-
PDF
- Split View
-
Views
-
Cite
Cite
Ana Cristina Silva, Pedro Soares Moreira, Vitor Costa Simões, Mónica Sampaio, Marisa Domingues Santos, Intussusception in a pregnant woman, Journal of Surgical Case Reports, Volume 2020, Issue 12, December 2020, rjaa554, https://doi.org/10.1093/jscr/rjaa554
Close - Share Icon Share
Abstract
Abdominal pain in a pregnant woman with a history of laparoscopic Roux-en-Y gastric bypass (LRYGB) in the emergency department is challenging. Intussusception is a rare cause of small bowel obstruction after LRYGB and can lead to intestinal necrosis, perforation, sepsis and death. The authors report a case of a 34-week pregnant patient, previously submitted to LRYGB, presenting to the emergency department with abdominal pain and vomiting. A computed tomography scan suggested the presence of ileoileal intussusception. So, an emergent laparotomy was performed with invagination reduction. The postoperative period was uneventful, as well as pregnancy and caesarian performed 4 weeks after surgery. At the 45-month follow-up, there was no recurrence of intussusception.
INTRODUCTION
Laparoscopic Roux-en-Y Gastric Bypass (LRYGB) is the second most common bariatric surgical procedure (38.2%) performed worldwide [1]. Over 80% of the patients submitted to this are female, and about 3/4 are between 18 and 49 years of age [2] meaning they are potentially fertile. On the other hand, weight loss is associated with the regularization of ovulatory function and improved fertility. Although intussusception is an infrequent cause of obstruction in adults, it is a well-established late complication of Roux-en-Y Gastric Bypass (RYGB), occurring typically after significant weight loss [3]. Published cases of intussusception during pregnancy are sporadic.
As a rare occurrence of intussusception in pregnancy, the difficulty of diagnosis (both for nonspecific symptoms and the risks of using imaging tests that imply an adequate risk/benefit assessment) and the delay in treatment can have severe but preventable consequences as long as there is clinical suspicion. That is why the authors report this case, probably being the first written in Portugal.
CASE REPORT
A 38-year-old, 34 weeks pregnant patient (G3 P1 T1 Ab1 LC1) with a history of antecolic retrogastric LRYGB 6 years before and with successful weight loss came to our institution with severe abdominal pain and vomited. The pain was epigastric, non-radiating, sharp and intermittent. It was also associated with incoercible vomiting, with 12 h of evolution.
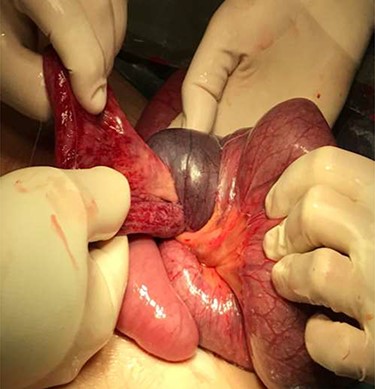
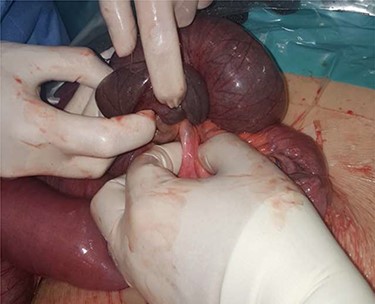
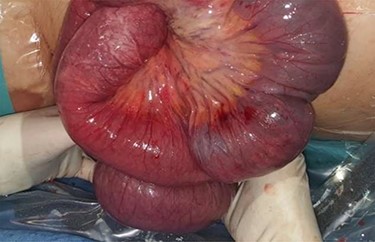
Physical examination presented normal vital signs. The abdomen was tender but lacked signs of peritonitis. Blood analysis revealed leukocytosis, neutrophilia and elevated lactate dehydrogenase. Obstetric ultrasonography (US) showed: fetus at cephalic presentation with good vitality, regular amniotic fluid volume, placenta without detachment. An abdominal computed tomography (CT) scan revealed proximal jejunal dilation caused by an ileoileal invagination and collapsed distal ileum (Figs 1 and 2). Betamethasone and atosiban were administered, and a supraumbilical laparotomy was performed. The intussusception in the common limb (80 cm distal to jejunojejunostomy) (Fig. 3) was reduced (Figs 4 and 5) with progressive and complete intestinal vascular perfusion (Fig. 6). The postoperative period was uneventful, and a caesarian was performed 4 weeks later. At the 45-month follow-up, there was no recurrence.
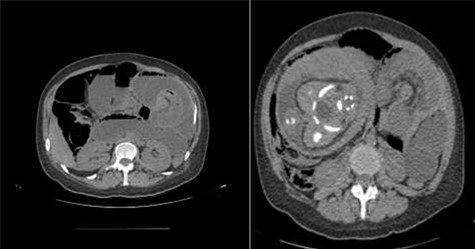
Axial view of the CT scan showing jejunojejunal intussusception with fat and blood vessels within the lumen of intestine (white arrow—typical “target sign”).
