-
PDF
- Split View
-
Views
-
Cite
Cite
Tran Que Son, Tran Hieu Hoc, Tran Thu Huong, Ngo Quang Dinh, Pham Van Tuyen, A ruptured pancreatic pseudocyst causes acute peritonitis with clinical characteristics of a gastrointestinal tract perforation, Journal of Surgical Case Reports, Volume 2022, Issue 5, May 2022, rjac164, https://doi.org/10.1093/jscr/rjac164
Close - Share Icon Share
Abstract
Intraperitoneal air in pancreatic pseudocysts is a rare complication that can jeopardize hemodynamic stability and requires emergency surgery. A 61-year-old man was admitted to our hospital after abdominal pain, vomiting and diarrhea. Computed tomography showed a hollow visceral perforation with intraperitoneal air and two pseudocysts close to the pancreas. The patient was transferred to the emergency operating room with symptoms of septic shock. We histopathologically diagnosed a ruptured pancreatic pseudocyst combined with an intracystic haemorrhage. We resected a portion of the pseudocyst wall using surface electrocautery inside the lumen, cholecystectomy and peritoneal toilet and maintained adequate external drainage. The patient was discharged on postoperative Day 12. The patient achieved relapse-free survival for 12 months postoperatively. Ruptured pancreatic pseudocysts with extraluminal gas are dangerous if effective medical interventions are not performed. Emergency surgery should be completed as soon as possible to drain the pancreatic cyst and cleanse the abdomen.
INTRODUCTION
A pancreatic pseudocyst (PP) is a well-known consequence of acute and chronic pancreatitis that can occur in either acute or chronic pancreatitis [1]. About half of them drain into the free peritoneal, port vein [2] or splenic vein [3–5]; the remainder leak into a nearby hollow organ [6–8]. When a pseudocyst ruptures into the intra-abdominal cavity, it can cause peritonitis, fatal if not adequately treated [1]. To the best of our knowledge, there is no report in the literature on ruptures resulting in peritonitis and abdominal gas. This disorder is frequently mistaken for peritonitis, which occurs due to gastrointestinal (GI) tract perforation.
Herein, we report a rare case of spontaneous rupture of an infectious PP in a patient with clinical characteristics of hollow visceral perforation. We successfully treated with pseudocyst resection combined with external drainage.
This report can be helpful for clinicians’ education and clinical practice purposes in terms of surgical indications and treatment options based on clinical characteristics. This case report was written by CARE guidelines [9].
CASE REPORT
A 61-year-old man was transferred to our hospital after presenting abdominal pain, vomiting and diarrhea for 3 days. The patient was not a heavy drinker but has had type 2 diabetes for 10 years, for which he is currently receiving daily insulin treatment.
Laboratory data showed a high inflammatory reaction and renal dysfunction: white blood cell count 2670/μL, C-reactive protein 15.03 mg/dL, aspartate aminotransferase 13 IU/L; alanine aminotransferase 7 IU/L; total bilirubin 32.5 μmol/L; serum amylase 88 U/L; serum lipase 152 U/L; urea 9.8 mmol/L, creatinine 135 μmol/L.
On admission, computed tomography (CT) scans revealed a significant amount of free abdominal fluid and identified the presence of extraluminal gas showed signs of GI perforation, as well as intra-cholecyst gallstones (Fig. 1). The pancreatic parenchyma has many calcified nodules. The patient was transferred to our emergency operating room with symptoms of septic shock. Subsequently, the abdominal cavity was aspirated with 1248 mL of the infected fluid. However, we found an entire GI tract and a rupture in the pseudocyst wall filled with a turbid fluid, similar to intra-abdominal fluid (Fig. 2a and b). This PP was encircled by the jejunal loop, digestive mesentery and splenic flexure of the colon, all located on the right side of the abdomen. The diametric pseudocyst was extremely large and connected with the intestinal lumen. We performed a partial resection of the pseudocyst wall surface electrocautery inside the lumen of the PP (Fig. 3).
