-
PDF
- Split View
-
Views
-
Cite
Cite
Hussain Al Jabran, Hameed Aljawad, Jawad S Alnajjar, Jawaher AlRaihan, Sarah Al Omar, Appendicular diverticulosis complicated by acute appendicitis and organizing abscess: what does the surgeon need to consider intraoperatively?, Journal of Surgical Case Reports, Volume 2024, Issue 10, October 2024, rjae618, https://doi.org/10.1093/jscr/rjae618
Close - Share Icon Share
Abstract
Acute appendicitis is a common surgical emergency, affecting 7%–10% of people worldwide, whereas appendicular diverticulosis is rare, occurring in 0.004%–2.1% of appendectomy cases and often mimicking appendicitis symptoms. A 35-year-old male presented with right lower quadrant pain, nausea, vomiting, and diarrhea. Clinical examination showed tenderness in the right iliac fossa. Imaging suggested uncomplicated acute appendicitis, but surgery revealed an appendiceal mass suspected to be a carcinoid tumor. Histopathology post-appendectomy diagnosed appendicular diverticulosis complicated by acute appendicitis. This case emphasizes the need for thorough histopathological examination in appendectomy cases to accurately diagnose and differentiate appendicular conditions. Appendiceal diverticulitis should be considered in the differential diagnosis of right lower quadrant pain to ensure proper surgical intervention and prevent complications.
Introduction
Acute appendicitis is a common surgical emergency with a 7%–10% prevalence [1]. Appendicular diverticulosis, a rare condition (0.004%–2.1% of appendectomy cases), mimics acute appendicitis symptoms, such as right lower quadrant pain, nausea, vomiting, and fever, but has a higher perforation risk [2, 3]. A definitive diagnosis is made through histological analysis post-surgery [4].
Case presentation
A 35-year-old male presented to the Emergency Department with right lower quadrant abdominal pain for 2 days, initially central then shifting to the right iliac fossa, accompanied by nausea, vomiting, and diarrhea. He reported no urinary symptoms, fever, chills, weight loss, or significant family history of cancer. His medical history included a right shoulder dislocation.
On examination, the patient was alert, oriented, and vitally stable. Abdominal examination revealed mild tenderness and rebound tenderness in the right iliac fossa. Laboratory investigations showed normal leukocyte counts and mildly elevated C-reactive proteins (38). An abdominal ultrasound suggested acute appendicitis or terminal ileitis (Fig. 1), prompting a CT scan despite the patient’s allergy to contrast.
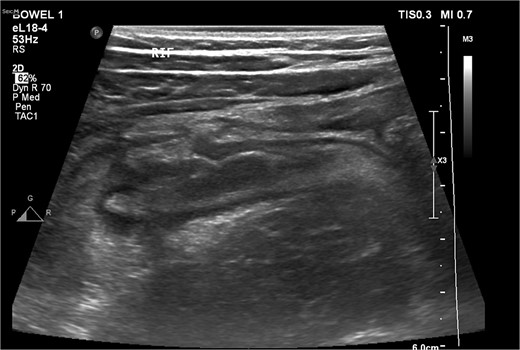
An ultrasound picture showing tubular-like structure surrounded by edematous fluid.
The non-contrast CT scan revealed a retrocecal appendix measuring 11 mm in diameter, with periappendiceal fluid and fat smudging, and reactive thickening of the cecum, indicating uncomplicated acute appendicitis. The patient was admitted to the surgical department and scheduled for a laparoscopic appendectomy (Figs 2 and 3).
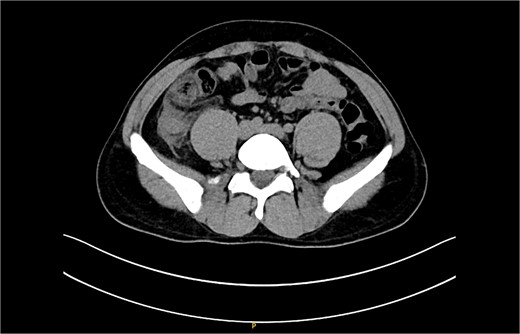
CT scan picture with an axial view showing acute inflamed appendix with peri-appendicular fat smudging, confirming the radiological finding of acute appendicitis.
