-
PDF
- Split View
-
Views
-
Cite
Cite
Toshihiro Kawahira, Fumihiro Miyashita, Tomoaki Suzuki, Rare case of ruptured muscular ventricular septal aneurysm due to silent myocardial ischemia in adult, Journal of Surgical Case Reports, Volume 2022, Issue 5, May 2022, rjac114, https://doi.org/10.1093/jscr/rjac114
Close - Share Icon Share
Abstract
Interventricular septal aneurysm of muscular type is uncommon in adult, to say nothing of membranous type. Acute or subacute left-to-right shunt (LR shunt) in a ventricular septum is mostly critical and usually shows severe symptoms. Therefore, ruptured muscular ventricular septal aneurysm (VSA) with LR shunt of unknown onset in adult is highly rare. A 70-year-old man was suffered from mild dyspnea and chest oppression. A muscular VSA was detected at the center of the ventricular septum and LR shunt of unknown onset in it had induced congestive heart failure. The sandwich patch technique through a right ventricular approach was simultaneously performed with coronary artery bypass grafting and the postoperative course was uneventful. In addition, concomitant myocardial biopsy of VSA wall during the surgery could reveal histopathologic evidence of acute or subacute myocardial infarction with old myocardial infarction as silent myocardial ischemia.
INTRODUCTION
Interventricular septal aneurysm of muscular type is uncommon in adult, to say nothing of membranous type. Because ventricular septal aneurysm (VSA) is mostly detected as membranous type in congenital cases as a rare cardiac anomaly associated with a ventricular septal defect (VSD) or other congenital anomalies. Conversely, acute or subacute left-to-right shunt (LR shunt) in a ventricular septum is generally developed in adult and mostly critical, regardless of the patient’s age. Therefore, ruptured muscular VSA with LR shunt of unknown onset in adult is highly rare and might be one of the life-threatening conditions [1, 2].
CASE REPORT
A 70-year-old man who had mild dyspnea and chest oppression was referred to our hospital for cardiac assessment of LR shunt of unknown onset in a interventricular septum. He had never been detected any congenital disorders or cardiovascular diseases before. Clinical examination revealed absence of fever and blood pressure of 97/58 mmHg with lower extremity edema.
Holosystolic murmur was audible at III–IV left sternal border as Levine III/VI. Cardiothoracic ratio was 62% on chest radiography and chest computed tomography (CT) showed bilateral pleural effusion with interstitial lung edema. Electrocardiogram (ECG) indicated normal sinus rhythm and ST depression of 0.1 mV on V4–V6 without abnormal Q wave (Fig. 1).
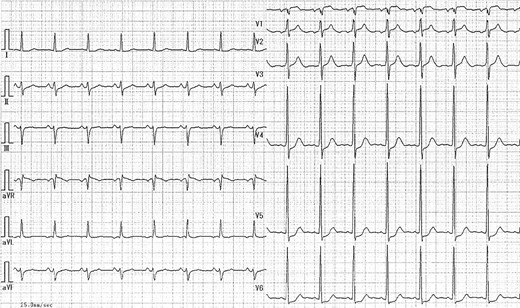
Laboratory data revealed hyperlipidemia and possible myocardial injury, as follows: creatinine kinase level of 202 IU/l, CK-MB level of 5.2 ng/ml, brain natriuretic peptide level of 412.6 pg/ml and Troponin T level of 1.58 ng/ml. Transthoracic echocardiogram (TTE) demonstrated mild pulmonary hypertension (PH), normal left ventricular ejection fraction (EF) of 67%, 15-mm VSA at the mid ventricular septum and ventricular septal rupture (VSR) of ~9 mm with estimated Qp/Qs of 2.56 (Fig. 2). Cardiac magnetic resonance imaging also recorded blood stream of shunt flow in VSA (Video 1). Moreover, coronary angiography revealed a 90% diameter stenosis of the right coronary artery and 75% lesion of the proximal left anterior descending coronary artery. Right catheterization revealed moderate PH and oxygen saturation increased due to LR shunt in the right ventricle (RV).
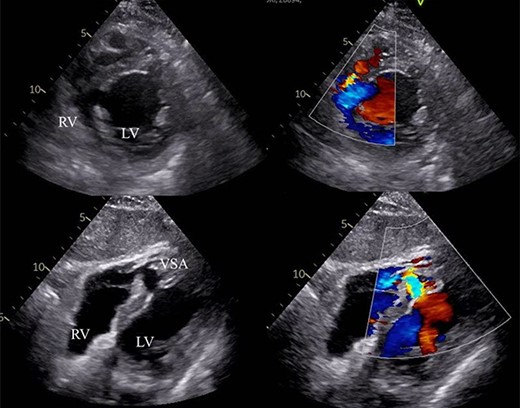
VSA with LR shunt flow. RV: right ventricle, LV: left ventricle, VSA: ventricular septal aneurysm.
After receiving informed consent, surgery was performed as patch closure of ruptured VSA and coronary artery bypass grafting (CABG) under cardiopulmonary bypass (CPB) on the 11th day after admission. Median sternotomy was done to establish a CPB by the ascending aorta and bicaval cannulation, and right supra-pulmonary venous venting was added. Cardiac arrest was obtained by cold blood cardioplegia via the coronary sinus with intermittent delivery to maintain cardiac standstill. In the surgical findings, VSA was noted at the center of the ventricular septum with circular wall defect of ~15 mm on the RV side (Fig. 3). A part of the perforated myocardium in the aneurysm was resected for histopathologic examination. After the defective edge of the VSA was carefully trimmed, it was closed by extended sandwich patch technique using the double Polyester patch. CABG was added on the left anterior descending artery using left internal thoracic artery and right coronary artery using the right greater saphenous vein.