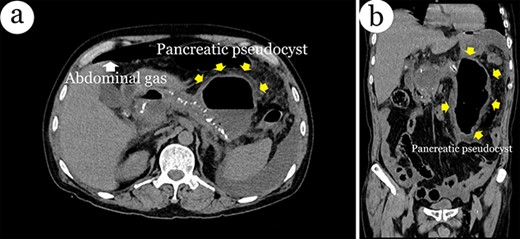
Computerized tomography of the abdomen with intravenous contrast shows a massive pseudocyst within the left side of the abdomen, extraluminal gas and gallstones in axial plane (a) and coronal plane (b).
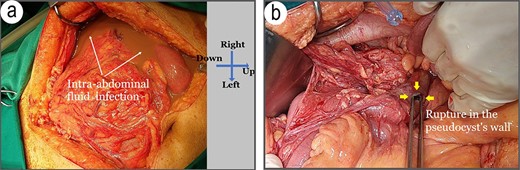
Injuries identified during surgery. (a) A large volume of infected intraperitoneal fluid, (b) a breach in the pseudocyst’s wall filled with a turbid fluid identical to that found in the abdomen (white arrow).
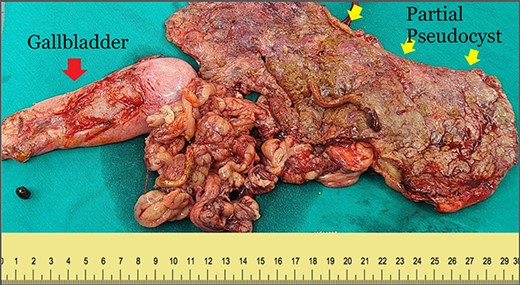
Postoperative specimens included the gallbladder (red arrow), part of the PP wall (yellow arrow) and the great omentum.
Histopathological examination indicated that the pancreatic cyst wall lacked endothelial cells was composed of fibroblasts with collagen fibres bordering the hematoma (Fig. 4a and b). We determined that the patient had peritonitis due to an infected PP rupture accompanied by an intracystic haemorrhage.
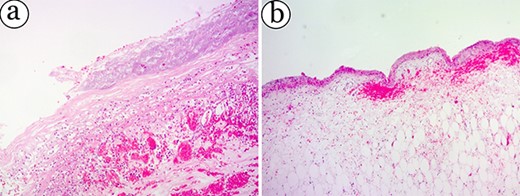
On the micrograph of a partial pancreatic pseudocyst. However, epithelial lining cells of cysts are absent—haemorrhage and oedema in lamina propria. (a, H&E stain, ×50; b, H&E stain, ×50).
We cleaned the abdominal cavity with 10 L of a 0.9% saline solution inserted into the drain. The patient was observed, and antibiotics were prescribed (meropenem 1 g × 3 vials for intravenous infusion in 3 divided doses; metronidazole 0.5 g × 2 vials for intravenous injection divided into 2 doses).
The patient spent 12 days in the hospital. Ultrasonography 12 months after surgery revealed no intra-abdominal fluid or PPs.
DISCUSSION
According to the updated Atlanta classification, a simple cyst is a confined fluid collection within an epithelial-walled capsule. A pseudocyst is a fluid collection covered by fibre and a granular tissue wall that is not epithelialized. Pseudocysts occur in 5–16% acute pancreatitis and 20–40% chronic pancreatitis [10]. Several factors contribute to increased risk: progressive digestion of the cyst wall by proteolytic enzymes activated by enterokinase, leading to invasion into adjacent structures, increased intra-abdominal pressure and minor abdominal trauma [11]. With the progression of the disease, PP rupture can occur in the GI tract lumen or the peritoneal cavity with ascites and severe peritonitis [5, 7, 8, 12, 13].
