-
PDF
- Split View
-
Views
-
Cite
Cite
Ryan C Yang, Yousef Abuhakmeh, John P Schriver, Daniel W Nelson, Recurrent pancreatitis due to intraductal papillary mucinous neoplasm in a young adult, Journal of Surgical Case Reports, Volume 2021, Issue 6, June 2021, rjab270, https://doi.org/10.1093/jscr/rjab270
Close - Share Icon Share
Abstract
A young adult male presented with recurrent pancreatitis and a 2.2 cm mixed duct intraductal papillary mucinous neoplasm (IPMN) located in the pancreatic body.
Our patient presented at age 21 with his second hospitalization for acute pancreatitis within a year. A mixed duct IPMN with main ductal dilation was identified, which prompted additional workup. Based upon the findings the patient was counseled regarding the risks and benefits of surveillance versus surgery. The patient elected to undergo a robotic-assisted laparoscopic distal pancreatectomy and splenectomy. Final pathology revealed an IPMN involving branch and main pancreatic ducts with low and focally high-grade dysplasia.
IPMNs are increasingly being identified. Consensus guidelines generally propose surveillance, but management in young adults can be complex. Herein we present the second youngest reported case and highlight the continued need for consensus management guidelines.
INTRODUCTION
The index case of intraductal papillary mucinous neoplasm (IPMN) was reported by Ohhashi in the 1980s [1]. While the true prevalence is unknown, estimates range from 0.8 per 100 000 persons to as high as 10% of the population over 70 years of age [2]. The growing prevalence is attributed to increasing incidental discovery during cross-sectional studies performed for other medical conditions, which is particularly true in the aging population [3, 4]. IPMNs are typically discovered in the sixth to seventh decade of life, with the youngest reported case at age 14 [5, 6]. To our knowledge, we are reporting the second youngest case of IPMN.
CASE REPORT
The patient is a 21-year-old male who presented for surgical consultation after his second hospitalization for acute pancreatitis over a 6 month period. During his most recent admission, magnetic resonant imaging (MRI) demonstrated a 2.2 cm cyst in the pancreatic body with dilatation of the main pancreatic duct to 5 mm suggestive of a mixed duct IPMN (Fig. 1). Presence of two ‘worrisome’ features, which included lesion size >2 cm and main duct dilation >5 mm according to the Fukuoka 2017 management guidelines, prompted a referral for endoscopic ultrasound (EUS) and cyst aspiration with pathologic fluid analysis [7]. A laboratory workup was performed, to include carbohydrate antigen 19-9, carcinoembryonic antigen and pancreatic islet antibody.
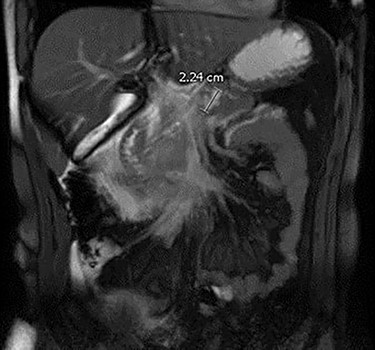
Laboratory workup was unremarkable. EUS aspirate analysis demonstrated the presence of mucin. Cytology was negative for evidence of malignancy. Upon follow-up, patient was counseled that his clinical history and radiographic imaging demonstrated several concerning findings including cyst size, main duct dilation diameter and recurrent episodes of pancreatitis. The constellation of findings were suggestive of a benign mixed type IPMN, however, the presence of several worrisome features posed increased risk for development of malignancy over time. The patient was counseled that active interval imaging surveillance was a reasonable option. However, given his young age and health status, surgical intervention, in his case robotic distal pancreatectomy with splenectomy, could prevent decades of interval imaging surveillance, reduce future malignancy risk, and prevent future episode of pancreatitis. After review of these options and time to discuss with his family, the patient ultimately opted for surgical intervention.
The patient received vaccinations preoperatively against encapsulated organisms to include Streptococcus pneumoniae, haemophilus influenzae type b and meningococcus. A dedicated pancreas protocol computed tomography scan was performed for operative planning, which demonstrated interval increase in the size of the cyst to 2.4 cm (Fig. 2). On the day of surgery a robotic-assisted laparoscopic distal pancreatectomy was performed. We elected to perform a splenectomy because the splenic vasculature was found to be densely adhered to the posterior aspect of the pancreas secondary to repeated bouts of pancreatitis. The distal pancreas and spleen specimen, along with 21 lymph nodes, were removed en bloc. Final pathology demonstrated a 1.4 cm IPMN with low-grade dysplasia involving the branch ducts and focal high-grade dysplasia involving the main duct. No invasive malignant component was identified in the specimen and all examined lymph nodes were benign. The patient had an uncomplicated recovery and was discharged on postoperative Day 5 following drain removal. Completion of his post-splenectomy vaccinations were confirmed at his initial follow-up clinic visit. The patient will report for an additional follow-up with active surveillance imaging in 6 months.
