-
PDF
- Split View
-
Views
-
Cite
Cite
Roberto Cunha, Manuel Silva, Alberto Henrique, Pedro Maximiano, Mafalda Correia, Isabel Vieira, Isabel Cássio, Nelson Oliveira, Emanuel Dias, Paradoxical embolism: a rare cause of acute upper limb ischemia, Journal of Surgical Case Reports, Volume 2023, Issue 7, July 2023, rjad435, https://doi.org/10.1093/jscr/rjad435
Close - Share Icon Share
Abstract
Paradoxical embolism is a rare cause of arterial embolism, even more those resulting in acute ischemia of the upper limb. A case of a 45-year-old patient with acute paradoxical upper limb embolization and acute limb ischemia is presented. A review of the most recent evidence on the diagnosis and management of paradoxical embolism were explored. The cardiac defect most associated with paradoxical embolism is a patent foramen oval. The diagnosis can be performed by transthoracic or transesophageal echocardiography. Closure of the foramen oval is a safe and effective procedure; however, there is no clear consensus on when it should be performed, so the strategy should be individualized. A high level of suspicion of paradoxical embolism should exist in the presence of simultaneous venous and arterial embolism. The investigation of the embolic source is fundamental to avoid the recurrence of events.
INTRODUCTION
Acute upper limb ischemia is a rare event, accounting for 1/5 of acute limb ischemia [1]. Paradoxical emboli are defined by the passage of venous embolic material into the arterial circulation through a cardiac shunt [2]. Paradoxical emboli represent <2% of all arterial emboli [1]. Patent foramen oval (PFO) is the most common intracardiac defect.
The authors present a case of a patient with acute upper limb ischemia in the context of paradoxical emboli due to PFO.
CASE REPORT
A 45-year-old female patient with a personal history of hypothyroidism, obesity, inferior parathyroidectomy for parathyroid adenoma and adnexectomy for benign ovarian cystadenoma presented with sudden onset dyspnoea as well as with pain, poikilothermia, pallor and weakness of left upper limb and hand. Physical examination showed peripheral O2 saturation of 80% and absence of radial and left brachial pulses. On Duplex ultrasound, deep or superficial vein thrombosis was not identified. On thoracic computed tomography angiography, bilateral pulmonary embolism (PE) and occlusion of the axillary artery were identified while aortic dissection was excluded (Fig.1). Given the concomitant upper limb ischemia and PE, the patient was hypocoagulated with low-molecular-weight heparin and underwent urgent thromboembolectomy and angiography, through a distal brachial surgical approach. Postoperatively, the patient recovered a radial and ulnar pulses. The embolic source was further investigated by transthoracic and transesophageal echocardiography, which identified a PFO (Fig.2). The patient was discharged on rivaroxaban for anticoagulation (20 mg once daily). During follow-up, thrombophilia screening was performed, including antiphospholipid antibody syndrome, factor V Leiden mutation, prothrombin gene mutation, antithrombin III defect, protein C and S deficiency assessments, but all results were negative. Considering the single event of right atrioventricular overload and flow-inversion through PFO associated with PE, PFO closure was not indicated.
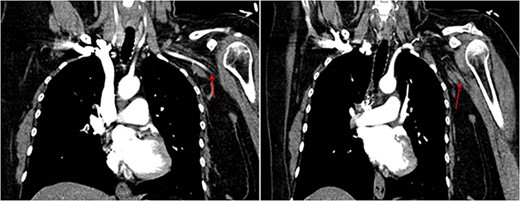
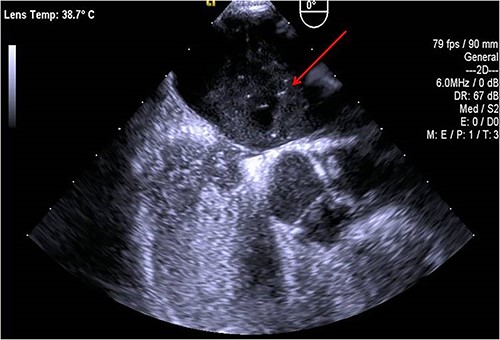
DISCUSSION
The cardiac defect most commonly associated with paradoxical embolism is PFO. However, a pulmonary arteriovenous malformation, atrial or ventricular septal defects, patent ductus arteriosus and Fallot Tetralogy may also be associated with paradoxical embolism. Depending on the territory in which embolization occurs, an ischemic stroke, an acute myocardial infarction, acute mesenteric ischemia, visceral or renal infarction or limb ischemia may occur [3].
Under physiological conditions, the pressure gradient between the left and right atria prevents any embolization through a PFO. However, in the case we herein report, the development of PE may have led to a transient increase of pressure in the heart chambers, producing right-to-left shunt, enabling paradoxical embolization to occur. Other situations that may allow this shunt are the Valsalva manoeuvre, tricuspid insufficiency or right ventricular insufficiency [3].
The diagnosis of cardiac defect can be performed by transthoracic or transesophageal echocardiography. Transthoracic echocardiography is a noninvasive and easily accessible examination but has a low sensitivity compared to the transesophageal technique for the diagnosis of PFO. In the case described, the diagnosis was made by transesophageal ultrasound, associated with a ‘bubble test’ (involves the delivery of saline mixed with air into a vein to assess the flow of blood through the heart) following an unconclusive transthoracic ultrasound.
There is no clear consensus regarding PFO treatment. Although PFO closure is a safe and effective procedure, its management should be individualized [1]. In the case described, given the absence of previous symptoms associated with PFO and absence of other embolic phenomena, PFO closure was not deemed indicated by our Cardiology department.
Regarding acute limb ischemia, the therapeutic options essentially consist of surgical embolectomy, thrombolysis or anticoagulation. Studies have shown greater complications with the anticoagulation and thrombolysis strategy than from surgical embolectomy [4]. In the case described, urgent embolectomy was performed associated with long-term anticoagulation with rivaroxaban.
To conclude, paradoxical embolism is a rare phenomenon that should be considered in the presence of venous thromboembolism simultaneously with arterial embolism, given it may affect the prognosis of patients. Thus, in addition to the treatment of the acute embolic event, a thorough investigation of the embolic source should be performed to avoid the recurrence of embolic events.
ACKNOWLEDGEMENTS
The authors acknowledge the Angiology and Vascular Surgery Department, Hospital do Divino Espírito Santo (HDES), Ponta Delgada, São Miguel Island, Azores, Portugal.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
DECLARATION OF PATIENT CONSENT
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understand that his name and initials will not be published, and due efforts will be made to conceal his identity.



