-
PDF
- Split View
-
Views
-
Cite
Cite
Georgina E Sellyn, Neil Kapil, Baldeep Pabla, Mujeeb Ur Rahman, Aimal Khan, Polyarteritis nodosa: a case report of isolated large bowel involvement and surgical intervention, Journal of Surgical Case Reports, Volume 2023, Issue 4, April 2023, rjad195, https://doi.org/10.1093/jscr/rjad195
Close - Share Icon Share
Abstract
Polyarteritis nodosa (PAN) is a necrotizing vasculitis commonly affecting small-sized vessels and medium-sized vessels. We present the case of surgical resection for ischemic colitis secondary to PAN. A 26-year-old woman presented with left lower quadrant pain, diarrhea and bloody stools. Colonoscopy showed diffuse circumferential ulceration and necrotic lining from the sigmoid colon to the splenic flexure. A subsequent computed tomography angiography (CTA) revealed left colonic wall thickening, hypoenhancement and multiple inferior mesenteric artery aneurysms, concerning for vasculitis. Ensuing laboratory workup all returned negative. Worsening pain, left-sided peritonitis, tachycardia and rising white blood cell necessitated a colectomy from the proximal descending to upper rectum with an end colostomy. Surgical pathology showed features consistent with PAN. The patient improved significantly after surgery and was discharged on a steroid taper and later started on mycophenolate mofetil. This case is a unique presentation of isolated large intestinal involvement and was treated with both medical and surgical interventions.
INTRODUCTION
Polyarteritis nodosa (PAN) is a necrotizing vasculitis that commonly affects small-sized vessels and medium-sized vessels. It can involve isolated organs or present as a multisystem disease of varying clinical severity and presenting symptoms. Most commonly involved systems include the peripheral nervous system and skin [1], with frequent presenting symptoms of livedo reticularis, subcutaneous nodules, ulcers, mononeuritis and polyneuritis [2, 3]. In addition, regular renal involvement can trigger hematuria, proteinuria and secondary hypertension [1, 4, 5]. Within the gastrointestinal tract, the small bowel and gallbladder are typically affected, with isolated colonic involvement being rare [6]. Diagnosis is usually established with the help of clinical features, angiography and histopathology [7]. The treatment for PAN includes glucocorticoids alone for mild forms of PAN, with cyclophosphamide, azathioprine or other disease modifying antirheumatic drugs reserved for nonresponding or relapsing cases [8–10]. Untreated PAN has a poor prognosis, with a mortality rate of 10–20% within 5 years; with treatment significantly improving its outcomes [11].
There is no clear role for surgery in treating most patients with PAN. However, in certain severe cases, especially with evidence of tissue necrosis, surgical intervention may be necessary for management. In this report, we describe a young patient who presented with significant gastrointestinal symptoms and was found to have colonic ischemia secondary to PAN.
CASE REPORT
A 26-year-old female with a medical history of polycystic ovarian syndrome presented with a 6-week history of significant left lower quadrant abdominal pain, diarrhea and mucoid bloody stools. Since the onset of these symptoms, the pain had progressively increased and was sharp in nature.
A computed tomography (CT) scan showed thickening of her left colon, extending from the splenic flexure to the mid-sigmoid colon. She was tentatively diagnosed with ulcerative colitis, started on prednisone. Blood work was significant for CRP of 27.7 and a white blood cell count (WBC) of 16 000.
Colonoscopy showed an unremarkable rectal mucosa; however, starting in the sigmoid colon, there was diffuse circumferential ulceration and evidence of a necrotic mucosal lining (Fig. 1). The area was ulcerated and firm, extending from the sigmoid colon, through the descending colon, to the splenic flexure. Once at the splenic flexure, the remainder of the colon and terminal ileum were unremarkable for significant inflammation. These findings raised concern for ischemic-type injury rather than inflammatory bowel disease. A subsequent CTA was primarily notable for left colonic thickening, hypoenhancement, and multiple aneurysms and irregularities of the inferior mesenteric artery in a distribution concerning for vasculitis (Fig. 2). Rheumatological recommendations included a laboratory workup with: antinuclear antibody, antineutrophilic-cytoplasmic antibody, cytomegalovirus, histoplasma, treponemal, hepatitis panel, which all returned negative.
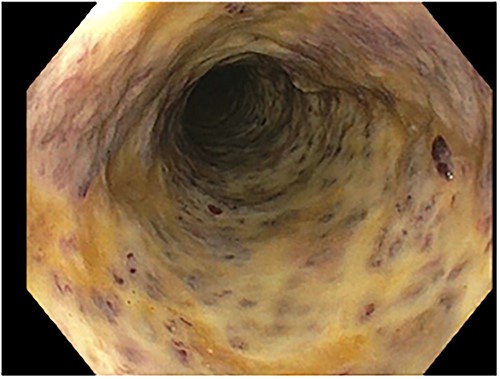
Colonoscopy: diffuse circumferential ulceration and a necrotic lining.