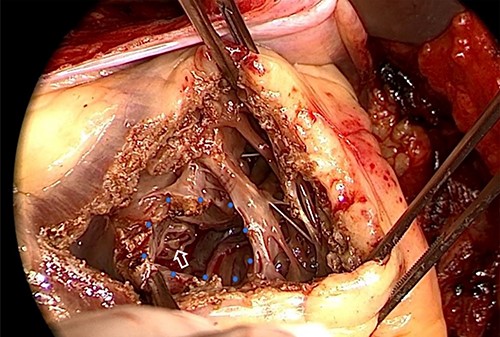
VSA at the center of ventricular septum (blue dot circle) with VSP to the RV cavity (white arrow) in the operative finding. VSA: ventricular septal aneurysm, VSP: ventricular septal perforation, RV: right ventricle.
CPB weaning was easy without any cardiac supports. Postoperative course was uneventful and the patient was discharged on the 16th day postoperatively. Residual shunt after the patch closure was not detected during postoperative investigations. Histopathologic examination on the resected myocardium of muscular VSA wall simultaneously showed necrotic tissue with fibrosis and fresh myocardial infarction (MI) area on hematoxylin and eosin stained sections (Fig. 4).
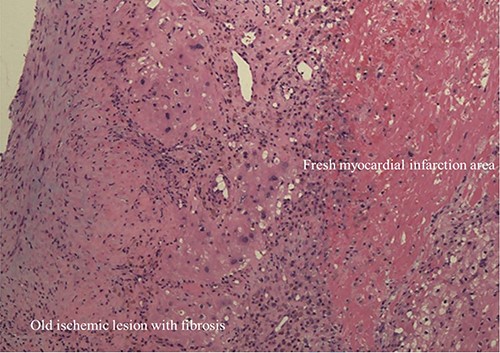
Histopathologic image of VSA wall showed old myocardial ischemic lesion with fibrosis and flesh myocardial infarction area (Hematoxylin and Eosin stain: ×200).
DISCUSSION
In the literature, VSA is a rare cardiac anomaly mostly associated with a VSD or other congenital heart diseases in childhood. VSA in childhood usually affect the membranous septum, therefore muscular VSAs are extremely rare compared with membranous type. In adult, they are related to post MI, infections, blunt trauma, previous spontaneous VSD closure and iatrogenic ischemia. Hence, most muscular VSAs are usually diagnosed by TTE or chest CT scan incidentally and complications of interventricular aneurysms may arise from chronic pressure erosion of the intervening septal myocardium, leading to LR shunting and paradoxical thromboembolism [3–6].
LR shunt on ventricular septum is generally detected as VSD in congenital cases. On the other hand, VSR usually inducing iatrogenic condition, trauma or MI is mostly developed in adult. It is substantially critical and worsened gradually, therefore, it is generally treated by surgical maneuver as soon as possible.
In this case, double patch closure using Polyester patch was performed according to extended sandwich patch technique [7]. The operation was performed after effective treatments for congestive heart failure on the 11th day after admission. Furthermore, complemental CABG is equally essential to increase coronary flow against the ischemic area and prevent recurrent myocardial ischemia.
Some symptoms suggested congestive heart failure due to acute or subacute LR shunt in previously unknown VSA, but there had been few significant manifestations of cardiac ischemia before admission. ECG and blood examinations did not show any remarkable findings of cardiac ischemia without abnormal Troponin T levels. Nevertheless, on the histopathological examination from myocardial biopsy during the surgery, apparent evidence of old myocardial infarction (OMI) with acute or subacute MI was revealed. In the histopathological image, coagulative necrosis could be detected, moreover fibrous tissue with myocardial cell lost nucleus and newborn blood vessels showed previous myocardial ischemia. In addition, bleeding and myocardial cell with infiltrated polymorphonuclear leukocyte revealed acute phase of myocardial ischemia. Two different phases of myocardial ischemia suggested that repeated silent myocardial ischemia (SMI) of Cohn type I had caused the VSA in muscular portion. And consequent acute or subacute MI occurred rupture of muscular VSA wall incidentally [8, 9].
In conclusion, we could describe a rare case of ruptured muscular VSA in adult without obvious myocardial ischemic symptoms, and myocardial biopsy of VSA wall during the surgery revealed histopathologic evidence of recurrent SMI and acute or subacute MI. It is necessary and important to acquire knowledge for high level of clinical suspicion and a relevant physical examination to lead prompt diagnosis for an accurate strategy like this rare condition.
CONFLICT OF INTEREST
The authors declare no conflict of interest.
References
- myocardial infarction
- silent myocardial ischemia
- coronary artery bypass surgery
- shunt left-right intracardiac
- dyspnea
- aneurysm
- congestive heart failure
- adult
- heart ventricle
- tissue membrane
- rupture
- surgical procedures, operative
- chest
- interventricular septum
- left to right cardiovascular shunt
- cardiac biopsy
- shunt
- histopathology tests



