-
PDF
- Split View
-
Views
-
Cite
Cite
Giovanni Parente, Marco Di Mitri, Eduje Thomas, Sara Maria Cravano, Simone D’Antonio, Tommaso Gargano, Michele Libri, Mario Lima, A case of massive subcutaneous emphysema and transient ischemic attack due to argon plasma coagulation following endoscopic pilonidal sinus treatment, Journal of Surgical Case Reports, Volume 2023, Issue 6, June 2023, rjad324, https://doi.org/10.1093/jscr/rjad324
Close - Share Icon Share
Abstract
Pilonidal sinus is a small hole affecting the skin and subcutaneous tissue, which usually contains hair and skin debris, resulting in the creation of the so-called pilonidal cyst. The endoscopic pilonidal sinus treatment (EPSiT) is a minimally invasive procedure consisting of the removal of hairs and cauterization of the cavity under direct endoscopic vision. In our institution, we used to end this procedure with argon plasma coagulation (APC). Here, we discuss a case of 22-year-old man affected by pilonidal disease, who developed a massive subcutaneous emphysema and suspected transient ischemic attack secondary to gas reabsorption after an EPSiT in which APC was used for the coagulation.
INTRODUCTION
A pilonidal sinus is a small hole or tunnel affecting the skin and subcutaneous tissue of the natal cleft, which is caused by the insertion of free hair into the subcutaneous tissue, resulting in the creation of the so-called pilonidal cyst [1, 2].
The endoscopic pilonidal sinus treatment (EPSiT) is a minimally invasive procedure consisting of the removal of hairs and cauterization of the cavity from inside the cyst under direct endoscopic vision. In our institution, we used to end this procedure with argon plasma coagulation (APC) for a more reliable hemostasis and thermoablation of the inflammatory tissue [3].
APC is a noncontact form of electrocautery which uses ionized argon gas (plasma) to conduct electrical current, resulting in the coagulation of the bleeding lesions; the depth of the coagulation is usually only a few millimeters [4–6].
Here, we discuss a case of massive subcutaneous emphysema and suspected transient ischemic attack (TIA) secondary to gas reabsorption after an EPSiT in which APC was used at the end of the procedure.
CASE REPORT
A 22-year-old man affected by pilonidal disease was admitted to our department and underwent an EPSiT procedure in spinal anesthesia. The post-operative course was uneventful and the patient was discharged on the same day.
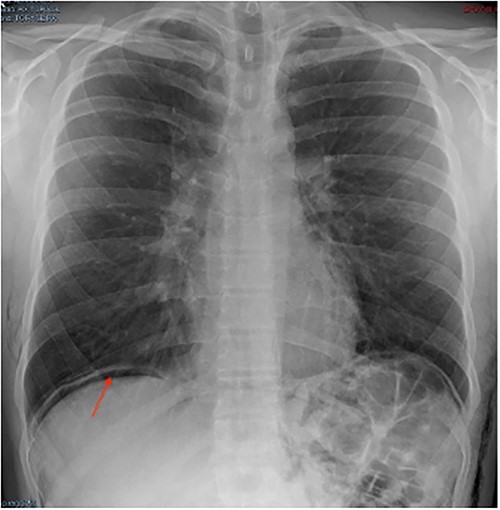
In the post-operative day (POD) I, the patient was referred to our emergency department due to thoracic pain. The patient’s general conditions were good except for a subcutaneous emphysema extended to thorax, abdomen, back and scrotum. A chest X-ray showed a suspected image of free intraperitoneal gas (Fig. 1); we, therefore, decided to perform further radiological study.
An abdominal and thorax computed tomography (CT) scan showed subcutaneous emphysema in the thorax, neck, abdomen, back, scrotum and intergluteal fold along with a pneumomediastinum (Fig. 2A and B).
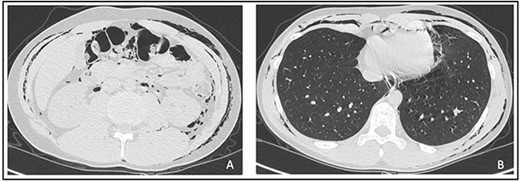
Signs neither of pulmonary embolism or pneumothorax nor free intraperitoneal gas were detected. Considering stable vital parameters, we opted for clinical observation in our department. The patient was discharged 3 days after with an almost completed reabsorption of the emphysema.
In POD V, the patient was referred during nighttime to the emergency department for a sudden episode of absence-like symptoms (amnesia, headache and confusion) that lasted for ~5 minutes. A brain CT scan was performed, and the result was negative. We admitted the patient to our department for clinical observation, but no other neurological symptoms were recorded. The next day, a brain magnetic resonance imaging was performed, and no injury or pathological findings were detected.
