-
PDF
- Split View
-
Views
-
Cite
Cite
Jane Tian, Shubham Bhatia, Youssef Mourad, Philip Hall, Martine A Louis, Noman Khan, A feeding jejunostomy causing an intussusception – case report and literature review, Journal of Surgical Case Reports, Volume 2022, Issue 9, September 2022, rjac446, https://doi.org/10.1093/jscr/rjac446
Close - Share Icon Share
Abstract
Use of enteral nutrition has increased dramatically over the past two decades due to improved nutritional formulas, better quality feeding tubes and the ability to use less invasive endoscopic, fluoroscopic and laparoscopic techniques. Intussusception accounts for 1–5% of adult intestinal obstructions, with feeding tubes acting as a lead point in < 1% of cases. Since intussusception is rare, especially in adults, it is not always considered in the initial differential diagnosis of patients presenting with abdominal pain, nausea, vomiting or constipation. If left untreated, intussusception can eventually lead to bowel compromise, poor outcomes and even death. Therefore, prompt recognition and correction are necessary. We present a case of small bowel obstruction in an elderly male secondary to a tube-related intussusception. A review of the signs, symptoms and treatment recommendations is provided.
INTRODUCTION
Adult intussusception is a rare clinical entity accounting for only 5% of all cases with resulting bowel obstruction in < 5% of those cases [1]. The majority of instances in adults can be attributed to a pathological lead point, most commonly malignancy [1]. The incidence of enteral feeding access with gastrostomy tubes (GTs) or jejunostomy tubes (JTs) as the cause of intussusception is <1% of adult cases [2].
Since intussusception in adults is exceedingly rare, especially with feeding tube involvement, it has not been well-described in the literature. Clinical presentation can be vague with symptoms such as abdominal pain, nausea, vomiting or constipation. The exact mechanism causing tube-related intussusception is unknown. A high index of suspicion is needed, and prompt surgical treatment may be required. Here we present a 70-year-old male initially presenting with a clogged JT. Imaging workup revealed a bowel obstruction secondary to intussusception around his JT. Despite removing the JT, operative intervention was still required.
CASE REPORT
A 70-year-old male with a significant surgical history of a Billroth type II reconstruction was admitted with a dislodged percutaneous endoscopic gastrectomy (PEG). After unsuccessful attempts for reinsertion, he underwent laparoscopic JT placement.
Three weeks later, he presented with a JT obstruction. Multiple attempts using carbonated fluids, enzymes and mechanical brushing failed to clear the obstruction. A computerized tomography of the abdomen and pelvis (CTAP) confirmed the position of the JT and demonstrated telescoping of a long 17 cm segment of jejunum starting from the tip of the JT as lead point (Fig. 1). The JT was removed in hopes of resolution. However, repeat CTAP showed persistent intussusception with mesenteric fat stranding, and possible intestinal ischemia (Fig. 2).
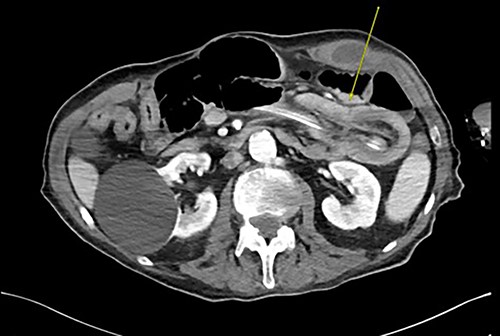
CT abdomen and pelvis revealing telescoping of J-tube (yellow arrow).
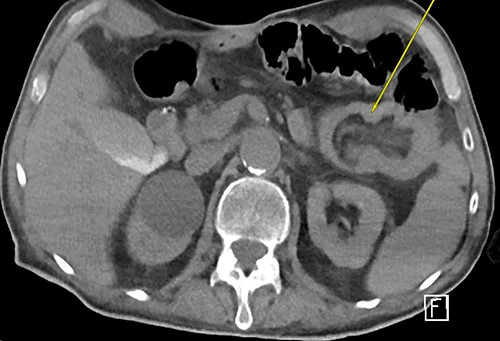
Repeat CTAP s/p JT removal revealed persistent J–J intussusception (yellow arrow).
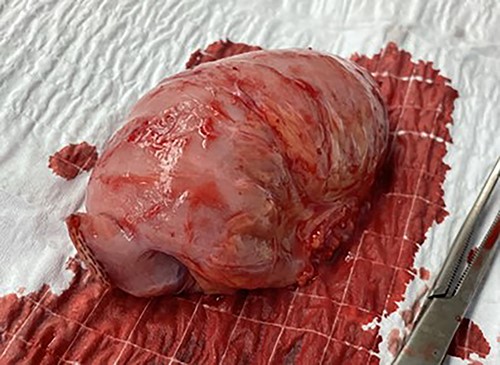
The patient underwent an exploratory laparotomy identifying the segment of intussusception in the jejunum (Fig. 3). The segment was resected (Fig. 4) and a new JT was placed. The patient was discharged successfully 8 days later. Final pathology revealed findings consistent with intussusception.
