-
PDF
- Split View
-
Views
-
Cite
Cite
Yuki Tamagawa, Masashi Kawamura, Masahiro Ryugo, Osamu Monta, Yasushi Tsutsumi, A rapid aneurysmal formation after late open conversion of endovascular abdominal aortic repair with complete endograft explant, Journal of Surgical Case Reports, Volume 2021, Issue 6, June 2021, rjab267, https://doi.org/10.1093/jscr/rjab267
Close - Share Icon Share
Abstract
Late open conversion (LOC) after endovascular aneurysm repair (EVAR) is associated with high morbidity and mortality. Standard surgical technique of LOC has not been established. This report presents a rapid aneurysmal formation in the unreplaced infrarenal aorta after LOC with complete endograft explantation without suprarenal fixations. A 76-year-old man presented with a left common iliac artery aneurysm (CIAA), for which he underwent EVAR to embolize the left internal iliac artery. Although his aneurysmal sac size initially showed a reduction, computed tomography at the 3-year interval post-EVAR demonstrated an increased sac size. Thus, he underwent open aortic repair of the CIAA. Though the postoperative course was uneventful, the size of the unreplaced infrarenal aorta showed a significant increase one year after open conversion. Reoperation was performed, but vascular prosthesis infection occurred as a complication and the patient died on the 196th postoperative day.
INTRODUCTION
Endovascular aneurysm repair (EVAR) has been widely accepted for the treatment of elderly patients with abdominal aortic aneurysms (AAA) or common iliac artery aneurysms (CIAAs). EVAR is associated with a lower operative mortality rate and a higher reintervention rate than open surgery for AAA [1]. The rate of graft-related complications with endovascular repair is 12.6%, and the rate of reintervention is 5.1% [1].
Late open conversion (LOC) in EVAR patients may be performed due to different causes. The rates of LOC procedures and overall mortality in LOC have been reported as 1.5–3.7% and 0–23.8% [2–6], respectively. LOC is still a technically demanding and challenging procedure, and its incidence has increased in the recent EVAR era. Herein, we report a unique case of rapid dilatation of the unreplaced infrarenal aorta after LOC with a complete endograft explantation.
CASE PRESENTATION
A 76-year-old man was incidentally diagnosed with a left CIAA by abdominal ultrasonography, with computed tomography (CT) demonstrating a left CIAA measuring 4.5 cm in diameter (Fig. 1A). The patient was referred to our hospital for surgical treatment. He had a medical history of liver cirrhosis and traumatic abdominal injury. Thus, he underwent EVAR using a GORE EXCLUDER AAA Endoprosthesis to embolize the left internal iliac artery. The postoperative course was uneventful, and postoperative CT showed no endoleak (Fig. 1B). Follow-up CT scans at 6-month, 1-year and 2-year intervals post-EVAR revealed a reduction in the size of the aneurysmal sac. However, the 3-year interval CT demonstrated an increase in the sac size (Fig. 2A). Contrast-enhanced CT and angiography revealed no endoleak but showed a dilatation of the CIAA. Therefore, the patient underwent open aortic repair of the CIAA.
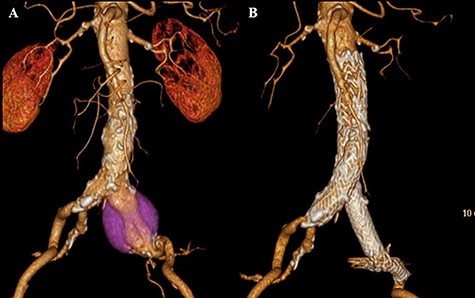
CT scan showing left CIAA (A). Contrast-enhanced CT demonstrating no endoleak after EVAR using a GORE EXCLUDER AAA Endoprosthesis to embolize the left internal iliac artery (B).
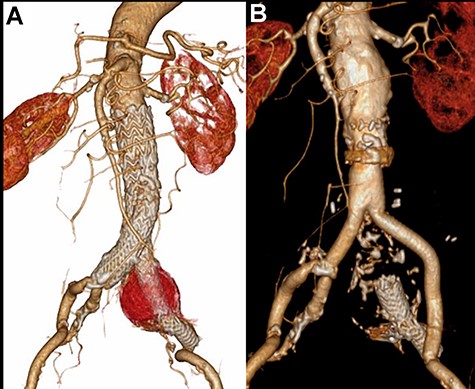
CT scan showing the increasing sac size of left CIAA with no endoleak (A) and aortic replacement with a Y-shaped vascular prosthesis performed with complete explantation of the endograft (B).
