-
PDF
- Split View
-
Views
-
Cite
Cite
Kentaro Kaji, Hirofumi Tsubouchi, Masahiko Mori, Shiro Suzuki, Postoperative transverse colon necrosis due to mesenteric injury during laparoscopic surgery for endometrial carcinoma, Journal of Surgical Case Reports, Volume 2023, Issue 1, January 2023, rjac636, https://doi.org/10.1093/jscr/rjac636
Close - Share Icon Share
Abstract
Hemorrhage and organ injury have been frequently reported as complications associated with trocar puncture in laparoscopic surgery. This report presents a case of delayed intestinal necrosis due to mesenteric injury. A 76-year-old woman who had a history of distal gastrectomy and adrenal insufficiency was diagnosed with stage IA endometrial cancer. We performed laparoscopic total hysterectomy and bilateral salpingo-oophorectomy. The upper abdominal wall and mesentery were adhered, and bleeding from the mesentery was noted during the first trocar puncture of the umbilical region, resulting in ligation and hemostasis. Abdominal pain and fever developed on the third postoperative day, and contrast-enhanced computed tomography demonstrated transverse colon perforation. Emergency laparotomy showed necrosis in the proximal transverse colon and a defect in the marginal artery. Mesenteric injury can lead to delayed intestinal necrosis without intraoperative macroscopic findings. In laparoscopic cases where adhesion is expected, trocar placement should be carefully considered.
INTRODUCTION
Many complications due to trocar puncture have been reported. But there is no case report of delayed intestinal necrosis due to mesenteric injury. We report a case in which the transverse mesocolonial marginal artery was injured during the first trocar puncture of laparoscopic surgery for endometrial carcinoma, resulting in postoperative necrosis of the transverse colon.
CASE REPORT
The patient was a 76-year-old woman with a history of distal gastrectomy for gastric cancer. She was taking hydrocortisone because of adrenal insufficiency due to adjuvant chemotherapy. She also had a history of cerebral infarction and was receiving clopidogrel.
She was diagnosed with Grade 1–2 endometrioid carcinoma by endometrial histology. Body mass index was 19.4. Her upper umbilicus–xiphoid process exhibited surgical scarring. On pelvic contrast-enhanced magnetic resonance imaging, no evidence of myometrial infiltration was found. Thoracic–pelvic contrast-enhanced computed tomography (CT) demonstrated no obvious metastases. Thus, preoperative stage was IA (International Federation of Gynecology and Obstetrics 2008).
She was on long-term oral steroids, and preoperative examination revealed diabetes, which was considered a high risk for wound infection and adhesion failure. Therefore, laparoscopic total hysterectomy (extrafascial surgery) and bilateral salpingo-oophorectomy were performed.
The first trocar was placed in the umbilical region by the open method. At that time, there was small arterial bleeding. When the fascia incision was extended, a ruptured blood vessel and the fat membrane considered to be the remaining omentum was confirmed, so the same site was ligated with 3–0 polyglactin thread. Abdominal wall on the cranial side of the umbilical region and the transverse colon were markedly adhered, making it difficult to sufficiently observe the upper abdomen. As no adhesion was found in the lower abdomen, surgical ports were placed in three additional locations (Fig. 1). The operation was completed after confirming that there was no color change or bleeding in the intestinal tract before closing the abdomen. The uterine manipulator was not used. The surgical time was 2 hours and 47 minutes, and the volume of blood loss was 15 ml.
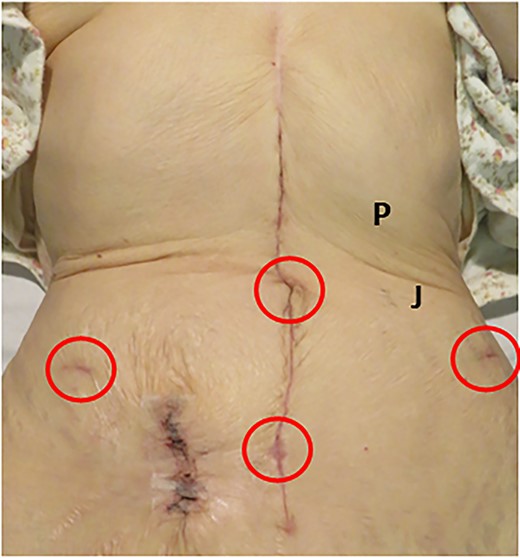
Abdomen of the patient, upper umbilicus–xiphoid process showed scarring during gastric cancer surgery. Trocars were placed in four places (red circles). Palmer’s point (P): 3 cm below the lower edge of the rib arch on the midclavicular line; Jain point (J): the left paraumbilical region 2.5 cm medially above the anterior superior iliac spine and up to the side of the navel.
The patient drank water the first day after surgery and resumed oral intake on the second day after surgery. On the morning of the third day after surgery, she developed lower abdominal pain and 38°C fever. Abdominal contrast-enhanced CT demonstrated that the continuity of the transverse colon wall was interrupted. Abscess formation with a surrounding stool mass was suspected (Fig. 2). Therefore, emergency laparotomy was performed.