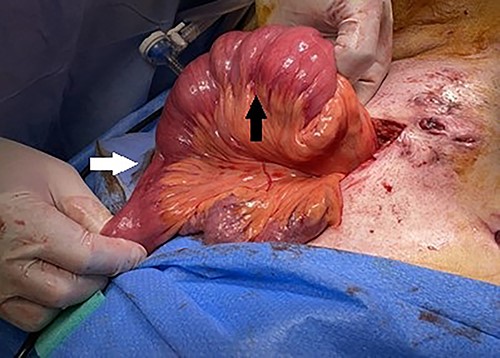
Intraoperative findings of jejunojejunal intussusception with distal collapsed bowel (white arrow) and proximal dilated bowel (black arrow).
DISCUSSION
Adult intussusception is rare, causing <5% of all bowel obstruction. Compared with those in children, 70–90% of adult intussusceptions have pathological lead points such as adhesions, inflammatory disease, benign lesions or malignant neoplasms, which represent 24% of cases [1]. When no lead point is identified, prolonged and excessive dryness of the intestines, local hypoxia, anesthetic agents or postoperative drugs are all possible explanations [2]. Functional and mechanical features, such as digestive tract antiperistalsis, gastroparesis, Roux stasis dysmotility syndrome, adhesions near suture lines and shortening of jejunal mesentery have been implicated [3]. Intestinal anastomosis in Billroth II or Roux-en-Y surgery may be associated with postoperative intussusception [4]. Retrograde jejunogastric intussusception is the most common type of intussusception after abdominal surgery, whereas jejunojejunal intussusception is rare [3].
A gastrojejunostomy tube acting as a lead point for intussusception accounts for 1% of cases. Retrograde jejunojejunal intussusception starting with a feeding JT has been reported [5]. In a review of 1840 patients with gastrointestinal anastomosis and gastrojejunostomy tube insertion, only seven (0.438%) presented with postoperative intussusceptions related to feeding tubes [6]. The exact mechanism remains unclear. Current literature assumes that a foreign body may cause intraluminal irritation, postoperative changes such as intermittent spasms or bowel edema can interfere with normal peristalsis, all triggering an invagination [7]. In our case, no contributors other than the JT were found.
To date, there is no consensus on feeding tube length and its role in postoperative intussusception. Some report that intussusception is more likely to occur when the feeding tube is farther away from the anastomosis, with a shorter JT causing the intestines to shrink over the tube, or with enteral formulas with low pH [8]. Some evidence suggests that intussusception is more frequent with larger tubes, with a distant tip acting as a leading point [9]. Some suggest that GT balloons are culprits. Manual manipulation of the tube with an inflated balloon during active peristalsis can result in telescoping [10]. In addition, angulation during tube placement has been suggested as a factor [11].
Idiopathic postoperative intussusception in adults occurs between the ages of 45 and 50. It is most common on the fourth or fifth day after surgery. Tube-related intussusception typically occurs later with a median time of 6 years after surgery (range 10 months to 18 years). [5].
Since clinical manifestations are vague in around 20% of cases, diagnosing adult intussusception may be challenging and time consuming. Clinical manifestations of postoperative intussusception can be acute and severe or chronic and indolent. Long-standing intussusception may go unnoticed, with resulting weight loss and fatigue. Abdominal discomfort, nausea and vomiting occur in around 70% of patients [3]. When an adult patient presents after a feeding tube placement with nausea, vomiting and non-specific abdominal pain, diagnostic modalities should begin with an abdominal ultrasound (US), although CTAP is preferred [12]. A sausage shaped mass, or an air fluid column on imaging should raise the suspicion for intussusception. The lead point can be identified as a ‘target sign’ or a three-layer structure including the intestinal wall, the mesentery and lining of the intestines [13]. CTAP is accurate for diagnosing intussusception in over 75% of cases [14]. Combining CT and US can increase pre-op diagnosis to 95.5% [15].
Although radiographic signs of JT intussusception may be transient, and intussusception can rarely spontaneously resolve, patients often need surgery. There is no standard technique and operative management can be done by laparoscopy or laparotomy. Most patients with intussusceptions secondary to surgically placed feeding tube do not require a new gastrointestinal anastomosis, as the JT is usually inserted > 20 cm away from the anastomosis. The surgical procedure may be limited to reduction of the intussusception, but bowel compromise requires resection [5]. Almost all resections are done with primary anastomosis, except in cases of peritonitis secondary to intestinal perforation.
Tube feedings often provide nutritional support to frail patients with increasing disease complexity. Tube-related intussusception is rare but may lead to bowel ischemia, requiring a high index of suspicion, prompt imaging studies and often surgical intervention.
ACKNOWLEDGEMENTS
The authors thank Dr Neil Mandava, Chairman, Department of Surgery, Flushing Hospital Medical Center.
CONFLICT OF INTEREST STATEMENT
The authors declare that there is no conflict of interest.
FUNDING
The authors received no financial support for the research, authorship, and/or publication of this article.



