-
PDF
- Split View
-
Views
-
Cite
Cite
David Armany, Matthew Allaway, Preet Gosal, Senarath Edirimanne, Sulman Ahmed, A new variation of duplicated extrahepatic bile duct encountered intraoperatively on cholangiogram, Journal of Surgical Case Reports, Volume 2022, Issue 10, October 2022, rjac463, https://doi.org/10.1093/jscr/rjac463
Close - Share Icon Share
Abstract
A potentially devastating complication of laparoscopic cholecystectomy (LC) includes iatrogenic bile duct injury, the incidence of which has remained stable at 0.3% over the past three decades. Although there are several relative risks such as surgeon experience and patient factors (male sex, obesity, older age), misinterpretation of biliary tree anatomy contributes towards 80% of iatrogenic common bile duct (CBD) injuries. Although extremely rare, an isolated duplicated common hepatic duct anomaly with a normal CBD remains a potential variation to encounter during biliary surgery. With only one similar variation published worldwide, we report the second case encountered during LC and confirmed on cholangiogram. Given these anomalies are asymptomatic and perpetuate iatrogenic CBD injuries, awareness of this variation is crucial. Preoperative diagnosis is possible with the use of magnetic resonance cholangiopancreatography; however, such imaging is not routinely used prior to LC in Australia due to factors including expense and availability.
INTRODUCTION
To date, the treatment of acute calculous cholecystitis with laparoscopic cholecystectomy (LC) remains the gold standard of surgical management [1]. Early cholecystectomy has been shown not be associated with higher morbidity and mortality compared with delayed cholecystectomy and hence is now the preferred approach at our institution [2]. Bile duct injury is a well-recognized complication of LC with an annual incidence of 0.23% seen in large volume audits. Currently, a contributor to iatrogenic biliary injury involves anatomical misidentification of the common bile duct (CBD) [3]. Misidentification can certainly be caused by anatomical biliary variation including congenital extrahepatic bile duct duplication [4]. Common hepatic duct (CHD) duplication is an extremely rare congenital biliary tree anomaly with only one previous documented case in a paediatric population [5]. Here we present a rare CHD anomaly. This would be the second such reporting of a similar CHD duplication worldwide and the first recorded within an Australian population.
CASE REPORT
A 61-year-old female with a background of Ischaemic Heart Disease, hypertension and hypercholesterolemia was referred to our institution with right upper quadrant abdominal pain with a background of known cholelithiasis. On further evaluation, the patient reported a 3-day history of right upper quadrant abdominal pain, nausea and vomiting. Abdominal examination revealed a tender right upper quadrant with localized voluntary guarding and a positive murphy’s sign. The patient was not clinically jaundiced. Her biochemical analysis revealed normal liver function tests with a mildly elevated CRP 14 mg/L and full blood count revealed an elevated WCC at 12.3 × 109/L.
Abdominal ultrasound revealed a thickened gallbladder wall measuring 3.6 mm, mobile sludge, small amounts of pericholecystic fluid and a positive sonographic murphy’s sign (Fig. 1). As such, the diagnosis of acute cholecystitis was made, and the patient underwent a LC.
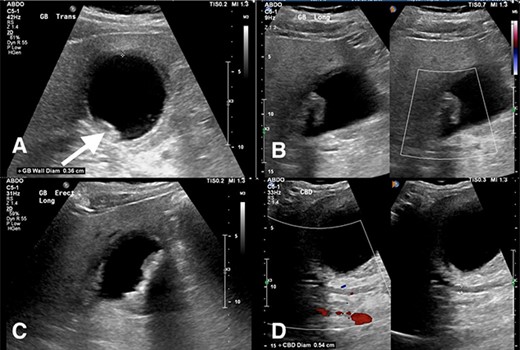
(A) Transverse view of the gallbladder showing a 3.6 mm wall diameter. Inferior arrow also shows small stones and sludge. (B) Longitudinal view of the gallbladder again showing mobile sludge. (C) Longitudinal view of the gallbladder showing a small amount of pericholecystic fluid. (D) Measurement of the CBD diameter at 5.4 mm (within normal limits).
Intraoperatively, standard 4 port laparoscopy was performed, and an oedematous gallbladder was encountered which required a combination of sharp and blunt dissection. The hepatocystic triangle dissection was challenging due to severe fibrosis. A ductal structure was isolated and seen to be entering the gallbladder which was subsequently clipped and a ductotomy performed. After cannulation of the ductotomy, an intraoperative cholangiogram (IOC) revealed what appeared to be a duplicated CHD separating the right and left hepatic drainage systems with a communicating aberrant extrahepatic duct (Fig. 2). Of note, no filling defects were appreciated in the distal common system.