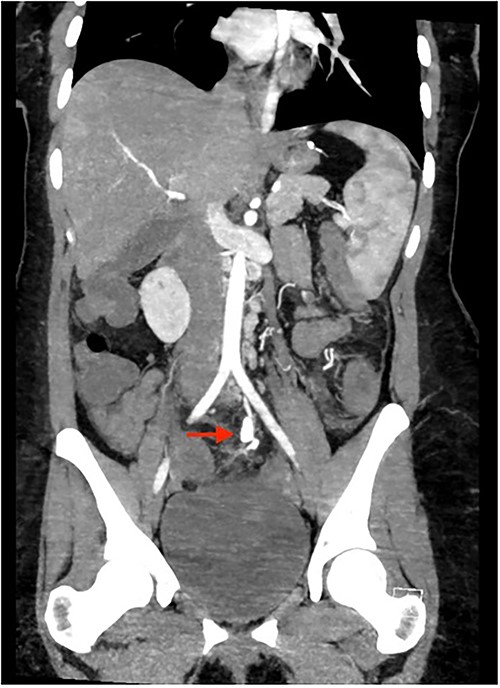
Due to the patient’s increasing abdominal pain, with focal left-sided peritonitis, tachycardia and elevated white count, she was taken to the operating room for abdominal exploration. Intraoperatively, she was noted to have ‘woody’ inflamed sigmoid and descending colon. Segmental resection of the proximal descending colon to the upper rectum with an end colostomy was performed. The surgical pathology showed focal, acute inflammation, ulceration and fibropurulent exudates as well as active and healed necrotizing arteritis with ischemic ulcer (Fig. 3). Small- and medium-sized vessel walls were noted to be thickened with necrosis in some areas and disruption of the internal elastic lamina. A few arteries showed mixed inflammatory infiltrates in the media. Overall, this pathology of necrotizing arteritis was consistent with features of PAN.
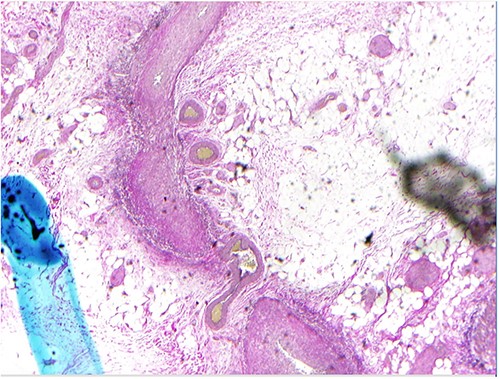
The patient’s postoperative course was uncomplicated with significant clinical improvement noted within 1 day. A CTA chest did not show abnormalities and the patient met all postoperative goals to be discharged on postoperative Day 4. In the outpatient setting, the patient was initially maintained on 40 mg prednisone therapy with plan for cyclophosphamide as additional therapy. Given her concerns for potential reduction in fertility related to cyclophosphamide, the patient was started on mycophenolate mofetil as chronic immunosuppressive treatment. She was eventually tapered off prednisone.
DISCUSSION
PAN is a type of necrotizing vasculitis, which most commonly presents as multisystem disease. Most commonly involved gastrointestinal organs are gallbladder and small bowel. Isolated colonic involvement is a rare manifestation of PAN [6], and is represented in our case.
Of the prior studies that report gastrointestinal involvement in PAN, there is limited isolated large bowel disease in their patient cohorts [11]. Hamzaoui et al., at the time of their publication in 2013, identified only 10 published cases of colitis related to PAN [12]. In addition, the few studies that report localized colonic PAN discuss patients with colonic perforation or disease onset and presentation later in life [9, 11, 13]. However, our young patient presented with colonic ischemia without perforation, which is a rare presentation of PAN [9]. The clinical presentation can potentially mimic inflammatory bowel disease and ischemic colitis related to hypoperfusion. Given the potential severity of the disease, timely diagnosis is critical in order to avoid the risks of perforation, hemorrhage, ulceration and obstruction. Our patient’s evidence of frank necrosis in her colon and acute abdominal signs, led her to be taken for surgical resection. Typically, the medical management of PAN involves high-dose steroids with an additional immunosuppressive agent such as cyclophosphamide; however, in the presence of concerning signs for an acute abdomen, urgent surgery for resection of affected bowel should be pursued.
As evidenced by this case, there is no laboratory testing specific for PAN [5]. Diagnosis of concurrent hepatitis can influence management, and imaging can be helpful in the work-up of potential vascular abnormalities. Our patient’s abdominal CTA showed multiple aneurysms, leading us to work up vasculitis as an etiology for her colitis. In an otherwise healthy patient who presents with multiple aneurysms on imaging, PAN should be on the differential diagnosis. Biopsy results are the gold-standard for definitive diagnosis, and in this clinical scenario, her colon biopsy showed active and healed necrotizing arteritis with an ischemic ulcer and contained features consistent with PAN.
CONCLUSION
This case highlights the clinically difficulty of diagnosing PAN, with minimal assistance from laboratory and endoscopy results. Due to the threatening consequences of untreated PAN, all physicians must remain cognizant to PAN on a differential for unexplained abdominal pain, and recognize a variety of available treatment interventions, including the possibility of surgical intervention.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
Footnotes
†Accepted for presentation at: Southeastern Surgical Congress Annual Meeting, Savannah, GA, 11–14 February 2023.
References
- polyarteritis nodosa
- tachycardia
- mycophenolate mofetil
- vasculitis
- aneurysm
- colectomy
- colonoscopy
- diarrhea
- ulcer
- hematochezia
- ischemic colitis
- intestine, large
- leukocytes
- inferior mesenteric artery
- necrosis
- pain
- surgical pathology
- peritonitis
- sigmoid colon
- steroids
- surgical procedures, operative
- rectum
- computed tomographic angiography
- necrotizing vasculitis
- splenic flexure
- colonic wall
- end colostomy
- excision
- left lower quadrant pain



