-
PDF
- Split View
-
Views
-
Cite
Cite
Sayaka Arita, Tomofumi Nishino, Yuuki Mitani, Kotaro Sakashita, Sho Totsuka, Ryunosuke Watanabe, Hajime Mishima, Hitomi Kawai, Daisuke Matsubara, Yoshionao Oda, Masashi Yamazaki, Hemiarthroplasty for tumor-induced osteomalacia caused by tumor localized in femoral head: a case report, Journal of Surgical Case Reports, Volume 2022, Issue 10, October 2022, rjac478, https://doi.org/10.1093/jscr/rjac478
Close - Share Icon Share
Abstract
Tumor-induced osteomalacia (TIO) is a rare tumor-associated syndrome in which osteomalacia is induced by a tumor. A 67-year-old male patient presented for the first time with low back pain, weakness of the lower extremities and difficulty in walking. Six years earlier, he had nonspecific symptoms such as low back pain, and blood tests showed high alkaline phosphatase and low phosphorus. In addition, fibroblast growth factor 23 (FGF23) was abnormally high at 454 pg/mL. A diagnosis of FGF23-related hypophosphatemic osteomalacia was made. Somatostatin receptor scintigraphy, venous sampling and MRI were performed to localize and diagnose TIO. The tumor was found to be confined to the right femoral head and hemiarthroplasty was performed. Pathological examination revealed a phosphaturic mesenchymal tumor. Postoperatively, symptoms and blood test data improved. Although resection of the lesion and osteochondral transplantation or total hip arthroplasty were considered, hemiarthroplasty was chosen over concerns about treatment failure due to seeding.
INTRODUCTION
Tumor-induced osteomalacia (TIO) is an uncommon paraneoplastic syndrome characterized by nonspecific clinical manifestations such as fatigue, bone pain and fractures leading to a more difficult and longer diagnosis [1]. It is induced by the tumoral expression of fibroblast growth factor 23 (FGF23), whose excess activity is known to cause hypophosphatemia via renal phosphate wasting, leading to decreased production and enhanced catabolism of 1,25-dihydroxyvitamin D [2].
CASE PRESENTATION
A 57-year-old man was referred to our hospital with a chief complaint of lower back pain and gait disturbance. Six years earlier, the symptoms of right lower limb pain, chest pain, lower back pain, fatigue, weakness of the trunk and muscle weakness had gradually appeared. His previous physician suspected a muscle disease such as amyotrophic lateral sclerosis, but no definite diagnosis was made. At the time of his first visit to our hospital, there was no obvious neurological deficit. Primary screening with X-ray radiography and bone scintigraphy revealed multiple fractures of the thoracolumbar vertebrae, pelvis and ribs (Fig. 1). Blood tests showed elevated alkaline phosphatase (IFCC: 385 U/L) and its fraction was predominantly bone type (58%). Serum phosphorus and 25OH vitamin D showed decreased levels (1.5 mg/dL and 15.8 ng/mL, respectively), whereas FGF23 was abnormally high (454 pg/mL; with the normal range being <30 pg/mL). Serum calcium and intact-parathyroid hormone were within normal limits and percent tubular reabsorption of phosphate (%TRP) was abnormally low at 55.8%. Based on the above, a diagnosis of FGF23-related hypophosphatemic osteomalacia was made.
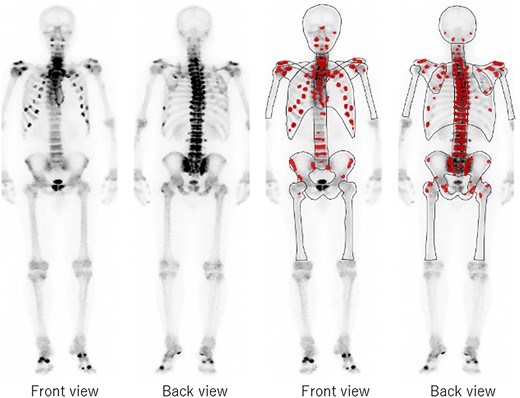
Bone scintigraphy shows numerous accumulations in the thoracolumbar spine, pelvis and ribs.
Bone mineral density (g/cm3) of the lumbar spine, right femoral neck and left femoral neck was 1.017, 0.952 and 0.750, respectively, with T-score of −0.2, −0.1 and − 0.9 and young adult mean of 97, 99 and 87, respectively. Somatostatin receptor scintigraphy showed an accumulation in the right femoral head (Fig. 2A and B), and magnetic resonance imaging showed a well-defined 14 × 16 × 17 mm borderline mass on the proximal lateral side of the right femoral head with low signal on T1-weighted images and high STIR signal on diffusion restriction (Fig. 2C–E). Venous sampling was then performed, revealing an elevated FGF23 concentration in the right medial femoral circumflex vein. Based on the above, a diagnosis of TIO in the right femoral head was made as the underlying cause of FGF23-related hypophosphatemic osteomalacia.
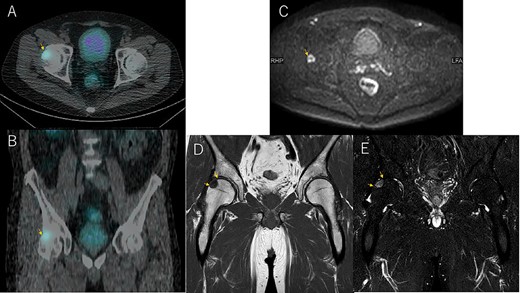
Somatostatin receptor scintigraphy shows a pale accumulation at 24 h (A and B). MRI diffusion-weighted images show a high-signal change in axial (C) consistent with the accumulation site (A). T1-weighted images (D) and STIR (E) in coronal.
