-
PDF
- Split View
-
Views
-
Cite
Cite
Akira Kawai, Shota Morimoto, Futoshi Morio, Toshiya Tachibana, Tomoya Iseki, Chronic Achilles tendon rupture in elderly treated with a combination of the side-locking loop suture technique and early rehabilitation protocol: two cases report, Journal of Surgical Case Reports, Volume 2023, Issue 6, June 2023, rjad339, https://doi.org/10.1093/jscr/rjad339
Close - Share Icon Share
Abstract
A chronic Achilles tendon rupture (ATR) is generally defined as a rupture that occurs more than 4–6 weeks after the initial injury. A variety of corrective techniques have been reported, such as direct repair, V-Y plasty, turndown flap, tendon transfer and free tendon grafting. These procedures generally produce good results, but have the disadvantage of requiring prolonged immobilization and weight-bearing restrictions. This may be a risk factor for falls and decreased function in the lower limbs, especially in older patients. Side-locking loop sutures (SLLS) were first introduced in 2010 as a direct repair technique for acute ATR. This technique provides higher tensile strength, which may allow for early rehabilitation protocols such as early range of motion and early weight-bearing of the ankle without postoperative immobilization. In this report, we describe two cases of chronic ATR in elderly patients treated with SLLS and an early rehabilitation protocol.
INTRODUCTION
A chronic Achilles tendon rupture (ATR) is generally defined as an ATR that occurs more than 4–6 weeks after the initial injury [1]. In general, the results of conservative treatment of chronic ATR are relatively poor, and surgical treatment is predominantly recommended [2]. A variety of surgical techniques have been reported, including direct repair, V-Y plasty, turndown flap, tendon transfer and free tendon grafting. Although these procedures generally provide good results, they have the disadvantage of requiring prolonged immobilization and limited weight-bearing [3]. This may be a risk factor for falls and reduced lower limb function, particularly in elderly patients [4].
The side-locking loop suture (SLLS) technique is a direct repair procedure for ATR that was first introduced by Yotsumoto et al. [5]. Compared with other direct repair techniques, the SLLS technique provides greater tensile strength and stiffness, allowing rehabilitation protocols such as range of motion exercises and weight-bearing to begin earlier without the need for postoperative immobilization [5, 6]. Recently, several studies have reported satisfactory surgical outcomes using the SLLS technique for acute ATR [5–7].
In this report, we describe two cases of chronic ATR in elderly patients treated with a combination of the SLLS technique and early rehabilitation protocol. Written informed consent was obtained from both patients before publishing this report.
CASE REPORT
Case 1
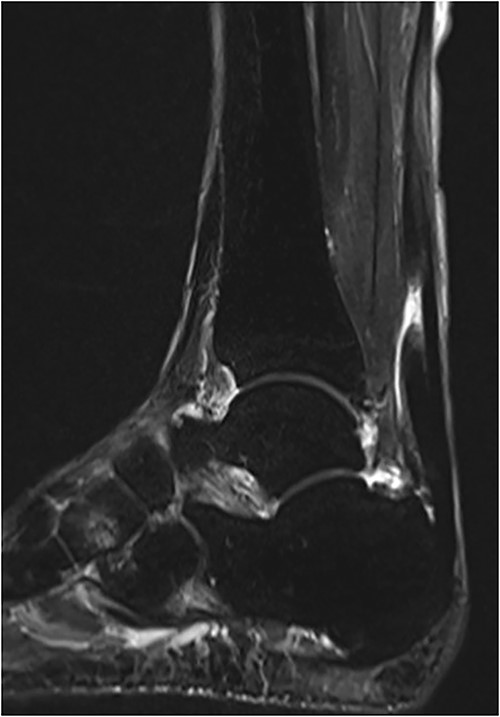
An 81-year-old male presented to a local clinic complaining of pain in his right heel without any precipitating trauma. He was diagnosed with Achilles tendinitis and treated with conservative treatment. After 2 months of conservative treatment, the patient visited our hospital because there had been no improvement in his heel pain. Physical examination revealed swelling and a palpable gap along the course of the Achilles tendon. A Thompson test was performed and proved negative, but showed reduced plantar flexion compared with the unaffected side. Plain radiographs showed no abnormal findings, whereas magnetic resonance imaging (MRI) revealed a rupture of the Achilles tendon with a gap between the tendon ends (Fig. 1). Based on physical examination and imaging findings, a diagnosis of chronic ATR was made and surgical treatment was given.
The operation was performed under general anesthesia in the prone position with an air tourniquet. First, a 6 cm longitudinal incision was made along the mid-medial aspect of the Achilles tendon to identify the rupture site. Scar tissue and degenerated tendon were found at the rupture site and were adequately debrided. With the operated ankle in neutral position, the Achilles tendon gap was 2 cm. Using the modified SLLS technique introduced by Imade et al. [6], the ruptured tendon was directly sutured with USP 5 braided polyethylene and polyester suture thread (FiberWire; Arthrex Co., Naples, FL, USA). A 4-0 monofilament nylon thread was then used to create a peripheral cross-stitch suture (Fig. 2). Finally, the wound was stitched closed and the operation was completed.
