-
PDF
- Split View
-
Views
-
Cite
Cite
Naoki Ishimaru, Hirohisa Fujikawa, Yoshifumi Kobayashi, Large bowel obstruction caused by a colonic polyp, Journal of Surgical Case Reports, Volume 2022, Issue 5, May 2022, rjac161, https://doi.org/10.1093/jscr/rjac161
Close - Share Icon Share
Abstract
A large bowel obstruction (LBO) is an emergency condition that requires early diagnosis and prompt treatment, and it is also crucial to identify the cause of the obstruction. Here, we describe a 76-year-old woman who presented to the hospital with a 1-day history of abdominal pain and vomiting and was diagnosed with LBO. Endoscopic findings showed that the cause of the LBO was initially determined to be a Bormann Type I tumour in the sigmoid colon. However, the surgery was performed later; the pathological findings led to the diagnosis of colonic obstruction caused by a colonic polyp in the sigmoid colon narrowed by chronic diverticulitis. Colonic polyps rarely cause LBO. Poor observation due to colonic stenosis can mask the morphology of the lesion. In cases of LBO, colonic polyps should be differentially diagnosed in addition to colon cancer.
INTRODUCTION
Large bowel obstruction (LBO) is an emergency that requires immediate diagnosis and treatment. Clinical presentation is frequently acute with abdominal pain, bloating and obstipation. It can lead to infarction or perforation of the bowel if not treated promptly [1].
Colorectal cancer is the most common cause of LBO in adults (>60%) [2]. Additional common causes of LBO include entities such as colonic volvulus (11–15%), diverticulitis (4–10%) and adhesions [1]. Other causes are rare (<5%) and include extrinsic, disease and intraluminal foreign bodies [1]. Among these, although an exact incidence is unknown, and a colonic polyp is a very rare aetiology of LBO.
Most cases of LBO ultimately require surgical intervention [3], such as primary resection, ileostomy/colostomy with interval resection and the Hartmann procedure. Self-expanding colonic endoluminal stents have been used as a non-invasive technique [4].
Herein, we report an uncommon case of LBO due to a colonic polyp that was initially misdiagnosed by endoscopy as a carcinoma.
CASE REPORT
A 76-year-old woman presented with a 1-day history of abdominal pain and vomiting. The patient’s previous medical diagnoses included hepatitis C and Type 2 diabetes. On examination, her abdomen was grossly distended and tympanitic with notable tenderness in the lower left quadrant. Laboratory examinations revealed a white cell count of 15.0 (normal 3.5–9.1) × 109/l. Other laboratory results, including carcinoembryonic antigen and carbohydrate antigen 19-9, showed no significant findings. Abdominal computed tomography (CT) revealed LBO with a transition at the level of the sigmoid colon with focal wall thickening (Fig. 1A and B). Colonoscopy was indicative of a Bormann Type I tumour in the sigmoid colon but could not be completed due to narrowing of the bowel lumen (Fig. 1C and D). The colon on the oral side of the lesion was not visualized in a gastrografin study. A guidewire could not pass the lesion, and a colonic stent or a rectal tube could not be placed. Although we inserted a nasogastric tube, the patient vomited and developed aspiration pneumonia due to colonic stenosis, and her general condition deteriorated. Therefore, we decided to perform an emergency surgery. We had initially planned to perform Hartmann’s procedure; however, after a multidisciplinary team meeting with an anaesthesiologist, internists and surgeons, it was thought that the patient would not be able to tolerate major surgical procedures for two reasons. First, on examination, the patient was progressively deteriorating and went into septic shock with a temperature of 40.1°C, pulse rate of 150 beats per minute, blood pressure of 90/55 mm Hg, respiratory rate of 28 breaths per minute and oxygen saturation of 84%, while she was breathing 10 l of oxygen per minute through a reservoir mask, along with impaired consciousness. Second, she was >70 years of age and had multiple co-morbidities, including Type 2 diabetes. Accordingly, she was thought to benefit from a damage control approach rather than a radical resection of the tumour [3], and therefore, we chose to perform a transverse colostomy. Based on the abdominal CT and colonoscopy findings, colon cancer was strongly suspected. We thoroughly explained the risks to the patient of not removing the tumour if it was colon cancer. Nonetheless, she refused to be examined and to have surgery.
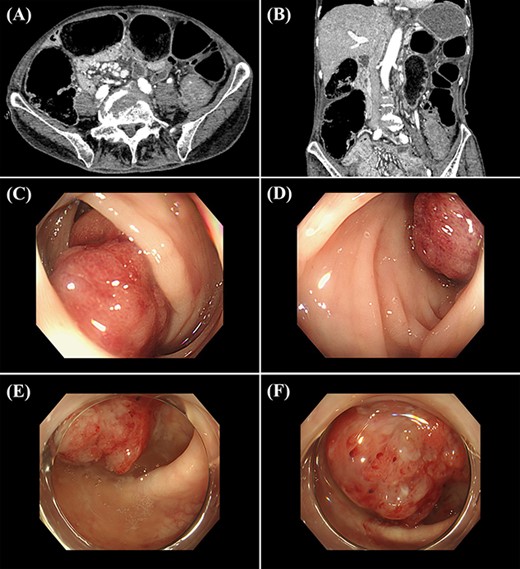
(A and B) abdominal CT shows a colonic obstruction with a transition at the level of the sigmoid colon with a thick wall (A, axial view; B, coronal view); (C and D) colonoscopy shows a lesion similar to a Bormann Type I tumour in the sigmoid colon; (E and F) 3 years later, colonoscopy shows the tumour in the same location.