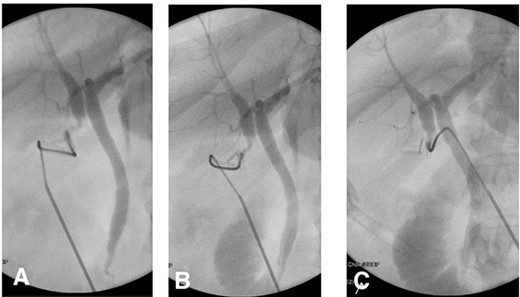
(A) IOC showing the point of cystic duct cannulation with retrograde contrast injection revealing a connection with a duplicated CHD draining the right system and another CHD draining the left system proximally. (B) and (C) Further contrast injection demonstrating no filling defects in the distal common system with good flow into the duodenum.
Given the extrahepatic duplication was directly confluent with the main system, an intraoperative consult with the hepatobiliary surgeon on call was placed. The decision was made to divide the cystic duct between clips and complete the cholecystectomy by dissecting the gallbladder from the cystic plate in the usual fashion, leaving the CHD duplication alone. At the end of the case, a 19Fr Blakes drain was inserted into the gallbladder fossae and secured.
The patient’s postoperative course was uneventful, the drain was removed on postoperative day three. Prior to discharge, a postoperative computed tomography (CT) cholangiogram was performed which revealed the duplicated CHD terminating within the region of the cholecystectomy clips with a communicating aberrant extrahepatic duct (Fig. 3). Subsequently, histopathology had shown chronic cholecystitis with cholelithiasis.
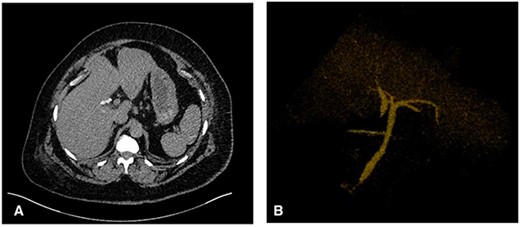
(A) Axial CT image showing the cholecystectomy clips at the base of a duplicated CHD with the corresponding CHD on the medial aspect. (B) 3D reconstruction demonstrating the CHD duplication with a single distal draining CBD.
DISCUSSION
CHD duplications are extremely rare, and the true incidence is unknown due to the condition’s asymptomatic nature [4]. The aetiology surrounding biliary tree abnormalities remains unclear. The current findings suggest a disruption in early human embryogenesis may limit the regression of primitive duct structures, although the exact cause of these anomalies is yet unknown [6].
Different variants of extrahepatic biliary tree anomalies have been encountered, typically intraoperatively at cholangiogram inciting the development of various classification systems of CBD duplications and aberrant right hepatic ducts [7, 8]. Amongst these, duplicated CBDs are the rarest which often include variations of duplicated CHDs that are always accompanied with duplicated CBDs (Fig. 4) [6]. Our case shows a duplicated CHD draining the right intrahepatic system with its counterpart draining the left and a communicating aberrant duct in between. A similar variant has been encountered only once in the literature in a 13-year-old male presenting with chronic epigastric pain and subsequent jaundice [5]. Despite the rarity of comparable variants, it is important to understand them owing to the risk of iatrogenic CBD injury [9]. The overall incidence of iatrogenic CBD injuries at LC has remained stable over the past three decades at 0.3% with current evidence suggesting that 80% of these injuries are due to a misinterpretation of biliary tree anatomy [10].
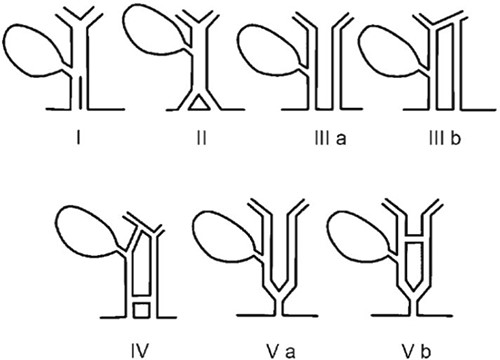
Duplicated CBD classification developed by Researchers E. Choi, J.H. Byun, D. Park et al. (2007). Type IIIa – Type Vb variants have duplicated CHD and CBD ducts with Type V duplications the rarest.
Given the rarity of this condition, diagnosis remains difficult within the preoperative stage. Although preoperative magnetic resonance cholangiopancreatography (MRCP) would have demonstrated the biliary variation prior to LC, its routine adoption in this setting is limited by its expense and availability [11]. In our institution for example, an average MRCP costs $AUD 1500 and may delay operative intervention and thus is not sustainable as a routine preoperative screening modality. Although ultrasound is both cheaper and more readily available at our institution, in this case it did not recognize the biliary variation. As such, the diagnosis of CHD duplication may have to be made intraoperatively at time of cholangiography. The routine use of IOC in all LC cases although not always necessary, may reduce rates of iatrogenic bile duct injuries by detecting various biliary tree anomalies [12]. In this case, an IOC helped confirm our intraoperative suspicion of aberrant biliary anatomy and helped outline the drainage system, prompting careful dissection of the gallbladder off the cystic plate and leaving the duplicated CHDs intact.
Consequently, this rare type of extrahepatic bile duct duplication was treated successfully and should be considered along with other encountered forms of interesting biliary tree abnormalities.
CONFLICT OF INTEREST STATEMENT
No conflicts of interest were identified in the preparation of this case report.
FUNDING
None.



