-
PDF
- Split View
-
Views
-
Cite
Cite
Yesha Maniar, Hassan Hashmi, Jeffrey Silverstein, Christine Chung, Venkata Kella, Anirudha Goparaju, Superior mesenteric artery thrombosis in a patient with COVID-19 pneumonia and Clostridium Difficle, Journal of Surgical Case Reports, Volume 2022, Issue 5, May 2022, rjac146, https://doi.org/10.1093/jscr/rjac146
Close - Share Icon Share
Abstract
COVID-19, a novel respiratory viral illness, has spread globally and led to over 111 million cases worldwide. Most commonly, patients present with respiratory symptoms, and those with increased severity progress to acute hypoxic respiratory failure. Additionally, a portion of patients are noted to have coagulopathy and are considered to be at an increased risk for thromboembolic events. In this article, we present a unique case of a patient with severe abdominal pain in the setting of COVID-19 pneumonia and community acquired Clostridium difficile, found to have superior mesenteric artery thrombosis requiring exploratory laparotomy, thrombectomy and small bowel resection.
INTRODUCTION
COVID-19, a novel respiratory viral illness primarily transmitted through respiratory droplets, has caused a global pandemic. The first cases were noted in Wuhan, China, over 2 years ago, where patients initially presented with respiratory symptoms and pneumonia of unknown etiology. Those that developed more severe symptoms, required intubation and mechanical ventilation for acute hypoxic respiratory failure [1]. Coagulopathy associated with COVID-19 was also observed and patients were at increased risk for thromboembolic events, most commonly deep venous thrombosis or pulmonary embolism. There have also been cases of arterial thromboembolism, such as ischemic stroke or acute limb ischemia [2]. In our report, we describe a unique case of superior mesenteric artery (SMA) thrombosis in a patient with COVID-19 and Clostridium difficile.
CASE REPORT
An 80-year-old female with a medical history of hypertension and type II diabetes mellitus presented to the emergency department with a 12-hour history of acute onset diffuse abdominal pain with nausea, vomiting and diarrhea. She had a past surgical history of cholecystectomy, no family history of arrhythmias or hypercoagulability and no history of smoking or illicit drug use. Initial vital signs were significant for blood pressure 217/123, heart rate 101 and oxygen saturation 91% on 5 L nasal cannula and a temperature of 36.6°C. On physical exam, she was noted to be in significant distress and writhing in pain. She was alert and oriented to person, time and place. She was noted to be in sinus tachycardia and tachypneic with diffuse crackles bilaterally. On abdominal exam, she was soft, non-distended and non-tender to palpation. Laboratory studies were significant for a lactic acid 2.4 on venous blood gas, a normal white blood cell count with 82% neutrophils and INR 1.23. Additionally, she was found to be positive for COVID-19 (cobas SARS-CoV-2 RT-PCR) and her stool assay was positive for C. difficile (Xpert C. difficile assay). Chest x-ray showed bilateral mild to moderate interstitial and ground glass opacities. CT abdomen and pelvis with intravenous (IV) contrast showed a 1.7 cm occlusion of the proximal SMA with distal reconstitution and no evidence of bowel ischemia (Fig. 1).
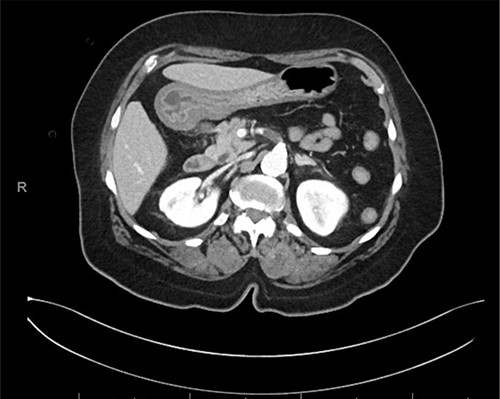
CT abdomen and pelvis with IV contrast, axial image of 1.7 cm occlusive thrombus of proximal SMA.