However, she requested surgery 3 years later because she observed blood and mucus in her stool. Chest-abdomen-pelvis CT scan showed no change in the size of the sigmoid colon mass and no obvious distant metastasis. A repeat colonoscopy revealed that the previously noted tumour was located in the same site, and it was still difficult to pass a scope through the area (Fig. 1E and F). Histological examination of the tumour biopsy showed tubulovillous adenoma. The transverse stoma was closed, and a sigmoid colon tumour resection was performed. Macroscopic pathology showed a sigmoid colon tumour with two heads that were 20 mm in diameter and one stem of 25 mm in length (Fig. 2). However, microscopically, the tumour was not a cancer but was rather a polyp. In the sigmoid colon, there were >10 pseudodiverticula with subserosal fibrosis and haemorrhage, indicating a history of diverticulitis (Fig. 3). These pathological findings led to the diagnosis of LBO caused by a colonic polyp in the sigmoid colon, which was narrowed by chronic diverticulitis.
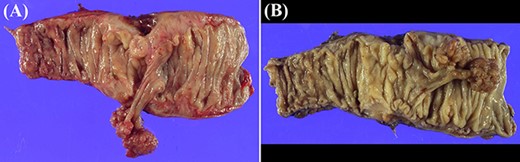
Macroscopic pathological examination demonstrates a sigmoid colon polyp with two heads that were 20 mm in diameter and one stem of 25 mm in length.
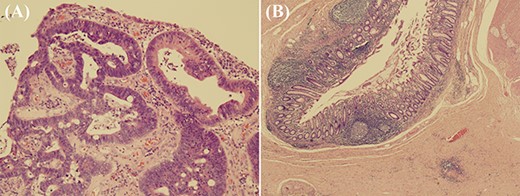
Microscopic pathological findings; (A) in the mucosa of the two heads of the polyp, there is proliferation of atypical villi and tubules with enlarged and stratified nuclei (haematoxylin and eosin stain, original magnification ×100); (B) in the non-tumour area, there are >10 diverticula (pseudodiverticula), some of which show fibrosis and haemorrhage in the subserosal tissue (haematoxylin and eosin stain, original magnification ×20); this finding is consistent with a history of diverticulitis.
The patient was discharged 12 days after the surgery without any complications. At present, the patient has no recurrence after 10 months of follow-up.
DISCUSSION
Colonic polyps are typically found during colonoscopy and rarely cause colonic obstruction [5]. In the present case, the colonic polyp obstructed the sigmoid colon, which was narrowed by chronic diverticulitis. This was a rare case of LBO caused by a polyp that was misdiagnosed as a Bormann Type I tumour due to inadequate endoscopic observation caused by colonic stenosis.
Colonic polyps are overgrowths of the colonic mucosa and carry a risk of malignancy [6]. With colonoscopy, snare polypectomy, endoscopic mucosal resection and endoscopic submucosal dissection are possible and are performed for both diagnostic and therapeutic purposes [7]. Colonic polyps can be treated with endoscopic resection. Histological examination of excisional biopsy specimens determines the curability of treatment and the need for additional surgical resection [8, 9].
LBO is an emergency condition that requires early identification and intervention. The aetiology of LBO varies, but in adults, the most common cause is colorectal cancer [2]. However, as previously mentioned, there are many causes that can lead to LBO. Thus, it is crucial to diagnose the aetiology of colon obstruction by history taking, physical examination and imaging, including colonoscopy and CT [1].
As in this case, poor observation due to colonic stenosis can obscure the morphology of the lesion. In a previous case report, colonoscopy initially diagnosed LBO due to one cancer lesion and resection of the large intestine was performed; however, pathological examination revealed a colorectal polyp in the vicinity of the lesion, which caused the obstruction [10]. In our case, a colonic polyp was initially misdiagnosed as a Bormann Type I tumour because the narrowing of the colon obstructed the view during endoscopic observation.
There are some potential limitations to the methods used in this case. First, a biopsy could not be performed during the first colonoscopy as the patient vomited and her general condition rapidly deteriorated. Second, although we suspected cancer, the patient did not consent to staging scans. Despite these limitations, the present study contributes significantly to the literature by illustrating a rare cause of LBO.
To conclude, we report a rare case of LBO due to a colonic polyp that was initially misdiagnosed by endoscopy as a carcinoma. Although LBO is a life-threatening condition that requires early identification, it is not always possible to determine the cause using colonoscopy. In cases of LBO, colonic polyps should be differentially diagnosed in addition to colon cancer.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.