Considering symptoms strongly suggestive of TIA due to reabsorbing of argon gas, but in the absence of a pulmonary embolism, we hypothesized a right-to-left (RTL) shunting secondary to a possible patent foramen ovale (PFO). We than performed a transesophageal echocardiogram along with a PFRO test (also called as ‘agitated saline’), which confirmed our hypothesis.
We concluded that the patient experienced a TIA secondary to argon bubbles arrived at the central nervous circulatory system via RTL shunting during reabsorption of the massive emphysema.
DISCUSSION
The etiology of cerebral gas embolism is multifactorial. Air can enter the arterial vessels secondary to an important trauma or during medical procedures [7, 8]. Rarely venous emboli can enter the arterial system through intracardiac shunt (PFO, atrial septal defect) or intrapulmonary shunt (vascular malformations) [9]. Air embolism can also occur during endoscopic procedures due to an excessive air insufflation, resulting in barotrauma to arteries and veins [10]. Air can also enter the cerebral circulation through a retrograde mechanism reaching the cerebral circulation by moving in the opposite direction of the venous blood flow [11, 12].
APC is an innovative electrosurgical coagulation device which uses a jet of argon gas with an ionized arc, resulting in a fine plasma spray electrical current.
APC finds major applications for hemostasis, tissue devitalization and reduction. Few cases of massive gas embolism due to APC during surgery have been referred in literature [13, 14].
Although argon is an inert gas, it is 17 times less soluble than carbon dioxide, and for this reason, argon emboli are not promptly dissolved and may pass into the systemic circulation [15, 16].
Clinically, gas embolism can manifest as right ventricular outflow obstruction, myocardial infarction or stroke, which can occur either by the introduction of gas directly into the pulmonary venous system and subsequently the left atrium or by the passage of gas in the left heart through a RTL intracardiac defect (PFO or atrial septum). Folch et al. described the mechanism behind gas embolism during APC in an explanted porcine model. They hypothesized that when the APC catheter enters in direct contact with the mucosa, there is gross evidence of submucosal gas transfer occurring at all gas flow settings; indeed, they concluded that decreasing the flow rate does not affect gas penetration [13]. Air cerebral embolism can result in stroke or TIAs. TIA usually lasts for few minutes: most signs and symptoms disappear within an hour, though, rarely, may last up to 24 hours. Neurological manifestations include weakness, numbness or paralysis of the face or limbs (typically on one side of the body), confused speech or difficulties in understanding others, blindness in one or both eyes or double vision, dizziness or loss of balance and coordination, loss of consciousness, amnesia and headache [17].
As previously discussed, our patients complained in POD V of a sudden onset of amnesia, headache and confusion that lasted for ~5 minutes. Considering the post-operative complication recorded, we concluded for a case of TIA secondary to cerebral argon embolism. It is, at our knowledge, the first case described in literature of TIA due to APC use during an endoscopic procedure. In our case, probably, the APC catheter was too close or even in direct contact with the subcutaneous tissue causing a subcutaneous damage, emphysema and consequently gas reabsorption in the systemic circulation (Fig. 3). Fortunately, the patient had no long-term consequences and was referred to cardiac surgeons for PFO treatment.
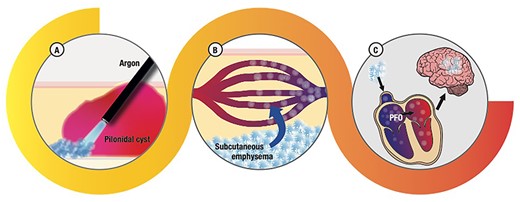
Hypotized mechanism that explains neurological symptoms of our patients: (A) the argon applicator too close to the tissue treated determined a massive passage of gas into the subcutaneous tissue; (B) argon bubbles entering the blood stream, some of them not dissolved (emboli); (C) argon emboli reaching the heart and, through PFO, the brain, resulting in the neurological symptoms described.
In conclusion, severe post-operative complications secondary to APC are extremely rare but are potentially life threating.
Our suggestions are to use APC with the lower flow settings possible and not to stay too close or in contact with tissues.
CONFLICT OF INTEREST STATEMENT
The authors declare that they have no competing interests.
FUNDING
No funding or grant support was received.
DATA AVAILABILITY
Please contact the author for data requests.
AUTHORS’ CONTRIBUTIONS
Study conception and design: G.P., M.D.M. and M.L.; data acquisition: G.P., E.T., S.M.C. and M.D.M.; analysis and data interpretation: G.P., M.D.M. and T.G.; drafting of the manuscript: G.P., E.T., M.D.M., S.M.C., S.D’A. and M.L.; critical revision: G.P., E.T., M.D.M. and M.L. All authors have read and agreed to the published version of the manuscript.
PATIENT CONSENT
Patient’s consent for data analysis and publication was obtained.
AUTHORSHIP
All authors attest that they meet the current ICMJE criteria for authorship.



