-
PDF
- Split View
-
Views
-
Cite
Cite
Yeabsera M Duguma, Tesfahun A Seid, Yonas G Shumiye, Tesfaye A Dinagde, Segni Kejela, Giant gastric GIST with fast-growing mass after intra-tumoral bleeding, Journal of Surgical Case Reports, Volume 2023, Issue 7, July 2023, rjad427, https://doi.org/10.1093/jscr/rjad427
Close - Share Icon Share
Abstract
Only a few instances of giant gastrointestinal stromal tumors and even fewer cases of such tumors with intra-tumoral bleeding have ever been reported. This report represents a case with both giant size and intra-tumoral spontaneous hemorrhage. Here a 42-year-old male patient presented with abdominal pain and abdominal distention of 5-month duration. The distention had fast growth over 1 month before the hospital presentation. Physical examination showed a conjunctival pallor and an ill-defined abdominal mass. A contrast-enhanced computed tomography (CT) scan showed a huge intra-abdominal mass with variable enhancements. Surgical exploration was done and a huge mass measuring 10.5 kg with dimensions of 32 × 30 × 15 cm was excised en-bloc with distal gastrectomy.
INTRODUCTION
Of all the abdominal tumors, gastrointestinal stromal tumors (GIST) remain the most common mesenchymal neoplasms [1]. The most common presentation of GIST is gastrointestinal bleeding [2]. GIST cases located on the stomach have the lowest rate of presentation with acute symptoms, whereas small bowel GISTs have the highest rate of surgical intervention on an emergency basis [2]. Thus far, only a minority of patients have been reported to present with a rupture of the tumor with intraperitoneal bleeding or signs and symptoms of peritonitis [3]. To date, only two case reports of acute anemia secondary to an intra-tumoral hemorrhage of GIST have ever been reported [4, 5]. This report presents the third case of a patient with rapidly progressing abdominal distention secondary to huge GIST with intra-tumoral hemorrhage.
CASE REPORT
We present a case of a 42-year-old male patient who presented with a complaint of abdominal pain of 5-month duration. The abdominal swelling had a fast increment over a period of 1 month before the hospital presentation. He had associated intermittent crampy abdominal pain, loss of appetite, early satiety and weight loss of 15% over the 5 months. He had no history of vomiting or tarry stool, and there is no family history of bleeding tendencies.
On physical examination, the patient was sick looking but had stable vital signs. Pertinent positive findings were pale conjunctivae, and a huge ill-defined abdominal mass occupying a major portion of the abdominal cavity that was firm to palpation and mildly tender. A routine blood test revealed the hemoglobin of 7.2 gm/dl and a negative fecal occult blood test. Contrast-enhanced CT of the abdomen showed a huge (30 × 26.5 × 15 cm) lobulated heterogeneous hyper-vascular mass lesion filling the whole abdominal cavity and extending down to the pelvis with internal poorly enhancing cystic components (Fig. 1). The tumor appeared to arise from the inferior wall of the gastric wall, and there was no evidence of lymphadenopathy or distant metastases. These findings were consistent with GIST arising from the stomach.
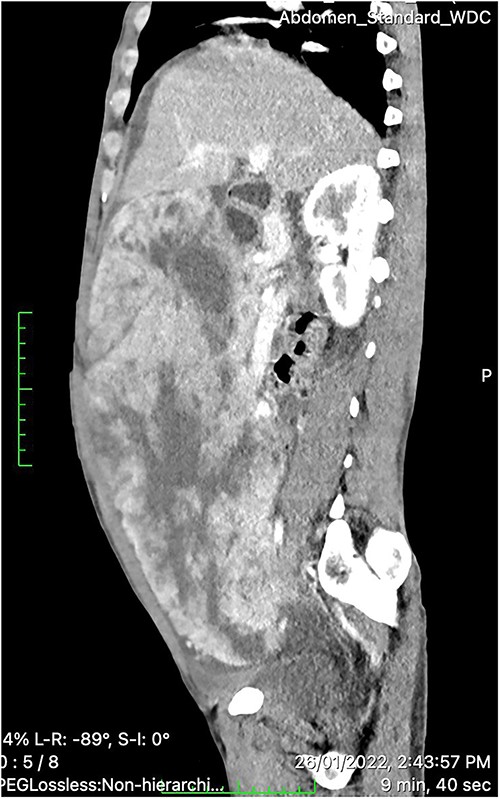
Contrast-enhanced CT scan showing a huge (30 × 26.5 × 15 cm) lobulated heterogeneously hyper-vascular mass lesion filling the whole abdominal cavity and extending down to the pelvis with internal cystic components.
The patient was transfused with four units of packed red blood cells, and a decision was made for an exploratory laparotomy. He was taken to the operating theater and the peritoneal cavity was accessed through a generous midline incision with an intraoperative finding of a huge highly vascular mass measuring 32 × 30 × 15 cm extending down to the pelvis. The tumor originated from the posterior aspect of the distal greater curvature with a wide base and adhering to the transverse colon and the transverse mesocolon (Figs 2 and 3). The main vascular origin was the right gastroepiploic artery. There was no true invasion of adjacent organs or metastasis. Mass was dissected free from adjacent organs and distal gastrectomy with total tumor excision and Roux-en-Y gastrojejunostomy was done. There was no intraoperative accident and the tumor weighed 10.5 kg. The postoperative course of the patient was uneventful and he was discharged on the 4th postoperative day to the case of the clinical oncologists for initiation of tyrosine kinases inhibitors.
