-
PDF
- Split View
-
Views
-
Cite
Cite
Masakatsu Hihara, Masayasu Takegawa, Natsuko Kakudo, Toshihito Mitsui, Michika Fukui, A stylized two-stage debridement strategy using an electric dermatome and a Versajet™ hydrosurgery system for deep axillary burns, Journal of Surgical Case Reports, Volume 2022, Issue 10, October 2022, rjac481, https://doi.org/10.1093/jscr/rjac481
Close - Share Icon Share
Abstract
Treatment of axillary contracture after extensive deep burns is a serious clinical challenge. Various surgical intervention for releasing contracture using skin grafts, flaps and artificial skin have been used, but no consensus on the optimal treatment has been obtained. A standardized two-stage debridement strategy using an electric dermatome (for eschar) and the Versajet™ hydrosurgery system (for slough) can be an appropriate debridement strategy that provides reliable wound bed preparation in cases of for axillary deep burns. Using this approach focus on management of acute axillary burns, it is possible to avoid engraftment failure and prevent contracture caused by prolonged infection. This treatment strategy can be standardized and can be performed easily, even by non-experts.
INTRODUCTION
In flame burns triggered by the ignition of clothing, the deep burn area often extends not only to the trunk but also to the axilla; thus, scar contracture in this area causes impairment in daily life functions. In the case of sequential debridement for deep burns, immediate debridement for eschar with electric devices and late debridement for slough with a Versajet™ hydrosurgery system and subsequent chemical debridement (which is performed at fixed intervals) can be a valid step in step surgical intervention. We herein report the usefulness of a stylized two-stage debridement strategy for the purpose of preventing strong scar contracture.
CASE PRESENTATION
The patient was a 70-year-old man with a flame burn that occurred due to the ignition of his clothing at home. He suffered deep burns (22% of his total body surface area [deep burn, 14%, superficial dermal burn, 8%] to the neck, back and right upper limb) and was transported to our critical care center. Respiratory and circulatory management was initiated immediately, and first-stage debridement for eschar using an electric dermatome (0.4-mm thickness) was performed 12 h after the burn injury (Fig. 1). Burned wound cleansing was then continued. Ten days after the injury, the necrotic tissue had softened, and second-stage debridement for slough using the Versajet ™ hydrosurgery system (power setting: 5–10) was performed as a late surgery (Fig. 2). At this time, necrotic tissue that required removal was floating on the burn wound and the line of debridement was clarified. Therefore, the surgeon could confidently perform radical debridement. The patient did not develop any infectious complications during the time. Achieving good granulation of the wound bed at 3 weeks after the injury, 3:1 mesh auto-grafts were applied to wound bed. After 8 weeks performing shoulder range of motion mobilization exercises, all skin grafts had taken, and an excellent range of motion was obtained without contracture (Fig. 3).
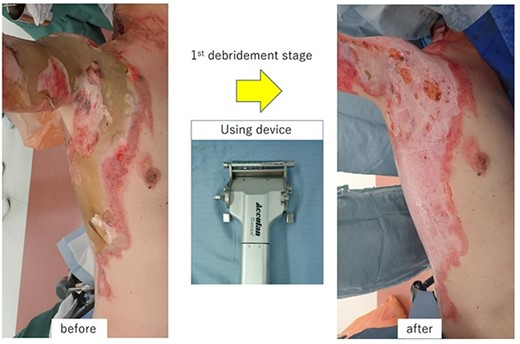
A first-stage debridement for eschar using an electric dermatome (0.4-mm thickness) was performed 12 h after the burn injury.
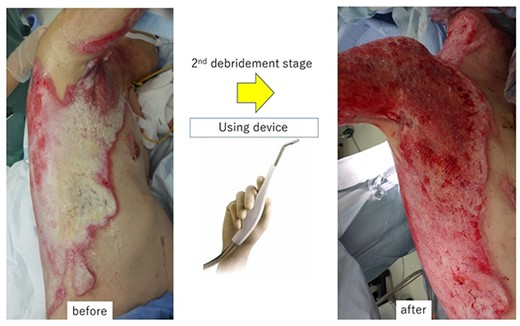
A second-stage debridement for slough using the Versajet™ hydrosurgery system (power setting: 5–10) was performed as a late surgery.
