-
PDF
- Split View
-
Views
-
Cite
Cite
Jay Lodhia, Mubashir Jusabani, David Msuya, Cross-leg flap in a burn patient: our experience from a tertiary center from Northern Tanzania, Journal of Surgical Case Reports, Volume 2022, Issue 10, October 2022, rjac460, https://doi.org/10.1093/jscr/rjac460
Close - Share Icon Share
Abstract
Lower limb trauma with significant tissue loss poses a great challenge to the surgeons. Cross-leg flaps were first described in 1854 and are still used for limb-salvage surgeries in those not suitable for free tissue transfer or in resource-limited settings. Herein we present a case of a 16-year-old girl, otherwise well, who sustained burn injury to her right leg while cooking exposing the anterior aspect of her tibia. Limb-salvage surgeries were done including cross-leg ‘fascio-cutaneous’ flap with positive outcome. Herein, we share our experience showing an impactful and reliable option for limb salvage in resource-limited setting.
INTRODUCTION
Burns and associated injuries caused by exposure to fire, hot substances can be very debilitating. Globally ~90% of burn injuries are from low-middle income countries, areas that lack the crucial health care related infrastructures to decrease the extent and the austerity of burns [1].
Cross-leg flaps were first outlined by Hamilton in 1854 for lower limb coverage for large soft tissue defects [2]. The goal of limb salvage is to attain definite wound closure by using the appropriate flap [3].
Kilimanjaro Christian Medical Centre is one of the four tertiary hospitals in Tanzania. This hospital covers a population of ~11 million people in the Northern Zone. In 2016, the hospital inaugurated a dedicated Burn unit, which has a total of 20 beds. One of the biggest challenges faced in the unit is lack of trained personnel in the field of plastic and reconstructive surgery, which is of utmost importance for treatment and rehabilitation of these patients [4].
CASE PRESENTATION
We present a 16-year-old female who was referred to our hospital 2 weeks after she sustained burn injury to her right leg while cooking. This preceded after the roof of her house fell due to heavy rain. There was a positive history of loss of consciousness for an unknown period of time followed by fully regain in the level of consciousness. She was brought in with extensive burn wounds on her right leg to her right foot exposing the Tibia, and gangrenous first, second toes. Surgical debridement and Rays amputation was done on the first and a disarticulation at the level of the proximal interphalangeal joint was done on the second toes.
She was planned for osteo-perforation (trephination) after 3 weeks in the ward to allow granulation tissue to attain bone coverage but failed (Fig. 1). She was then planned for cross-leg flap. After the flap design was made by the surgeons, the patient and the family were counselled on the treatment procedure, morbidity of the donor site, need for skin grafting and the duration of treatment and stay in the ward and possible complications were also addressed. She was then taken to the theatre whereby thorough surgical debridement was done, intra medullary irrigation was also done through the osteo-perforated areas with copious amount of saline. The defect was covered using a conventional cross-leg flap based anteromedially with a 1:3 flap ratio was done; fascio-cutaneous flap was grafted from the posterior aspect of her left leg and covered the exposed tibia of the affected leg (Fig. 2). The flap is nourished by the tibial perforators through the pedicle. External-fixator was used to attain proper leg position to allow better post-operative wound dressing and to allow knee and ankle physiotherapy and mobilization (Fig. 3).
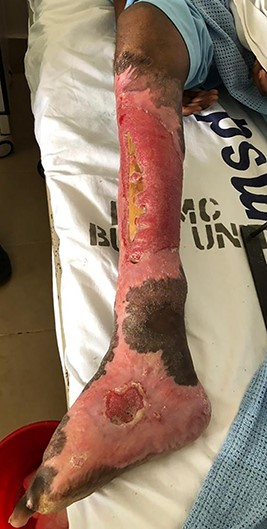
Post amputation of big and second toes and post trephination, exposed tibia.
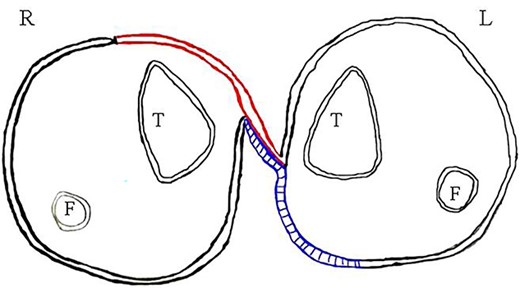
Diagrammatic representation (L-left, R-right, T-tibia, F-fibula, red-flap and blue-grafted area).
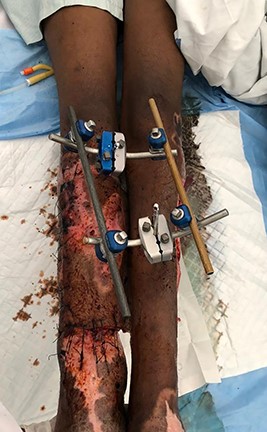
Post cross-leg flap with external-fixator for immobilization of both lower limbs.