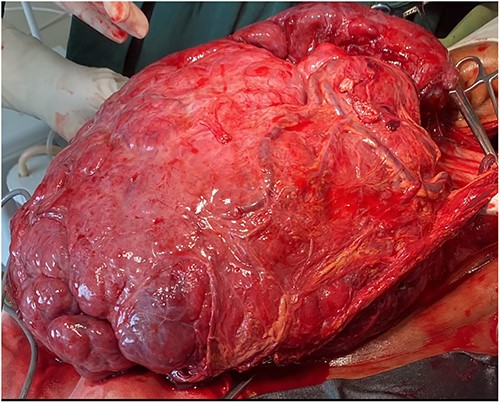
A large hyper-vascular abdominal tumor (32 × 30 × 15 cm) excised en-block with distal gastrectomy.
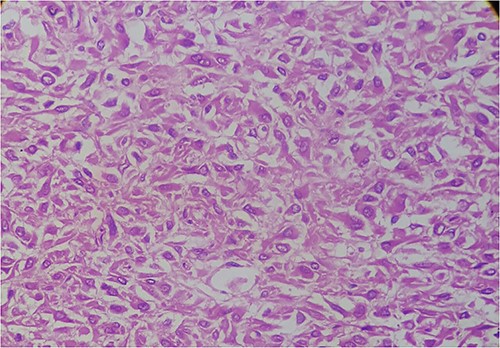
Histologic section of the tumor showing epithelioid cells with paranuclear clearance.
Histopathology revealed the proliferation of epithelioid cells with paranuclear clearance and skinoid fibers with areas of necrosis, but no mitotic activities. The final diagnosis became that of a moderate risk of epithelioid GIST (Fig. 4).
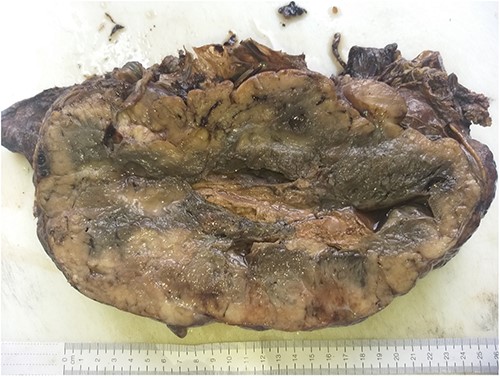
Gross tumor sectioned appearance with a well-circumscribed gray, white solid mass with areas of hemorrhage and cyst.
DISCUSSION
GISTs are relatively large-sized tumors with an average reported size of 6.8 cm, although even larger median sizes have been reported [6, 7]. In our patient’s case, he was symptomatic with a tumor size closer to the largest GIST ever reported 42 cm than the average size [8]. Fortunately, there was no metastasis detected at the time of surgical exploration.
The two previous reports of intra-tumoral bleeding-related presentations of GISTs were both in patients with huge intra-abdominal tumors of size larger than 30 cm [6, 7]. Both patients presented with GIST had complaints and physical findings consistent with anemia, as in our case. One of the previously reported cases originated from the distal stomach, whereas the other was from the jejunum [6, 7] In both of the previous reports of GIST patients with intra-tumoral bleeding, CT scan demonstrated solid and cystic components of the tumor depicting tumor necrosis with a potential of the space to occupy central hemorrhage into the tumor [8, 9]. Similar imaging characteristics were seen in our case as well. But one peculiar finding is the absence of CT signs of active hemorrhage seen as a contrast blush.
Exploratory laparotomy with excision of the mass en-block was done in our case, as well as the two cases reported with similar diagnoses [6, 7]. Surgery could be the favored approach for a few reasons. First, these tumors are generally large and symptomatic besides symptoms associated with bleeding, including pain, early satiety, respiratory distress and obstructive symptoms mandating tumor excision. Second, surgical excision of GIST is considered curative, and adjacent organ involvement is generally rare making the excision relatively a safe and effective endeavor [10, 11]. On the other hand, surgical exploration comes with the risk of tumor rupture and consequent hemorrhage, tumor recurrence and shortened survival [12].
Tumors larger than 10 cm originating from the stomach are either moderate or high risk based on the associated levels of mitotic index [13]. This risk stratification is associated with the overall outcome of the patients [14]. A peculiar finding in our report is that unlike most reports associating size with an increase in mitotic index, with such a large tumor the mitosis was not detected during histologic examination [15].
All patients with GIST except low-risk patients with complete tumor excision require adjuvant treatment with imatinib [16]. Similarly in our case, the patient had fulfilled size criteria of >10 cm to fulfill a risk stratification above low risk requiring imatinib therapy.
In conclusion, patients presenting with symptoms and signs consistent with anemia that has developed over a short duration of time with an associated increase in a newly diagnosed or previously detected abdominal mass require an investigation with a contrast-enhanced CT scan. With suspicion of GIST with intra-tumoral bleeding, the management should be surgical en-block excision of the tumor and adjuvant treatment with imatinib based on the risk stratification.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
No funding received.