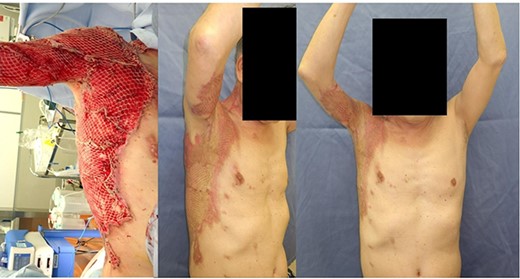
Mesh auto-grafts were applied, and an excellent range of motion was obtained without contracture after 8 weeks.
DISCUSSION
Whenever debridement is performed for extensive deep burns, the physician must decide whether to perform fascial excision or sequential excision, taking into account the costs and benefits for the patient. Fascial excision, which prioritizes the saving of life and skin graft engraftment, is associated with serious problems, including severe scarring and scar contracture. On the other hand, sequential excision is associated with other severe problems, including increased intraoperative bleeding and a decreased skin graft engraftment rate, but it can reduce the occurrence of severe scarring and scar contracture. In flame burn injuries caused by clothing ignition, the deep burn area often extends not only to the trunk but also to the axilla. In such cases, axillary scar contracture is inevitable and often requires additional skin graft or flap surgery, and it is clinically categorized by the degree of progression to the anterior axillary fold, posterior axillary fold and axillary dome [1]. It has been reported that contracture can be prevented by extended grafting and early splinting [2], that contracture can be improved by subcutaneous pedicled flap [3] and the usefulness of islanded posterior arm flap has been described [4]. On the other hand, in their review, Stekelenburg et al. noted that no consensus or definitive conclusion had been obtained regarding the outcomes of surgical intervention using grafts, flaps and dermal substitutes [5].
In local management, it is possible to prevent the deepening and contracture of burn wounds due to prolonged infection [6]. With the passage of time, necrotic tissue of the burn wounds degenerates from an indistinct and firmly adhered ‘eschar’ state to a well-defined and fragile infiltrated ‘slough’ state. Furthermore, at the initial stage, immediately after the patient is transported after having suffered a serious burn injury, it is difficult to strictly evaluate the depth of skin damage. Therefore, for preferable graft bed preparation, it is extremely important to select an appropriate debridement device at each stage. In the two-stage debridement strategy for deep axillary and trunk burns, in the first step, immediate debridement is performed with an electric dermatome (thickness: 0.4 mm). At this stage, under-debridement and bleeding control should be taken into consideration without excessive debridement of the tightly adhered necrotic tissue. At 1–2 weeks after the injury, a Versajet™ hydrosurgery system is applied in the second step, to perform radical debridement of the infiltrating necrotic tissue to achieve suitable wound bed preparation for the skin graft. Figure 4 shows the schema of the concept. In the treatment of extensive deep burns, failure of single-stage skin grafting is often due to residual necrosis caused by surgeon error [7]. The use of an electric dermatome (for eschar) and a Versajet™ (for slough) allows for debridement without over- or under-utilizing the characteristics of each device.
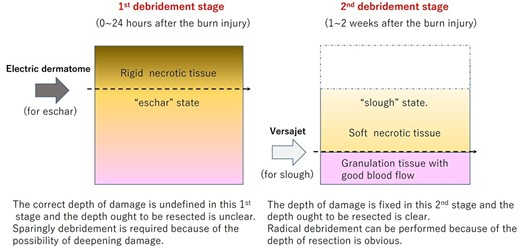
The schema of the concept of a stylized two-stage debridement strategy using an electric dermatome and a Versajet™ hydrosurgery system.
Taking advantage of the features of each device, step-by-step debridement eliminates the need for strict evaluation of the damaged skin depth by experts.
CONCLUSION
Determining the depth of skin burn damage in the early stages is always challenging. A two-stage debridement strategy with an electric dermatome and the Versajet™ hydrosurgery system can eliminate this difficulty and standardize the debridement procedure. The advantage of this strategy is that it is possible to reduce the risk of sepsis caused by adhesion of necrotic tissue in the general care setting.
AUTHORS’ CONTRIBUTIONS
M.H., M.T., and T.M. performed the surgery, M.H., N.K. and M.F. designed and directed the treatment. All authors read and approved the final manuscript.
CONFLICT OF INTEREST STATEMENT
The authors declare that they have no competing interests.
FUNDING
None declared.
CONSENT FOR PUBLICATION
Written informed consent was obtained from the patient for the publication of this case report and the accompanying images.