Forty-eight hours post operatively the patient had some marginal skin necrosis, which was excised bed-side not hindering the flap and coverage (Fig. 4A). Four days post-operative surgical site infection was noted with pus discharge from the recipient site (Fig. 4B), of which pus swab for culture and sensitivity isolated Klebsiella spp. sensitive to Meropenem and Gentamicin of which she was kept on intravenous Gentamicin for 14 days with positive outcome.
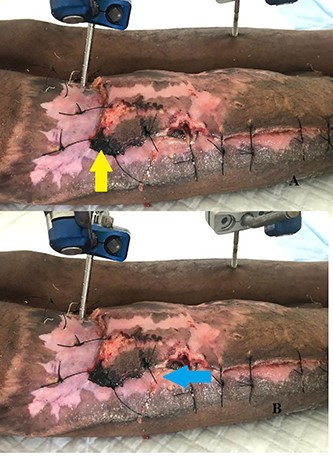
(A) Flap edge necrosis (yellow arrow) (B) pus discharge (blue arrow).
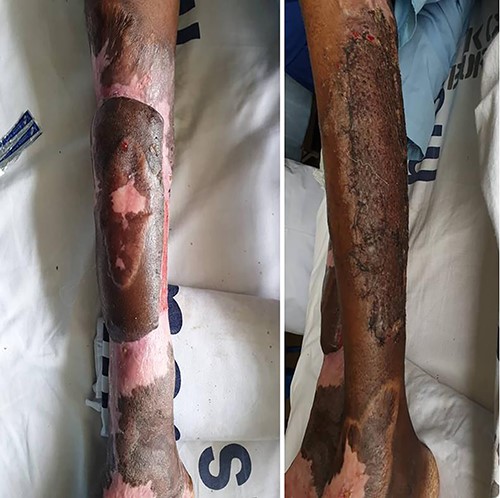
Flap division was done 4 weeks later and split thickness skin grafting was done on the donor site (Fig. 5). The wounds were dressed with sterile saline and covered with sterile Vaseline gause. The patient faired well and was discharged after 3 weeks to continue with dressing at the nearby health center. She was then reviewed after 6 months where she was walking with a walking stick with moderate ankle joint stiffness. There were no signs of local infection and the grafted areas were healed well.
DISCUSSION
Lower extremity trauma with extensive tissue loss continues to present a challenge to the surgeons. Cross-leg flaps were first described in 1854 by Hamilton and are still used to salvage lower extremities in those not suitable for free tissue transfer or those in resource-limited settings [5]. Soft tissue injury can be extensive to the extent bone, tendon and blood vessels can be exposed with a risk of desiccation if early tissue coverage is not provided due to many reasons including lack of personnel [6].
There are several lower limb injury severity scoring systems to guide surgeons in deciding whether to amputate or perform limb-salvage surgeries. These scoring systems have not shown to be good predictors of limb amputation or salvage, but rather outcome depends on the surgeons’ experience and the facilities available [6].
Extensive burn injuries can be a complex problem especially when associated with bone exposures, which eventually lead to drying and sequestration and would necessitate amputation if the bone coverage is not attained as early as possible. The fascio-cutaneous flap is a local flap, which includes the skin, subcutaneous fat and the fascia but not the muscle [7]. In resource constrained areas like ours, cross-leg flaps are a decent way of attaining huge soft tissue defects when advanced reconstructive and microsurgical facilities are not available, however this still poses a significant challenge. Cross-leg flaps serve as a nutrient flap for the distal limb even after pedicle division.
Free flap requires expertise and microvascular reconstruction and with the prolonged surgery and high risk of failure, it was not an option in our case hence cross-leg flap was opted. Its use does impose risk of necrosis, donor site cosmetic deformity and joint stiffness due to the prolonged immobilization [6].
Extensive Soft tissue injuries comprise a big percent of inpatients in the Burns and Trauma unit, involving the underlying tendons, vessels and bone. Cross-leg flap plays an important role in coverage and does not require sophisticated surgical expertise and equipment. Efforts to salvage can be rewarding and should be opted where possible.
ACKNOWLEDGMENT
The authors would like to thank the patient’s mother for permission to share her child’s medical history for educational purposes and publication.
CONFLICT OF INTEREST STATEMENT
The authors declare they have no competing interests.
FUNDING
There was no funding towards this research.
AUTHORS’ CONTRIBUTIONS
JL drafted and conceptualized the manuscript. JL and MJ were the lead surgeons and reviewed medical records. DM was the clinical supervisor and did the final editing. All authors have read and approved the final script.
CONSENT
Written informed consent was obtained from the patient’s mother for publication for this case report; additionally, accompanying images have been censored to ensure that the patient cannot be identified. A copy of the consent is available on record.



