-
PDF
- Split View
-
Views
-
Cite
Cite
Shilpa Malik, Tina Jagtiani, Odise Cenaj, Aleksandr Rakhlin, Amebic appendicitis: a case report, Journal of Surgical Case Reports, Volume 2023, Issue 1, January 2023, rjac551, https://doi.org/10.1093/jscr/rjac551
Close - Share Icon Share
Abstract
Changing the paradigm of treatment of acute appendicitis to non-operative management can miss unusual etiologies that can only be diagnosed on pathologic analysis. Presented is a case of amebic appendicitis in which antibiotic management was dictated by post-operative pathology findings.
INTRODUCTION
Acute appendicitis is a common general surgical entity; however, the management of appendicitis while being invariably operative is changing to antibiotic administration and observation [1]. The diagnosis has been clinical but imaging, often a computed tomography (CT) scan, has become an integral part of the workup. Whereas luminal obstruction is the common denominator in the pathophysiology of the disease and is commonly caused by fecaliths or lymphoid hyperplasia, a multitude of microorganisms are implicated in pathogenesis including Entamoeba histolytica. Entamoeba histolytica instigating amebic appendicitis is rare however, it is seen among those who traveled to or reside in high-risk countries such as India, Uganda, Pakistan and Turkey [2]. The most common treatment for acute appendicitis is still operative, via laparoscopic appendectomy, and is performed quickly after diagnosis. The underlying cause of appendicitis is often not discovered until pathology is later analyzed. Here, we present a patient with amebic appendicitis who would not have been treated adequately if only first-line antibiotics such as amoxicillin/clavulanate were given [1].
CASE REPORT
A 48-year-old female with history of diabetes presented with right lower quadrant (RLQ) pain for one day. The patient complained of nausea and denied vomiting or fever. She denied diarrhea, constipation, or pain before this and took no medications before arrival. Her last travel was 1 year before the Dominican Republic.
Physical exam was significant for RLQ tenderness, without peritoneal signs. On laboratory analysis, she had slight leukocytosis (11 000 with 90% neutrophils); however, electrolytes and liver function tests were normal.
CT imaging showed an appendix dilated to 13 mm with wall thickening, periappendiceal induration and appendicoliths (Fig. 1).
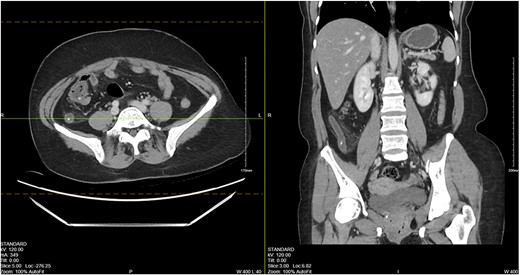
CT abdomen/pelvis showing a dilated appendix with wall thickening, periappendiceal induration and appendicoliths.
After discussion of treatment options and consent for surgery, a laparoscopic appendectomy was performed for an acutely inflamed appendix draping along the right pelvic sidewall, up the ascending colon. The patient was discharged without antibiotics and was seen without complications after 1 week.
Pathology resulted on post-operative day three showing an inflamed appendix, 1.4 cm in diameter, with an exudative-filled lumen. On microscopic stains, there was evidence of acute appendicitis with frequent scattered unicellular organisms within areas of ulcerated appendiceal mucosa and submucosa (Figs 6 and 7). These cellular forms have round cell membranes, single prominent round eosinophilic nuclei and foamy cytoplasm (Fig. 5). Occasional forms show evidence of erythrophagocytosis (Fig. 3). Forms were also highlighted by trichrome and PAS special stains (block A1) and were negative for CD68 (a marker of macrophages; block A1) (Figs 2–4). These morphologic features are most consistent with E. histolytica, which is a pathogenic parasite in the lower GI tract, and likely the causative agent for acute appendicitis in this case.
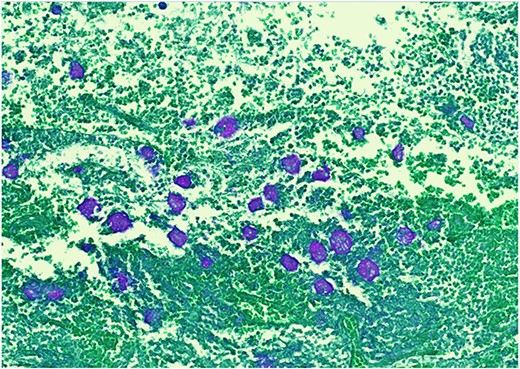
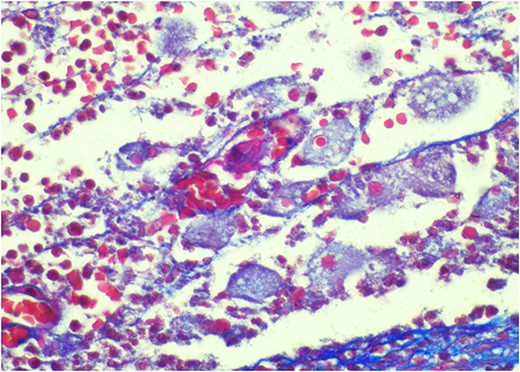
Trichrome stain—parasites are positive; erythrophagocytosis supporting Entamoeba histolytica.