The patient received broad spectrum antibiotics and fluid resuscitation. She was emergently taken to the operating room, and underwent an exploratory laparotomy, thrombectomy of SMA, and resection of 60 cm of ischemic distal ileum. The patient was left in discontinuity with an open abdomen and admitted to the surgical intensive care unit (SICU). In the SICU, she was started on continuous IV heparin therapy. On post-operative Day (POD) #2, she was taken back to the operating room, with additional resection of 14 cm of ileum with primary anastomosis, palpable pulse of SMA noted and abdominal closure.
The patient remained intubated post-operatively and required ventilatory support for management of COVID-19 pneumonia. She continued with antibiotic treatment of C. Diff, remained on a continuous IV heparin infusion, and received IV dexamethasone and IV remdisivir for treatment of COVID pneumonia. On POD#4, she was not able to respond to commands, or move her extremities even when sedation was held. Initially the patient remained unstable for transport to CT scan due to ongoing ventilatory management, requiring airway pressure release ventilation.
On POD#9, she had been on stable ventilatory settings, and underwent CT head non-contrast that demonstrated no intracranial hemorrhage or infarct. Her decline in mental status was thought to be due to COVID encephalopathy. On POD#10, she had a decrease in her hemoglobin and hematocrit and a positive fecal occult blood test, requiring two units of packed red blood cells with adequate response.
The patient had an increasing fraction of inspiratory oxygen requirement with no improvement in arterial oxygen measurements. Despite maximal ventilatory settings, she was unable to maintain oxygen saturation. Additionally, she had a rising creatinine that did resolve with IV fluid administration. On POD #12, there was a discussion with the family regarding pursuing further medical treatment and the patient was made DNR and the family deferred hemodialysis. On POD#14, due to increasing oxygen requirements and no clinical improvement, the family decided to pursue palliative extubation.
DISCUSSION
Acute mesenteric ischemia (AMI) has a mortality rate of 26%, which has declined since the 1990s with improvement in diagnosis and imaging. It is often a diagnosis that is missed initially and discovered when it is too late to successfully treat. The most common cause of AMI is SMA occlusion from embolism in 70% of cases and thrombosis in 30% of cases [3].
AMI is an uncommon complication of COVID-19 and C. diff, with our case being one of the first cases reported in the literature. Although patients with COVID-19 do present with thromboembolic complications, these complications are usually deep venous thrombosis or pulmonary embolism [2]. There have been rare cases of superior mesenteric vein thrombosis as well [4]. In a literature review of AMI in patients with COVID-19, there were 13 cases previously reported with an average age of 56 years and median day of diagnosis on hospital Day 7. Of these cases, 10 patients underwent surgery and 4 out of 13 patients expired [5]. Although the exact pathogenesis remains unknown, one possible explanation for AMI in COVID-19 is the combination of hypercoagulability, endothelial dysfunction, hypoxia and immobilization [6].
Additionally, C. diff has not been previously associated with AMI. However, intra-abdominal inflammatory conditions are a known risk factor for splanchnic vein thrombosis [7]. One case report describes a patient with abdominal pain, COVID-19 and C. diff, diagnosed with portal vein thrombosis [8]. The combination of intra-abdominal infection, and COVID-19 could be associated with splanchnic vessel thrombosis.
CONCLUSION
Since patients with COVID-19 can present with gastrointestinal symptoms, it can be difficult to determine whether these symptoms are part of the viral illness or AMI [9]. Additionally, C. diff is not a known risk factor for AMI. Our case report demonstrates that in patients with abdominal pain, intra-abdominal infection and COVID-19, AMI should be considered as part of the differential with prompt imaging to establish a diagnosis.
References
- abdominal pain
- hypoxia
- blood coagulation disorders
- clostridium
- pneumonia
- respiratory insufficiency
- signs and symptoms, respiratory
- thrombectomy
- virus diseases
- small-intestine resection
- thromboembolic event
- laparotomy, exploratory
- community
- clostridium difficile
- superior mesenteric artery thrombosis
- covid-19



