-
PDF
- Split View
-
Views
-
Cite
Cite
Daniel Isaac, Fondas Haris, Dean Panos, Jason Diab, Zackariah Clement, Inguinal bladder hernia: differentials for a male groin mass, Journal of Surgical Case Reports, Volume 2022, Issue 11, November 2022, rjac493, https://doi.org/10.1093/jscr/rjac493
Close - Share Icon Share
Abstract
Inguinal bladder hernia (IBH) is an uncommon occurrence in males with a groin mass. It may be present with lower urinary tract symptoms but is often asymptomatic, making it a diagnostic challenge. IBH is frequently an incidental finding during surgery, which increases the risk of iatrogenic injury of the bladder. This report examines the case of a 77-year-old male who experienced a painful, reducible right-sided groin mass with acute urinary retention. Investigations conducted through computed tomography exhibited a right indirect inguinal hernia containing omental fat and a portion of the urinary bladder. The patient underwent a right open herniorrhaphy with mesh repair. This report presents a systematic approach to differential diagnoses for a male groin mass and its relationship to IBH.
INTRODUCTION
Groin mass is a common occurrence in the inguinofemoral region. In men, the most common occurrence is an inguinal hernia, whereas in females, femoral hernia is most common. There are several other underlying pathological processes for a groin mass including cysts, infection/inflammation, vascular, neoplasms and congenital abnormalities. Clinical history and physical examination are normally sufficient in diagnosing an inguinal hernia; however, urinary symptoms and renal failure should prompt consideration for other differentials. This case report examines a 77-year-old man who was diagnosed with a right-sided inguinal bladder hernia (IBH) and explores the differential diagnoses for a male groin mass, examining the key features of an IBH.
CASE REPORT
A 77-year-old male was admitted to the emergency department with a gradual 3-day onset of sharp right-sided groin pain, a decrease in the urine output and a new mass. The lump and pain were prominent when standing, extending into the scrotum and reduced spontaneously when lying. He was opening his bowels and experienced diarrhoea for 1 week; however, he did not report any vomiting.
His medical history included chronic kidney disease and cystitis treated 4 weeks prior. His surgical history included a transurethral resection of the prostate for benign prostatic hyperplasia before 1 year. Post-operatively, the patient developed urinary retention leading to the insertion of a permanent supra pubic catheter. On examination, the right inguinal region was swollen and tender. The inguinal mass was reducible on palpation with a pronounced cough impulse both when the patient stood upright and lied down. The scrotum and perineum did not demonstrate any swelling, erythema or mass.
Biochemical results showed a serum sodium of 129 mmol/l, serum creatinine 168 μmol/l (baseline 104 μmol/l) and estimated glomerular filtration rate 33 ml/min/1.73m2. Urinalysis was positive for leukocytes and blood. An abdominal computed tomography (CT) scan with contrast showed an incarcerated right indirect inguinal hernia containing omental fat and a portion of the urinary bladder passing into the scrotum (Fig. 1). The patient received intravenous fluids; his renal function was optimized before he underwent a right open herniorrhaphy with mesh. The patient was discharged 2 days later with no complications.
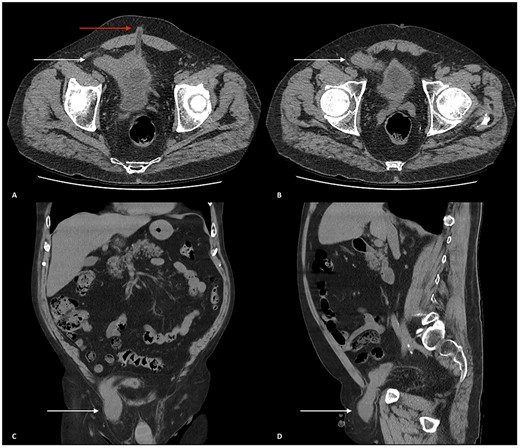
(A and B) Axial CT scan of the abdomen and pelvis showing the urinary bladder herniating into the right inguinal canal (white arrows). (A) Urinary bladder extending towards the right deep inguinal ring before herniating into the right inguinal canal. An umbilical hernia can also be seen (red arrow). (B) Urinary bladder herniating into the inguinal canal. (C) Coronal CT scan of the abdomen and pelvis displaying the urinary bladder herniating into the right inguinal canal and traversing through the right scrotum (white arrow). (D) Sagittal CT scan of the abdomen and pelvis showing the urinary bladder herniating through the right inguinal canal, through the right spermatic cord and positioned superiorly above the right testicle.