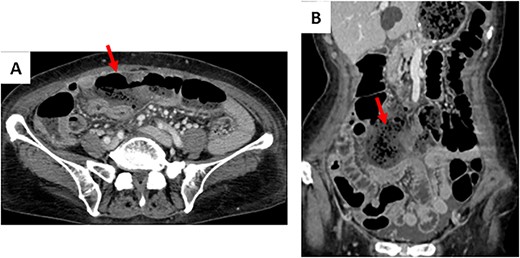
Contrast-enhanced CT on the third day after the primary operation. (A) The continuity of the transverse colon wall was interrupted. (B) Abscess formation was suspected with a surrounding stool mass.
The proximal transverse colon was necrotic for ~5 cm, and the wall was markedly thin, but no perforation was noted (Fig. 3). The marginal artery of the mesentery corresponding to the necrotic transverse colon was missing, suggesting intestinal necrosis due to ischemia. As the ascending colon was short, right hemicolectomy was performed, and a temporary ileostomy was constructed.
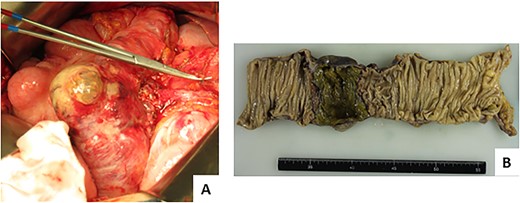
Findings on repeat surgery. (A) The wall was markedly thin, but no perforation was noted. (B) Necrotic changes were observed locally on the mucosal surface of the colon by ~5 cm.
The pathological diagnosis of endometrial cancer was Grade 3 endometrioid carcinoma and was stage IA. The patient was followed up without adjuvant chemotherapy in consideration of her age, history and her own opinion. The postoperative course was favorable, and ileostomy closure was performed ~2 months after the operation. The patient had been followed up for 23 months after surgery without notable findings.
DISCUSSION
We reported a first case of delayed partial intestinal necrosis due to mesenteric injury during the first trocar puncture.
In this case, the missing blood vessel was a marginal artery of the transverse mesentery. The marginal arteries that run parallel to the colon in the mesentery are the major collaterals from the ileocolic artery to the sigmoid artery [1]. Therefore, the marginal artery defect site may have gradually developed ischemia. It is insufficient to judge the intestinal blood flow based on the gross findings of the intestinal surface, and the indocyanine green fluorescence method is useful for evaluating the blood flow [2]. Even gynecologists should assume that damage of mesenteric blood vessels can have a serious outcome.
With regard to the first trocar puncture, there are reports comparing the open and closed method [3, 4] and the usefulness of the optical method of performing the first trocar puncture under visualization with an endoscope has also been reported [5]. However, Cochrane’s meta-analysis concluded that there is insufficient evidence to compare these methods for vascular and organ damage [6]. For the first trocar placement position, puncture from Palmer’s point is currently the most common when adhesion in the umbilical region is expected. Palmer’s point is a point 3 cm below the lower edge of the rib arch on the midclavicular line (Fig. 1) [7], and it is contraindicated in patients with a history of gastric and pancreatic spleen surgery. Jain et al. reported the Jain point as a safe puncture position for patients after gastric or pancreatic spleen surgery. The Jain point is in the left paraumbilical region 2.5 cm medially above the anterior superior iliac spine and up to the side of the navel (Fig. 1) [8]. However, in this case, puncture from the Jain point was considered difficult because the abdominal wall at the umbilical level was markedly adhered to the intestinal tract on both the left and right sides. There is other report on the usefulness of puncture from the left ninth intercostal space [9], but it is considered difficult to select after gastric surgery. As no adhesion in the lower abdomen was observed in this case, the abdominal cavity may have been able to be safely observed if the first trocar puncture was performed by the open method at the position of the operation port in the middle of the lower abdomen (Fig. 1). Bladder elevation is unlikely in patients with no history of lower abdominal surgery. Therefore, in gynecological laparoscopic surgery after open surgery of the upper abdomen, setting the first trocar puncture in the middle of the lower abdomen only in patients with no history of surgery in the lower abdomen may be the first option.
Damage of mesenteric blood vessels can occur delayed intestinal necrosis. And for patients with expected intra-abdominal adhesion, we must carefully consider the indications for laparoscopic surgery and the placement of the first trocar.
CONSENT
Informed consent has been obtained from the patient and assent has been given. The patient consented to report this case and the attached images.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
DATA AVAILABILITY
Data sharing is not applicable to this article as no datasets were generated or analyzed.
References
- abdominal pain
- computed tomography
- marginal branch of right coronary artery
- hemorrhage
- hemostatic function
- adrenal gland hypofunction
- endometrial cancer
- fever
- adhesions
- intestines
- intraoperative care
- intraoperative complications
- laparoscopy
- laparotomy
- ligation
- mesentery
- necrosis
- umbilicus
- hemostasis procedures
- laparoscopic surgery
- abdominal wall
- trocar
- hysterectomy, laparoscopic
- endometrial carcinoma
- salpingo-oophorectomy
- hysterectomy, radical
- billroth i procedure
- mesenteric injuries
- transverse colon



