-
PDF
- Split View
-
Views
-
Cite
Cite
Mauricio Palacios, Alex Guachilema R, Sandra Morocho, Andrea Lisintuña, Julio Yepez, Mariela Andrade, Emergent conversion from single-anastomosis gastric bypass to Roux-en-Y gastric bypass with subsequent obstruction of entero-enteric anastomosis by ascaris, Journal of Surgical Case Reports, Volume 2023, Issue 8, August 2023, rjad428, https://doi.org/10.1093/jscr/rjad428
Close - Share Icon Share
Abstract
One anastomosis gastric bypass (OAGB), the third most commonly performed procedure worldwide, has shown excellent results in terms of weight loss and resolution of comorbidities compared with other bariatric surgeries. However, its use remains limited in various parts of the world due to postoperative complications. After the efficacy of this procedure was established, the focus of treatment shifted toward resolving postoperative complications. Protein-energy malnutrition after OAGB is one of the main issues that needs to be addressed. There are several operative options for patients who require revision surgery including reversal and conversion to Roux-en-Y gastric bypass (RYGB). The conversion from OAGB to RYGB is a feasible method that has shown excellent results when performed by experts in the field. Here, we present the case of a woman with symptoms of acute obstruction secondary to OAGB who underwent conversion to RYGB under emergent conditions.
INTRODUCTION
Obesity and its associated comorbidities have become one of the most significant challenges related to health and they decrease the quality of life of those affected. Bariatric surgery is an effective long-term treatment for obesity and its associated comorbidities, and several restrictive and malabsorptive surgical procedures have been developed for the treatment of this condition. Generally, highly complex procedures lead to greater weight loss and better resolution of comorbidities [1].
Mini gastric bypass or one anastomosis gastric bypass (OAGB) is a simple and effective procedure based on gastrojejunal anastomosis that combines the advantages of other bariatric procedures. There are few reports in the literature describing its complications compared with those of Roux-en-Y gastric bypass (RYGB). The revision rate after OAGB is ⁓2.3–4.7%, and malnutrition and ulcers are the most common indications. Bariatric procedures are associated with various complications, which are infrequent when performed by experienced surgeons; however, these complications can be severe in the presence of inexperienced surgeons, resulting in an increase in the mortality rate [1, 2].
CASE PRESENTATION
A 29-year-old woman originally from Ecuador’s Amazon region who presented with a history of grade II obesity (body mass index of 37) had undergone bariatric surgery (OAGB) 30 days before admission to our hospital. The patient showed intolerance to a liquid diet and symptoms of reflux starting at the immediate postoperative period, in addition to repeated bilious vomiting after progression to a semisolid diet. Physical examination showed normal vital signs, the abdomen was tender without signs of peritoneal irritation. The protein profile showed alterations with evidence of malnutrition. Abdominal Computed Tomography showed evidence of efferent intestinal loop bending with decreased passage of enteric contrast (Fig. 1A and B). An endoscopy showed stenosis of the gastroenteric anastomosis and obstruction of the efferent loop (Fig. 2).
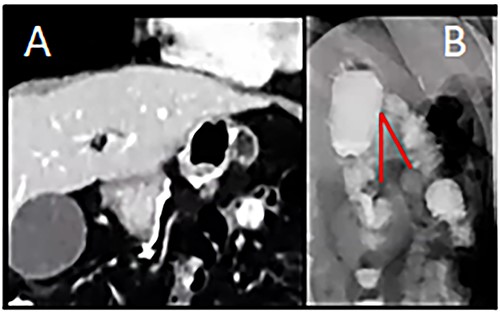
(A) Computed Tomography: Afferent loop bending and gastroenteric anastomotic stenosis. (B) Radiograph showing distal efferent obstruction.
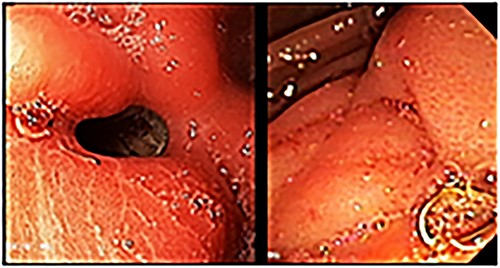
Upper gastrointestinal endoscopy showing gastroenteric anastomotic stenosis.
The patient was referred for laparoscopic revision surgery with conversion to RYGB (Fig. 3). In the postoperative period, a torpid evolution included vomiting on various occasions, as well as the detection of ascaris on one occasion. A new upper GI endoscopy showed evidence of permeable gastrojejunal anastomosis and acute inflammatory changes (Fig. 4), and the patient received antiparasitic treatment. Because of persistent symptoms of obstruction, a new surgical intervention was performed, which showed the presence of ascaris in the entero-enteric anastomosis causing its obstruction (Fig. 5). A new anastomosis was performed at a distance of 30 cm from the obstruction (Fig. 6). After the patient showed improvement and tolerated a liquid diet, she received treatment for ascaris and was discharged with good evolution.