The infrarenal aorta up to the right common iliac artery and the left external iliac artery were exposed via a retroperitoneal approach. Proximal control was achieved by clamping midway between the renal arteries and the aortic bifurcation, and distal control was achieved by inserting an occlusion balloon into the right common iliac artery and clamping the left external iliac artery. The sac of the CIAA was opened, and many thrombi were noted around the stent graft. No backbleeding of the lumbar arteries or junctional bleeding of the stent was detected, and the entire endograft was removed easily. Abdominal aortic replacement with a Y-shaped vascular prosthesis (J Graft SHIELD NEO, bifurcated vascular prosthesis) was performed (Fig. 2B). Proximal and distal anastomoses were performed at the level of midway between the renal arteries and the aortic bifurcation where the endograft was fixed, and at the level of the right common and left external iliac arteries, respectively.
The patient recovered uneventfully, however, 1 year after open conversion, CT revealed a significant increase in the size of the unreplaced infrarenal aorta (Figs 3A, 4A and B). Reoperation was performed to treat the new aneurysm and on intraoperative findings, it was a true aneurysm. Abdominal aortic replacement was performed, however, infection of the vascular prosthesis occurred as a complication of this second open surgery. The infection was not controlled, and unfortunately, the patient died.
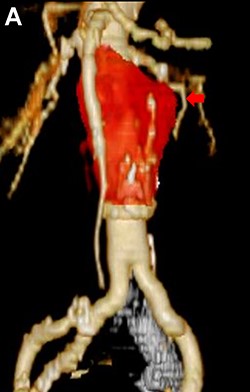
CT scan showing the significantly dilated infrarenal aorta, 1 year after open conversion (A, red arrow).
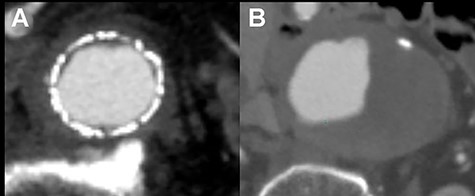
One year after open conversion, CT scan showing the significantly dilated infrarenal aorta (A) compared with the aorta before open repair (B).
DISCUSSION
LOC is associated with high mortality. Surgical techniques of LOC vary with regards to the site of proximal control and the site of endograft explantation, and no gold standard procedure has been established. LOC can be performed with either a complete or partial endograft explantation. A complete endograft explantation is often technically demanding. Suprarenal clamping is usually required and grafts with suprarenal fixation require supraceliac clamping to avoid damage to the native aorta. Suprarenal or supraceliac cross-clamping may be associated with a higher rate of mesenteric ischemia, acute renal failure and increased operative mortality [7].
In this case, the patient’s left CIAA re-expanded, and while the infrarenal abdominal aorta retained its normal size. The proximal clamp site was easily exposed, unlike the distal clamp site, which contained severe adhesions making its exposure difficult. Balloon occlusions were used to achieve hemostasis after the aneurysm was incised, a technique that could be useful for LOC.
It has been previously reported that periaortic inflammation has been observed with endograft fixation in well-incorporated endografts [6, 8], and that periaortic inflammation and suprarenal barbs may increase the risk of aortic wall injury [9]. In this reported case, the patient underwent EVAR using endograft without suprarenal barbs, and complete graft removal was easily accomplished. No difficulties such as the presence of severe adhesions between the aorta and the endograft, were encountered while removing the graft. However, the unreplaced infrarenal aorta enlarged significantly within a short period of time.
Intimal injury when the endograft was explanted and periaortic inflammation between the aorta and the endograft might have been responsible for the new true aneurysmal formation. Direct damaging from the radial force of the stents to the aortic wall and the proximal anastomosis site might have contributed to its formation as well. Partial preservation of the endograft may be a favorable potential option to reduce the risk of future aneurysm or pseudoaneurysm development.
CONCLUSION
This case presented a rapid dilatation of the unreplaced infrarenal aorta on which the endograft was fixed, a year after LOC with complete endograft explantation. Complete endograft explantation might increase the risk of future aneurysm development even in the absence of suprarenal barbs.
CONFLICT OF INTEREST STATEMENT
None declared.
ETHICAL APPROVAL
The patient consented to the publication of this report.



