-
PDF
- Split View
-
Views
-
Cite
Cite
Samantha Scarola, Udai S Sibia, Glen Gibson, Gallbladder cancer presenting as hemobilia on capsule endoscopy, Journal of Surgical Case Reports, Volume 2022, Issue 5, May 2022, rjac202, https://doi.org/10.1093/jscr/rjac202
Close - Share Icon Share
Abstract
Gallbladder adenocarcinoma is a rare gastrointestinal malignancy and is associated with a poor prognosis. These malignancies are most often discovered incidentally in |$\sim$|1% of all cholecystectomy procedures. We report an 80-year-old male patient with iron deficiency anemia, who underwent an unremarkable endoscopy and colonoscopy, and was subsequently found to have hemobilia discovered on capsule endoscopy. Magnetic resonance cholangiopancreatography revealed a space-occupying process involving the posterior wall of the gallbladder. The patient underwent an unremarkable laparoscopic cholecystectomy with final pathology revealing a well-differentiated, 8 cm intracystic papillary neoplasm with high-grade dysplasia involving the majority of the gallbladder, with focally invasive adenocarcinoma invading the muscular layer of the gallbladder wall. Postoperative staging work-up revealed no evidence of metastatic disease. Patient then underwent a radical resection of segments 4B/5 of the gallbladder fossa and lymph node resection of the porta hepatis. Final pathology revealed Stage I adenocarcinoma of the gallbladder (T1bNxM0).
INTRODUCTION
Gallbladder adenocarcinoma is a rare gastrointestinal malignancy. It is associated with a poor prognosis, with a mean survival of 6 months and a 5-year survival of 5–20% [1]. In the United States, the incidence of gallbladder adenocarcinoma is one to two cases per 100 000 people. It is more prevalent in women than men [2]. Risk factors include cholelithiasis, porcelain gallbladder, gallbladder polyps, primary sclerosing cholangitis, chronic infection (i.e. salmonella, helicobacter), congenital biliary cysts, abnormal pancreaticobiliary duct junction, obesity and medications (i.e. methyldopa, oral contraceptives and isoniazid). Chronic gallbladder inflammation plays a key role in the pathogenesis. The most common histologic subtype is adenocarcinoma, making up 76% of all gallbladder neoplasms [3]. These malignancies are most often discovered incidentally, in |$\sim$|1% of all cholecystectomy procedures [4].
Gallbladder neoplasms are associated with nonspecific findings. Early disease is often asymptomatic. Patients present with symptoms of biliary colic, cholelithiasis and cholecystitis. More advanced malignancy presents with constitutional symptoms, such as malaise and weight loss. This report outlines a case of an 80-year-old male patient with iron deficiency anemia (IDA) who was diagnosed with hemobilia on capsule endoscopy and ultimately found to have a gallbladder neoplasm. Hemobilia is a (1–7%) rare presenting sign of biliary neoplasm. To the best of our knowledge, this is the first report of gallbladder cancer presenting as hemobilia on capsule endoscopy.
CASE REPORT
An 80-year-old male patient presented to his primary care physician with a chief complaint of fatigue. Further work-up was notable for IDA (Table 1). He was referred to a gastroenterologist and underwent an upper endoscopy that demonstrated some nodularity in the duodenum with evidence of mucosal changes of celiac disease, but final biopsy showed no suspicious findings. The colonoscopy was unremarkable. A capsule endoscopy was then performed which demonstrated fresh blood from an otherwise normal appearing ampulla of Vater, suggestive of a hepato-pancreatico-biliary source of hemobilia (Fig. 1). A follow-up computer tomography (CT) enterography demonstrated an abnormal appearing gallbladder with linear calcifications and intraluminal debris. The patient was subsequently referred to a surgical oncologist for hemobilia and an abnormal appearing gallbladder.
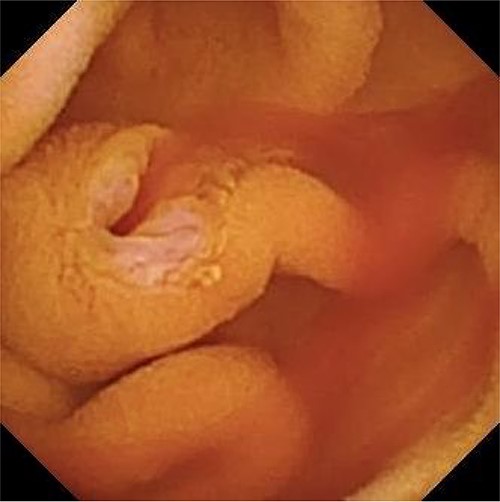
Capsule endoscopy showing fresh blood from an otherwise normal appearing ampulla of Vater.