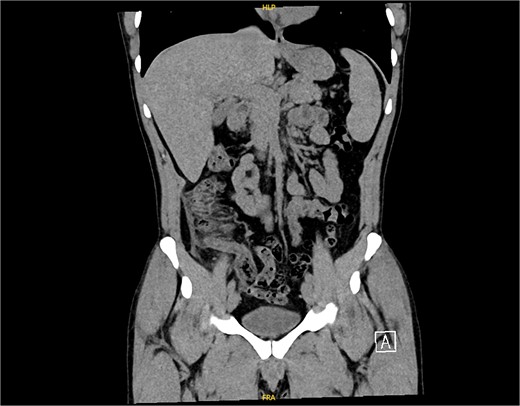
CT scan picture with a coronal view showing acute inflamed appendix with peri-appendicular fat smudging, confirming the radiological finding of acute appendicitis.
The patient was admitted and scheduled for a laparoscopic appendectomy. During surgery, the appendix was identified in the retrocecal position, extending to the right paracolic gutter. It was dissected from surrounding tissues, revealing a large mass at the tip and multiple nodules on its surface. The surgical team employed minimal manipulation techniques to avoid tumor rupture, suspecting a carcinoid or other appendicular tumor (Fig. 4). The mesoappendix was dissected and transected at the base using an EndoGI stapler. The specimen was removed in a bag and sent for histopathology (Fig. 5).
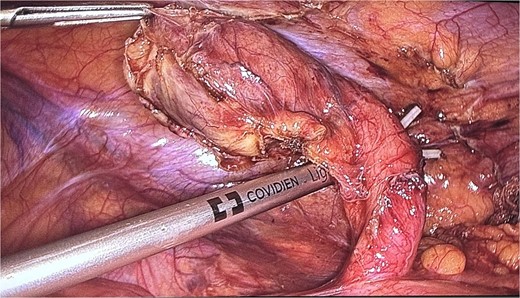
An intraoperative picture of an acutely inflamed appendix with mass seen at the tip; the mass was manipulated carefully and grasped at peri-appendicular tissue to avoid mass rupture.
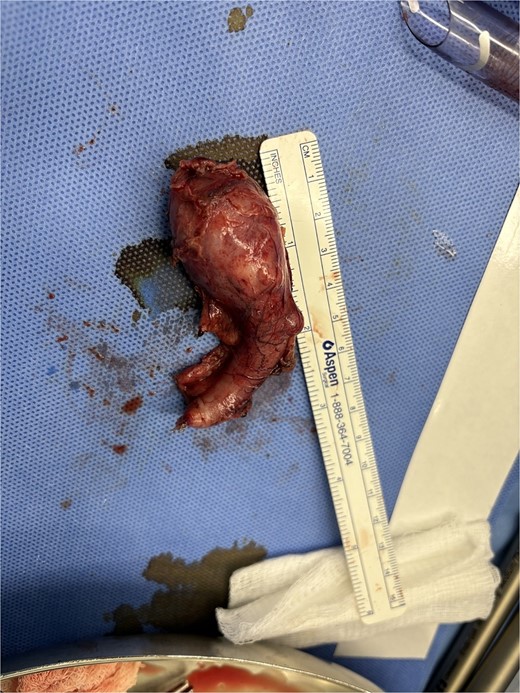
A gross picture of the appendix with mass noticed at the tip and multiple nodules over the appendicular surface.