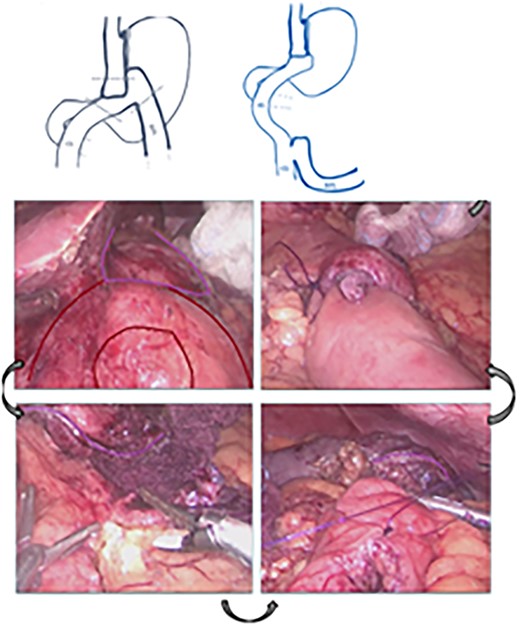
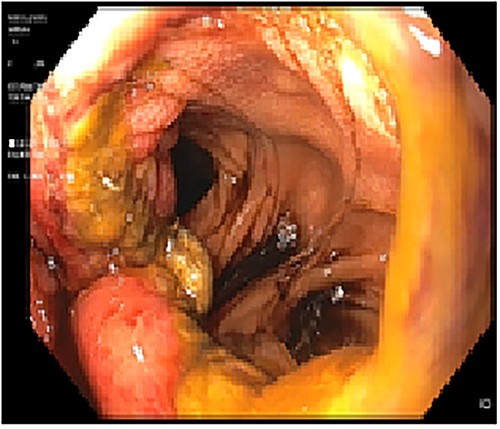
Acute inflammatory changes associated with gastrojejunal anastomosis.
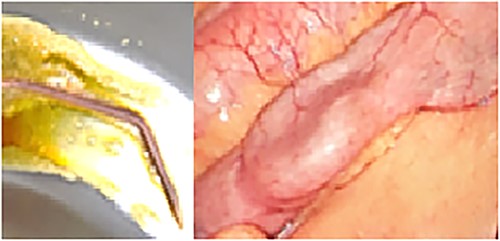
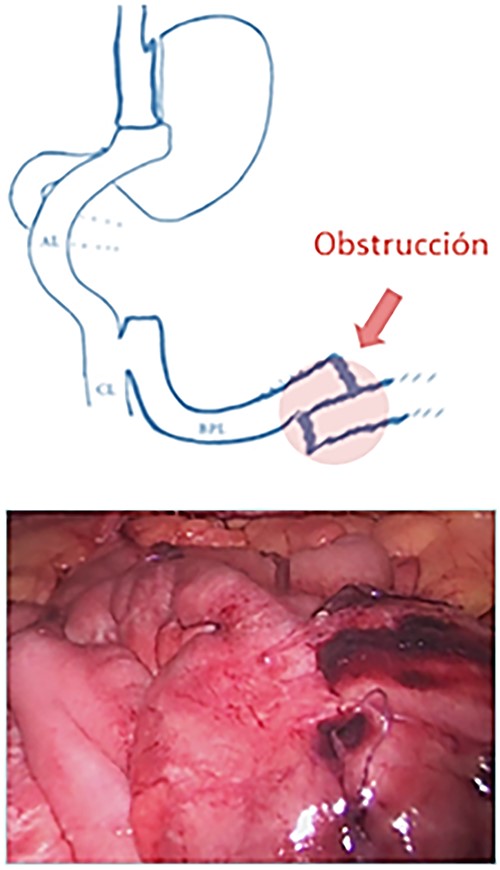
Diagram showing the construction of a new entero-enteric anastomosis.
DISCUSSION
Obesity has become a worldwide pandemic, as 39% of adults are overweight and 13% are obese [2]. The surgical treatment of obesity is the most effective approach for achieving long-term weight loss and for the resolution of comorbidities. According to the International Federation for the Surgery of Obesity and Metabolic Disorders, 634 897 primary procedures (92.6%) were performed in 2016, and OAGB was performed in 4.8% of cases [1].
Conversion surgery implies a complex situation because it applies to patients who failed a previous intervention for the control of obesity and its associated comorbidities [3]. Regardless of the underlying motive, the conversion from OAGB to RYGB is technically feasible and is not associated with significant complications [2, 4]. Among the early complications of OAGB, anastomotic stenosis accounts for ˂1% of cases [5] and can be managed conservatively; however, in cases of persistent symptoms, revision surgery is indicated.
Certain final details of the technique are essential to ensure the success of these procedures [1]. In the present case, the patient showed oral intolerance and evidence of malnutrition, which led us to consider revision surgery. Conversion to RYGB was performed in an emergency context in a safe and effective manner. In the postoperative period, we found obstruction of the entero-enteric anastomosis caused by a parasite, which was removed and the anastomosis was repaired, showing adequate postoperative evolution.
The laparoscopic revision of the anastomosis, the correction of any obstruction or bending, and the conversion to RYGB are treatment options for patients presenting with complications. Anastomotic stenosis after OAGB or RYGB can be treated endoscopically, whereas entero-enteric obstruction cannot be treated by endoscopy [6].
In an emergency scenario, such as that of the present patient, revision and conversion were the correct treatments. However, as a special consideration, patients who are referred from an Eastern Amazonian region that is endemic for parasites should receive antiparasitic treatment prior to bariatric surgery.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.