DISCUSSION
Male groin mass differentials may be categorized into hernias, cysts, infectious/inflammatory, vascular, malignancy or other causes (Table 1). In males, groin masses occur more frequently than in females with the most common being an inguinal hernia. This is because of a larger inguinal canal in males, containing the spermatic cord allowing contents of the abdominal cavity to pass through more readily. Risk factors of inguinal hernias include a positive family history, chronic obstructive pulmonary disease, smoking, obesity, increased intraabdominal pressure, weak pelvic musculature and collagen vascular disease.
| Categories . | Differential diagnosis . | Typical features . |
|---|---|---|
| Hernia | Indirect inguinal hernia | Protrusion of mass through the deep inguinal ring, lateral to the inferior epigastric artery. |
| Direct inguinal hernia | Mass protrudes through superficial inguinal ring, medial to the inferior epigastric artery. | |
| Femoral hernia | A mass inferior to the inguinal ligament protruding through the femoral ring | |
| Cyst | Hydrocele | Painless scrotal swelling around the testes, which is positive to transillumination. |
| Varicocele | Soft lumps above the testicle, usually described as a ‘bag of worms’. This is because of the dilatation of the scrotal venous pampiniform plexus. | |
| Encysted hydrocele of the spermatic cord | Loculated fluid along the spermatic cord. | |
| Spermatocele | Cyst located at the head of the epididymis that contains fluid and possibly sperm. | |
| Infection/inflammation | Inguinal or femoral lymphadenitis and lymphadenopathy | Inflammation and/or swelling of a singular or multiple lymph node. |
| Psoas Abscess | Painful and erythematous skin, which is associated with a fever, groin lymphadenopathy and flank pain. | |
| Iliopectineal/iliopsoas bursitis | Can be present as pelvic or inguinal masses and is associated with pain. | |
| Vascular | Femoral artery aneurysm | A painless, pulsatile mass in the groin usually accompanied with a loud, continuous murmur upon auscultation. |
| Saphena varix | Saccular swelling of the great saphenous vein. | |
| Other | Cutaneous or subcutaneous masses in the groin • Lipoma • Sebaceous cyst • Haematoma | Lipoma: benign tumour presents as soft lumps of fat tissue. Sebaceous cyst: lesion containing sebum can become inflamed. Hematoma: abnormal collection of blood. |
| Cryptorchidism | The testicle cannot be manipulated in the scrotum, sometimes the testicle is absent from the scrotum. | |
| Neoplasms | Testicular cancer | Hard, painless nodule felt on palpation of the testes. |
| Pelvic malignancy | Develops from the organs of the pelvic region. Is associated with weight loss, lymphadenopathy of the groin and, sometimes, palpable pelvic masses. |
| Categories . | Differential diagnosis . | Typical features . |
|---|---|---|
| Hernia | Indirect inguinal hernia | Protrusion of mass through the deep inguinal ring, lateral to the inferior epigastric artery. |
| Direct inguinal hernia | Mass protrudes through superficial inguinal ring, medial to the inferior epigastric artery. | |
| Femoral hernia | A mass inferior to the inguinal ligament protruding through the femoral ring | |
| Cyst | Hydrocele | Painless scrotal swelling around the testes, which is positive to transillumination. |
| Varicocele | Soft lumps above the testicle, usually described as a ‘bag of worms’. This is because of the dilatation of the scrotal venous pampiniform plexus. | |
| Encysted hydrocele of the spermatic cord | Loculated fluid along the spermatic cord. | |
| Spermatocele | Cyst located at the head of the epididymis that contains fluid and possibly sperm. | |
| Infection/inflammation | Inguinal or femoral lymphadenitis and lymphadenopathy | Inflammation and/or swelling of a singular or multiple lymph node. |
| Psoas Abscess | Painful and erythematous skin, which is associated with a fever, groin lymphadenopathy and flank pain. | |
| Iliopectineal/iliopsoas bursitis | Can be present as pelvic or inguinal masses and is associated with pain. | |
| Vascular | Femoral artery aneurysm | A painless, pulsatile mass in the groin usually accompanied with a loud, continuous murmur upon auscultation. |
| Saphena varix | Saccular swelling of the great saphenous vein. | |
