-
PDF
- Split View
-
Views
-
Cite
Cite
Yusuke Takahashi, Hitoshi Seki, Akira Kobayashi, Chronic expanding hematoma mimicking seroma, following a totally extraperitoneal approach for inguinal hernia: a case report, Journal of Surgical Case Reports, Volume 2021, Issue 6, June 2021, rjab260, https://doi.org/10.1093/jscr/rjab260
Close - Share Icon Share
Abstract
Chronic expanding hematoma (CEH) mimicking seroma following inguinal hernia surgery has not been reported previously. A 78-year-old man underwent laparoscopic repair of a left direct hernia via a totally extraperitoneal approach. He was discharged 2 days after surgery without any complications. Two weeks later, he complained of left inguinal bulging without pain. We considered seroma and decided to observe the patient for 1 month. However, the cyst did not change in size. Additional cyst aspiration and drainage attempts were unsuccessful. Three months after the initial surgery, we performed a second surgery (resection of the cyst) because conservative therapies were ineffective. The resected cyst was pathologically diagnosed as a CEH. The postoperative course was uneventful, and no recurrence was observed. Complete excision of a CEH is mandatory because aspiration and drainage cannot prevent recurrence.
INTRODUCTION
Chronic expanding hematoma (CEH) occasionally develops after trauma and surgery, and can occur anywhere in the body; however, to our knowledge, no cases have been reported following herniorrhaphy [1, 2]. Therefore, the incidence of this entity following herniorrhaphy is unclear, and symptoms are likely independent of size. Regardless of the CEH site, complete excision with removal of the capsule is reportedly necessary to prevent recurrence [3–5]. Postoperative seroma, which occasionally occurs following herniorrhaphy and has a similar appearance to CEH, should be clearly differentiated from CEH because, unlike CEHs, they often recede without surgical intervention. Herein, we report a rare case of CEH following herniorrhaphy.
CASE REPORT
A 78-year-old man was admitted to our hospital with a left inguinal hernia. We performed laparoscopic hernia repair via a totally extraperitoneal approach (TEP) using a 3D Max® mesh (Bard, Japan). The mesh was fixed using a CapSure® (Bard, Japan) Permanent Fixation System. The hernia was a type M2 according to the groin hernia classification of the European Hernia Association [6]. The postoperative course was uneventful, and the patient was discharged 2 days after the surgery.
Two weeks later, he complained of an asymptomatic left inguinal bulging. Plain computed tomography (CT) revealed fluid retention with coating and no hernia recurrence (Fig. 1a). Ultrasound echography revealed a mosaic pattern within a 5.0 × 4.0 cm cyst (Fig. 1b). We considered the possibility of postoperative seroma; therefore, we decided to observe the patient for 1 month.
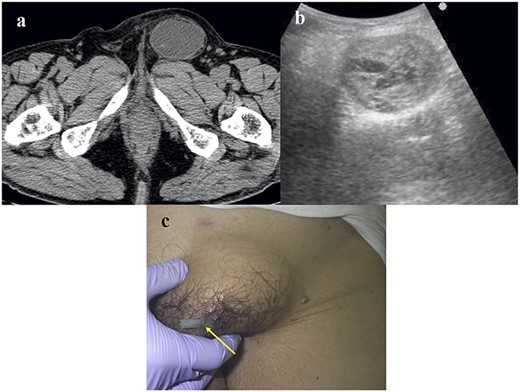
Images of the CEH. (a) Plain CT image. No hernia recurrence was observed and fluid collection was identified within the capsule. (b) Echography revealed a mosaic pattern. (c) A Penrose drain (arrow) was inserted into the CEH.
One month later, the cyst had not changed in size. The cyst was punctured, and a chocolate-like old hematoma (30 ml in volume) was aspirated. One week later, the temporally contrasting cyst had enlarged again. We inserted a Penrose drain into the cyst (Fig. 1c), which was also ineffective. Contrast-enhanced CT revealed findings similar to those of the plain CT performed for the diagnosis of fluid retention, with no extravasation. We decided to perform surgery because the conservative treatments trialed, including conservative observation, aspiration and drainage, had been unsuccessful.
An anterior rather than a laparoscopic approach was selected. The cyst was separated from the spermatic cord (Fig. 2a) and its connecting vessels were divided (Fig. 2b). A prophylactic onlay mesh was placed to reinforce the posterior wall of the inguinal canal, despite the absence of hernia recurrence.
