-
PDF
- Split View
-
Views
-
Cite
Cite
Krystal Dinh, Lucy Manuel, Alison McGill, Thomas Daly, Fenestration of the common iliac vein: an unusual cause of deep venous thrombus, Journal of Surgical Case Reports, Volume 2021, Issue 4, April 2021, rjab045, https://doi.org/10.1093/jscr/rjab045
Close - Share Icon Share
Abstract
Iliac venous anomalies are reported in 20.9% of patients; however, fenestration or bifurcation of the common iliac vein only accounts for ~0.4% of patients [ 1]. Herein, we present and discuss the rare case of an iliofemoral deep vein thrombosis precipitated by a fenestrated left common iliac vein.
CLINICAL SUMMARY
A 56-year-old man presented to the emergency department with acute left leg swelling, discolouration and pain. He had undergone a cardiac ablation procedure for atrial arrhythmia via a bilateral femoral vein approach ~2 weeks prior. His other significant medical comorbidities included hypertension, diabetes, renal calculi, supraventricular tachycardia (SVT), hypercholesterolaemia, obesity, suspected obstructive sleep apnoea and depression. He worked as a hospital cleaner. On examination, his left leg was grossly swollen from the hip down, with tense compartments. His leg illustrated a purple discolouration (Fig. 1), and his foot was cool to touch with a capillary refill of ~2–3 seconds. His femoral pulse and posterior tibial pulses were palpable. Motor function and sensation in the lower limb were both preserved.
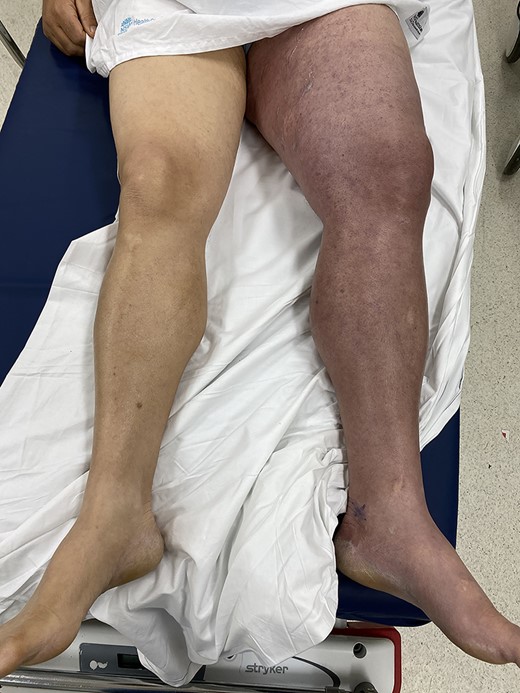
Patient presents with a grossly swollen and discoloured left leg.
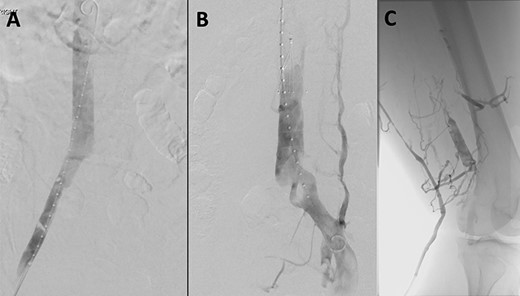
(A) Venogram illustrating patent IVC and renal vein position. (B) Post-thrombectomy venogram showing fenestrated left common iliac vein. (C) Venogram illustrating patent popliteal vein via small saphenous vein access.
On computed tomography venography he was found to have an extensive deep vein thrombosis (DVT) involving both the left external iliac and common iliac vein. He was commenced on a heparin infusion and proceeded to catheter-directed thrombolysis urgently that day. Notably, no DVT was seen in his right common iliac or external iliac vein.
After ultrasound-guided right common femoral vein access, venogram illustrated both the position of the renal veins and a patent inferior vena cava (IVC) (Fig. 2A). An infrarenal IVC filter was deployed (Celect Platinum Vena Cava Filter by COOK Medical) (Fig. 2B). A diagnostic venogram was performed via the left short saphenous vein (Fig. 2C), and this confirmed patency of the common femoral vein, femoral vein and the popliteal vein. Ultrasound was again utilized to puncture the left great saphenous vein proximally, with insertion of a 6-Fr sheath with a glide and Bern catheter used to cross the occluded common iliac vein and external iliac vein. An Angiojet thrombectomy catheter (by Boston Scientific) was placed within the thrombus, and a total of 19.4 mg of alteplase was infiltrated. After waiting 30 minutes for the alteplase to diffuse, a venogram was performed that demonstrated some resolution of the thrombus. Suction thrombectomy was then performed. Completion venogram illustrated a fenestrated left common iliac vein with resolution of the DVT (Fig. 2B). A balloon was inflated at the level of the fenestration to confirm separate channels. The irritation of the access vein’s intima for the SVT ablation in conjunction with the fenestrated common iliac vein was the suspected cause of the patient’s DVT. The patient was changed to therapeutic low-molecular-weight heparin post-operatively.
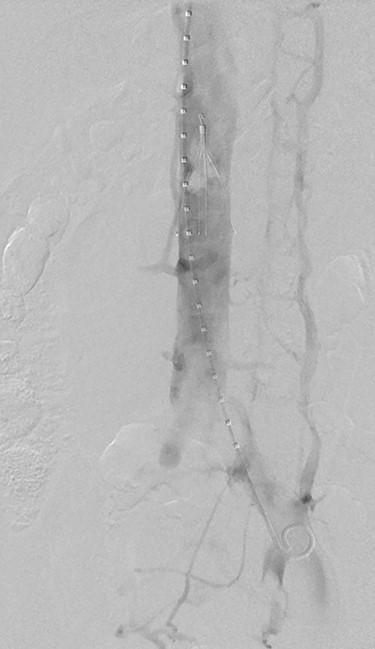
Two days after thrombectomy, a venogram of the IVC was performed to assess suitability for removal of the IVC filter. This was performed by placement of a pigtail catheter via right internal jugular vein access. This venogram illustrated fresh thrombus in IVC filter (Fig. 3), and thus, a decision was made to leave the filter in situ, remain on anticoagulation and revisit in 6 weeks to assess removal. The patient was changed to warfarin upon discharge. A venogram of the IVC was performed 6 weeks after discharge; the thrombus within the IVC filter had resolved, and the filter was successfully removed.
DISCUSSION
There are eight described variations in iliac vein anatomy [1, 2]. Type 8, which is classified by common iliac vein fenestration, is both a rare vascular anomaly and rarely reported in the literature. The significance of a fenestrated common iliac vein is unknown; however, as demonstrated in this case, it possibly may precipitate the development of a DVT. The small calibre of the veins associated with a fenestrated vein, in addition to intimal irritation of the recent procedure may be the reason the patient developed a DVT on his left side and not his right. It is important to be aware of the different type of anomalies associated with the common iliac vein and their potential risk for developing pathology.
CONFLICT OF INTEREST STATEMENT
None declared.