| Other | Cutaneous or subcutaneous masses in the groin • Lipoma • Sebaceous cyst • Haematoma | Lipoma: benign tumour presents as soft lumps of fat tissue. Sebaceous cyst: lesion containing sebum can become inflamed. Hematoma: abnormal collection of blood. |
| Cryptorchidism | The testicle cannot be manipulated in the scrotum, sometimes the testicle is absent from the scrotum. | |
| Neoplasms | Testicular cancer | Hard, painless nodule felt on palpation of the testes. |
| Pelvic malignancy | Develops from the organs of the pelvic region. Is associated with weight loss, lymphadenopathy of the groin and, sometimes, palpable pelvic masses. |
| Categories . | Differential diagnosis . | Typical features . |
|---|---|---|
| Hernia | Indirect inguinal hernia | Protrusion of mass through the deep inguinal ring, lateral to the inferior epigastric artery. |
| Direct inguinal hernia | Mass protrudes through superficial inguinal ring, medial to the inferior epigastric artery. | |
| Femoral hernia | A mass inferior to the inguinal ligament protruding through the femoral ring | |
| Cyst | Hydrocele | Painless scrotal swelling around the testes, which is positive to transillumination. |
| Varicocele | Soft lumps above the testicle, usually described as a ‘bag of worms’. This is because of the dilatation of the scrotal venous pampiniform plexus. | |
| Encysted hydrocele of the spermatic cord | Loculated fluid along the spermatic cord. | |
| Spermatocele | Cyst located at the head of the epididymis that contains fluid and possibly sperm. | |
| Infection/inflammation | Inguinal or femoral lymphadenitis and lymphadenopathy | Inflammation and/or swelling of a singular or multiple lymph node. |
| Psoas Abscess | Painful and erythematous skin, which is associated with a fever, groin lymphadenopathy and flank pain. | |
| Iliopectineal/iliopsoas bursitis | Can be present as pelvic or inguinal masses and is associated with pain. | |
| Vascular | Femoral artery aneurysm | A painless, pulsatile mass in the groin usually accompanied with a loud, continuous murmur upon auscultation. |
| Saphena varix | Saccular swelling of the great saphenous vein. | |
| Other | Cutaneous or subcutaneous masses in the groin • Lipoma • Sebaceous cyst • Haematoma | Lipoma: benign tumour presents as soft lumps of fat tissue. Sebaceous cyst: lesion containing sebum can become inflamed. Hematoma: abnormal collection of blood. |
| Cryptorchidism | The testicle cannot be manipulated in the scrotum, sometimes the testicle is absent from the scrotum. | |
| Neoplasms | Testicular cancer | Hard, painless nodule felt on palpation of the testes. |
| Pelvic malignancy | Develops from the organs of the pelvic region. Is associated with weight loss, lymphadenopathy of the groin and, sometimes, palpable pelvic masses. |
| Categories . | Differential diagnosis . | Typical features . |
|---|---|---|
| Hernia | Indirect inguinal hernia | Protrusion of mass through the deep inguinal ring, lateral to the inferior epigastric artery. |
| Direct inguinal hernia | Mass protrudes through superficial inguinal ring, medial to the inferior epigastric artery. | |
| Femoral hernia | A mass inferior to the inguinal ligament protruding through the femoral ring | |
| Cyst | Hydrocele | Painless scrotal swelling around the testes, which is positive to transillumination. |
| Varicocele | Soft lumps above the testicle, usually described as a ‘bag of worms’. This is because of the dilatation of the scrotal venous pampiniform plexus. | |
| Encysted hydrocele of the spermatic cord | Loculated fluid along the spermatic cord. | |
| Spermatocele | Cyst located at the head of the epididymis that contains fluid and possibly sperm. | |
| Infection/inflammation | Inguinal or femoral lymphadenitis and lymphadenopathy | Inflammation and/or swelling of a singular or multiple lymph node. |
| Psoas Abscess | Painful and erythematous skin, which is associated with a fever, groin lymphadenopathy and flank pain. | |
| Iliopectineal/iliopsoas bursitis | Can be present as pelvic or inguinal masses and is associated with pain. | |
| Vascular | Femoral artery aneurysm | A painless, pulsatile mass in the groin usually accompanied with a loud, continuous murmur upon auscultation. |
| Saphena varix | Saccular swelling of the great saphenous vein. | |