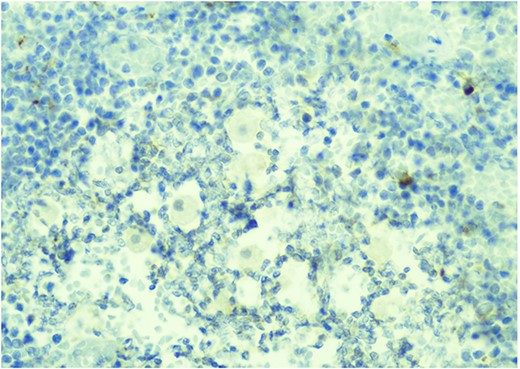
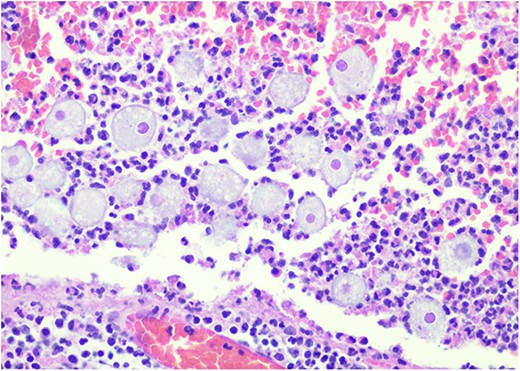
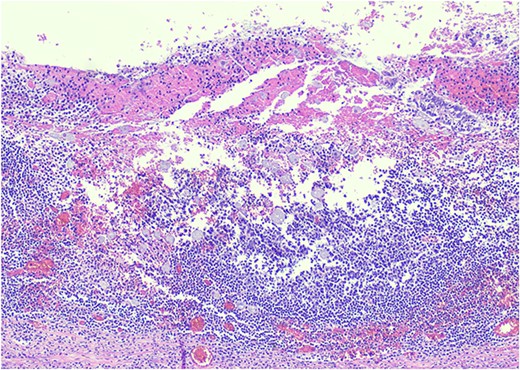
H&E 200X—unicellular parasites within submucosal tissue with inflammation.
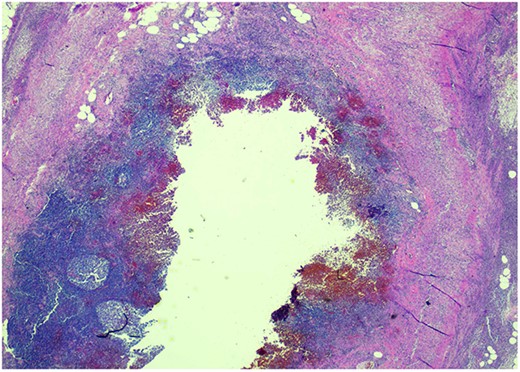
DISCUSSION
Amebiasis presents in a multitude of ways ranging from asymptomatic disease to pathologic effects on the colon or liver [3]. Entamoeba histolytica is transmitted through a fecal-oral route and presents with symptoms of dysentery such as bloody diarrhea or liver abscess [4]. On pathological sections, E. histolytica can present as either trophozoites with engulfed red blood cells in the cytoplasm or as multinucleated cysts in a stool sample [5]. In addition to amebiasis, E. histolytica can incite appendicitis through the invasion of the appendiceal wall, obstructing its lumen. Acute appendicitis of parasitic origin is rare, with E. histolytica accounting for an incidence of 0.5–2.3% [3]. The presentation of amebic appendicitis is no different than appendicitis of non-amebic origin, making it difficult to distinguish before pathologic evaluation.
Acute appendicitis presents with periumbilical pain migrating to the RLQ, often associated with nausea and vomiting. Viscerosomatic reflexes of the midgut contribute to the colicky abdominal pain, whereas the engagement of the parietal peritoneum contributes to the more localised RLQ pain. On physical exam, rigidity, rebound tenderness and guarding can be appreciated. Tachycardia and pyrexia may also be appreciated because possible infection and can be reflected by leukocytosis with neutrophilia (>75%) [6]. Various modalities of imaging can be used to diagnose appendicitis, with CT being the most sensitive and specific. An abnormal appendix can present on CT as a calcified appendicolith with periappendiceal inflammation.
Infection with parasites is uncommon in countries with proper sanitary conditions and clean water supply. Entamoeba histolytica is seen in high-risk countries [2] or diagnosed in patients with a history of travel to high-risk countries (64%). Appendicitis because of parasitic origin is overlooked in developed countries, which often delays intervention. Entamoeba histolytica-related appendicitis should be treated with appropriate measures including metronidazole followed by paromomycin or iodoquinol after being diagnosed post-operatively. With the increasing prevalence of non-operative treatment of appendicitis, this diagnosis of amebic appendicitis may have been missed. Subsequently, insufficient antibiotics would have been prescribed, leading to increased morbidity, thus supporting operative treatment of appendicitis.
Treatment for acute appendicitis is historically managed with surgery; however, some studies indicate treatment with antibiotics alone. Whereas antibiotics may manage symptoms, other etiologies of appendicitis can be left untreated leading to further disease progression. Besides parasitic causes, carcinoid tumors of the appendix can be diagnosed with the same symptomatology as acute appendicitis and are often detected post-operatively on histopathology. Although the incidence is 0.30–2.27%, carcinoid tumors greater than 1–2 cm may need subsequent hemicolectomy, especially if the mesoappendix is involved [7]. This further supports the paradigm that operative treatment of appendicitis can aid in the diagnosis of underlying pathologies that may be missed otherwise.
CONFLICT OF INTEREST STATEMENT
None declared.
FUNDING
None.
References
Author notes
S. Malik and T. Jagtiani contributed equally to this work



