-
PDF
- Split View
-
Views
-
Cite
Cite
Jia Xi Julian Li, Howard Shihao Fan, Schistosomal appendicitis: a rare cause of a common surgical condition, Journal of Surgical Case Reports, Volume 2023, Issue 4, April 2023, rjad188, https://doi.org/10.1093/jscr/rjad188
Close - Share Icon Share
Abstract
Despite the prevalence of schistosomiasis across the world, appendicitis secondary to schistosomiasis is a rarely encountered presentation even in endemic areas, let alone in developed Western countries. We report a case of a 34-year-old male in Australia with acute appendicitis and subsequent histopathology, demonstrating the presence of schistosome ova. The case highlights the difficulties in pre-operative diagnosis of this entity and the importance of its recognition for the practising surgeon, especially in the developed world, where this rare condition may be encountered because of changing global travel and migration patterns.
INTRODUCTION
Appendicitis secondary to schistosomiasis is a rarely encountered condition even in endemic areas, let alone in developed Western countries. Recognition by the practising surgeon, especially in non-endemic areas, and institution of appropriate treatment with appendicectomy and anti-helminthic therapy are important components to managing the acute appendicitis as well as preventing long-term sequelae of schistosomiasis. We report a case of a 34-year-old male in Australia with acute appendicitis and subsequent histopathology, demonstrating the presence of schistosome ova.
CASE PRESENTATION
We present an interesting case of a 34-year-old male with appendicitis secondary to schistosomiasis. The patient presented to a major Australian tertiary hospital with a 1-day history of abdominal pain, anorexia and nausea. He had no other significant medical history, no regular medications, did not smoke and rarely consumed alcohol. He originated from the Philippines but had been working on a cruise ship as a bartender for the past year.
On initial presentation, he had a heart rate of 80 beats per minute, blood pressure of 130/80 mmHg and was apyrexial with a temperature of 37.5°C. On examination, he had localized tenderness over the right iliac fossa without evidence of peritonism. His blood counts revealed a white blood count of 15.0 ×109/l with a neutrophilia of 12.3 × 109/l and a C-reactive protein of 5.3 mg/l. Computed tomography (CT) imaging revealed an acute uncomplicated appendicitis, with the appendix measuring 9.9 mm (Fig. 1).
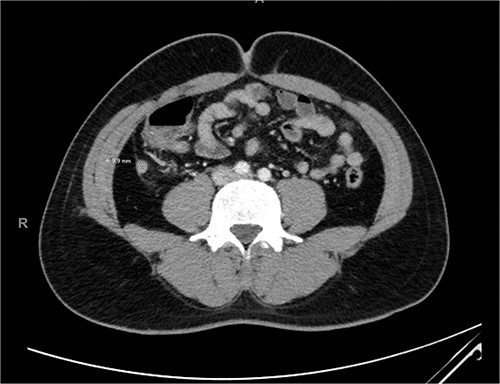
The patient was treated with initial fluid resuscitation and intravenous antibiotics, which was followed by a laparoscopic appendicectomy on the same day of presentation. Intra-operative findings demonstrated an inflamed but non-perforated appendix with overlying fibrinopurulent exudate. He had an uneventful recovery and was discharged the next morning. There were no clinical concerns during clinic follow-up 1 week later.
Subsequent histology demonstrated, in addition to features consistent with acute appendicitis, the presence of amorphous, round calcified deposits within the appendiceal wall and mesoappendix, representing Schistosoma ova (Fig. 2). The patient had no further symptoms and was prescribed a single dose of praziquantel for completion of therapy.
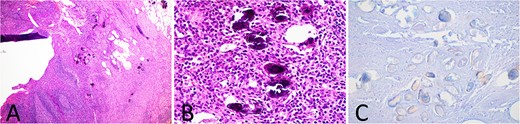
Histology slides of the appendix specimen; (A) (H&E stain, 20× magnification) features of transmural inflammatory infiltrate and serositis consistent with appendicitis and round calcified deposits within the appendiceal wall and mesoappendix; (B) (H&E stain, 400× magnification) amorphous, round, blue-black calcified deposits representing Schistosoma ova; (C) (modified Ziehl-Neelsen stain, 200× magnification) red-brown appearance of the Schistosoma ova shell.
DISCUSSION
Schistosomiasis represents one of the most prevalent parasitic diseases in the world and is endemic in many developing countries [1]. Despite this, appendicitis secondary to schistosomiasis is a rarely encountered condition even in endemic areas, let alone in developed Western countries. A systematic review of the international literature demonstrated a total prevalence of 1.3%, while stratification by continents revealed a prevalence of 2.8% in Africa compared to 0.5% in the Middle East [2]. By contrast, studies in non-endemic countries reveal a prevalence rate of 0.1–0.2% [3, 4].
While the pathophysiological mechanisms of schistosomal appendicitis is incompletely understood, the proposed mechanisms relate to the host immune response to schistosome eggs deposited in the appendix [1, 2]. The ensuing granulomatous inflammation may destroy the eggs as well as the surrounding tissue to cause acute appendicitis or chronic inflammation, and calcification of eggs results in fibrosis and obstruction of the appendiceal lumen with secondary bacterial infection [4, 5].
Clinical presentation of schistosomal appendicitis is indistinguishable from other causes of acute appendicitis, and routine haematological and biochemical investigations provide limited additional information to suggest a schistosomal aetiology [2]. When suspected based on risk factors, serology, polymerase chain reaction assays and presence of eggs in urine or faeces may be used to establish schistosomal infection, although diagnosis of schistosomal appendicitis requires histopathological confirmation with the presence of schistosomal ova and granulomatous inflammation in the appendix [1, 2, 6].
Treatment of the acute appendicitis is with appendicectomy. As appendicitis may be the first presentation of underlying schistosomiasis, confirmation on histopathology is valuable in initiating subsequent anti-helminthic therapy to eradicate the parasite and prevent its sequelae [1, 2]. With changes in global migration patterns and returning travellers from endemic to non-endemic areas, the practising surgeon, particularly in developed Western countries, needs to be increasingly cognizant of schistosomiasis as a rare cause of appendicitis and its implications on further treatment.
ACKNOWLEDGEMENTS
The authors would like to acknowledge the Anatomical Pathology Department at St Vincent’s Pathology for the review and provision of the histology slides included in this case report.
CONFLICT OF INTEREST STATEMENT
The authors have no conflicts of interest to declare.
FUNDING
No funding was received for the preparation and publication of this case report.
DATA AVAILABILITY
No new data were generated or analysed in support of this research.