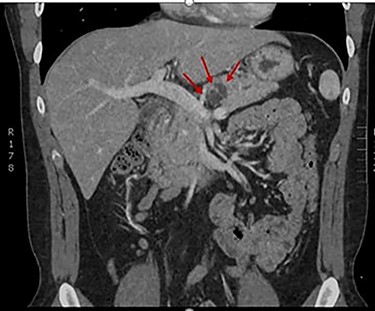
CT demonstrating resolution of pancreatitis and interval growth of IPMN to 2.4 cm.
DISCUSSION
IPMN is a known premalignant pancreatic lesion, though the exact mechanism and transformation rate is unknown [8]. A recent retrospective study demonstrated a 5-year incidence rate of malignant transformation at 3.3%, which increased to 15.0% at 15 years after the initial diagnosis of IPMN [9]. Although several consensus guidelines have been published, there is significant variance regarding their recommendations for surveillance versus surgical intervention and in particular, a scarcity of data to inform the management of young adults. The existing societal guidelines include the International Association of Pancreatology (IAP), the European Study Group on Cystic tumors of the Pancreas (ESGCP), the American Gastroenterology Association (AGA) and the American College of Gastroenterology (ACG). These are all based on low-quality data and lack unifying indications for surgical intervention [10]. Notably, a retrospective study of these guidelines demonstrated overtreatment in the IAP and ESCGP, while the AGA guidelines were associated with undertreatment [11].
Our patient did not meet absolute indications for surgery as defined by the aforementioned guidelines such as presence of jaundice, an enhancing mural nodule greater than 5 mm, or main pancreatic duct dilation over 10 mm. However, our patient did exhibit several ‘worrisome’ features including size of cyst >2 cm, main duct dilation of 5 mm and history of recurrent pancreatitis. According to the European guidelines, pancreatitis is reported to occur at a rate of 12 to 67% [12]. In a patient who had already suffered two bouts of acute pancreatitis in a 6-month time frame, nonoperative management would require persistent life-long MRI surveillance every 3 months. We believe he met relative guideline indications for resection and practical consideration against surveillance. Since his final pathology demonstrated IPMN without an invasive component, he will only need post-resection surveillance imaging at the 2 and 5 year marks instead of life-long surveillance [13].
We considered the morbidity and mortality risk associated with surgical intervention in our patient. In respect to postoperative morbidity risk, a retrospective study of patients receiving surgical intervention for IPMNs demonstrated an overall 12% rate of morbidity in patients who underwent a distal pancreatectomy with biochemical leak as the most frequently reported complication (44%) [14]. Weighing the relative risk of postoperative morbidity against recurrent pancreatitis and potential for malignant transformation as high as 10.7% [15], we believe surgical intervention was justified.
Our case reinforces the growing field of pancreatic neoplasia, particularly IPMNs as their prevalence continues to rise with improved cross-sectional imaging. Given the established premalignant nature of IPMNs and the lack of consensus guidelines with strong evidence, we highlight the necessity of continued data collection and reporting to develop a standard of care for this disease and to further elucidate the mechanism for malignant transformation.
DISCLOSURE
The views expressed in this publication are those of the author(s) and do not reflect the official policy or position of William Beaumont Army Medical Center, Department of the Army, Defense Health Agency, or the US Government.
CONFLICT OF INTEREST STATEMENT
None declared.
References
Ohhashi K, Murakami Y, Muruayama M, et al. Four cases of “mucin-producing” cancer of the pancreas on specific findings of the papilla of vater.
- pancreatitis, acute
- pancreatitis, chronic
- dilatation, pathologic
- laparoscopy
- pancreatic ducts
- splenectomy
- surgical procedures, operative
- guidelines
- neoplasms
- pancreas
- pathology
- surveillance, medical
- pancreatectomy, distal
- pancreatic intraductal papillary-mucinous neoplasm
- young adult
- dysplasia
- consensus