The patient visited our orthopedic surgery department for tumor resection, and cemented hemiarthroplasty (C-stem AMT and SELF-CENTERING Bipolar; Depuy Synthes, Warsaw, IN) was performed (Fig. 3A and B). The tumor could not be identified grossly from the articular surface and the femoral head was sliced and cross-sectioned. The boundaries of the tumor were not clear to the naked eye, and the boundaries could only be inferred in conjunction with the imaging findings (Fig. 4A). The size was approximately 18 × 13 mm. Pathologically, the tumor cells were spindle-shaped, with no nuclear atypia, and showed cotton mass-like calcification (Fig. 4B). Immunohistochemically, tumor cells were positive for CD56, ERG and SATB2. The diagnosis was spindle to round cell tumor, most likely a phosphaturic mesenchymal tumor (PMT). One month after tumor removal, the serum phosphorus concentration and %TRP increased to 3.3 mg/dL and 89.3%, respectively, when compared with the preoperative level, and the FGF23 concentration decreased to 25.4 pg/mL, and was within the normal range. At 9 months postoperatively, the patient’s back pain and fatigue had improved and he was able to walk without a cane. There were no specific symptoms in the right hip joint, and X-ray radiography showed no changes. At that time, FGF23 was 28.0 pg/mL, which was within normal range.
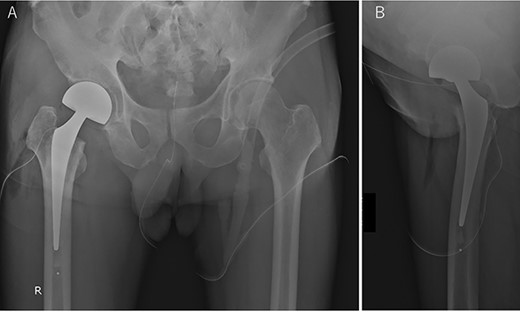
Postoperative anterior–posterior radiographic view of the both hip joints (A) and lateral view of the right hip joint (B).
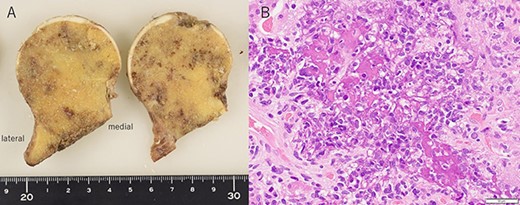
Cross section of the sliced femoral head (A) and histological findings of hematoxylin and eosin staining (B).
DISCUSSION
Surgical resection of the tumor is the standard treatment module for phosphate stromal tumors with TIO, with the aim of biochemical remission. A retrospective surveillance in Japan by Hidaka et al. showed that extensive resection had the highest biochemical remission rate (15/16, 93.8%), followed by marginal resection (15/23, 65.2%), and with curettage (11/19, 57.9%) being the least successful [3]. These results indicate that FGF23-producing cells in PMTs have a downward shift in the threshold for sensing phosphate via FGF receptor 1 and may therefore overproduce FGF23 to maintain low levels of serum phosphate even in small residual PMTs [4]. Furthermore, pathological examination has shown that PMTs are invasive, regardless of tumor size. Therefore, numerous studies state that a wide resection is the ideal choice for treatment, if possible, to avoid the possibility of residual tumor, local recurrence or distant metastasis [3, 5, 6].
However, as disease itself is very rare, there have been only a few reports describing detailed treatment options. In this case, because the lesion was located within the femoral head near the joint, surgical options other than hemiarthroplasty, which was performed in this case, which were considered were tumor resection and osteochondral transplantation and total hip arthroplasty. The former was abandoned due to concerns about recurrence and secondary osteoarthritis of the hip joint, after considering the tumor’s location in the loading zone, and the possibility of remnant scarring from the grabbing [7]. Due to the patient’s age and physical activity, the latter, in conjugation with total hip arthroplasty rather than with hemiarthroplasty, appeared to be a better option, especially regarding its long-term results. Considering the residual seeding of the tumor, we chose hemiarthroplasty, as we decided that a total hip arthroplasty with manipulation on the acetabular side would be risky. However, given that a report of total hip and knee replacements for TIO showed good results in all the cases, and if the concerns of seeding and invasiveness could be dispelled, it might have been considered as an option [8]. In the present case, the surgical outcome proved to be effective, and the patient remained in biochemical remission, albeit for a short period of time. Although this patient may experience cartilage failure on the acetabular side and migration of the bipolar head in the future, conversion to a hip prosthesis should be considered in this case. A polished cemented stem was chosen for its ease of removal, if such event was necessary.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
References
- magnetic resonance imaging
- hypophosphatemia
- alkaline phosphatase
- blood tests
- asthenia
- femoral head
- low back pain
- osteomalacia
- phlebotomy
- treatment failure
- diagnosis
- hip replacement arthroplasty
- leg
- neoplasms
- transplantation
- oncogenic osteomalacia
- hemiarthroplasty
- somatostatin receptor scintigraphy
- fibroblast growth factor 23