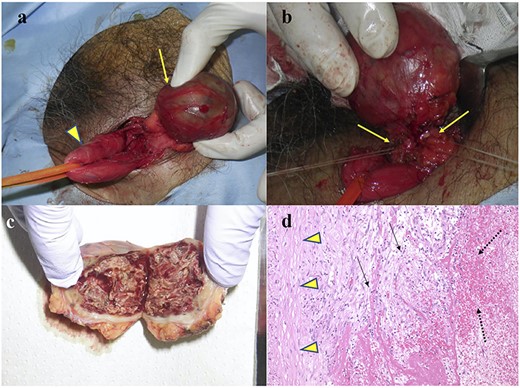
Intraoperative and pathological findings. (a) The CEH (arrow) was separated from the spermatic sheath (arrowhead). (b) The vessels (arrow) connected to the CEH were divided. (c) Cut surface of the resected specimen. (d). Hematoxylin–eosin staining of the CEH (×100). The specimen contained inflammatory cells (arrow), such as lymphocytes and macrophages, and the hematoma (dotted line) was capsulized with collagen fibers (arrowhead).
The cut surface of the resected specimen contained the fascia, and the content had a mosaic-like appearance (Fig. 2c). Pathologically, the cyst consisted of an old hematoma, chronic inflammatory infiltrates, such as lymphocytes and macrophages and fibrous tissue (Fig. 2d). The final diagnosis was CEH. The postoperative course was uneventful, and no recurrence of CEH or inguinal hernia was observed. The treatment strategy is presented in Fig. 3.
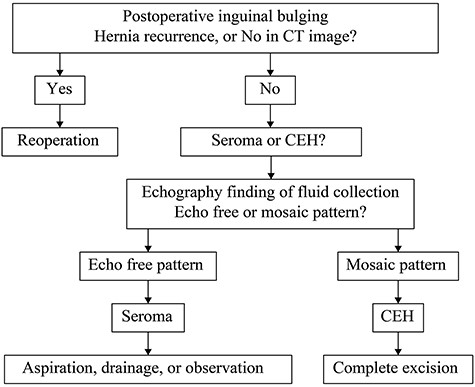
Treatment strategy for inguinal bulging following inguinal hernia surgery.
DISCUSSION
CEH was first reported by Friedlander et al. in 1968 [7] and the detailed pathophysiology was later confirmed by Reid et al. in 1980 [8]. Certain stimuli, such as trauma and surgery, are related to the development of CEH [5, 7, 8]. In fact, some rare cases of surgery-related CEH have been reported [5, 9, 10]. Therefore, CEH can theoretically occur anywhere in the body. However, to our knowledge, the occurrence of CEH following herniorrhaphy has not yet been reported.
In the laparoscopic approach to groin hernia repair, such as TEP or laparoscopic transabdominal preperitoneal repair, the surgical field is mainly the preperitoneal space, not the inguinal subcutaneous region. In contrast, in the anterior approach, such as the Lichtenstein and Kugel methods, the surgical field includes the inguinal subcutaneous region. In the laparoscopic approach, adhesion does not occur in the inguinal subcutaneous region. Therefore, although CEH has not been reported following herniorrhaphy, CEH may be a specific complication of laparoscopic herniorrhaphy.
The appearance of CEH is similar to that of seroma, which occasionally occurs following TEP, although the latter typically resolves without a specific procedure [11]. CT is useful for the discrimination of hernia recurrence and other pathologies. However, CT could not differentiate postoperative seroma from this rare entity of CEH. In contrast, magnetic resonance imaging is useful for diagnosing CEH [7, 8] but is often too expensive for this purpose. As shown in Fig. 1b, the echography findings of CEH, a mosaic pattern, differ from those of seroma, an echo-free pattern. Mosaic patterns likely reflect old hematomas with plasma from vessels. Because we did not observe the CEH following TEP, we first considered seroma and elected to observe the patient. After 1 month without observing the seroma, aspiration and drainage of the CEH were performed. At this point, CEH was considered because an old hematoma was evident.
Complete excision of the CEH is mandatory because aspiration or drainage of the fluid cannot prevent recurrence [1–5]. Indeed, in our case, aspiration and drainage of the CEH were unsuccessful.
CONCLUSION
CEH should be considered in cases of postoperative inguinal bulging following inguinal hernia repair. Differentiating it from seroma is important because the treatment strategies of these two entities differ. After exclusion of hernia recurrence, echography was useful for the differential diagnosis of CEH. Rather than aspiration, drainage and observation, complete excision, including of the fascia, should be performed when CEH is suspected.
ACKNOWLEDGEMENT
We would like to thank Editage (www.editage.com) for English language editing.
CONFLICT OF INTEREST STATEMENT
None declared.



