-
PDF
- Split View
-
Views
-
Cite
Cite
Roberto Cunha, Manuel Silva, Alberto Henrique, Pedro Maximiano, Mafalda Correia, Isabel Vieira, Isabel Cássio, Nelson Oliveira, Emanuel Dias, Management of median arcuate ligament syndrome: a case-based review, Journal of Surgical Case Reports, Volume 2023, Issue 7, July 2023, rjad424, https://doi.org/10.1093/jscr/rjad424
Close - Share Icon Share
Abstract
Dunbar syndrome or median arcuate ligament syndrome is a rare pathology that has a great impact on the quality of life of patients. This brief report aims to present a case report of a successful treatment of Dunbar syndrome and to review the current management of this entity. We present the case of a 37 year-old patient, who was treated by median arcuate ligament laparoscopic resection. The median arcuate ligament syndrome is associated with significant morbidity. There are no diagnostic criteria established so alternative causes of abdominal pain must be excluded. Celiac artery decompression by laparoscopic approach is currently the preferred treatment. Early diagnosis and treatment of this pathology allow a significant improvement in the quality of life of patients.
INTRODUCTION
Dunbar syndrome or median arcuate ligament syndrome (MALS) is a rare pathology caused by compression of the celiac artery by the median arcuate ligament (MAL)—a fibrous arch connecting the right and left crura of the diaphragm. It occurs mainly in female patients between 30 and 50 years old and is manifested by the classic triad of postprandial epigastric pain, weight loss and epigastric bruit. It may also manifest as exercise-induced pain, nausea and vomiting. The diagnosis depends on the exclusion of alternative causes of abdominal pain, since there is no universal diagnostic criteria [1]. Due to the important morbidity, the treatment can significantly improve the quality of life of patients.
CASE REPORT
A 37-year-old woman with autoimmune thyroiditis, epilepsy, anti-erythrocyte S antibody and with suspected mixed cryoglobulinemia under study was evaluated for recurrent postprandial abdominal pain with 6 months of evolution, fullness and vomiting with copious meals and weight loss of about 7 kg in 6 months, having already performed a computed tomography angiography (CTA) that revealed MALS (Fig.1). In collaboration with the General Surgery Department, a section of the MAL and lysis of the adhesions by laparoscopic approach was performed. On the third postoperative day, the patient developed a chylous fistula that resolved with conservative strategy including oral diet discontinuation, parenteral nutrition and octreotide. At 1 year follow-up, the patient showed clinical improvement in abdominal pain and food tolerance, and imagiological improvement (Fig.2).
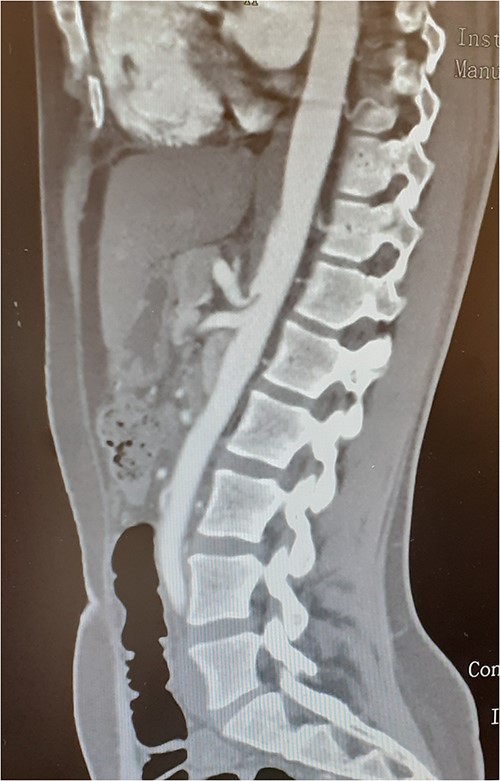
Compression of the celiac artery origin compatible with MALS; note the indentation on the superior wall of the celiac artery, leading to focal stenosis and absence of arterial wall thickening close to the stenosis.
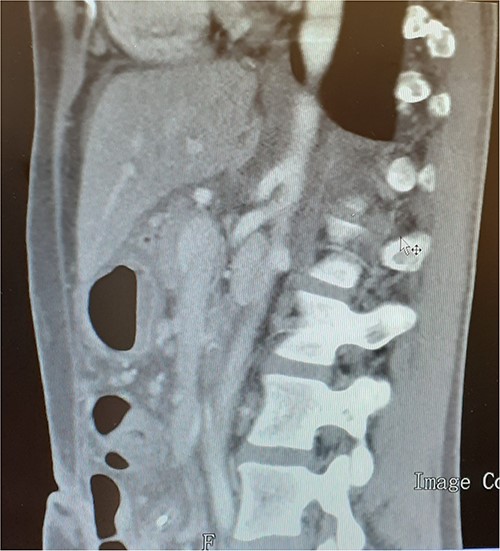
DISCUSSION
The location of the MAL and the origin of the celiac artery may vary, so a caudal location of the MAL or a cranial origin of the celiac artery may trigger MALS. Compression is increased during expiration and reduced during deep inspiration due to diaphragm movements [2]. The proximity to the celiac ganglion, neuropathic pain by overstimulation of the sympathetic nervous system fibers by compression may occur. At a histological level, chronic compression of the celiac artery may induce proliferation of smooth muscle cells, abnormal elastic fibers and disorganization of the media and adventitial layers that may end up to arterial occlusion [1].
The diagnosis of MALS is based on the association of symptoms of chronic mesenteric ischemia with imagiologic findings [3]. Since there is no consensus on diagnostic criteria, Doppler ultrasound can be used as an initial screening, identifying an increase in peak systolic velocities (>200 cm/s) during forced expiration and post-stenotic dilation. CTA during expiration reveals a hook-shaped stenosis and allows the determination of the celiac artery deflection angle, which, if >45–50°, may be suggestive of MALS, differentiating it from an atherosclerotic stenosis. Angiography is the gold-standard for revealing dynamic compression with forced expiration and allows assessing the degree of collateralization.
Some authors demonstrated that individuals with extensive collateral mesenteric circulation (classified as at least one collateral clearly visible on nonselective angiography) are less likely to benefit from MAL release [1].
Treatment consists of celiac artery decompression by transection of the MAL, with or without resection or ablation of the celiac ganglion to relieve neuropathic pain. Laparoscopic decompression is currently the preferred treatment. Balloon or stent angioplasty or conventional artery revascularization (aortoceliac bypass or a celiac artery patch angioplasty) may be used as adjuvants, but preferably after decompression in case of refractory symptoms. Robot-assisted MAL release and celiac ganglionectomy represents an emerging treatment modality but with higher operative time [4].
To conclude, MALS is a rare pathology that causes great morbidity. Thus, early diagnosis and treatment allow a significant improvement in the quality of life of patients.
CONFLICT OF INTEREST STATEMENT
The authors declare that there is no conflict of interest.
FUNDING
This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
DECLARATION OF PATIENT CONSENT
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understand that his name and initials will not be published, and due efforts will be made to conceal his identity.