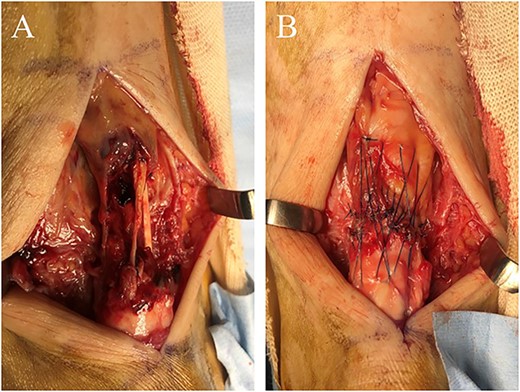
(A) In the rupture site, scar tissues and degenerative tendon were seen. (B) After these tissues were adequately debrided, the ruptured tendon was directly repaired using the modified SLLS technique.
Postoperatively, the ankle was not immobilized and active and passive range-of-motion exercises were started immediately. Partial weight-bearing was allowed 1 week postoperatively and full weight-bearing 4 weeks postoperatively. Double heel-raise exercises were started 6 weeks after surgery and single heel-raise exercises at 8 weeks. Two years after the surgery, the patient had no symptoms or dysfunctions and displayed an American Orthopaedic Foot and Ankle Scale (AOFAS) score of 100 points.
Case 2
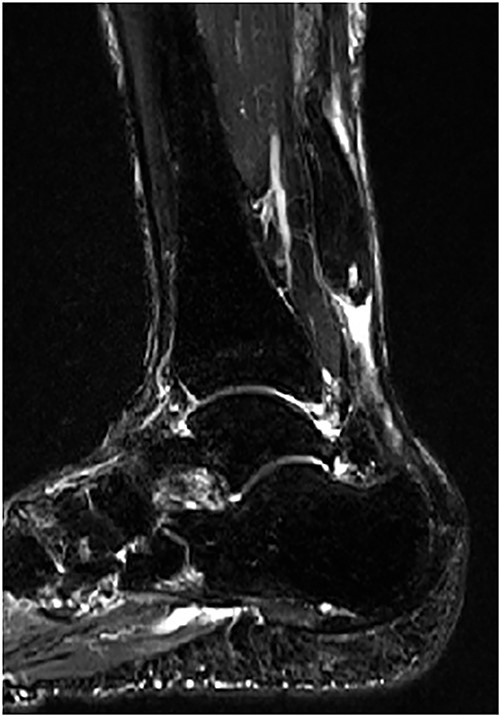
A 75-year-old male presented to a local clinic complaining of right heel pain after spraining his right ankle. He was diagnosed with an ankle sprain and treated conservatively for 2 months. However, the heel pain did not improve and so he visited our hospital. Physical examination revealed a palpable gap along the course of the Achilles tendon and a positive Thompson test. Plain radiographs showed no abnormalities, but MRI revealed a rupture of the Achilles tendon with a gap between the tendon ends (Fig. 3). Based on physical examination and imaging findings, we diagnosed the patient with chronic ATR and administered surgical treatment.
The operation (Fig. 4) and postoperative treatment performed were the same as Case 1.
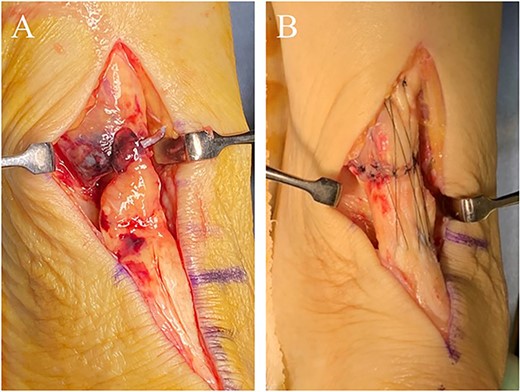
(A) In the rupture site, scar tissues and degenerative tendon were confirmed. (B) The operation was performed as same as Case 1.
One year after the operation, the patient showed no symptoms or dysfunctions and had also achieved an AOFAS score of 100 points.
DISCUSSION
Various surgical procedures have been reported for the treatment of chronic ATR, including direct repair, V-Y plasty, turndown flap, tendon transfer and free tendon grafting [3]. Although there is no clear consensus on the optimal choice of surgical procedure for chronic ATR, it has been reported that the size of the Achilles tendon defect is an important factor [8]. Direct repair is generally used in cases of chronic ATR with <2.5 cm of tendon defect [9]. For cases with a tendon defect of more than 2.5 cm, reconstructive surgery including V-Y plasty, turndown flap, tendon transfer and free tendon grafting is suggested [9]. Although both direct repair and reconstructive procedures generally yield good results, both procedures have the disadvantage of requiring prolonged immobilization and limited weight-bearing [3].
In 2010, the SLLS technique was first introduced as a direct repair procedure for acute ATR [5]. Compared with other direct repair procedures, the SLLS technique provides greater tensile strength and stiffness, which eliminates the need for postoperative immobilization and safely allows for an early rehabilitation protocol, including early ankle range of motion and early weight-bearing [5, 6]. Several studies have reported that direct repair using the SLLS technique provides satisfactory results for acute ATR [5–7].
As the patients in the present cases were elderly, it was considered that postoperative prolonged immobilization and restricted weight bearing may be a risk factor for falls and reduced lower limb function. Also, the size of the Achilles tendon defect was <2.5 cm, so we treated both cases with direct repair using the SLLS technique, which allowed for early rehabilitation protocol without postoperative immobilization.
In this report, we described two cases of chronic ATR in elderly patients treated with a combination of the SLLS technique and an early rehabilitation protocol. This type of treatment may be a useful option for chronic ATR in the elderly.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
No funding.
DATA AVAILABILITY
Not applicable.



