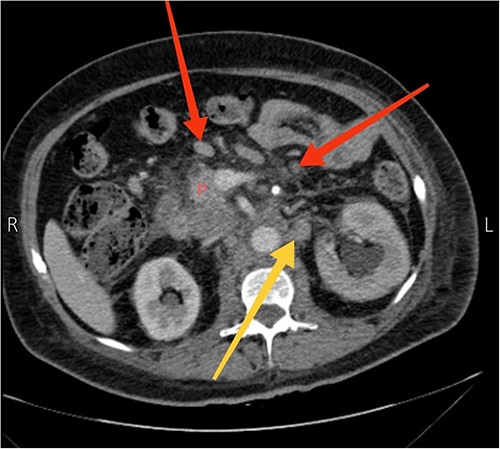
Axial view CT scan showing the head of the pancreas (P), enlarged peripancreatic lymph nodes (the two arrows at the top), and a 4.1 × 2.4 cm necrotic and heterogeneous enlarged lymph node in the para-aortic area (the arrow at the bottom).
Upon examination, she had normal vital signs. Abdominal examination revealed a mildly distended and generally soft abdomen with tenderness in the upper quadrants. Bowel sounds were reduced. Lab tests showed a significantly elevated C-reactive protein level of 265 mg/dL (normal range: <0.3 mg/dL). Axial CT scan revealed mesenteric edema, jejunal wall thickening, surrounding fat stranding, and an enlarged mesenteric lymph node (Fig. 2). An emergent diagnostic laparoscopy revealed a mildly dilated viable jejunal loop, ~16 cm in length, located 10-cm distal to the ligament of Treitz. Additionally, a milky jejunal mesentery and a moderate amount of chalky ascitic fluid in perihepatic, perisplenic, and pelvic regions were observed (Fig. 3). Fluid analysis confirmed chylous ascites with a triglyceride level of 320 mg/dL (normal range: <110 mg/dL). Histopathological analysis of an excisional biopsy revealed abnormally dilated lymph vessels, leading to a diagnosis of cavernous mesenteric lymphangioma with chylous ascites. Surgical excision was not pursued because of the patient’s aggressive metastatic CUP state. She had an uneventful postoperative course, discharged on the fourth day, and was referred for follow-up with the oncology team for palliative chemotherapy.
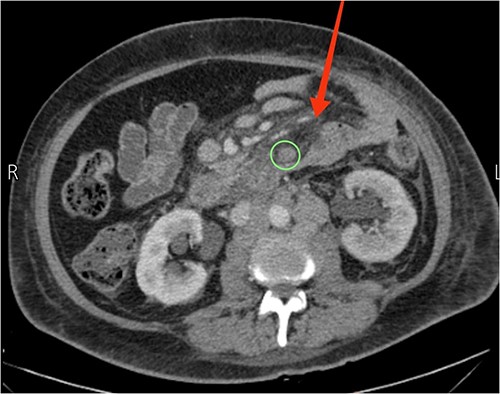
Axial view CT showing prominent mesenteric edema with jejunal wall thickening and surrounding fat stranding (arrow). An enlarged mesenteric lymph node can also be seen (circle).
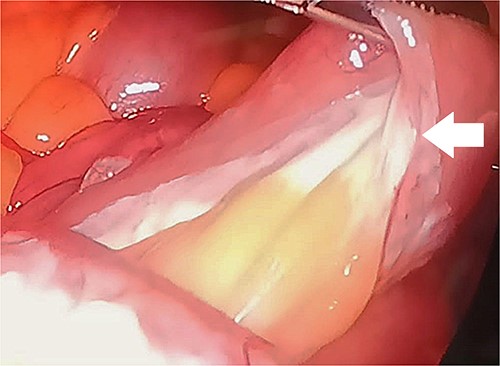
Laparoscopic findings demonstrate a milky or whitish jejunal mesentery (arrow).
Discussion
Lymphangioma is a rare benign condition, typically found in the pediatric population, often in the axillary, neck, and head regions. It seldom occurs in the mediastinal or abdominal cavities, with limited documented cases in the mesentery of the small intestines [5, 6]. The cause of lymphangiomas is uncertain, with theories suggesting vascular malformations impede communication between lymph sacs and venous drainage terminals [7]. Other potential causes include secondary development from abdominal trauma, surgery, inflammation, or lymphatic obstructive conditions [3].
Lymphangiomas present with diverse symptoms, commonly nonspecific, including abdominal pain, vomiting, and distention. Pathological analysis is crucial for a definitive diagnosis, as imaging studies may pose challenges in distinguishing cystic intra-abdominal lesions. Such lesions can mimic conditions like lymphoma, tuberculoid mass, hydatid cyst, secondary metastatic mass, small bowel adenocarcinoma, or mesenteric tumors such as schwannomas, desmoid, smooth muscle tumors, or sarcomas [5, 8]. Despite diverse differentials and the requirement for pathological examination, lymphangiomas often require radical intraoperative resection because of potential involvement of adjacent structures, risk of sarcoma transformation, or a 10%–15% chance of recurrence with incomplete resections. Post-complete surgical excision, the prognosis for lymphangiomas is generally favorable [9, 10].
Chylous ascites or mesentery, stemming from cavernous mesenteric lymphangioma, is a rare occurrence, involving the leakage of thoracic or intestinal lymph into the abdominal cavity. It may result from congenital factors like lymphangiectasia causing vessel dilation, traumatic events leading to lymphoperitoneal fistula formation, or obstructive causes associated with increased intestinal lymphatic system pressure, particularly in the context of lymphatic malignancies [4].
To our knowledge, only two documented cases in the literature discuss chylous ascites and chylous mesentery related to cavernous mesenteric lymphangioma. Goel et al. [11] reported on an 8-year-old male with intestinal lymphangiectasia, who presented with symptoms of chylous ascites, pleural effusion, diarrhea, pitting edema, and malabsorption. Additionally, Chamberlain et al. [4] are the first to document chylous ascites and mesentery in an adult female with symptoms of intestinal obstruction and suspected internal hernia, with no history of malignancy. Contrastingly, our case has a significantly different history and presentation. Therefore, we appear to be the first to document the development of chylous mesentery and ascites secondary to cavernous mesenteric lymphangioma in the context of CUP.
All in all, lymphangiomas are benign vascular malformations. They usually arise in the axilla, neck, and head, making their occurrence in the abdominal small intestine’s mesentery a surgical rarity. A rare consequence is chylous mesentery. CUPs present challenges for both patients and healthcare professionals. This case report highlights the potential development of chylous mesentery within the context of CUPs, suggesting the exploration of therapeutic surgical interventions in similar cases.
Conflict of interest statement
None declared.
Funding
None declared.