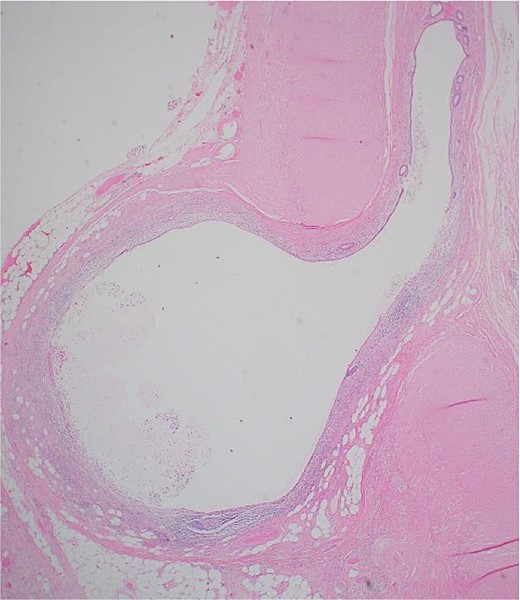
An image showing a whole-slide longitudinal section of the distal appendix demonstrating multiple outpouchings of mucosa through weak points of the muscular wall.
Postoperatively, the patient had an uneventful recovery and was discharged the next day with simple analgesia. Histopathology revealed an 8 × 1.2 cm appendix with a 3.5 × 2.5 cm distal bulge, filled with pus and multiple diverticula. Examination showed acquired appendicular diverticulosis with mucosal and submucosal outpouchings through the muscularis propria. The mucosa and diverticula were infiltrated by neutrophils extending to the submucosa and muscular wall, with inflammation reaching the mesenteric fibroadipose tissue. Reparative changes included edema, macrophages, and fibroblastic proliferation. The final diagnosis was appendicular diverticulosis complicated by acute appendicitis with an organizing abscess (Figs 6 and 7).
Discussion
Appendiceal diverticulitis (AD), first described in 1893 by Kelynack, is a rare cause of right iliac fossa pain and acute abdomen, often mimicking acute appendicitis [5, 6]. A retrospective study found that diverticular disease accounts for 2% of all appendectomies [7]. Risk factors for acquired AD include male gender, age over 30, Hirschsprung’s disease, and cystic fibrosis [8]. AD can resemble conditions like acute appendicitis, Crohn’s disease, and other pathologies [5]. It is also linked to pseudomyxoma peritonei [9] and appendiceal neoplasms, such as carcinoid tumors, mucinous adenomas, tubular adenomas, and primary appendiceal adenocarcinomas [4]. Common complications include diverticulitis and perforation, potentially leading to a localized abscess or generalized peritonitis [4].
Differentiating between AD and appendiceal neoplasia based on clinical or radiological assessments alone is challenging. Therefore, an appendectomy followed by thorough histopathological examination is recommended to avoid missing serious conditions. Histopathological analysis is crucial, as clinical and radiological distinctions between AD and acute appendicitis are often unclear [6]. Appendectomy is the preferred treatment for acute AD, and elective prophylactic appendectomy is advised for patients with a diverticulum to prevent progression to diverticulitis, perforation, or malignancy.
Due to diagnostic uncertainty at initial presentation, surgeons must use careful and minimal manipulation techniques to avoid tumor rupture. In this case, the appendicular mass mimicked a carcinoid tumor intraoperatively, so minimal manipulation techniques were employed by grasping the appendix with periappendicular tissue. The mesoappendix was dissected at its root to obtain as many lymph nodes as possible to assist the pathologist in making a final diagnosis, especially in cases of malignancy. Clinicians should always consider various differential diagnoses of acute appendicitis, including AD, when evaluating patients with right lower quadrant abdominal pain [3].
Conclusion
Acute appendicitis is common, while rare appendicular diverticulosis mimics its symptoms, complicating diagnosis. This case highlights the importance of thorough histopathological examination post-appendectomy. Prompt surgical intervention and considering AD in differential diagnoses of right lower quadrant pain are crucial. Prophylactic appendectomy is recommended for known diverticulosis cases to prevent complications.
Conflict of interest statement
None declared.
Funding
None declared.



