-
PDF
- Split View
-
Views
-
Cite
Cite
Noriaki Koizumi, Hiroki Kobayashi, Kanehisa Fukumoto, Massive chronic irreducible rectal prolapse successfully treated with Altemeier’s procedure, Journal of Surgical Case Reports, Volume 2018, Issue 4, April 2018, rjy064, https://doi.org/10.1093/jscr/rjy064
Close - Share Icon Share
Abstract
The guideline for the treatment of rectal prolapse recommends that surgeons select appropriate surgical procedures individually based on each patient’s overall status. However, in cases of irreducible or incarcerated rectal prolapse, surgical options are quite limited. Here we present a case of an elderly woman with massive chronic irreducible rectal prolapse. An 87-year-old woman presented to our hospital with a complaint of massive rectal prolapse. The prolapsed rectum was over 20 cm long, and completely irreducible. She underwent perineal rectosigmoidectomy with levatorplasty known as Altemeier’s procedure. More than 30 cm of rectosigmoid colon was resected. After the operation, rectal prolapse was resolved completely. Her postoperative course was uneventful, and her quality of life and bowel movements improved. She has since been healthy without recurrence for over 2 years. Altemeier’s procedure is applicable even in cases of irreducible rectal prolapse and features acceptable safety and a satisfactory outcome.
INTRODUCTION
Rectal prolapse is defined as a full-thickness protrusion of the rectal wall through the anal canal. It commonly occurs in aged women and is suspected to be triggered by loosening of the pelvic floor muscles associated with aging, childbirth and straining during defecation. Since rectal prolapse may cause anal discomfort or disturbance of defecation, it can seriously impair patients’ quality of life (QOL).
While only surgical treatment enables radical cure of rectal prolapse, a wide spectrum of operative procedures are now available. Of them, an appropriate operative procedure should be selected for each patient according to disease severity and patient performance status [1]. However, surgical procedures to treat irreducible or incarcerated rectal prolapse are limited [2].
Here we present a case of an elderly woman with massive chronic irreducible rectal prolapse that was successfully treated with perineal rectosigmoidectomy and levatorplasty known as Altemeier’s procedure. Altemeier’s procedure is a well-established surgical procedure and seemed to be a less invasive approach that can be used to treat even irreducible cases.
CASE REPORT
An 87-year-old woman presented to our hospital with a complaint of spontaneous massive rectal prolapse. She had been suffering from persistent rectal prolapse for over 5 years, and the length of the prolapsed rectum continued increasing. At the time of presentation, the prolapsed rectum was over 20 cm long and severely edematous (Fig. 1); therefore, it was completely irreducible. She had no apparent past medical history, and no other remarkable finding was present on physical examination. Her QOL was severely impaired since she was unable to even sit normally. Pelvic computed tomography showed full-thickness prolapse of the redundant rectosigmoid colon from the anus (Fig. 2); thus, she was diagnosed with Tuttle II type complete rectal prolapse.
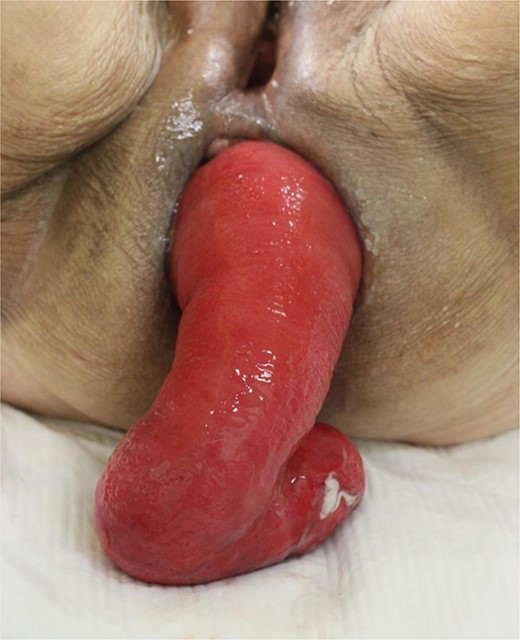
Preoperative findings. A massive rectal prolapse is observed. The prolapsed rectum shows edematous changes.
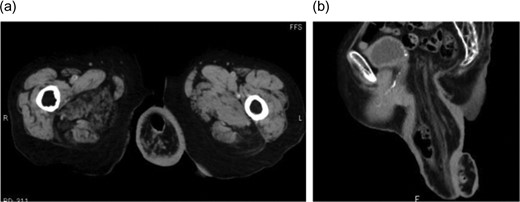
Pelvic computed tomography image. Full-thickness prolapse of redundant rectosigmoid colon from the anus is observed. (a) Axial section and (b) sagittal section.
Since it seemed that resection of the redundant rectosigmoid colon would provide a complete cure, she underwent Altemeier’s procedure. Under spinal anesthesia, the patient was placed in the lithotomy position. The ventral side of the prolapsed rectum was incised across its full-thickness at 1 cm proximal to the dentate line, and Douglas’s pouch was opened. The dorsal side of the prolapsed rectum was also incised at the same distance from the dentate line. After circumferential incision, the redundant rectosigmoid colon was pulled out through the anus. The vessels of the mesosigmoid colon were carefully ligated and cut, and the redundant rectosigmoid colon was resected. A subsequent levatorplasty was performed by suturing of bilateral puborectalis muscles to each other. A coloanal anastomosis was performed using a hand-sewn maneuver with circumferential 3-0 absorbable sutures.