| Other | Cutaneous or subcutaneous masses in the groin • Lipoma • Sebaceous cyst • Haematoma | Lipoma: benign tumour presents as soft lumps of fat tissue. Sebaceous cyst: lesion containing sebum can become inflamed. Hematoma: abnormal collection of blood. |
| Cryptorchidism | The testicle cannot be manipulated in the scrotum, sometimes the testicle is absent from the scrotum. | |
| Neoplasms | Testicular cancer | Hard, painless nodule felt on palpation of the testes. |
| Pelvic malignancy | Develops from the organs of the pelvic region. Is associated with weight loss, lymphadenopathy of the groin and, sometimes, palpable pelvic masses. |
Infrequently, the bladder may be present in ~0.5–5% of male inguinal hernias [1]. IBH increases with age occurring in up to 10% of obese males over 50 years old [2]. Bladder involvement is because of weakness in the bladder wall, causing it to stretch and pass into the inguinal canal. The bladder can also herniate into the femoral canal accounting for 23% of cases, with IBH accounting for 75%. The remaining 2% occur through the perineum, ischiorectal, obturator and abdominal defects [2]. Specific risk factors for bladder wall weakness include chronic bladder distention due to bladder outlet obstruction [3, 4].
Clinically, IBH infrequently has lower urinary tract symptoms including dysuria, straining, intermittent stream, increased frequency and prolonged micturition time [5]. The frequency of symptoms increases in proportion to the size of the bladder herniation. Signs of IBH include a noticeable swelling of the groin and/or scrotum that reduces after voiding. Some patients require manual compression of the mass to complete bladder voiding known as Mery’s sign, which should raise suspicion of IBH and prompt imaging to avoid intraoperative bladder injury [6]. Complications of IBH include acute kidney injury because of obstructive uropathy, bladder infarction because of strangulation, urinary tract infections, epididymitis and rarely malignancy.
IBH symptoms are non-specific, making it a diagnostic challenge. Seven percent are diagnosed preoperatively; 77% are diagnosed intraoperatively as an incidental finding and 16% are diagnosed post-operatively because of complications [7]. Intraoperative IBH diagnosis increases the risk of iatrogenic bladder injury, which has been reported to occur in 12% of all IBH repairs [8]. Diagnosis is made through various imaging modalities with ultrasound being first line due ease of accessibility, demonstrating a hypoechoic mass lesion protruding from the inguinal canal into the scrotum. The gold standard investigation for IBH diagnosis is voiding cystourethrography, showing a ‘dog-ear’ or ‘dumbbell’ bladder. CT and magnetic resonance imaging are useful especially if there are concerns for malignancy [3].
Open herniorrhaphy with mesh is the main method of treatment and is associated with a similar rate of recurrence compared with laparoscopy [9, 10]. Laparoscopically, a total extraperitoneal approach has the lowest risk of complications and allows for visualization of the bladder because of its retroperitoneal position. However, 10.8% of laparoscopic cases are converted to open surgery because of difficulties obtaining a proper operative visual field to mitigate any iatrogenic structural injury [11]. Another disadvantage with this approach is that the hernia sac is not routinely sent for microscopic examination meaning a malignancy, although uncommon, may be missed [9]. Resection of the bladder during surgery is rare and is only performed under the conditions when the bladder is incarcerated, necrotic or when the hernia occurs in combination with a bladder diverticulum or tumour [12]. Post-operative complications include sepsis, haematuria and fistula formation. Hernia recurrence can occur because of a haematoma and/or seroma forming between the mesh and the anterior rectus sheath causing displacement of the mesh [13].
CONCLUSION
Male groin mass is a common occurrence with many differential diagnoses. IBH is similar to an inguinal hernia and should be considered in patients with a groin mass and urinary symptoms. Voiding cystourethrography is the preferred imaging modality in identifying IBH to prevent iatrogenic injury during surgical management.
ACKNOWLEDGEMENTS
We would like to acknowledge and thank Dr Jason Diab.
CONFLICT OF INTEREST STATEMENT
We have no conflicts of interest or sources of funding to declare. Patient consent was obtained.