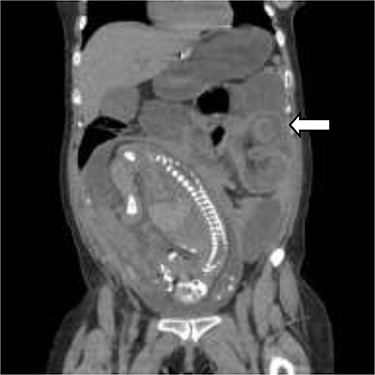
Coronal view of the CT scan showing intussusception (white arrow—sausage-shaped thickened bowel Wall).
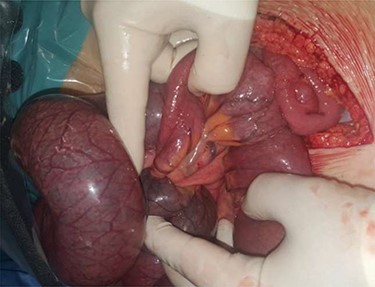
Retrograde intussusception of the common limb into the jejunojejunostomy.
DISCUSSION
An organic lesion cause 90% of all intussusceptions in adults, such as benign or malignant neoplasms, postoperative adhesions, inflammatory bowel disease and congenital abnormalities as Meckel’s diverticulum or even iatrogenically lesions [4].
Agha first described intussusception following a Roux-en-Y gastrojejunostomy in 1986 [4] with a prevalence estimated at 0.07–0.6% [3]. Intussusceptions account for about 5% of all intestinal obstructions during pregnancy [5]. The incidence of intussusception after LRYGB during pregnancy is not well known. The first case of intussusception complicating pregnancy following LRYGB was reported in 2007 by Wax et al. [6]. As far as we have known, only 23 cases have been described in the literature [6].
The etiopathogenesis of intussusception after RYGB remains under discussion. Several hypotheses have been postulated, but the most accepted is that the proximal jejunum division allows the emergence of ectopic pacemakers or migratory motor complexes in the Roux limb to produce conflicting peristaltic waves that would ultimately cause the invagination [7]. In RYGB-associated intussusceptions, the common limb is the most common intussusception site, and most are retrograde [7]. Pregnancy predisposes to obstruction after RYGB remains a matter of debate, particularly regarding intussusception. A review of the literature regarding intussusception after RYGB in pregnant women reported that most is retrograde and in the jejunojejunostomy [6].
The presence of symptoms is variable, nonspecific and the presentation form can be acute, recurrent or chronic. Abdominal pain and nausea/vomiting are the main complaints [7]. Intestinal obstruction may be complete or incomplete with scarce or none of the classic obstruction signs. However, the hyperemesis gravidarium is a frequent and confounding factor that can delay timely diagnosis [8].
Physical examination is also often nonspecific and not helpful. The abdomen is usually tender but lacking signs of peritonitis. A palpable mass is found in ~10% [7].
The analytical study may indicate an inflammatory syndrome in up to half the cases, causing misdiagnosis [1]. When presented, abdominal pain with increase pancreatic enzymes of blood can lead to an incorrect diagnosis of acute pancreatitis [9].
Plain abdominal radiographs may reveal intestinal obstruction or perforation signs but will rarely enlighten the cause, and US is technically demanding and user dependent [10]. CT is commonly the study of choice with a reported sensitivity of 66–78% [10]. It can reveal dilated bowel loops, air-fluid levels, and the typical ‘target sign’ (present in 80%) [7]. Magnetic resonance imaging can be an option if available, especially in the first trimester of pregnancy [10]. However, it is often unavailable in the acute setting. In the second and third trimester, CT entails little risk to the fetus while providing a clear benefit from a fast and accurate diagnosis [10]. The timely diagnosis can prevent intestinal necrosis and peritonitis, with a previously reported maternal mortality of 6% and fetal mortality of 26% [2].
Surgery may be the only way to establish the diagnosis. If there is a high index of suspicion a CT scan can be forgone since a negative result should not prevent surgical exploration in that setting.
Diagnostic laparoscopy is feasible when the pneumoperitoneum can be created [2].
Even though intussusception may resolve spontaneously, conservative management is not recommended because it is difficult to assure the absence of necrosis [7]. The surgical options are intussusception reduction, reduction with plication, intestinal resection and resection with revision of the anastomosis [3]. In most patients simple reduction is possible [3] but with higher recurrence rates than those with intestinal resection (33.3% versus 7.7%, P = 0.02) [7], suggesting that resection is preferable [7, 10].
Nevertheless, the management of intussusceptions during pregnancy demands further considerations. On the one hand, recurrence increases with reduction alone. On the other hand, performing a resection with anastomosis adds significant length to the operation and greatly enhances complications. The literature review on intussusception after RYGB in pregnant women revealed resection was performed only if necrosis/perforation present.
In our clinical case, early diagnosis prevented an intestinal resection reduced the likelihood of postoperative complications, and made it possible to deliver at term, without morbidity for mother or fetus.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.