The operation was completed in 63 min with little intraoperative blood loss. More than 30 cm of rectosigmoid colon was resected (Fig. 3). The patient’s postoperative course was uneventful and the rectal prolapse was completely resolved (Fig. 4). She became to be able to sit in a normal way, and her bowel movements also improved. She was discharged 13 days after the operation with satisfactory QOL, and has since been healthy without prolapse recurrence for over 2 years.
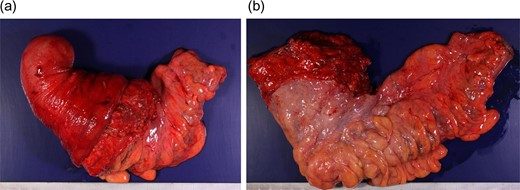
Resected specimen. The resected rectosigmoid colon was >30 cm long. (a) Before reduction and (b) after reduction.
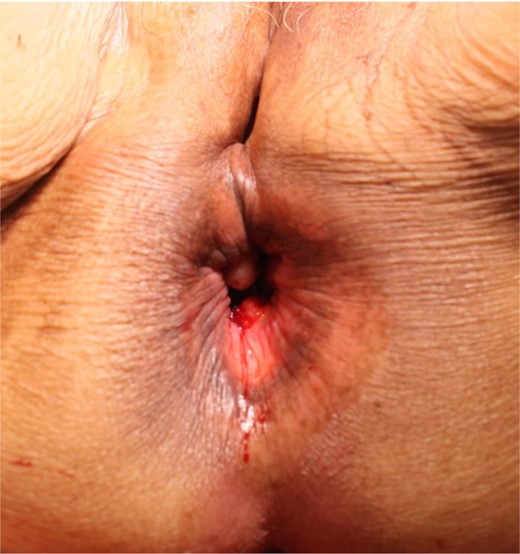
Postoperative findings. The rectal prolapse is completely resolved.
DISCUSSION
It is known that there are more than 100 operative procedures for the treatment of rectal prolapse, and these are categorized into abdominal and perineal approaches [3]. Of them, ~10 procedures are currently performed in daily clinical practice. Delorme’s and Altemeier’s procedures are now considered representative perineal approaches, while laparoscopic rectopexy is considered the representative abdominal approach. Naturally, each procedure has its advantages and disadvantages.
Regarding laparoscopic rectopexy, a number of reports have demonstrated its lower invasiveness and satisfactory operative results [4, 5]. On the other hand, however, several reports have described that neither laparoscopic rectopexy nor Delorme’s procedure demonstrate definite superiority in clinical and functional outcomes [3, 6]. Furthermore, especially in elderly patients, no statistical differences in complication and recurrence rates were reported between laparoscopic rectopexy and Altemeier’s procedure [7]. These results suggest that there might not be a need to adopt laparoscopic rectopexy for elderly patients. Therefore, the operative procedure for rectal prolapse should be individualized according to each patient’s background and degree of rectal prolapse.
The treatment guideline published by the American Society of Colon and Rectal Surgeons recommends that surgeons select appropriate procedures individually based on each patient’s overall status [8]. The guideline states that laparoscopic rectopexy is recommended for patients with good performance status, while the perineal approach is more appropriate for patients with poor performance status or high operative risk. The guideline also mentions that Delorme’s procedure is preferable in cases of relatively shorter rectal prolapse, while Altemeier’s procedure is preferable for cases of relatively longer rectal prolapse. Thus, we performed Altemeier’s procedure in the current case.
The results of a randomized controlled study of 293 patients with rectal prolapse were recently published [9]. In that trial, patients were randomized into the perineal or abdominal approach groups. Patients in the perineal approach group were further randomized into Altemeier’s procedure or Delorme’s procedure groups. The recurrence rates were similar for Altemeier’s procedure and Delorme’s procedure (24 vs. 31%, P = 0.4). Overall, recurrence rates did not differ significantly between the perineal and abdominal approaches (20 vs. 26%, P = 0.8). Furthermore, incontinence, bowel function and QOL were similar between groups. These results suggest that individualization is quite important in the surgical management of rectal prolapse.
Meanwhile, in cases of irreducible or incarcerated rectal prolapse, surgical options were quite limited. Since the abdominal approach is difficult to adopt, we had no choice but to select the perineal approach in this case. Delorme’s procedure was not suitable for the present case of a long rectal prolapse; therefore, we performed Altemeier’s procedure. Although Altemeier’s procedure requires coloanal anastomosis, the incidence of severe complications including anastomotic leakage is considered acceptable [10]. Furthermore, in Altemeier’s procedure, subsequent levatorplasty enables pelvic floor muscle repair, which is considered a more radical treatment. Although it seems that further discussion about adequate resection length and optimal lavatorplasty is needed, Altemeier’s procedure is applicable even in cases of irreducible rectal prolapse and features acceptable safety and a satisfactory surgical outcome.
CONFLICT OF INTEREST STATEMENT
None declared.