A literature review also found that surgical treatment of ruptured PPs is unusual, with only a few cases (Table 1). Traditionally, the ideal surgical option is drainage of the cyst to the GI tract through cystogastrostomy, cystoduodenostomy, Roux-en-Y gastrojejunostomy, distal pancreatectomy and lavage [6]. Therefore, local conditions make internal drainage impossible when a rupture occurs [12, 14]. Most of the operations were conducted using open procedures. It is critical to achieve the peritoneal toilet and maintain adequate external drainage in such cases. Following drainage, the recurrence rate of pseudocysts is 2.5–5%; however, comorbidities may reach 30% [15]. An emergency procedure must be performed based on the patient’s hemodynamic instability. To our knowledge, there are only a few reports of emergency laparoscopic surgery or endoscopic ultrasonography-guided drainage for the treatment of ruptured PPs [1, 2]. Several aspects need to be considered, including the patient’s hemodynamic instability, difficulty resecting a massive, actively infected pseudocyst using a minimally invasive approach and the surgeon’s prior experience (Table 1).
| N0 . | Author . | Year . | Age . | Sex . | Medical history or/and combined disease . | Size of pseudocyst (maximum) (cm) . | Cause of rupturation . | Method . | Days of hospital . |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Stavrou | 2008 | 5 | F | N/A | 8 | Abdominal blunt trauma | CT-guided drain was inserted percutaneousley | 50 |
| 2 | Rocha | 2016 | 50 | F | N/A | 23 | N/A | Cystojejunostomy | 10 |
| 3 | 2016 | 59 | M | N/A | 11 | N/A | External drainage, extensive peritoneal toilette and lavage system | 30 | |
| 4 | Okamura | 2017 | 74 | M | Renal Cell Carcinoma | N/A | Intracystic hemorrhage | Distal pancreatectomy with concomitant resection of transverse colon and left kidney | 29 |
| 5 | Gerosa | 2018 | 64 | M | N/A | 12 | Inflammatory of the cystic wall | Cystogastrostomy | 15 |
| 6 | Mujer | 2018 | 50 | F | N/A | 13.6 | N/A | Laparotomy; Roux-en Y cyst jejunostomy | N/A |
| 7 | Jehangir | 2019 | 34 | F | Pancreatic panniculitis | 20.3 | N/A | Surgical lavage and supportive care | 8 |
| 8 | Koizumi | 2020 | 75 | M | Autoimmune pancreatitis | 15 | N/A | EUS-guided drainage Double-pig-tail plastic stent into the ruptured cyst via the gastric wall | 30 |
| 9 | Linn | 2020 | 53 | M | Coronary artery bypass grafting. Follicular lymphoma | 17.7 | N/A | Emergency laparoscopic necrosectomy, distal pancreaticosplenectomy and cholecystectomy | 32 |
| 10 | Linn | 2020 | 66 | M | CBD-stones ERCP-ES | 11 | N/A | Hand assistance. Necrosectomy and cholecystectomy, pancreatosplenectomy | 24 |
| 11 | Park | 2021 | 46 | M | EUS-guided intervention | 9 | Intracystic hemorrhage | EUS-guided gastrocystostomy with a fully covered self-expandable metallic stent | 12 |
| 12 | Our | 2022 | 61 | M | Diabetes Gallstones | 17 | Inflammatory of the cystic wall | Partial resection of the pseudocyst wall, surface electrocautery inside the lumen cholecystectomy | 12 |
| N0 | Author | Year | Age | Sex | Medical history or/and combined disease | Size of pseudocyst (maximum) | Cause of rupturation | Method | Days of hospital |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Stavrou | 2008 | 5 | F | N/A | 8 | Abdominal blunt trauma | CT-guided drain was inserted percutaneousley | 50 |
| 2 | Rocha | 2016 | 50 | F | N/A | 23 | N/A | Cystojejunostomy | 10 |
| 3 | 2016 | 59 | M | N/A | 11 | N/A | External drainage, extensive peritoneal toilette and lavage system | 30 | |
| 4 | Okamura | 2017 | 74 | M | Renal Cell Carcinoma | N/A | Intracystic hemorrhage | Distal pancreatectomy with concomitant resection of transverse colon and left kidney | 29 |
| 5 | Gerosa | 2018 | 64 | M | N/A | 12 | Inflammatory of the cystic wall | Cystogastrostomy | 15 |
| 6 | Mujer | 2018 | 50 | F | N/A | 13.6 | N/A | Laparotomy; Roux-en Y cyst jejunostomy | N/A |