The preoperative work-up included a magnetic resonance cholangiopancreatography (MRCP), which showed a normal appearing biliary tree, but an abnormal appearing gallbladder with numerous gallstones and a space-occupying process involving the posterior wall (Fig. 2). The patient subsequently underwent an unremarkable laparoscopic cholecystectomy. Intraoperative findings revealed a distended, chronically inflamed gallbladder. No other suspicious findings were noted. Final pathology revealed a well-differentiated, 8 cm intracystic papillary neoplasm with high-grade dysplasia involving the majority of the gallbladder, with focally invasive adenocarcinoma invading the muscular layer of the gallbladder wall. These findings were consistent with a pT1bNx tumor.
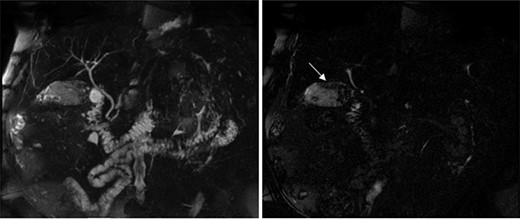
MRCP showing a normal appearing biliary tree (left), but an abnormal appearing gallbladder with numerous gallstones and a space-occupying process (right marked by arrow) involving the posterior wall.
| Laboratory test . | Value . |
|---|---|
| Hemoglobin | 13 g/dl |
| Hematocrit | 40.8% |
| Iron | 45 μg/dl |
| Iron saturation | 13% |
| Iron binding | 354 μg/dl |
| Ferritin | 25.6 ng/ml |
| Vitamin B12 | 410 pg/ml |
| Laboratory test | Value |
|---|---|
| Hemoglobin | 13 g/dl |
| Hematocrit | 40.8% |
| Iron | 45 μg/dl |
| Iron saturation | 13% |
| Iron binding | 354 μg/dl |
| Ferritin | 25.6 ng/ml |
| Vitamin B12 | 410 pg/ml |
Staging work-up revealed a carcinoembryonic antigen (CEA) level < 0.5 ng/ml, CA 19–9 level 8.0 U/ml and a positron emission tomography scan without evidence of metastatic disease. In accordance with National Comprehensive Cancer Network guidelines, the patient then underwent a radical resection of segments 4B and 5 of the gallbladder fossa, and lymph node resection of the porta hepatis [5]. Final pathology revealed Stage I adenocarcinoma of the gallbladder (T1bNxM0). Patient had no evidence of disease at his 6-month follow-up.
DISCUSSION
Gallbladder adenocarcinoma, due to its insidious and often asymptomatic onset, is a rare gastrointestinal malignancy associated with a poor prognosis. In symptomatic cases, patients typically present with a cholestasis pattern of jaundice, biliary colic or steatorrhea. This report outlines a rare presentation of an 80-year-old male patient with Stage I T1bNx gallbladder adenocarcinoma discovered via a CT enterography revealing hemobilia.
Hemobilia is defined by bleeding into the biliary tract and is commonly associated with colicky pain and jaundice [6]. Hemobilia accounts for only 2–5% of gastrointestinal bleeding. It is most commonly caused by trauma, calculi, inflammation or vascular disorders. Hemobilia caused by gallbladder cancer is an even rarer finding [6], with only 1% of hemobilia cases caused by cancer [6, 7]. Upper endoscopy is the gold standard for diagnosis, with >60% of hemobilia cases diagnosed by endoscopy [6, 7]. Those with inconclusive endoscopy then undergo CT angiography of the abdomen.
Capsule endoscopy is often reserved for patient with gastrointestinal bleeding that is not identified on upper or lower endoscopy. The study helps localize the source of bleeding in the small bowel. This report describes a rare clinical scenario where this patient was found to have hemobilia on capsule endoscopy, which is not the standard for diagnosing hemobilia. This highlights the need to consider all imaging modalities in patients with IDA, as rare cases of gallbladder cancer can be identified using additional imaging modalities.
This patient underwent an uncomplicated laparoscopic cholecystectomy, followed by a radical resection of segments 4B and 5 of the gallbladder fossa, and lymph node resection of the porta hepatis for a Stage I adenocarcinoma of the gallbladder (T1bNxM0). This is a unique case of IDA resulting from hemobilia, which on thorough work-up that included a capsule endoscopy, led to the diagnosis and eventual successful treatment for an otherwise ominous disease. To the best of our knowledge, this is the first report of gallbladder cancer presenting as hemobilia on capsule endoscopy.
References
- cancer
- cholecystectomy
- colonoscopy
- adenocarcinoma
- endoscopy
- gallbladder cancer
- gastrointestinal cancer
- biliary tract hemorrhage
- iron deficiency anemia
- lymph node excision
- neoplasm metastasis
- gallbladder
- neoplasms
- pathology
- laparoscopic cholecystectomy
- magnetic resonance cholangiopancreatography
- gallbladder adenocarcinoma
- capsule endoscopy
- porta hepatis
- dysplasia
- gallbladder wall