| 7 | Jehangir | 2019 | 34 | F | Pancreatic panniculitis | 20.3 | N/A | Surgical lavage and supportive care | 8 |
| 8 | Koizumi | 2020 | 75 | M | Autoimmune pancreatitis | 15 | N/A | EUS-guided drainage | 30 |
| 9 | Linn | 2020 | 53 | M | Coronary artery bypass grafting. | 17.7 | N/A | Emergency laparoscopic necrosectomy, distal pancreaticosplenectomy and cholecystectomy | 32 |
| 10 | Linn | 2020 | 66 | M | CBD-stones | 11 | N/A | Hand assistance. | 24 |
| 11 | Park | 2021 | 46 | M | EUS-guided intervention | 9 | Intracystic hemorrhage | EUS-guided gastrocystostomy with a fully covered self-expandable metallic stent | 12 |
| 12 | Our | 2022 | 61 | M | Diabetes | 17 | Inflammatory of the cystic wall | Partial resection of the pseudocyst wall, surface | 12 |
M, male; F, female; CBD, Common Bile Duct; ERCP-ES, Endoscopic Retrograde Cholangiopancreatography-Endoscopic Sphincterotomy; EUS, Endoscopic ultrasound; N/A, Not Available
Emergency surgery was performed because we suspected peritonitis caused by perforation of the hollow viscera. In the literature, PP was successfully treated with endoscopic ultrasound (EUS)-guided gastrocystostomy with a fully covered self-expandable metallic stent or emergency laparoscopic surgery performed for ruptured PP [2] (Table 1). Strong cooperation with the endoscopist, laparoscopic splicing equipment and experienced surgeons is required to accomplish these procedures. We first performed open surgery on this patient to shorten the operative time and avoid the difficulties associated with laparoscopic surgery when the patient is in a state of shock, has acute peritonitis. We did not create an anastomosis to aid in the outflow of the PP into the GI system, thus avoiding the need for an external drain. Initially, as the pseudocyst wall was thin, we could not remove the complete wall of the PP as the cyst was closely attached to adjacent structures. However, we were cautious if the pseudocyst communicates with the pancreatic duct, resulting in pancreatic leakage following surgery. As a result, abdominal drainage may continue for more than a week after the procedure.
CONCLUSION
Ruptured PP with abdominal free air is a dangerous and uncommon clinical manifestation. Emergency surgery should be performed as soon as possible to drain the pancreatic cyst and cleanse the abdomen.
AUTHORS' CONTRIBUTIONS
All the authors have substantial contributions to the manuscript.
T.Q.S., T.H.H.: conception, drafting the manuscript, interpretation of data and critical revision of the necessary intellectual content, edited picture and final edit manuscript. T.T.H.: concept, drafting the manuscript, review literature.
N.Q.D., P.V.T.: Interpretation of data, critical revision of the essential intellectual content.
All authors approved the final version to be published.
ACKNOWLEDGEMENTS
We would like to express our most profound appreciation to the leadership of the department of anesthesiology and the Center of emergency medicine for supporting the completion of this article. Many thanks to The Editage Team (www.editage.com) for editing a draft of this manuscript.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
The author(s) received no financial support for this article’s research, authorship, and publication.
ETHICS APPROVAL
Our institution does not require ethical approval for reporting individual cases or case series.
INFORMED CONSENT
Verbal informed consent was obtained from the patient for their anonymized information published in this article.
REFERENCES
Author notes
T. Q. Son and T. H. Hoc contributed equally to this work.
- hemodynamics
- abdominal pain
- computed tomography
- hemorrhage
- septic shock
- cholecystectomy
- diarrhea
- operating room
- pancreatic cyst
- pancreatic pseudocyst
- rupture
- vomiting
- abdomen
- electrocoagulation
- pancreas
- peritoneum
- pseudocyst
- gastrointestinal tract
- peritonitis, acute
- therapeutic intervention
- intraperitoneal infusion
- doppler hemodynamics
- emergency surgical procedure



